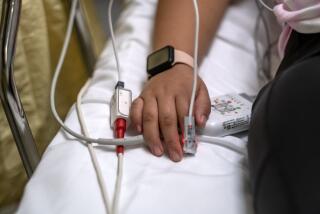
Ebola safeguards are being taken, Southland health officials say

- Share via
The paramedics at Los Angeles Fire Station 51 got the call Tuesday night: A traveler, just off an evening flight, was ill in an airport terminal and needed medical care.
The patient had flown in from a U.S. airport, the crew learned, but had initially set out from Liberia — an epicenter of the uncontrolled Ebola outbreak in West Africa, which has killed more than 4,000 people so far.
The revelation set off a series of precautions. The paramedics donned protective gear and called ahead to warn emergency room workers at Centinela Hospital Medical Center in Inglewood, who placed the patient in isolation and called public health authorities.
------------
FOR THE RECORD:
Ebola preparations: In the Oct. 13 LATExtra section, an article about what medical workers are doing to prepare should an Ebola case emerge in Southern California said that a nurse in Spain had contracted the disease from a patient and died. As of Monday, the nurse was alive and in serious but stable condition. —
------------
Within 24 hours, based on new details and a careful review of the patient’s symptoms and tests, county health officials said they had not been dealing with a suspected Ebola case after all, and praised medical teams for thinking on their feet.
“What we’re hearing about is good news,” Dr. Jeffrey Gunzenhauser, interim public health officer for the county, said during a phone call with reporters last week. “It shows hospitals are doing what they’re supposed to do. They’re looking out for cases and contacting us and making sure everyone is protected.”
Amid news of the first Ebola death in the U.S. — that of Thomas Eric Duncan, who died in a Dallas hospital that initially misdiagnosed him and sent him away — local officials say they are working to get medical providers ready, should an Ebola case emerge in Southern California.
So far, there have been no confirmed or suspected Ebola cases in Los Angeles County, and officials say they do not expect a major outbreak.
But some on the front lines, alarmed by the death last week of a nurse in Spain who contracted the virus from a patient, are concerned that efforts to prepare healthcare workers aren’t going far enough. On Sunday, officials reported a healthcare worker who treated Duncan has contracted Ebola.
“The tools are minimal and the training is minimal,” said Jonathan Bestwick, an emergency room nurse at Kaiser Permanente’s Baldwin Park Medical Center. “Everyone needs to step up to the plate.”
Public health authorities in Los Angeles County are rolling out Ebola guidelines based on recommendations from the U.S. Centers for Disease Control and Prevention, which call for providers to don protective gear — goggles, gloves, masks and gowns — when working with a suspected Ebola patient; to isolate suspected Ebola cases in a room with its own bathroom; and — perhaps most key — to immediately ask patients with symptoms such as vomiting, nausea and fever if they have traveled to West Africa or been in contact with someone who has.
Last week, during an emergency report to county supervisors, Gunzenhauser said his department was getting the message out.
“We’re reaching out to all the providers and hospitals,” Gunzenhauser told reporters the following day. “There are 25,000 [licensed doctors] — and I wish I could meet with all of them and make sure they were on top of it. This is a teachable moment.”
Cathy Chidester, director of the county’s Emergency Medical Services Agency, told The Times that her organization had issued guidance and taken part in conference calls with fire chiefs, ambulance companies and hospitals to make sure providers understood all Ebola guidelines, including requirements for protective gear and how to properly decontaminate transport vehicles.
It is largely up to healthcare providers such as ambulance companies and hospitals to follow through and make sure medical staff know proper procedures and have access to the equipment they need — a circumstance that worries some nurses and other workers.
The union National Nurses United has been calling on hospitals to step up preparations, publicizing results from a voluntary Web survey that show that more than 85% of responding nurses think their employers aren’t doing enough.
“We see hospitals disseminating fact sheets and referring people to CDC or public health websites,” said Bonnie Castillo, who directs the organization’s Ebola response program. “We see that as woefully inadequate in terms of training and education.”
Several nurses interviewed by The Times questioned whether their hospitals could execute plans.
Marilen Castanon, an intensive care unit charge nurse at St. Francis Medical Center in Lynwood, said that her employer was planning on a staffing ratio of 3 nurses to 1 Ebola patient in intensive care, but that current staffing levels would make that adjustment difficult.
“We already struggle with 2 to 1,” she said. “We’re just going to have to deal with it.”
Dr. Arun Patel, director of quality, patient safety and risk management at the county’s Department of Health Services, said that hospitals and clinics were continuously assessing their supplies of protective gear, and that additional training was rolling out first to the places most likely to see an Ebola patient walk through the door: emergency departments and urgent care clinics, then primary care settings.
“I think anyone who didn’t have concerns about their preparedness just hasn’t thought about it,” Patel said. “You should be concerned and you should be checking it.”
Infection control experts at UCLA medical centers in Westwood and Santa Monica have provided emergency departments with Ebola kits containing recommended protective gear such as suits, masks, gloves and booties.
UCLA has an Ebola response team that will take the lead should a case arise and designated areas that are equipped to handle waste disposal, said infectious disease specialist Dr. Daniel Uslan, who is part of the effort.
The hospital is also drilling medical workers on procedures.
“We’d like to work out the kinks in advance and not in hindsight,” Uslan said.
At St. Joseph Hospital in Orange, a task force was “tightening up protocols” for managing Ebola and other emerging diseases, said Dr. Raymond Casciari, a pulmonologist and former medical director.
He said he was confident hospitals were ready to handle whatever came their way, but he worried about a different scenario: what might happen in public places.
“Doctors and nurses are satisfied with the current isolation procedures. The fear is that someone will not tell the truth, or that something will slip through,” he said.
Some colleagues from St. Joseph saw Elton John perform at Staples Center this month, Casciari said.
“Do you realize what one Ebola patient could do at a concert like that?” he asked.
Emergency personnel are not the only ones on edge.
On Sunday, a United Airlines flight that landed at Los Angeles International Airport was diverted for several hours to a remote gate after a passenger exhibited “flu-like symptoms” associated with Ebola. It was later determined that the woman was not at risk for the deadly virus but instead suffered from motion sickness.
Twitter: @LATerynbrown
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.