COVID-19 lung patterns show few clues for treating pneumonia
- Share via
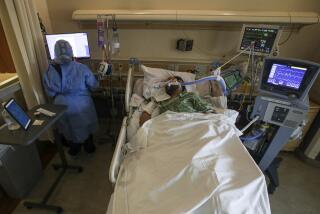
Scans of the lungs of the sickest COVID-19 patients show distinctive patterns of infection, but so far those clues are offering little help in predicting which patients will pull through.
For now, doctors are relying on what’s called supportive care, which is standard for treating patients with severe pneumonia.
Doctors in areas still bracing for an onslaught of sick patients are scouring medical reports and hosting webinars with Chinese doctors to get the best advice on what has and hasn’t worked.
One thing that’s clear around the globe: Age makes a huge difference in survival. And one reason is that seniors’ lungs don’t have as much of what geriatrics expert Dr. Richard Baron calls reserve capacity.
“At age 18, you have a lot of extra lung capacity you don’t use unless you’re running a marathon,” said Baron, who heads the American Board of Internal Medicine. That capacity gradually declines with age even in otherwise healthy people, so “if you’re an old person, even a mild form can overwhelm your lungs if you don’t have enough reserve.”
Here’s what scientists can say so far about treating those who become severely ill.
How does COVID-19 harm the lungs?
The new coronavirus, like most respiratory viruses, is spread by droplets from someone’s cough or sneeze. The vast majority of patients recover, most after experiencing mild or moderate symptoms such as fever and cough. But sometimes the virus makes its way deep into the lungs and causes pneumonia.
Lungs contain grapelike clusters of tiny air sacs called alveoli. When you breathe, oxygen fills the sacs and passes straight into blood vessels that nestle alongside them. Pneumonia occurs when an infection — of any sort, not just this new virus — inflames the alveoli. In severe cases they fill with fluid, dead cells and other debris, preventing oxygen from getting through.
If other countries have the same experience as China, about 5% of COVID-19 patients could become sick enough to require intensive care.
How does that lung damage appear?
Doctors at New York’s Mount Sinai Health System analyzed 121 chest CT scans shared by colleagues in China, and they spotted something unusual.
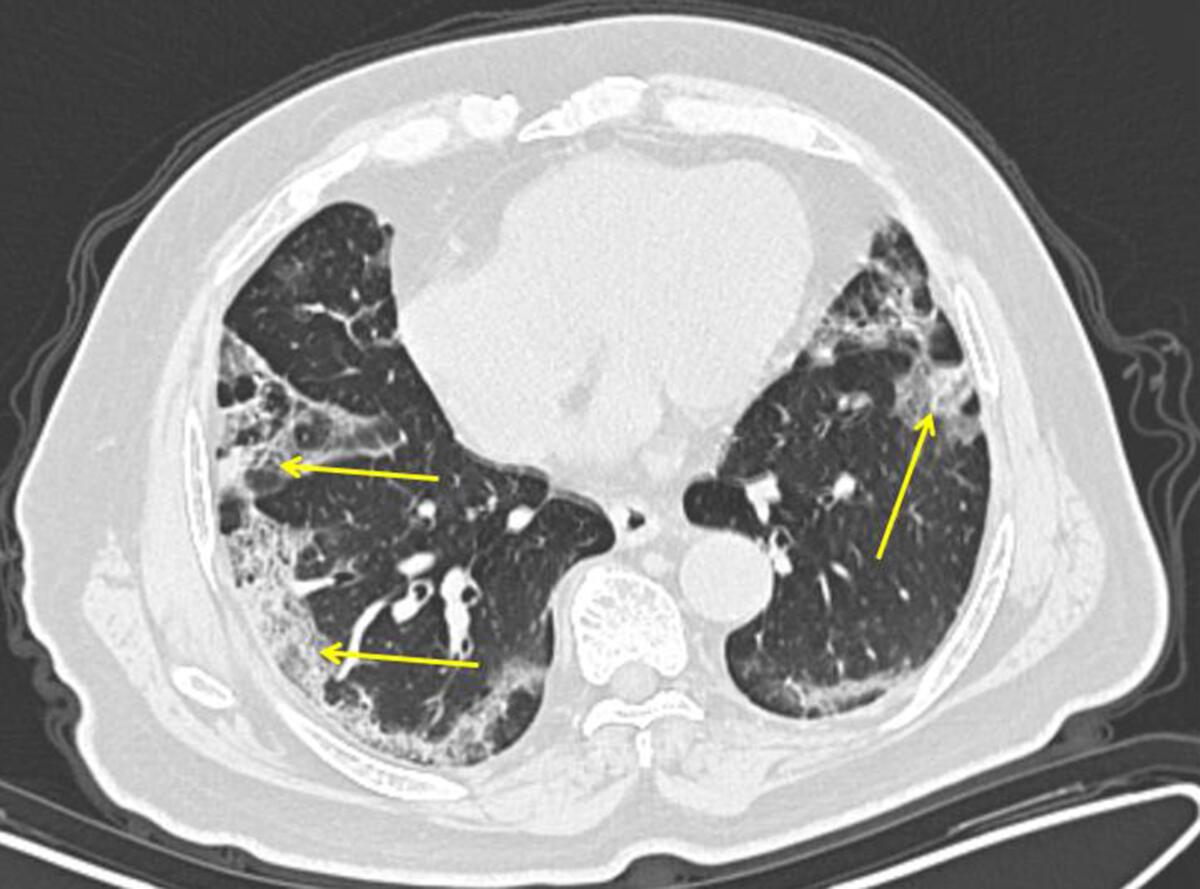
Healthy lungs look mostly black on medical scans because they’re full of air. An early infection with bacterial pneumonia tends to show up as a white blotch in one section of one lung. Pneumonia caused by a virus can show up as hazy patches that doctors call “ground glass opacities.”
In people who get COVID-19 pneumonia, that haze tends to cluster on the outside edge of both lungs, by the ribs. It’s a distinctive pattern, said Dr. Adam Bernheim, a radiologist at Mount Sinai.
As infection worsens, the haze forms rounder clusters and gradually turns more white as the air sacs become increasingly clogged.
How do doctors treat that pneumonia?
So far, there are no drugs that directly attack the new coronavirus, although doctors are trying some experimentally, including an old malaria treatment and one under development to treat Ebola.
“The best treatment we have is supportive care,” said Dr. Aimee Moulin, an emergency care physician at UC Davis Medical Center.
That centers around helping patients breathe when the oxygen levels in their blood start to drop. For some people, oxygen delivered through a mask or tubes in the nose is enough. More severely ill patients will need a breathing machine.
“The goal is to keep the person alive until the disease takes its course” and the lungs begin to heal, said Dr. Neil Schachter, a pulmonary and critical care specialist at Mount Sinai.
The very worst cases develop an inflammatory condition called ARDS — acute respiratory distress syndrome — that floods the lungs with fluid. That’s when the immune system’s attempt to fight infection “is going crazy and itself attacking the lung,” Baron explained.
Many things besides the coronavirus can cause the condition. Regardless of the cause, it comes with a high risk of death.
What else is affected?
Severe pneumonia of any sort can cause shock and other organ damage. But in a webinar last week, Chinese doctors told members of the American College of Cardiology to watch for some additional problems in severe COVID-19, especially in people with heart disease. The worst off may need blood thinners as their blood starts to abnormally clot, and the heart itself may sustain damage not just from lack of oxygen but from the inflammation engulfing the body.
Another caution: The sickest patients can deteriorate rapidly, something a hospital in Kirkland, Wa., witnessed.
Of 21 patients who needed critical care at Evergreen Hospital, 17 were moved into the ICU within 24 hours of hospital admission, doctors reported last week in the Journal of the American Medical Assn.
Age isn’t the only risk factor. Data from China show that regardless of age, 40% of people who required critical care had other chronic health problems, such as heart disease and diabetes.
Does COVID-19 leave lasting lung damage?
It’s too soon to know. The World Health Organization has said that it can take three to six weeks to recover from a severe case of COVID-19.
But it can take months to get back to normal activity after any form of severe pneumonia, particularly if the person had earlier health problems. Recovery in part depends on how long someone was on a breathing machine.
“If you’re on a ventilator for four weeks in deep sleep in an intensive care unit, it takes six months to a year to rehabilitate,” Dr. Diederik Gommers of the Netherlands Assn. for Intensive Care told Dutch lawmakers. “It is very debilitating if you are in intensive care for so long.”