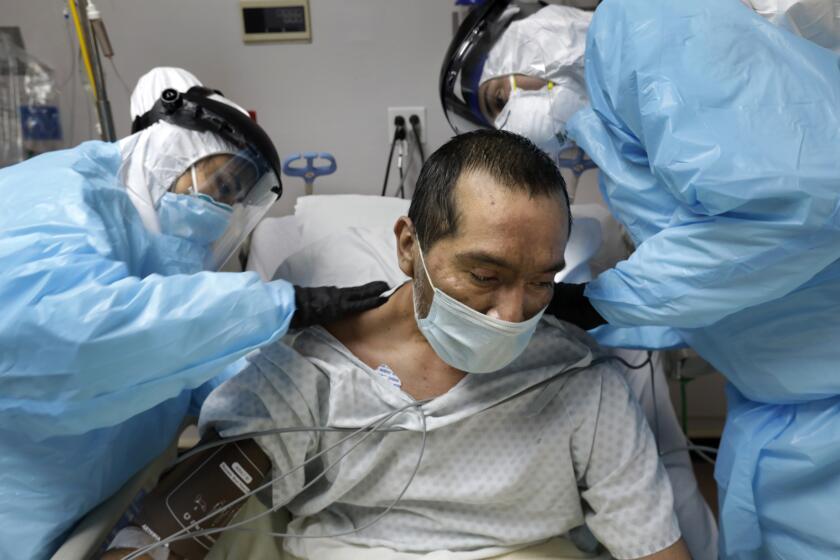
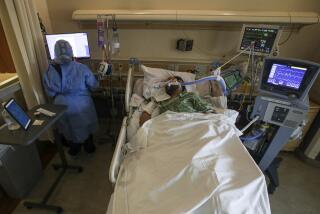
CDC data reveal another racial disparity for COVID-19 victims — age at death
- Share via
Here’s another way COVID-19 isn’t playing fair when it comes to race: It claims the lives of Black and Latino Americans earlier than whites.
Among a group of more than 10,000 people who died of COVID-19 in the U.S. in the early months of the outbreak, the typical white victim was 10 years older than the typical Latino victim. He was also nine years older than the typical nonwhite, non-Latino victim, a category dominated by Black Americans.
These findings are based on data from the health departments of 15 states and New York City and may not reflect the true extent of racial disparities across the country. Still, they point to troubling patterns that health authorities should work hard to address, according to a new report led by researchers from the Centers for Disease Control and Prevention.
The information that states, territories and local public health departments had been sending to the CDC didn’t include as many specifics about race, ethnicity, age and underlying medical conditions as the researchers would have liked. So they asked 56 such departments for supplemental information and received more detailed records from 16 of them.
The resulting data set included 10,647 people with laboratory-confirmed coronavirus infections who died between Feb. 12 and April 24.
The older you are, the greater your risk for a severe case of COVID-19, the CDC says as it expands its list of risky underlying health conditions.
Consistent with previous reports, 61% of these COVID-19 victims were men, and 75% were at least 65 years old. In addition, 35% were white, 35% were Black, 24% were Latino and 6% were Asian.
Among Latinos, the median age of death was 71 years. Among those who were neither Latino nor white, it was 72 years.
For whites, by contrast, the median age of death was 81 years.
Here’s another way of looking at the age gap: In this group, the percentage of Latinos who died who were not yet 65 years old was 35%. For nonwhites, it was 30%. Yet for whites it was only 13% — a “notable” difference, the study authors wrote.
Some of that difference might be explained by the fact that white Americans, on the whole, are older than other Americans. In the U.S., the median age of whites is 44, versus 31 for nonwhites.
But that’s clearly not the whole story, the researchers noted.
In the study population, 34% of those who were younger than 65 when they died were Latino, even though Latinos account for only 20% of all Americans under 65. Similarly, 40% of those who were under 65 when they died of COVID-19 were nonwhite, even though nonwhites account for only 23% of deaths among Americans under the age of 65, according to the report.
“Further study is needed to understand the reasons for these differences,” the authors wrote.
One possible explanation is that SARS-CoV-2, the coronavirus that causes COVID-19, is spreading more among these groups because they are more likely to be employed as essential workers in jobs that make physical distancing more difficult, the authors wrote.
COVID-19 has killed more than 100,000 people in the U.S., but some are more vulnerable than others. These charts show how Americans have been affected.
Dr. Georges Benjamin, executive director of the American Public Health Assn., echoed the idea that on-the-job exposure could be a factor in testimony he gave Friday to a congressional subcommittee on emergency preparedness and response.
“The health disparities that have occurred during the COVID-19 pandemic have four causative factors: increased exposure, increased susceptibility, social determinants that lead to unequal access to goods and services, and racism in all of its forms,” Benjamin said. “These four factors put communities of color at disproportionate risk for getting infected and getting sicker with COVID-19.”
He added that “this disparity in the impact of COVID-19 is not surprising in its presence, only in its scope.”
The authors of the CDC report suggested that healthcare providers counter this gap by being on the lookout for severe cases of disease among younger nonwhite adults: “More prompt diagnoses could facilitate earlier implementation of supportive care to minimize morbidity.”
The researchers also reported that 76% of those who died of COVID-19 had at least one underlying medical condition. That was especially true among the younger victims — 83% of those younger than 65 had at least one health problem before the coronavirus came along.
By far the most common chronic health condition reported was cardiovascular disease (61%). Diabetes was a distant second (40%), followed by chronic kidney disease (21%) and chronic lung disease (19%).
Among the 3,021 people for whom there was information about the onset of their illness, the median time between first symptoms and death was 10 days.
In addition to New York City, the study included data from Alaska, Colorado, Indiana, Louisiana, Maine, Michigan, Minnesota, New Jersey, North Carolina, Oregon, Tennessee, Utah, Vermont, Washington and Wisconsin.
The findings were published Friday in the CDC’s Morbidity and Mortality Weekly Report.