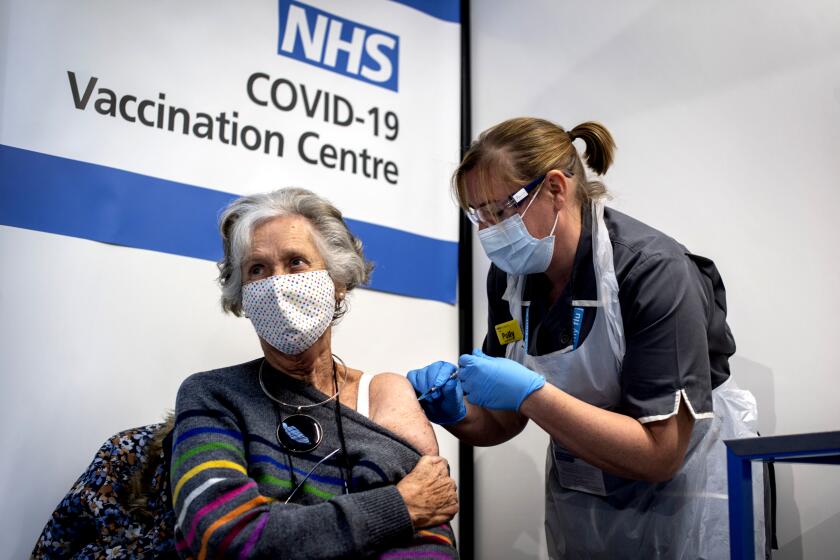
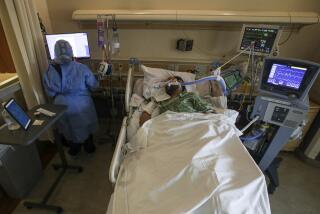
Doctors tally COVID-19’s toll on hospitalized patients: ‘It’s costly and it’s deadly’
- Share via
A new study of nearly 200,000 adults hospitalized with COVID-19 in hundreds of medical centers across the U.S. found that the oldest patients were 19 times more likely to die than the youngest patients.
Overall, death rates declined significantly over six months — an encouraging sign that as health workers learned more about the disease, they got better at keeping sick patients alive.
The findings, published Friday in the journal JAMA Network Open, offer a broad view of the mark the coronavirus has left on a wide swath of Americans.
“It’s a debilitating disease; it’s costly and it’s deadly,” said Dr. Ninh Ngyuen, a gastrointestinal surgeon at UC Irvine Medical Center who led the study. “But the bright outlook is it has improved since the initial surge in March and April.”
Using a nationwide clinical database, Nguyen and his colleagues analyzed records for 192,550 adults hospitalized with COVID-19 who were discharged from 555 medical centers across the country.
A little over half (52.5%) of the patients were men, and 43.3% were white.
Dr. Safiya Richardson, an internist at the Donald and Barbara Zucker School of Medicine at Hofstra/Northwell in New York, pointed out that nonwhite people appeared to make up a disproportionate share of the hospitalized patients in the study.
“This supports lots of evidence so far that people of color are more likely to contract and have severe cases of COVID,” said Richardson, who was not involved in the new study but conducted a similar, smaller one in New York earlier in the pandemic.
Many of the hospitalized patients already suffered from health conditions such as diabetes (38.4%) and obesity (27.4%), which make people more vulnerable to a severe case of COVID-19. The majority of patients also suffered from hypertension (61.5%), a chronic health condition that might be a risk factor for severe COVID-19, according to the Centers for Disease Control and Prevention.
By putting homeless people in hotels for isolation or quarantine, San Francisco freed up hospital space for patients with serious cases of COVID-19.
Of all patients admitted to a hospital between March 1 and Aug. 31, 28.9% received treatment in the intensive care unit. Of the patients who were admitted to the ICU, 27.8% died.
The median hospital stay for patients who didn’t need intensive care was six days, with a median cost of $10,520 per admission. For patients who ended up in the ICU, the median hospital stay was 15 days, with a median cost of $39,825.
Overall, 13.6% of the COVID-19 patients died during their first hospitalization, but Nguyen said that figure climbed to 16.6% when patients who were transferred to hospice care were factored in.
Though hospice patients may die weeks or months after leaving the hospital, they should still be taken into account, said Dr. David Asch, an internist at the University of Pennsylvania who was not involved in the new research.
“We were sending a lot of people to hospice, which means you think they’re going to die,” Asch said. “A lot of these people weren’t going to be hospice candidates, except for COVID.”
The risk of death in hospitals fell significantly over the study’s six-month period, declining from 22.1% in March to 6.5% in August. That’s probably because treatments and practices improved as doctors and nurses gained experience with caring for COVID-19 patients, Nguyen said.
After 90 days, the immunity developed in response to a coronavirus infection is about as protective as a COVID-19 vaccine, according to a new study.
As has been made devastatingly clear during the pandemic, elderly people were the most vulnerable to dying of COVID-19: Among the 12,644 hospitalized patients between the ages 18 and 29, 179 (or 1.4%) died. Meanwhile, among the 31,135 hospitalized patients who were 80 or older, 8,277 (or 26.6%) died.
Richardson praised the study for providing a “bigger picture” of the patterns among hospitalized COVID-19 patients. She also added that she would have liked to see how the number and percentage of hospitalized patients in each age group changed over time.
“When reflecting on the nationwide public health data and the decreased overall mortality from COVID compared to total case rates, we think a part of this is that more young people have gotten it,” Richardson said in an email. “It would have been nice to see if that played out in their data and [if] the percent of younger people admitted to hospitals with COVID increased over time.”
Asch said it would have been useful to see how these mortality rates varied among hospitals, given that the death rates between hospitals can be dramatically different, as his previous work showed.
“Some hospitals are going to keep you alive better than others,” he said.
That’s not to mention that different regions — and thus, the hospitals within them — experienced the surge differently.
“New York City in March is different from Wichita in March,” Asch said. “New York City in March was getting hammered and probably learned a lot from that.”
Just one dose of the Pfizer-BioNTech vaccine was 60% to 70% effective at preventing symptomatic COVID-19 disease in people age 70 and older, a new report says.
When it comes to patient care, there are some factors that affect a patient’s risk of death that doctors can’t change, Asch pointed out. They can’t change the point in the pandemic at which patients get sick, for instance, and they can’t change a patient’s age.
But as researchers gather more information about the nature of COVID-19, he said, they might be able to use large data sets like this to figure out what factors they can change to improve a patient’s chances of survival.
Were the patients who were more likely to live given aspirin? Were they put in rooms with windows? What was it that helped?
“To the extent that their data could be used to tease apart what are the actionable clinical determinants of differential survival, that would be great,” he said.