What’s the difference between ‘pandemic’ and ‘endemic’?

- Share via
COVID-19 will never go away, infectious disease experts tell us, but the global health emergency it sparked will be over when the disease becomes “endemic.”
That certainly sounds like something to look forward to. But what exactly does it mean?
Endemic is related to two words we’ve come to know well:
- epidemic: an infectious disease outbreak that is spreading rapidly through a community.
- pandemic: an epidemic that affects people throughout a large region or across multiple continents.
When COVID-19 is endemic, it will still spread from one person to another, and it will still affect people all over the world. The key difference is that it will do both of those things at stable levels.
Stability is important because it translates into predictability. Knowing how many people will come down with COVID-19, when they’re most likely to get sick and where they’ll be most vulnerable will allow health officials to contain the disease with far fewer disruptions to the public at large.
A leading World Health Organization official says the worst of the COVID-19 pandemic — including deaths, hospitalizations and lockdowns — could be over this year if huge inequities in vaccinations and medicines are addressed quickly.
Influenza is a good example of an endemic disease. About 8% of the U.S. population comes down with it every year, and the bulk of cases are clustered in the winter months. Epidemiologists have established who is most likely to get it (children and teens) and who faces the highest risk of becoming seriously ill (senior citizens, people with chronic health conditions, pregnant women and children under 5).
The things we do to minimize the impact of the flu — washing our hands, covering our coughs and sneezes, staying home when ill — are so routine that we barely even notice we’re doing them. (The exception is getting a flu shot; roughly one-third to one-half of Americans skip it each year.)
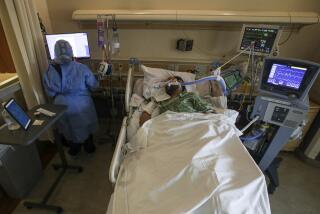
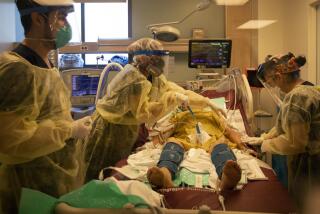
An endemic disease typically produces fewer serious illnesses than COVID-19 does now. In 2020, 53,544 Americans died of influenza and pneumonia combined, according to the Centers for Disease Control and Prevention. By contrast, more than 350,000 Americans died of COVID-19 that year, as did more than 475,000 in 2021.
Unfortunately, there’s no easy formula for calculating how long it takes for a pandemic disease to transition to an endemic state, said Dr. Mike Ryan, executive director of the World Health Organization’s Emergencies Program.
“It’s a somewhat subjective judgment because it’s not just about the number of cases. It’s about severity and it’s about impact,” he said.
Elite commentators say COVID is over. That may be true for them but not for millions of others.
One thing experts can predict is that COVID-19 will continue to cause serious illnesses and deaths even when it’s endemic.
“Endemic does not mean it’s not dangerous,” said Dr. Maria Van Kerkhove, the WHO’s technical lead on COVID-19.“We will continue to see outbreaks among susceptible populations.”
Jennifer Nuzzo, an infectious diseases expert at the Johns Hopkins Center for Health Security, agreed that the coronavirus will be keeping us on our toes for the foreseeable future.
“All pandemics end,” she said during a panel discussion hosted by the National Academy of Medicine and the American Public Health Assn. “But this virus isn’t going away. It’s not going to disappear.”