Coronavirus Today: The front-line workers turning down the vaccine
- Share via
Good evening. I’m Amina Khan, and it’s Tuesday, Jan. 5. Here’s what’s happening with the coronavirus in California and beyond.
Firefighters in Los Angeles have been serving on the front lines of the pandemic, and they’re regularly exposed to the coronavirus — especially those who work as paramedics and emergency medical technicians. More than 670 city firefighters have tested positive for infections so far, a dozen have been hospitalized and two have died. So it makes sense that firefighters were the first city workers to get access to the COVID-19 vaccine.
Yet some are turning the doses down. “The Fire Department is a reflection of society,” Los Angeles Fire Department Chief Ralph M. Terrazas said. “There are some people who are reluctant because of fear of the unknown.” In case protection from a deadly virus isn’t enough of an incentive, firefighters who get their shots are being offered a chance to win some tempting prizes, including an Airbnb gift card, a home security system and a bicycle.
L.A.’s bravest aren’t the only front-line workers who have been turning down their chance at a potentially lifesaving vaccine. Some healthcare workers in hospitals and care facilities are also refusing to roll up their sleeves. Around 20% to 40% of L.A. County’s front-line medical workers who were offered the vaccine have turned it down. So have roughly half of their counterparts in Riverside County.
Public health officials have worried about vaccine skepticism in the general population. They were not expecting to run into these doubts among healthcare workers, assuming hospital staff would have a clear understanding of the strong scientific data backing the vaccines. But a recent survey by the Kaiser Family Foundation found that 29% of healthcare workers were “vaccine hesitant” — slightly higher than the general population’s rate of 27%.
For the record, the evidence regarding the vaccines’ safety and efficacy is clear, and it comes from advanced clinical trials involving tens of thousands of participants, including the elderly and people with chronic health conditions. The shots are recommended for all adults except those who have had a severe allergic reaction to any of the ingredients.
But skepticism remains, and the reasons may sound familiar: Vaccine-hesitant health workers said they worried about side effects; they didn’t trust the government to ensure the vaccines were safe; they had concerns about the role of politics in the development of the vaccines; or they believed the dangers of COVID-19 had been exaggerated.
Some front-line workers, like the rest of us, may have fallen victim to misinformation about the vaccine. It’s also possible that the undermining of science at the highest levels of government has made some people reluctant to take advantage of their vaccine priority status. And as I’ve written in this newsletter before, vaccine hesitancy has been especially prevalent among Black Californians, who have long faced racism in healthcare and have reason to distrust that system.
“Even the name, Operation Warp Speed, draws some concern for people about the rush to push it through,” said Dr. Medell Briggs-Malonson, an emergency medicine physician at UCLA Health who has received the vaccine. (In case you’re wondering, the speedy development was largely thanks to a decade of behind-the-scenes research that was already in the works before the pandemic hit.)
“It’s certainly disappointing,” added Sal Rosselli, the president of the National Union of Healthcare Workers. “But it’s not shocking, given what the federal administration has done over the past 10 months. ... Trust science. It’s about science, and reality, and what’s right.”
For their part, officials in California are trying to address these doubts and encourage health workers to step forward. Many hospitals are using instructional videos and interactive webinars that show staff getting vaccinated. At one Orange County hospital, intensive care nurse Anthony Wilkinson made a Facebook video about the science behind the vaccine and updated friends and family on his progress after receiving it.
“People are scared for me,” he said. “I can understand why. It’s new, and no one wants to be the first.”
Personally, I wonder if there is a silver lining here. As public health authorities reach out to these skeptical front-line workers, perhaps they’ll discover some effective ways to win over doubters in the general population.
They’re going to need all the guidance they can get: According to a report last month in the Journal of the American Medical Assn., the share of U.S. adults who said they were “somewhat” or “very” likely to get a COVID-19 vaccine dropped from 74.1% in early April to just 56.2% in late November and early December.
That could be a huge problem, as experts say that perhaps 85% of the population needs to be vaccinated in order to achieve herd immunity, which would offer some protection for the vulnerable among us who simply aren’t able to get the vaccine. And it’s a challenge that extends beyond our national borders: In the first six days of the European Union’s coordinated vaccination campaign, France gave the shot to just 516 people — such a low number in a population of 67 million that it’s statistically indistinguishable from zero.
For his part, L.A. Fire Chief Terrazas said he would consider making the shot mandatory after COVID-19 vaccines become available for broader use. But for now, he’s making personal appeals to firefighters, even getting his first dose alongside union leaders in a videotaped event to be distributed this week. Leading by example is a tactic that many health authorities will likely bank on.
By the numbers
California cases, deaths and vaccinations as of 4:36 p.m. PST Tuesday:
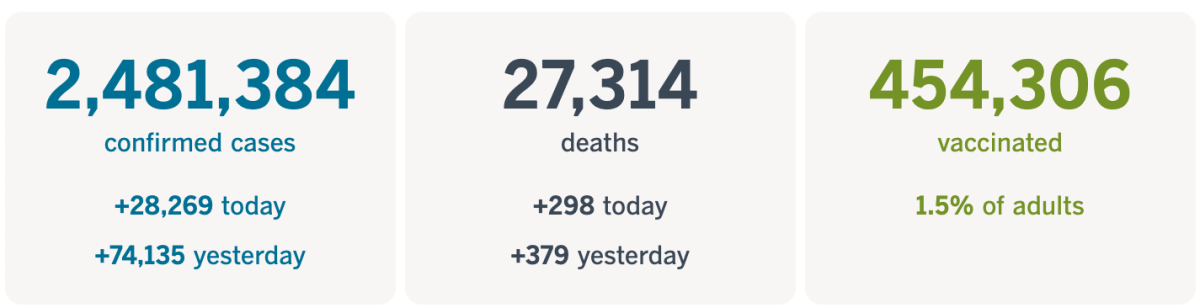
Track the latest numbers and how they break down in California with our graphics.
Across California
The risk of becoming infected by the coronavirus in Los Angeles County has never been higher — about one in every five people getting tested for it is positive. That’s five times the positivity rate on Nov. 1. Over the last week, the county has been averaging 184 COVID-19 deaths per day — the equivalent of one every eight minutes. And things are almost certain to get worse as people who were infected during the holidays get sick and spread the virus to others.
“Everyone should keep in mind that community transmission rates are so high that you run the risk of an exposure whenever you leave your home,” Los Angeles County Public Health Director Barbara Ferrer said. “Assume that this deadly invisible virus is everywhere, looking for a willing host.”
L.A. County and the rest of Southern California are still under a stay-at-home order that was extended last week. But because things are so bad, officials are offering more specific suggestions:
Never remove your face mask when you’re near others. Avoid eating or drinking with anyone who’s not in your household. Wash or sanitize your hands every hour if you’re around others. Take a break from shopping. Don’t gather with anyone outside your household. Exercise by yourself or only with others from your household.
Los Angeles County has now logged 11,000 COVID-19 deaths over the course of the pandemic, and more than 1,000 of those deaths have occurred just within the last week — a sign of just how brutal the current surge has been. More lives are sure to be lost as some of those infected in the post-Christmas surge start to fall seriously ill.
The unrelenting violence of this surge is no secret to L.A.’s medical system, as healthcare providers run low on ventilators, dialysis machines and other essential medical equipment. At Harbor-UCLA Medical Center near Torrance, the ICU is running at 150% of its normal capacity. Two refrigerated trucks are parked out back because the morgue keeps running out of space for bodies.
“We are basically overrun with critically ill patients. ... It’s extraordinarily difficult,” said Dr. Anish Mahajan, the chief medical officer. “People are exhausted.” The hospital is expecting some staffing help on Thursday; the U.S. Department of Defense is sending six combat medics, three respiratory therapists and 11 nurses to help with the influx of patients for at least the next 30 days. More staff will go to L.A. County-USC Medical Center on the Eastside.
The dire situation in Los Angeles helped California set yet another record Monday for new coronavirus cases in a single day, with more than 74,000 cases statewide, a Times tally shows. That far outstrips the previous record of 66,726 logged on Dec. 28. The state is now averaging about 37,000 new cases per day over the last week. While that’s down from a high of about 45,000 in mid-December, it’s still far worse than the beginning of December, when 14,000 cases per day were coming in.
Over the past week, California has averaged roughly 96 new daily cases per 100,000 residents. That puts us in a tie with Rhode Island for the second-highest rate among all states, trailing only Arizona’s 112, according to data from the Centers for Disease Control and Prevention. The nationwide daily average over the past week has been far lower — about 64 per 100,000 people.
Monday also brought 379 deaths, marking California’s sixth-highest daily death toll.
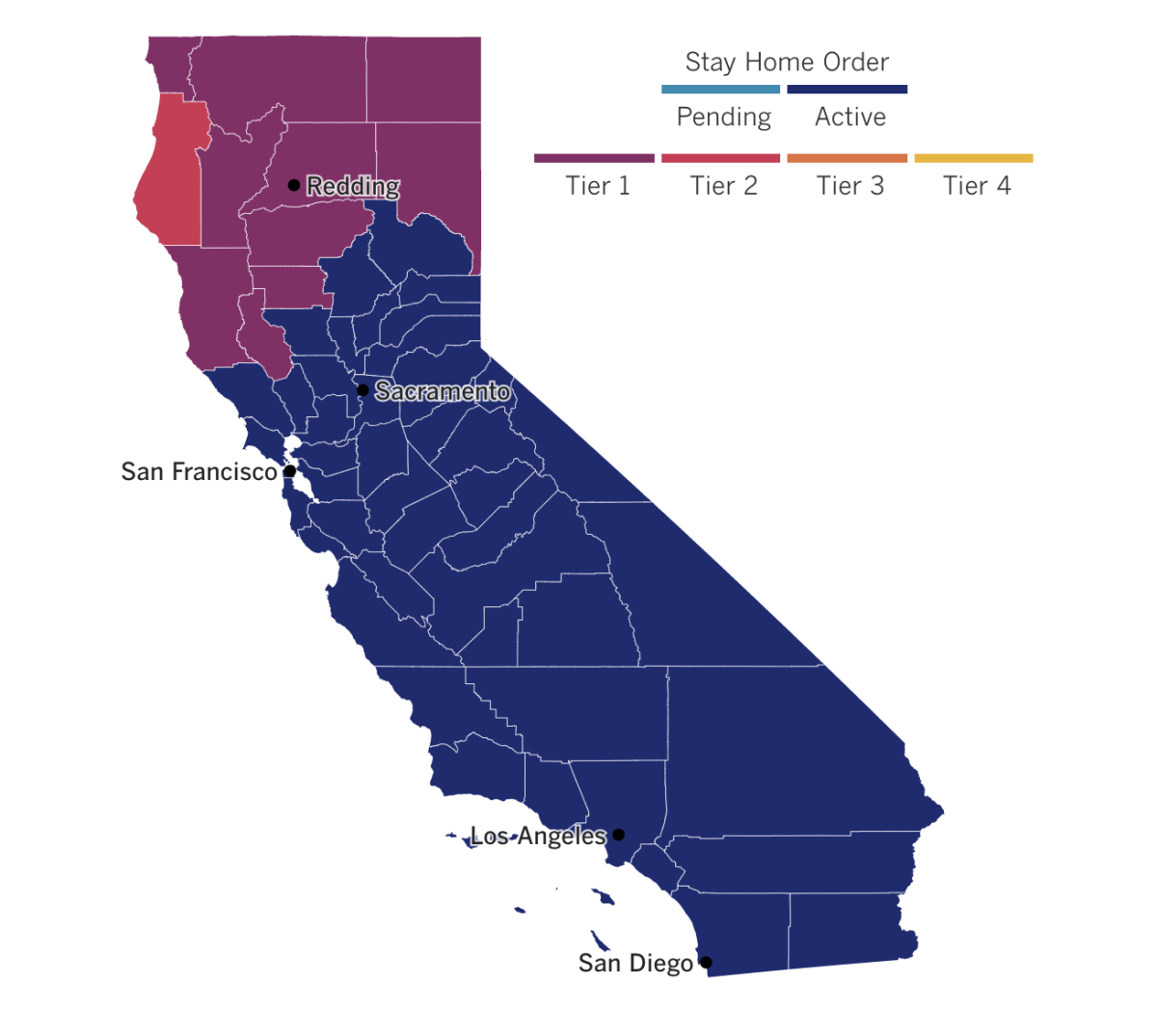
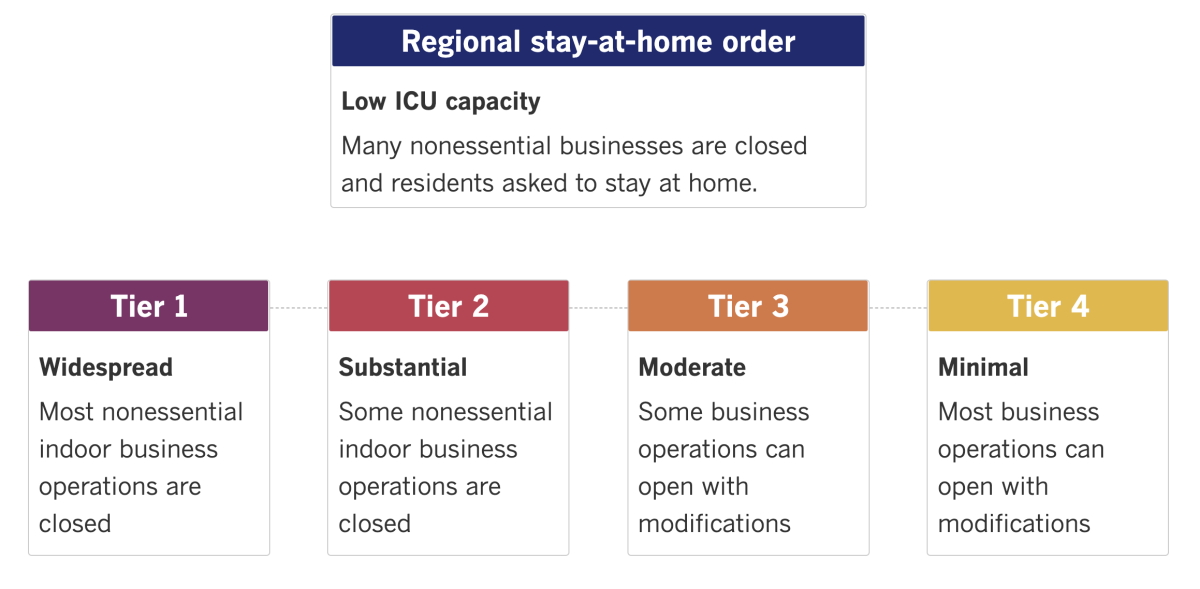
See the latest on California’s coronavirus closures and reopenings, and the metrics that inform them, with our tracker.
Consider subscribing to the Los Angeles Times
Your support helps us deliver the news that matters most. Become a subscriber.
Around the nation and the world
The dangers of vaccine misinformation seem to have come to a head in this story of a Wisconsin pharmacist who intentionally spoiled hundreds of doses of COVID-19 vaccine. Steven Brandenburg ruined 57 vials of the Moderna vaccine, which contained enough doses to inoculate more than 500 people, because he wrongly believed the shots would alter people’s DNA, according to court documents released Monday.
“He’d formed this belief they were unsafe,” Ozaukee County District Attorney Adam Gerol said during a virtual hearing.
Brandenburg, an admitted conspiracy theorist, reportedly said that he deliberately removed the vials from refrigeration at the Grafton medical center where he worked, left them out overnight on Christmas Eve, returned them, then left them out again overnight on Christmas. A pharmacy technician discovered the vials outside on Dec. 26. Police said the likely ruined doses were worth between $8,000 and $11,000 — though Gerol said the doses will have to be tested to make sure they’re ineffective before charges can be filed.
In Germany, Chancellor Angela Merkel said Tuesday that she has agreed with state governors to extend the country’s current lockdown by three weeks, until Jan. 31. Merkel said they will also tighten curbs on social contacts, as they did back in March during the pandemic’s early days. With new cases and deaths remaining high and showing no sign of coming down, the leaders also called for restrictions on movement for residents of areas with very high infection rates.
The good news in Germany: The nation of 83 million had logged close to 265,000 vaccinations less than 10 days after the European Union started rolling out the Pfizer-BioNTech doses in its 27-nation bloc. But in a nod to heavy pressure due to the campaign’s slow start, Health Minister Jens Spahn said he’s asked if the second shot of the vaccine could be delayed in order quickly to vaccinate more people with a first dose. While Britain has taken this route with its vaccine rollout, the move is triggering fierce debate among scientists and governments around the globe.
In Singapore, a government minister told lawmakers that the data collected by the city-state’s contact-tracing program could be used for criminal investigations in spite of earlier assurances that this would not happen. Participation in the program is technically voluntary, but officials have threatened social penalties for those who don’t opt in. So far, 78% of residents — 4.2 million people — have signed up.
It’s exactly the kind of scenario that’s sown distrust in government and made it very difficult for public officials around the world to perform the kind of contact tracing necessary to track the disease and curb its spread. In Singapore, the move has sparked a backlash on social media and set off alarms for rights advocates. The one-party-ruled state has little tolerance for criticism, my colleague David Pierson writes.
“Singapore’s betrayal of its solemn promises to limit use of TraceTogether information to public health matters exposes how the government has been covertly exploiting the pandemic to deepen its surveillance and control over the population, and undermine the right to privacy,” Phil Robertson, deputy Asia director for Human Rights Watch, said in a statement.
Desmond Tan, Singapore’s minister of state for home affairs, said any TraceTogether data needed for criminal investigations could be accessed only by “authorized officers” and that any misuse of the information could result in a $3,800 fine and/or up to two years in prison.
Your questions answered
Today’s question comes from readers who want to know: How worried should we be about the new coronavirus variant from the United Kingdom?
By now you’ve heard about the new, potentially more contagious variant of coronavirus that was discovered in England before Christmas. Now the virus has made its way to the United States, with at least a half dozen known cases in California. Some experts say there’s not yet any cause for alarm — and several of my colleagues have put together a guide on what we know about the variant at this point.
First off, the emergence of a variant like this is no surprise, said Dr. Anthony Fauci, the nation’s top infectious-disease expert. Mutations in the virus’s genome are to be expected, he said, since “the more you replicate, the more you mutate. So, when you have a lot of virus that’s circulating in the community, it means it’s infecting a lot of people; it’s replicating a lot.”
Fauci said the “overwhelming majority of mutations are irrelevant,” but “every once in a while, you get a mutation that does impact a function of the virus.”
In this case, he said, it appears that some of the changes make the virus better at jumping from one person to another. But other scientists have been more skeptical that genetic changes in the strain, called B.1.1.7, really do make it more contagious, and are waiting for more evidence.
Either way, “there’s no indication at all that it increases the virulence … the ability to make you sick or kill you,” Fauci said of the variant. Existing vaccines also appear to remain effective against it, he added.
We want to hear from you. Email us your coronavirus questions, and we’ll do our best to answer them.
Resources
Practice social distancing using these tips, and wear a mask. Here’s how to do it right.
Watch for symptoms such as fever, cough, shortness of breath, chills, shaking with chills, muscle pain, headache, sore throat and loss of taste or smell. Here’s what to look for and when.
Need to get tested? Here’s where you can in L.A. County and around California.
Americans are hurting in many ways. We have advice for helping kids cope, resources for people experiencing domestic abuse and a newsletter to help you make ends meet.
For our most up-to-date coverage, visit our homepage and our Health section, get our breaking news alerts, and follow us on Twitter and Instagram.




