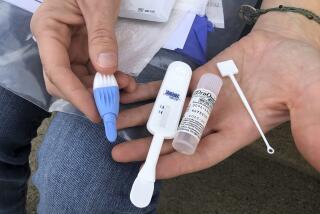
Truvada, a pill to fight HIV, stirs controversy among gays

- Share via
It would have seemed the stuff of fantasy in the dark days of the 1980s, when an AIDS diagnosis was tantamount to a death sentence: a pill, taken daily, that could protect against HIV infection.
But today, such a drug exists. The blue tablet, marketed as Truvada, has been available to people at risk of being exposed to HIV since 2012.
The pill can be highly effective — reducing infection risk by as much as 92%, according to the U.S. Centers for Disease Control and Prevention.
It could have a dramatic effect in Los Angeles County, where about 47,000 people are known to live with HIV. Contracting the virus is no longer a death sentence because of a cocktail of drugs that suppress it, but the county still reports more than 1,000 new HIV infections each year.
“We want to bring HIV to its knees, and this will help,” said Mario Perez, who directs the county’s prevention program.
But the concept of using the pill — known in medical circles as pre-exposure prophylaxis — has stirred a surprising debate in the gay community, with some longtime activists calling Truvada a “party drug” that people will never take consistently enough to stave off infections. If not taken daily, the CDC warns, protection levels are lower.
Most notable among the skeptics is AIDS Healthcare Foundation President Michael Weinstein, whose organization recently launched a new advertising campaign urging the CDC to rethink its support for a communitywide prevention method that does not emphasize condom use first and foremost.
Those with a more sanguine view of the pill wonder why critics such as Weinstein’s foundation would dismiss any tool with the potential to decrease HIV infection rates, which are creeping up among young gay and bisexual men of color.
“There is a moral imperative to make this available for folks who think it’s the right approach,” Perez said. “We’re big fans in giving people options to achieve their goals, with no judgment.”
Public health officials throughout the U.S. have already made the approach a key part of their official HIV prevention strategies. Last spring, the CDC added its stamp of approval when it released official guidelines on pre-exposure prophylaxis. In July, New York Gov. Andrew Cuomo put the method at the center of an effort to drastically cut the numbers of new HIV infections in his state by 2020.
Truvada combines two drugs that have been part of the anti-retroviral cocktail taken by HIV-positive patients for years. The medicines, tenofovir and emtricitabine, work together to block an enzyme called reverse transcriptase that allows HIV cells to multiply. In addition to suppressing HIV that is already in the body, the drugs can also prevent the virus from gaining a foothold initially.
It’s unclear how many in California are taking the drug to prevent HIV infection, but the number probably isn’t very large. At $13,000 a year, Truvada is expensive, but it is covered by most insurance plans.
In early November, Gilead Sciences, the company that manufactures the drug, reviewed retail pharmacy records from a little more than half of U.S. pharmacies that dispensed Truvada between January 1, 2012, and March 31, 2014, and found that 3,253 people in the U.S. started the prevention regimen during that period.
Advocates of pre-exposure prophylaxis blame the slow increase at least in part on moralizing by people such as Weinstein. The crux of critics’ concern is that offering gay men another way to block AIDS infection will undermine a long-standing push in the community to promote condom use, which is known to also prevent the transmission of HIV and STDs.
CDC guidelines for administering pre-exposure prophylaxis stipulate that Truvada should be used with condoms, not instead of them. But some, most notably Weinstein, say that men won’t bother with condoms if they believe they are protected by a pill.
“You have to be really paranoid about your health to wear a belt and suspenders,” he said. “If the culture shifts to unprotected sex because of the campaign to promote Truvada, then [HIV] rates will go up.”
Weinstein and others have noted that overall risk reductions in clinical trials for pre-exposure prophylaxis were lower than the CDC-cited 92%. The so-called iPrEx study, for instance, reported that people who took Truvada experienced only a 44% reduction in HIV infection risk.
The overall risk reduction rate was low because many participants in the study did not take their medication as directed, scientists say.
Weinstein argues that others will also fail to use the drug correctly, leading to a rise in new HIV cases and other sexually transmitted infections.
Adherence is a common worry. Mitchell Katz, who directs Los Angeles County’s Department of Health Services, said that patients who have been careless about HIV prevention thus far — choosing not to use a condom despite the risks — are unlikely to ask their doctor about Truvada or follow through on daily dosing.
“I think [pre-exposure prophylaxis] is a very useful intervention for a very small percentage of people,” he said. “I don’t think it’s for everyone.” Katz said county hospitals and clinics do not have rules against providing the method, but that use was not yet widespread.
Even the most enthusiastic supporters acknowledge that responsibly expanding Truvada use will mean setting up systems to make sure patients take the pill as directed.
Speaking with health advocates in August, Sonali Kulkarni, medical director of the Los Angeles County Department of Public Health’s Division of HIV and STD Programs, said her agency was trying to figure out how to provide “wraparound counseling” to such users.
Such support would be designed to boost drug adherence and HIV risk reduction, county health officials said.
Pre-exposure prophylaxis “is a responsibility,” added AIDS Project Los Angeles health and wellness outreach worker Ken Almanza, who began using the method earlier this year and is trying to teach other Latinos about the intervention.
But supporters also cite mounting evidence that the regimen is highly effective when followed properly — and argue that focusing on supporting adherence makes more sense than counting Truvada out altogether.
Weinstein’s foundation “looked at the data and came out in opposition; the majority of the rest of the groups that do HIV work have come to an opposite conclusion,” said David Evans, director of research advocacy at Project Inform in San Francisco. “It’s not a silver bullet, it’s not a magic pill, it’s best with condoms — but there’s also a recognition that not everybody uses condoms, and for those people, even a moderate effect would be advantageous.”
Advocates in the gay community see critics such as Weinstein as Puritans, engaging in what they call a shaming exercise similar to the disapproval unmarried women faced 50 years ago when they demanded access to the birth control pill.
Users have been branded as taking the pill so they can engage in promiscuous sex without condoms.
“There’s still a fair amount of stigma around being a Truvada user,” said Jim Pickett, director of prevention advocacy at the AIDS Foundation of Chicago, and an advocate. “It’s an admission: I don’t use condoms all the time. I’m not perfect, but I can be prepared.”
Pickett operates a website that allows Truvada users to announce their decision to take the drug, and to discuss their experiences.
Los Feliz resident Jesse Reed took his Truvada story to Facebook.
“Today is the first day in a new chapter of HIV prevention in my personal journey,” he wrote, posting a photo of the oblong tablet.
For men such as Reed, 39, who came of age shortly after the 1980s AIDS epidemic, the fear of contracting HIV has always been the monster under the bed.
He’s hoping that will change now.
Twitter: @LATerynbrown
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.