Clinical trial of remdesivir may be a turning point in coronavirus fight
- Share via
In the first clear signal that a drug can effectively treat those sickened by the coronavirus, government researchers reported Wednesday that the antiviral medication remdesivir helped patients with advanced COVID-19 recover more quickly than a placebo treatment.
The early results, emerging from a large clinical trial sponsored by the National Institute of Allergy and Infectious Diseases, appears to position the drug as the standard therapy for hospitalized COVID-19 patients going forward.
In the trial, patients who received remdesivir recovered 31% faster than those who received a placebo, a finding of superiority that could not be attributed to chance, researchers reported. Specifically, half of the patients who were randomly selected to be treated with remdesivir were considered completely recovered within 11 days, and half of those patients took longer. By comparison, it took 15 days or less for half of those who received the placebo to recover.
The results also suggested that patients who were given remdesivir were more likely to survive COVID-19 than were those who got the placebo. But the difference in fatality rates — 8% for the group that took the drug versus 11.6% for the placebo group — fell slightly below the cutoff point at which researchers could rule out a statistical fluke.
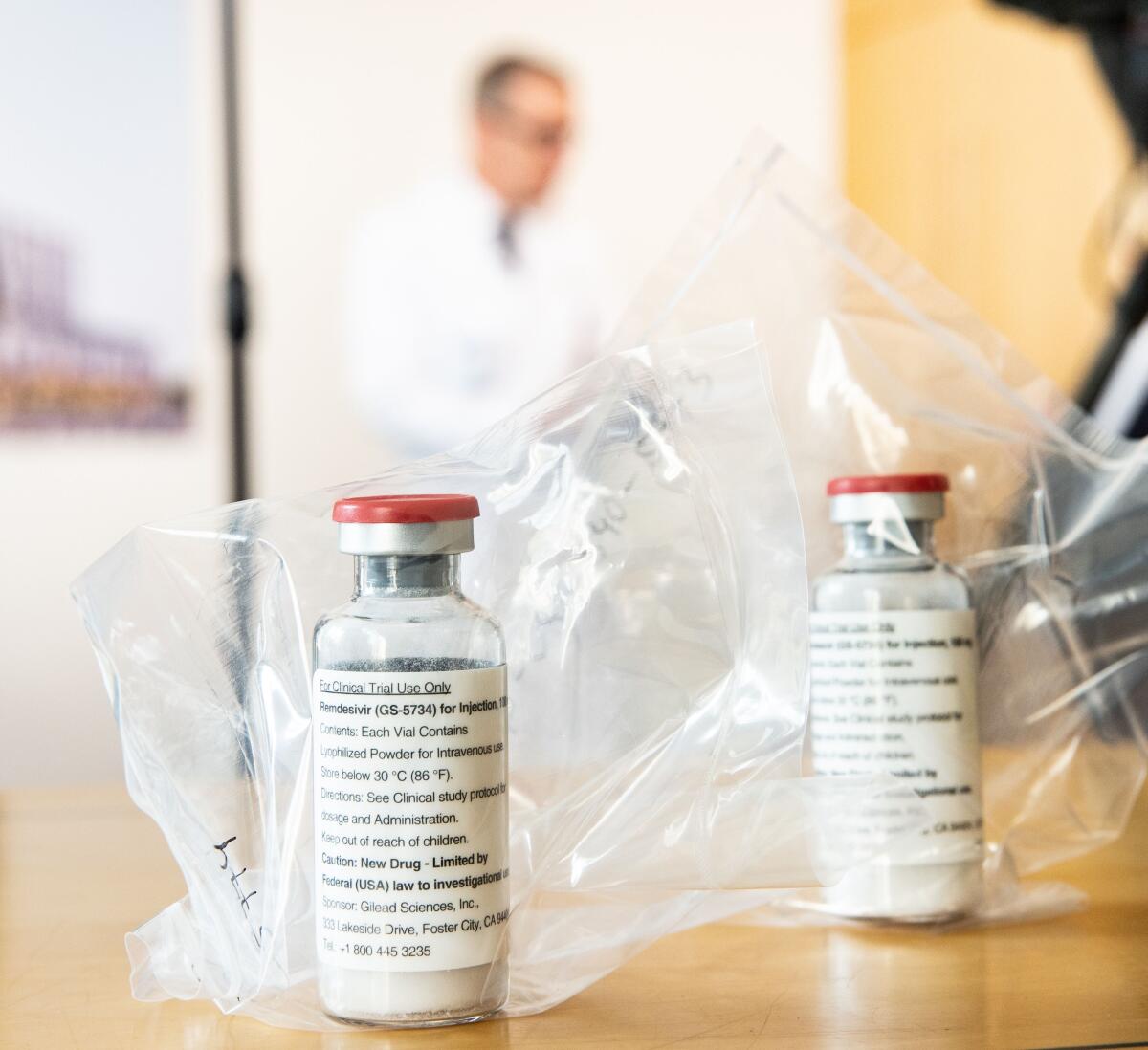
Remdesivir was originally designed by California-based Gilead Sciences Inc. as a drug to treat Ebola disease. But since it was less effective than other medications for that use, the experimental drug never entered full-scale production.
Dr. Anthony Fauci, who leads the National Institute of Allergy and Infectious Diseases, hailed the new findings as a “really quite important” milestone in the scramble to find any effective treatment for a pandemic that has claimed more than 227,000 lives around the world, including more than 60,000 in the United States.
“What [the clinical trial] has proven is that a drug can block this virus,” Fauci said Wednesday in the Oval Office of the White House. “This drug happens to be blocking an enzyme that the virus uses.”
Indeed, the benefits were so clear that an independent review board opted to halt this portion of the trial early. As researchers move on to investigate the efficacy of other drugs against COVID-19, researchers will give all trial participants remdesivir and will make the antiviral the new standard against which other drugs are compared, Fauci said.
“Whenever you have clear-cut evidence that a drug works,” he explained, “you have an ethical obligation to immediately let the people who are in the placebo group know so that they could have access.”
Fauci added that after the data have been analyzed more completely, “some of the numbers may change a little, but the conclusion will not change.”
Full results will be submitted for publication in a peer-reviewed medical journal, he said.
Fauci, who took the helm of NIAID in 1984, likened the new findings to the 1986 discovery that the anti-retroviral drug azidothymidine, or AZT, could suppress the HIV virus in patients with AIDS. That drug, which became known as Retrovir, marked the beginning of a turnaround that, over the course of a decade, transformed HIV infection from a death sentence into a manageable chronic health condition.
The coronavirus outbreak has put science on hold. Now there are discoveries that may never be made and patients who will miss the chance at a breakthrough cure.
On Wednesday, Fauci suggested the remdesivir results could “open the door” to studies that would pair the drug with other medications or new antivirals, just as the AZT find paved the way for combination therapies for HIV.
“All of the other trials that are taking place now have a new standard of care,” he said.
The U.S. Food and Drug Administration has been working with Gilead Sciences to make remdesivir available to patients as quickly as possible, NIAID officials added.
Despite Fauci’s enthusiasm, it will probably take a while for redemsivir to become widely used in clinical trials or in the routine care of hospitalized patients, said Dr. Mark McClellan, who served as FDA commissioner under President George W. Bush. Like ventilators and personal protective gear, remdesivir is in short supply, and until that changes, scientists can continue to flesh out the drug’s risks and benefits.
“This is progress, but we need to learn more,” said McClellan, founding director of the Duke-Margolis Center for Health Policy. “I do hope this works, but it’s not enough to pin our hat on. We’re definitely not done yet.”
The NIAID trial began on Feb. 21 and enrolled 1,063 patients across the country. The first participant was an American who became ill after traveling on the Diamond Princess cruise ship and was treated at the University of Nebraska. A total of 68 sites ultimately joined the study, including 47 in the United States and 21 in Europe and Asia.
As the coronavirus keeps us stuck at home, scientists and health officials fear that social distancing could take a toll on our mental health.
Dr. Aneesh Mehta, an infectious diseases expert at Emory University, said that the trial was limited to patients who had already developed breathing problems and that other drugs were still needed to block the coronavirus in the early stages of infection.
“It is very important to understand remdesivir and antivirals in general are not silver bullets,” said Mehta, who is leading the trial at Emory.
Separately, Gilead announced Wednesday that remdesivir appeared to be equally effective at shortening COVID-19 illness when it’s administered at half the dose currently considered necessary.
Of the 200 hospitalized patients who took the drug for five days, 60% made a full recovery and 8% died. The 197 hospitalized patients who took the drug for the usual 10 days fared marginally worse: 54% of them made a full recovery and 11% died. The difference between the two groups was judged to be statistically equivalent.
The results were seen as welcome news considering that the drug is not yet rolling off production lines in large quantities. With limited stocks now in hand, and coronavirus cases continuing to pile up, the new findings suggest the medication could go twice as far as previously thought possible.
Shares of Gilead rose $4.47 to close at $83.14 in Nasdaq trading Wednesday, a gain of more than 5%.
Coronavirus: L.A. now offering free tests to all residents, Garcetti says
The new findings are set against a backdrop of considerable uncertainty about remdesivir’s effectiveness. In addition to the NIAID trial, two other major clinical trials are now underway across the country.
All told, in close to 7,500 patients at more than 430 hospitals and care centers, the disease trajectories of patients on remdesivir are being rigorously compared with those of patients getting a range of other treatments.
The results of early studies have been promising but mixed.
In a preliminary report published this month in the New England Journal of Medicine, remdesivir appeared to reduce the risk of death in severely ill COVID-19 patients and improve the condition of those who required a range of devices for breathing assistance. Researchers reported that 68% of the patients saw their symptoms improve within 28 days and 13% died. That study, however, tracked the outcomes of just 53 patients and did not compare them with patients who did not get remdesivir.
Researchers in China who did put remdesivir head-to-head against a placebo found that the drug appeared to make no significant difference in how sick patients became or how quickly they recovered.
Their study, published Wednesday in the medical journal Lancet, was a double-blind trial in which neither patients nor the doctors treating them knew who got the drug and who got the placebo. That trial design is considered the gold standard of medical research.
The researchers, however, were only able to enroll 237 of the 453 patients they thought they would need to be able to detect a benefit with remdesivir. They drew study volunteers from 10 hospitals in Wuhan, but as outbreak conditions improved in that Chinese city, they ran out of patients to recruit.
“Considering the Lancet study didn’t meet the enrollment target, it’s hard to make a broader judgment on their findings,” Mehta said.
The NIAID trial doesn’t have that problem, he added: “We should have a wealth of data that will guide our use of remdesivir beyond the preliminary data we have today.”
Times staff writer Deborah Netburn contributed to this report.










