Obamacare 101: Are health insurance marketplaces in a death spiral?
- Share via
Washington — It’s been a rocky few months for the health insurance marketplaces created by the Affordable Care Act.
Even if you’re not one of the roughly 11 million Americans who rely on these online exchanges to get your health insurance, you’ve probably seen the headlines about rising premiums and insurance companies pulling out of the system.
Last week, national insurance giant Humana announced it would stop selling plans on the marketplace. Aetna’s chief executive claimed the marketplaces are in a “death spiral.” Republicans say the marketplaces are Exhibit A that Obamacare is collapsing.
So what’s the real story? Are these things really kaput or can they be fixed? Here’s a rundown of where things stand.
How do marketplaces work?
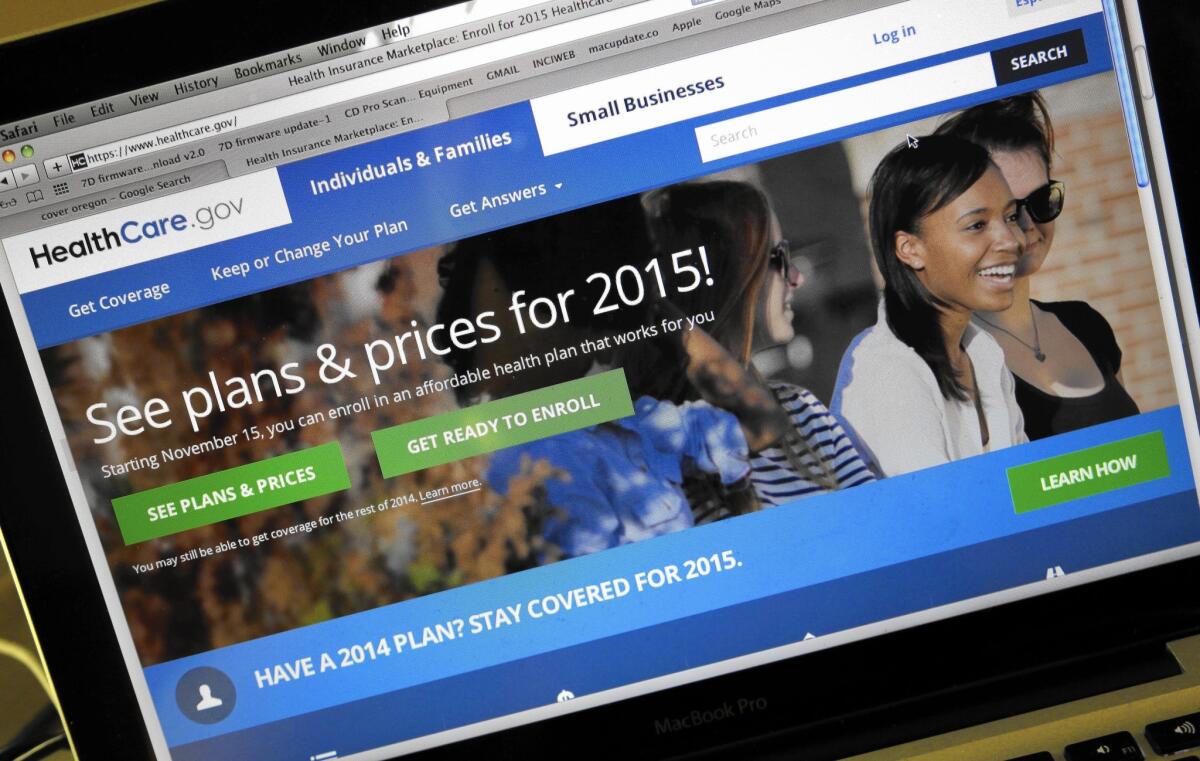
Buying health insurance on the marketplaces was set up to be like shopping online for a hotel room. The Obamacare marketplaces, such as HealthCare.gov, allow people who don’t get health benefits at work to compare a variety of competing plans that all have to offer a basic set of benefits.
Low- and moderate-income consumers — currently about 80% of the 11 million Obamacare enrolees — get federal subsidies to help pay their monthly premiums. And the plans are prohibited from turning away customers who are sick.
This was a big deal. Before Obamacare, insurance companies were free to reject sick people. And even customers who could get a plan often found it didn’t cover what they thought because health plans didn’t have to meet the same standards they now must.
What went wrong?
Like all insurance markets, the Obamacare marketplaces rely on having a good mix of customers. Younger, healthier people, who typically have lower medical costs, offset the higher cost of older, sicker people.
Unfortunately, many insurers discovered that the people who were signing up were sicker and more costly than they expected. That meant some insurers were losing money. Nobody likes that.
Insurers basically had two ways to deal with this. They could raise premiums. Or they could bail on the marketplaces.
There’s been a little of both over the past year. In some states, average 2017 premiums shot up more than 50%, though premium increases were more modest in other places.
Some insurers — like Humana, Aetna and UnitedHealthcare, all of whom are for-profit companies that have to answer to shareholders — pulled out of marketplaces altogether.
That’s created a lot of angry customers in some parts of the country.
So are the marketplaces going to collapse?
Probably not.
In a traditional “death spiral,” younger, healthier customers flee as premiums rise. That leaves behind sicker people, who are willing to pay higher premiums to keep coverage they need. Because the remaining customers have high medical costs, premiums tend to rise further, pushing away even more customers until the cycle destroys the market.
To date, there is little evidence this is happening. Enrollment on the marketplaces this year has remained relatively steady, even with the premium hikes.
Nonetheless, the departure of insurers has left consumers in some parts of the country with few options to choose from. In a handful of places, there may be no insurer next year unless something changes.
Many industry officials and independent experts believe that the marketplaces need some fixing.
What would it take to fix the marketplaces?
Everyone agrees that the key is attracting more young, healthy people into the market.
Insurers say too many people are gaming the system by signing up only when they are sick. The industry wants tighter restrictions on when consumers can enroll in coverage on the marketplaces. The Trump administration just gave the industry some of what it wanted by limiting when people could sign up.
Insurers also say they could make health plans cheaper and more attractive to younger people if they could charge those people less, though that might mean charging older customers more. That, of course, doesn’t sit well with groups like AARP.
Others say that offering consumers more financial assistance to pay their premiums would help, though that would naturally cost the government more money.
What do Republicans want to do?
We don’t really know yet.
Many GOP lawmakers are talking about completely overhauling the way Americans who use the marketplaces get coverage.
Instead of making insurers all meet basic standards, for example, Republicans would let states set their own standards. That means that insurers in some places might no longer have to offer the same sets of benefits.
As importantly, many GOP plans would also replace the way that marketplace consumers get financial assistance with their premiums.
The Obamacare subsidies are linked both to consumers’ incomes and to how much health plans cost in their states.
Republicans are talking about linking the value of the subsidy to age, with older consumers getting more financial assistance than younger consumers.
Will that work?
It’s difficult to say since Republicans haven’t offered many details about their plans. What’s important to understand is that everything involves tradeoffs.
Reducing requirements on which benefits insurers must offer, for example, might allow more plans with limited benefits. Those could be cheaper.
But they might also leave consumers without vital protections they need. That was common before Obamacare, when insurers routinely sold policies that limited treatment of some conditions or excluded some benefits, such as prescription drugs.
Similarly, a new system of financial aid that is based only on a consumer’s age would be much simpler than the current system.
But it also would mean that young people with low incomes might have a hard time affording a health plan. That would deprive insurance markets of the healthy enrollees they most need.
Editor’s Note: Obamacare 101 is a periodic primer on the debate over repealing and replacing the Affordable Care Act
ALSO
Molina Healthcare stock dives on ‘clearly unacceptable’ earnings
More to Read
Get the L.A. Times Politics newsletter
Deeply reported insights into legislation, politics and policy from Sacramento, Washington and beyond. In your inbox twice per week.
You may occasionally receive promotional content from the Los Angeles Times.











