Pfizer’s COVID-19 vaccine gets nod from scientists, paving way for FDA authorization
- Share via
An influential panel of independent scientists endorsed a COVID-19 vaccine developed in record time by Pfizer Inc. and its partner, BioNTech, and urged the Food and Drug Administration to make it available for use in the U.S.
If the FDA agrees and grants emergency use authorization — a widely expected action that could come as soon as Friday — it would mark a turning point in a pandemic that has claimed more than 292,000 American lives and is still getting worse.
Once authorization is secured, states and territories will be able to place their orders for the coveted vaccine. Millions of doses could be administered to healthcare workers and nursing home residents within a matter of days.
The FDA advisory committee voted 17 to 4 Thursday in favor of recommending the experimental vaccine for use in people ages 16 and up. One committee member abstained.
The vote came after the panel of independent experts heard hours of testimony on the vaccine’s development and testing, along with discussion of the logistical and ethical issues raised by a decision to approve its use in the midst of a public health emergency.
Several members expressed discomfort with having to assess the vaccine on such a compressed schedule. But they also acknowledged that the experimental vaccine’s unexpectedly strong performance, as well as the relentless pace of the coronavirus’ spread, left them little choice but to wave it on.
“It isn’t a question of when you know everything, it’s a question of when you have enough” information to declare that a vaccine is worth a try, said Dr. Paul A. Offit, a vaccinologist at Children’s Hospital of Philadelphia who voted in favor of emergency use authorization.
“We have clear evidence of benefit,” Offit added. “All we have on the other side is theoretical risk.”
The two-dose vaccine blew past the FDA’s minimum requirements for both safety and efficacy. In Phase 3 clinical trials involving more than 43,000 volunteers, the experimental vaccine was found to be 95% effective in reducing the risk of developing COVID-19.
A total of 170 cases of COVID-19 developed during the abbreviated study period. Among them, 162 were in people who were randomly assigned to receive a placebo made of nothing but saline. Only eight of the illnesses developed in people who received the actual vaccine.
The vaccine performed similarly well for people at risk of developing more serious cases of COVID-19. For instance, the vaccine was 94% effective for those who were at least 56 years old, 95% effective for those with at least one high-risk medical condition and 96% effective for those who were obese.
In addition, the vaccine was almost equally effective for Latinos (94.5%) and non-Latinos (94.7%), and it was 100% effective among the Black study participants.
Dr. Margaret Hamburg, who led the FDA during the Obama administration, said she was particularly impressed by how well the vaccine performed for those more vulnerable groups.
“The good news couldn’t come any sooner,” she said. “We can begin to see the light at the end of the tunnel.”
None of the volunteers experienced a serious side effect in the roughly two months after they received their second dose of the vaccine. The most common side effects were fatigue, headache, muscle pain and chills, all of which were more likely after the second dose.
Well over half of the study participants who got the vaccine experienced short-term pain at the injection site.
Trial participants under 55 were more likely to report reactions to the vaccine than were older subjects.
Six of the volunteers died after joining the study, but researchers determined that their deaths — from causes such as cardiac arrest, heart attack and stroke — were not related to their participation in the study.
The vaccine was not studied in pregnant women, but the FDA will get results from animal studies next month that could signal whether it could harm a developing fetus.
A leading source of contention during the committee’s daylong meeting was whether the FDA should allow the vaccine to be used in 16- and 17-year-olds.
A mere 153 people in that narrow age group were included in the clinical trial, and some panel members felt that wasn’t enough to make an informed decision about the vaccine. Only one case of COVID-19 developed in this group, in a teen who received the placebo.
Advisory panel members also bemoaned the absence of evidence that Pfizer’s vaccine will help prevent people with few or no symptoms of infection from spreading the coronavirus, as well as the thin evidence of its power to prevent severe disease or death in people who do get infected.
“No one cares about preventing a sore throat,” said New Haven, Conn., attorney Sheldon Toubman, a consumer representative on the FDA panel.
But sussing out whether the vaccine can meet those higher bars of effectiveness will require more months of tracking clinical trial participants, the FDA and Pfizer told the committee.
That leaves both researchers and the public in a bit of a pickle: Once this vaccine has been cleared for emergency use, Pfizer researchers are ethically obliged to tell clinical trial participants who got the placebo that they can have the vaccine if they want it.
FDA experts have asked committee members to help them figure out how to keep the trial going as study participants abandon their roles as guinea pigs and demand the vaccine.
Pfizer plans to monitor all of the study participants for two years to see how long the vaccine’s protection lasts and whether longer-term side effects crop up. And several arms of the federal government — including the FDA, the CDC and the Department of Veterans Affairs — will do their own monitoring to detect any safety problems that emerge as the vaccine gets into millions of Americans’ arms.
The FDA typically follows the advice of the panel, known as the Vaccines and Related Biological Products Advisory Committee. Its members have expertise in infectious diseases, vaccines, biostatistics and law.
The vaccine has already been approved for use in Britain and Canada. As the British government began vaccinating its citizens on Tuesday, it quickly encountered an unexpected problem: Two people suffered what were believed to be severe allergic reactions after receiving their first dose of the vaccine.
In response, the U.K.’s Medical and Healthcare Products Regulatory Agency advised Britons with a “significant history” of allergic reactions to wait before getting the shot.
FDA officials told members of the advisory committee that they would require Pfizer to keep track of any such reactions in the U.S. Until it has a clearer picture of the risk, the FDA will warn physicians to avoid giving the vaccine to people who have severe allergies to any of its ingredients, or to those with a history of anaphylaxis.
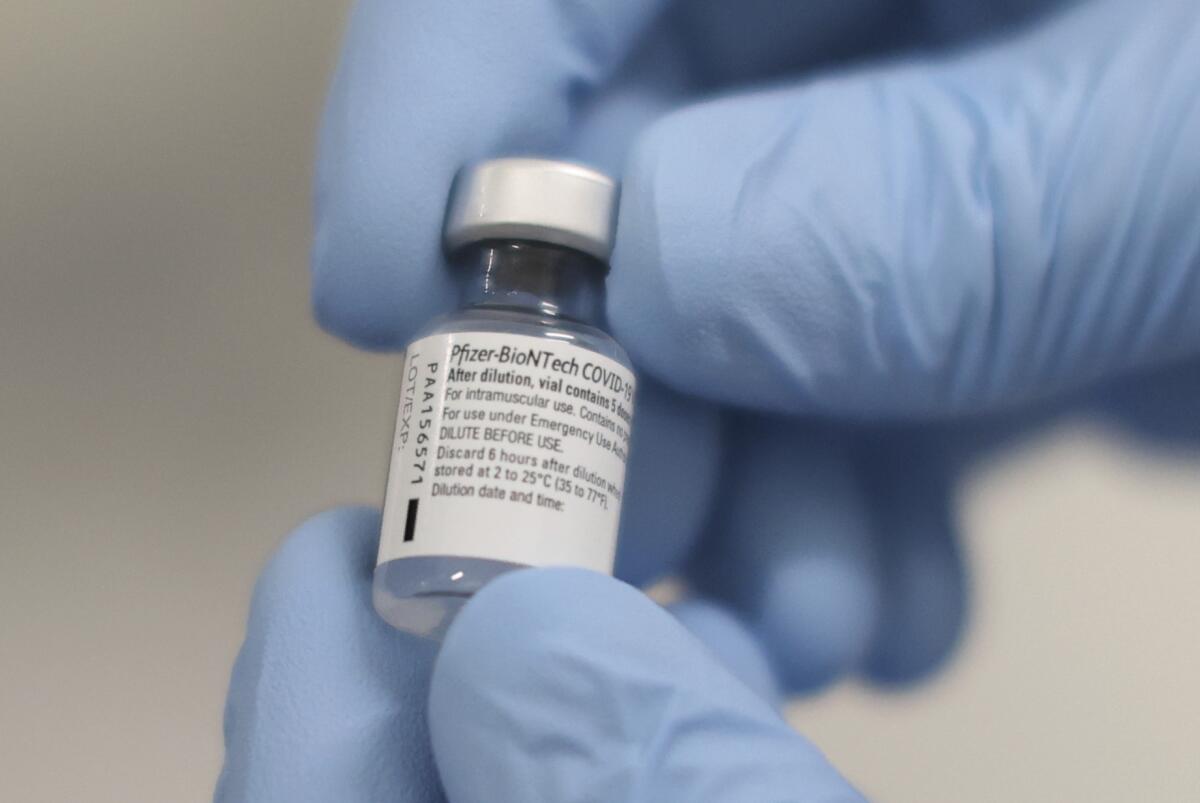
BNT162b2, as the vaccine is officially known, was developed in a matter of months thanks to a new method that uses a piece of the coronavirus’ genetic code rather than the virus itself.
Once the vaccine is injected into the body, the genetic payload — called messenger RNA, or mRNA — instructs cells to produce specific coronavirus proteins. The immune system responds by creating antibodies that are primed to attack the real coronavirus, said Dr. Bruce Walker, an immunology and infectious diseases researcher at Harvard and MIT.
“The process lasts in the body for about 36 hours,” Walker said. “Then the vaccine is degraded and essentially gone.” But the crucial antibodies remain.
The FDA has never approved or authorized an mRNA vaccine before. Nevertheless, Commissioner Stephen Hahn said the technology has been around long enough that regulators are “very comfortable” with the platform.
The vaccines do have an important downside: the need to be kept in a deep freeze to prevent the fragile mRNA from falling apart. The Pfizer-BioNTech product requires specialized refrigerated shipping containers that will be set at an optimal minus-94 degrees Fahrenheit. That’s colder than the coldest parts of Antarctica.
The advisory committee will be back in action next week to consider another mRNA vaccine that was developed by Moderna Inc. and the National Institutes of Health. That vaccine proved to be nearly 95% effective in Phase 3 clinical trials, a further endorsement of the new technology.