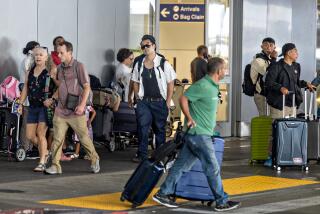Luck is essential for any successful coronavirus variant, study shows
- Share via
Let’s say you are a new member of the SARS-CoV-2 family, with a few genetic tweaks that distinguish you from the rest of the clan. Maybe you have changes in your spike protein that allow you to more easily to invade cells, or a random mutation that helps you elude the virus-killing effects of a COVID-19 treatment.
You could be a contender. But first, you have to get out of the body you’re in and infect some more people.
What would it take for you to succeed and prosper? Alternatively, what would cause you to die on the vine, a short-lived experiment in evolution’s harsh proving chamber?
A modeling exercise by researchers at the Fred Hutchinson Cancer Research Center in Seattle suggests that for a genetic variant of SARS-CoV-2 to become a menacing new presence, it’s not enough to be scary and highly transmissible. It also needs a string of lucky breaks to establish itself.
Most notably, it must gain entree to a superspreader event if it is to have a fighting chance of planting its flag in a population. In the brief period during which its carrier is at or close to his peak viral load, the new variant needs to hitch a ride to someplace like a choir practice, a political rally, a poorly ventilated barroom, or a packed indoor arena where people are mingling at close quarters and many are not wearing masks.
Once there, it needs to infect at least a handful of people. Five would be enough for the new variant to live on to compete for more victims. Infecting 20 or more will give it a real chance of becoming predominant in its new community.
Time is of the essence, the new research suggests: Even for a new variant that’s armed with transmission superpowers, that first superspreader event needs to come within a month of its arrival for the variant to stand a chance of becoming established.
That’s a lot of narrow windows and a lot of high hurdles, and the likelihood that a new variant will clear all of those obstacles is actually pretty slim, the researchers concluded. And that should offer humans a bit of hope.
A pair of studies in Science examine how coronavirus variants evolve in human hosts and why experts are concerned about relaxing restrictions too soon.
But then there’s reality: At least five new “variants of concern” have apparently overcome these forbidding odds in the span of about six months.
That suggests something rather ominous: There are probably many more such variants out there, each looking for its lucky break. While few variants will get it, it only takes one or two with the right constellation of mutations to prolong or escalate the pandemic — or to undermine the vaccines and medicines that could end it.
The team’s model was posted this week to MedRxiv, a site where researchers share their research results and seek feedback from colleagues. As such, its findings are considered preliminary.
For researchers hoping to see around the next corner of the pandemic, a modeling exercise like this is more than an idle speculation.
The coronavirus that causes COVID-19 is known to mutate constantly, but almost always in ways that don’t significantly change its behavior. So it would be nice to know how these variants are born and whether there are many more like them. And if there are, it would be useful to know how they can be bottled up quickly.
“Phenomenological” modeling studies such as this one gather the wildly erratic patterns of spread buried in pandemic data, combine them with well-documented cases of superspreader events, and drop in a new actor that plays by slightly different rules. Then they play out what happens next over and over again in computer models that act as digital test tubes.
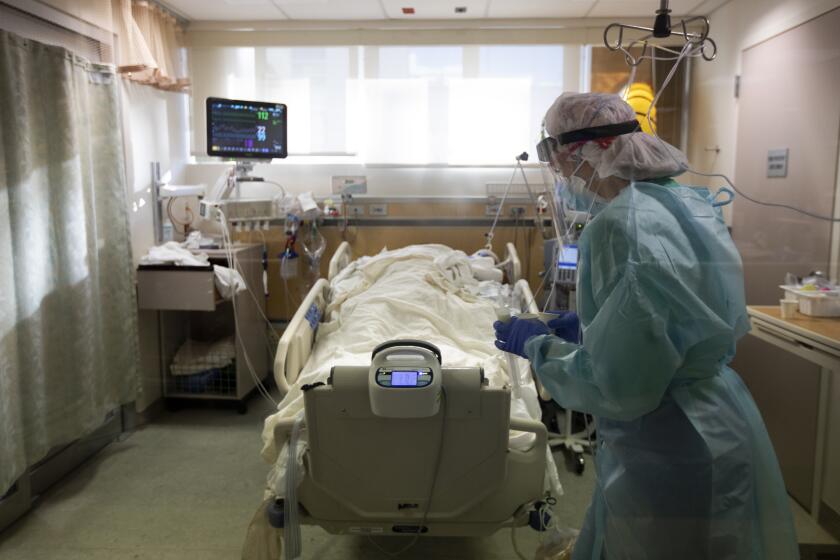
One thing researchers are increasingly sure of is that in patients with compromised immune systems, the coronavirus is more likely to take on not just one but a passel of mutations. Those genetic changes could make it even harder to fight the virus with medicines, masks and vaccines.
COVID-19 patients who take months to overcome their coronavirus infections despite treatment can become incubators of dangerous new strains.
A model like this doesn’t yield calibrated measurements of how effectively an intervention like universal masking can stop spread. It doesn’t generate predictions about the pandemic’s next stage. But it does provide insights into how a virus behaves under a range of circumstances, along with probabilistic estimates that can sharpen the intuitions of public health officials.
“We will in all likelihood create new variants on top of those that have emerged,” said Dr. Joshua T. Schiffer, who led the modeling team at Fred Hutch. “And the ones that will win are the ones that dodge the vaccine or transmit more easily.”
These variants don’t have names yet and may not pop up for months, Schiffer added. But when they do arise, they’ll be subject to the same harsh early-life experiences.
After running through thousands of scenarios, the team concluded that variants with potentially frightening capabilities to spread and sicken probably occur frequently in the course of a pandemic the size of this one. After all, there are dozens of branches on the SARS-CoV-2 family tree, and each of them might have been a chance for genetic mischief. Given the punishing attrition rate of new variants, ill-fated ones must be born every day around the world for so many branches to have emerged.
Periods of high transmission seem to create an “all comers welcome” atmosphere for variants. So when infections are surging, even a variant that’s no more transmissible than those already in circulation stands a better chance of elbowing its way into the game, the modeling shows. And a genetic variant that arrives with a biological advantage in that department is even more likely to succeed.
The Biden administration is boosting efforts to identify and track coronavirus variants to help scientists see where the pandemic is heading next.
All of these newcomers still face tall odds. But if many variants are out there, and if careless societies afford them the chance of an early superspreader event, then it’s reasonable to assume that at least one or two may gain enough of a foothold to take off.
Their impact on the pandemic’s trajectory will be a genetic roll of the dice.
In the meantime, the research offers some actionable advice for both experts and the general public.
The most effective way to reduce the number of new variants is to prevent “large waves of infection” from happening in the first place, the study authors write. Not only is a surge an ideal environment for generating new variants, it also offers plenty of opportunity for a superspreading event.
And that means we all have a role to play by wearing masks, practicing social distancing, avoiding large gatherings and taking other precautions that can deprive a new variant of the luck it needs.