Obamacare helping improve access to medical care for the poor, new studies show
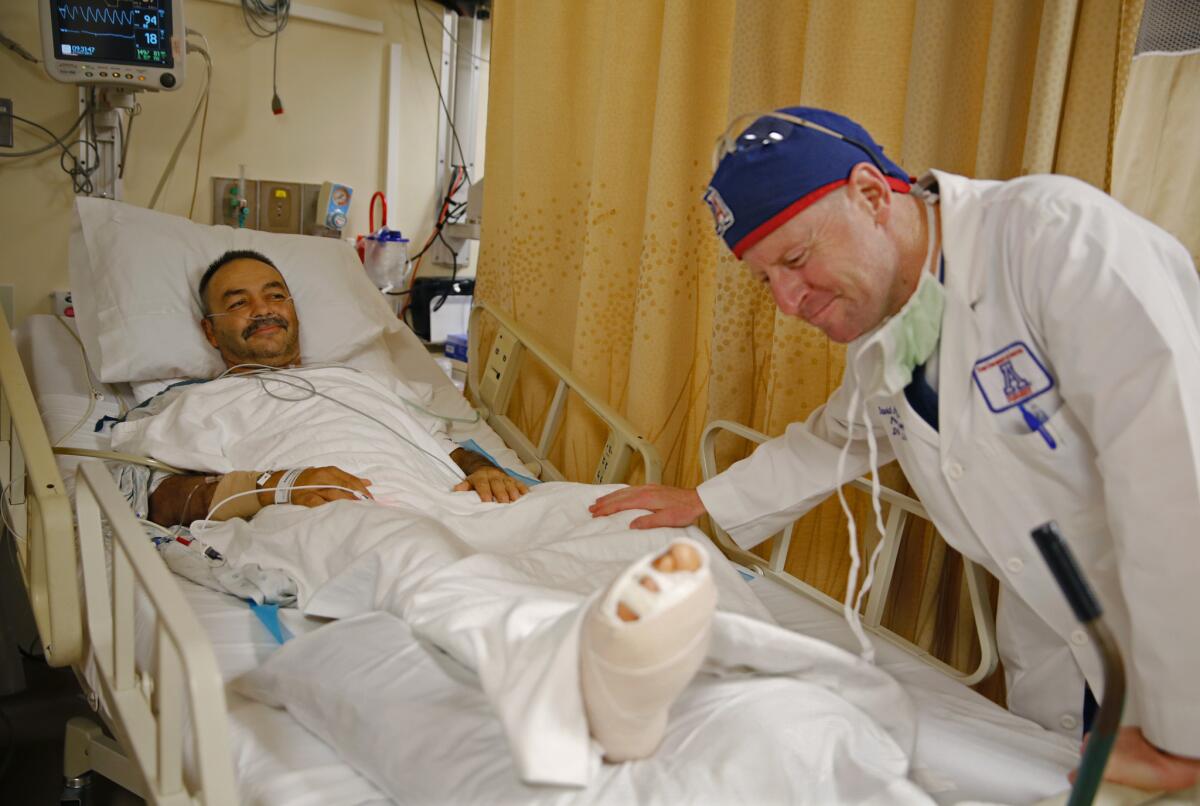
Dr. David Armstrong reassures Jesus Duarte that his foot surgery went well at the University of Arizona Medical Center. Arizona is among 30 states that have expanded their Medicaid programs under the Affordable Care Act.
- Share via
Reporting from Washington — States’ Medicaid expansions through the Affordable Care Act are helping low-income patients access medical care and improving hospitals’ bottom lines, according to two new studies that add to growing evidence about the benefits of the health law.
Fewer low-income residents of Kentucky and Arkansas, two poor states that expanded Medicaid in 2014, reported problems paying medical bills after the coverage expansions, especially compared with residents of Texas, which has rejected the health law.
And hospitals in Medicaid expansion states saw a marked decline in the share of patients without insurance compared with hospitals in states that have not broadened access to Medicaid, a second study found.
“Our findings underscore the significant benefits of Medicaid expansion not only for low-income adults, but also for the hospitals that serve this population,” the authors of that study conclude.
The two studies, both published Tuesday in the journal Health Affairs, come as new states consider Medicaid expansion, a key pillar of the healthcare law that President Obama signed in 2010.
To date, 30 states and the District of Columbia have elected to take federal aid to broaden eligibility for Medicaid to low-income, working-age adults. (The program traditionally limited coverage to vulnerable populations such as poor children, seniors and the disabled.)
Several more traditionally conservative states, including Louisiana, South Dakota and Wyoming, are looking into expanding.
But many Republican governors and state legislators continue to reject Medicaid expansion, arguing that the program is ineffective and unaffordable.
Meanwhile, in Washington, congressional Republicans for the first time have passed a bill to repeal most of Obamacare, which the president vetoed Friday.
GOP resistance to Obamacare is already affecting low-income residents, the new studies suggest.
In Texas, for example, the percentage of residents reporting trouble paying medical bills, skipping prescriptions or delaying care because of cost barely moved between 2013 and 2014.
By comparison, Kentucky and Arkansas saw major declines in all three measures of access to medical care after the Medicaid expansion began in 2014.
The share of residents in the two states who reported skipping a medication because of cost fell more than 10 percentage points. And the percentage of Kentucky residents who said they had trouble paying medical bills dropped by more than 14 percentage points, from 42.7% to 28.4%.
Researchers also found major gains in the share of residents who said they had a checkup in the prior year, which increased more than 8 percentage points in both Kentucky and Arkansas.
And they found sizable increases in the percentage of patients with chronic medical conditions who got regular care, which increased more than 6 percentage points in the two states.
Texas, by contrast, saw a decline in the percentage of chronically ill residents who got regular care between 2013 and 2014, according to the study, which was based on a telephone survey of 5,665 low-income, working-age adults in the three states.
Researchers at Harvard chose the states in part because the three have historically had high uninsured rates and because Kentucky and Arkansas chose different models of Medicaid expansion.
Kentucky took a more traditional approach, enrolling poor adults in a standard government Medicaid plan. Arkansas set up a new system that allows Medicaid enrollees to select a subsidized commercial health plan.
The Arkansas system, which was approved by Republican lawmakers in the state, has been held up as a potential conservative alternative to traditional Medicaid.
The researchers found little difference in the impact of the two expansions.
“Deciding whether or not to expand matters much more than deciding how to expand,” the study concluded. “Both Arkansas’ private option and Kentucky’s traditional Medicaid expansion appear to be promising approaches that have thus far generated similar improvements in access care.”
The researchers found less evidence that the improved access was delivering better health, as residents’ self-reported health changed little in all three states.
Dr. Benjamin Sommers, one of the study’s authors, said he hoped researchers would be able to dig into the health effects of the coverage expansions further as more data become available.
noam.levey@latimes.com
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.














