Coronavirus discoveries can come along faster with adaptive clinical trials

- Share via
As the medical profession scrambles to treat patients sick and dying from COVID-19, improvisation has become one of its most improbable — and important — tools. Could the same strategy be applied to coronavirus research, to suss out the best treatments for infected patients at a quicker pace?
The federal government is counting on it.
To identify the most effective COVID-19 drugs at top speed, the National Institutes of Health have embraced an approach called the adaptive clinical trial. The Adaptive COVID-19 Treatment Trial, better known to medical researchers as ACTT, has been hailed as a fast, flexible and relatively cheap way to sort through an array of drugs and provide doctors with standard treatment protocols for their patients.
ACTT is the trial that prompted Dr. Anthony Fauci to declare from the Oval Office that scientists had broken new ground in the pandemic by demonstrating that the antiviral medication remdesivir “can block this virus.” Those results created a new “standard of care” for treating COVID-19 patients, he said.
The trial marks a highly visible departure from the double-blind, placebo-controlled randomized clinical trials that have ruled medical science for most of the last four decades. Often called RCTs, they’ve allowed researchers to assess the safety and effectiveness of drugs before they reach American patients.
Though revered for their scientific purity, RCTs have come under fire from a growing number of critics who bristle at their cost, rigidity and sluggish pace. They see adaptive clinical trials as the way to make the drug testing process faster and cheaper.
Sometimes called “learn as you go” trials, they accelerate the testing process by allowing early results to dictate changes in a trial’s objectives, its participant pool and even the standards of comparison it uses. By slashing through regulatory strictures built up over decades, it has given Fauci a rare bit of common ground with President Trump.
In an RCT, patients with similar characteristics were randomly assigned to test either the experimental treatment or a placebo. To keep the evaluation as unbiased as possible, neither the study participants nor their doctors knew which people were actually getting the drug. If any differences emerged between the two groups, researchers could reliably attribute them to the treatment.
In an adaptive clinical trial, whether participants are assigned to receive an active drug or a placebo may not be decided at random. Both researchers and their study subjects are more likely to know which group the participants are in because their doses may change, or they may be shuffled from one group to another. And as new drugs like remdesivir are found to be helpful, researchers may even phase out the placebo altogether.
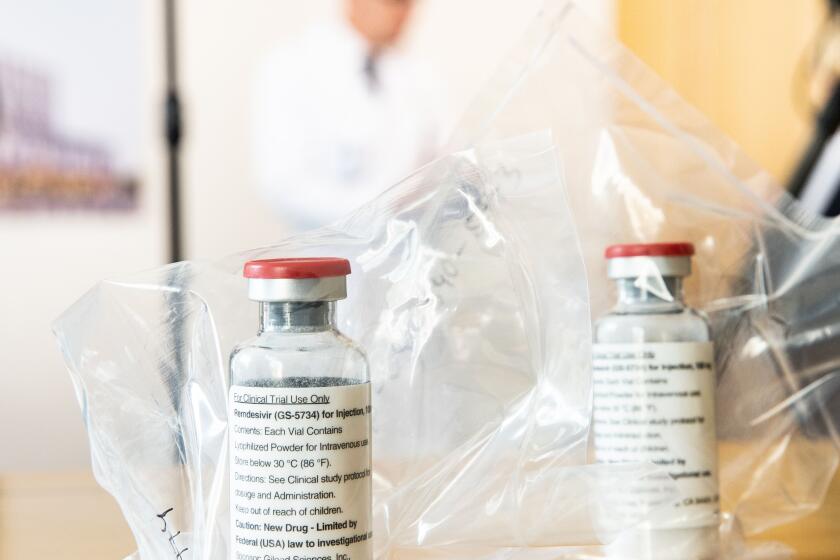
In a clinical trial, the drug remdesivir shortened recovery time for patients with advanced cases of COVID-19, the disease caused by the coronavirus.
ACTT enrolled its first subject on Feb. 25 at the University of Nebraska. The trial, sponsored by the National Institutes of Health, now has 800 participants in 39 sites across the country, and several sites abroad.
It was originally designed to test hydroxychloroquine, but after early studies cast doubt on the malaria drug’s safety and effectiveness, researchers switched to remdesivir. Over the coming months, the trial’s sponsor, the National Institute of Allergy and Infectious Diseases, is expected to enroll new COVID-19 patients and expand the number of drugs to be tested.
It took less than two months for an independent review board made up of biostatistician and drug safety experts to declare remdesivir an unequivocal, if modest, success. The 200 hospitalized patients who took the drug developed as an Ebola treatment recovered in a median of 11 days, 31% faster than the 15 days it took for the 197 patients who were randomly assigned to get the placebo.
Patients who got remdesivir were less likely to die, but the difference was so small that researchers could not rule out that the finding was the result of statistical happenstance.
The benefit was good enough to flip ACTT’s first adaptive switch. Now the rheumatoid arthritis drug baricitinib will take center stage as the experimental medication. Remdesivir will become the comparator drug, a role once played by placebo.
With that change, researchers will likely adjust their focus on measures of success. For instance, since baricitinib is thought to calm the immune system’s overreaction to coronavirus infection, differences in inflammation levels between the groups will get a close look.
If baricitinib performs well, it could join with remdesivir to serve as a new standard against which a third medication will be tried, and a panel of drug experts is already considering which drug that might be. As the treatment cocktail expands, researchers may reset the standards they use to declare a new drug beneficial.
The trial’s final accounting of remdesivir’s performance in 1,063 patients is not expected before the end of May. But ACTT’s design dictates that it is time to move on.
Stunning visualizations show what the novel coronavirus, SARS-CoV-2, looks like at an atomic level of detail.
For years before the novel coronavirus appeared in China, the idea that the U.S. drug-approval process should be faster and more flexible had been gathering momentum. One of the most prominent champions of adaptive clinical trials was Dr. Scott Gottlieb, an entrepreneur, independent healthcare analyst and former official at the Food and Drug Administration.
Gottlieb’s views appealed to Trump as a way to make good on his promise to slash regulations and cut bureaucracy, and he became the administration’s first FDA commissioner. In his nearly two years in that job, Gottlieb pressed the regulators under his command to consider adaptive clinical trials as a way to unleash innovation and get new drugs to patients more quickly.
It was not always an easy sell.
A series of drug-safety debacles in the 1960s had focused the FDA on the need for drug companies to rigorously test their products before they could be allowed on on the market. The RCT became the gold standard of scientifically rigorous research.
The rules for these gold-standard trials are strict. The number of participants needed and the criteria for enrolling them remain the same from beginning to end. The hypothesis to be tested and the outcomes to be measured are set in stone from the start. Statistical considerations dictate the number of subjects needed to draw conclusions with confidence. And a drug’s feared side effects, or an agreed-upon measure of clinical improvement, guides the length of time needed for a drug’s safety and effectiveness to become apparent.
If a drug fell short, it was pretty much game over. Researchers rarely dared to declare a new criterion for success or to focus on only a portion of subjects who seemed to have a better response. They couldn’t keep the trial going past its planned endpoint in hopes of detecting benefits still unseen.
If a drug failed to meet pre-determined measures of success, all its sponsors could do was design a new trial and start again.
The first challenge to those rules was prompted by the HIV/AIDS pandemic of the 1980s. The advocacy group ACT UP urged the agency to allow trial participants to be enrolled on demand and gain access to drugs without having to take the chance of getting the placebo. The FDA refused on the grounds that doing so would undermine the scientific validity of research results.
(A few years later, the FDA relented and created a process granting AIDS patients access to experimental drugs in an “expanded use” program that ran parallel to standard clinical trials. That program is in wide use today for drugs being used experimentally to treat COVID-19.)
Despite President Trump’s statements that the coronavirus was released from a laboratory in Wuhan, scientists say the evidence points to a natural origin.
The reason for such rigidity is to minimize the impact that researchers’ intuitions, preconceptions or motives might have on a trial’s findings, said Dr. Adams Dudley, a drug safety expert at UC San Francisco.
Drug trials are overwhelmingly funded by companies whose financial prospects depend on their outcomes, and allowing them to change the rules midstream would be an invitation to data-fudging and cherry-picking of results, Dudley said. Speeding drugs to the market based on early, skewed or serendipitous findings could result in useless — and possibly dangerous — drugs making their way to market.
“It’s all about getting the best science,” Dudley said.
At the same time, he added, “that is slow and expensive.” With thousands of people dying every day of COVID-19, the deliberate pace of this gold standard research may not be the best way to end the crisis quickly, he said.
ACTT is evidence that in a crisis, at least, flexibility in research will rule the day. As they get an early glimpse of a drug’s impact, the people running the trial have the latitude to change many key features of the trial.
That flexibility has limits. If an experimental drug appeared to work better in women, for instance, they couldn’t throw men out of the study. But they could, in principle, split off a chunk of trial participants to explore those findings.
The remdesivir results already have shown ACTT’s ability to flex. When the antiviral drug’s effectiveness became clear earlier than expected, the trial runners ended that phase of the trial early and offered it to everyone.
Likewise, when a separate trial found that COVID-19 patients getting five days of treatment did as well as those who got it for 10 days, everyone in ACTT was put on a five-day regimen.
In the process of all this shifting, the “blinding” that keep researchers and participants from knowing who is getting the experimental treatment and who is getting the placebo can sometime slip.
Dr. Andre Kalil, ACTT’s principal investigator at the University of Nebraska, acknowledged that such shifts are a departure for most clinical researchers. But these are not normal times, he said, “and we need to provide these treatments to patients.”
Moreover, with hundreds of other clinical trials of COVID-19 treatments across the country, the ACTT findings will rarely be the last word on a treatment’s safety and effectiveness. “The most important thing is to replicate” the trial’s findings, he said.
The search for existing drugs that may help treat coronavirus infections now has researchers testing the heartburn drug Pepcid, among others.
Other researchers are eager to play that role. At USC, a team led by Dr. Heinz-Josef Lenz will be testing baricitinib and remdesivir in a clinical trial with 59 COVID0-19 patients, while another group at the University of Colorado’s Anschutz Medical Campus turned on a dime to design a clinical trial of baricitinib in 80 COVID-19 patients.
“As a general principal, reproducibility in science is a central pillar,” said Dr. Joaquin Espinosa, who is leading the work in Colorado.
Neither his trial nor the one conducted at USC will be as large or as highly anticipated as ACTT, but they have the potential to dig deeper into how patients respond to the drugs by measuring blood chemicals or looking at more subtle indicators of improvement.
“These are very modest, very humble trials,” Espinosa said. “But doing them is the way to fact-check everything. Because we scientists are not very good at shutting up — if a trial doesn’t reproduce your results, we’ll say something.”