Experts wrestle with how to update COVID-19 vaccines
- Share via
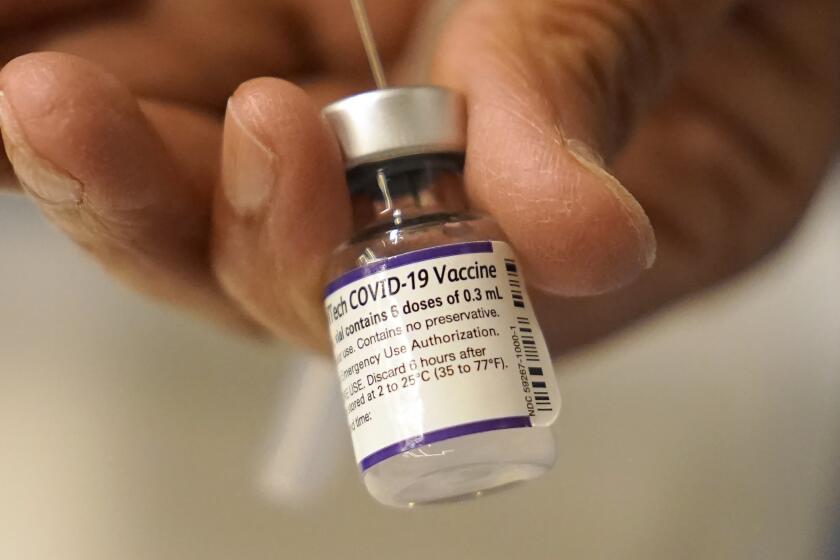
WASHINGTON — More than two years into the COVID-19 pandemic, U.S. health officials are beginning to grapple with how to keep the vaccines updated to best protect Americans from the ever-changing coronavirus.
On Wednesday, a panel of vaccine advisors to the Food and Drug Administration spent hours debating key questions for revamping the shots and conducting future booster campaigns. They didn’t reach any firm conclusions.
The questions facing the experts included: how often to update the vaccines against new strains, how effective they should be to warrant approval and whether updates should be coordinated with global health authorities.
Last week, the FDA authorized a fourth dose of the Pfizer or Moderna vaccines for anyone 50 or older and for some younger people with severely weakened immune systems. It’s an effort to get ahead of another possible surge.
But the FDA’s vaccine chief, Dr. Peter Marks, acknowledged at the meeting “we simply can’t be boosting people as frequently as we are.” He called the latest booster update a “stopgap” measure to protect vulnerable Americans while regulators decide whether and how to tweak the current vaccines.
The FDA and CDC offered little guidance about who should get the newly authorized second COVID-19 booster shot. We break it down.
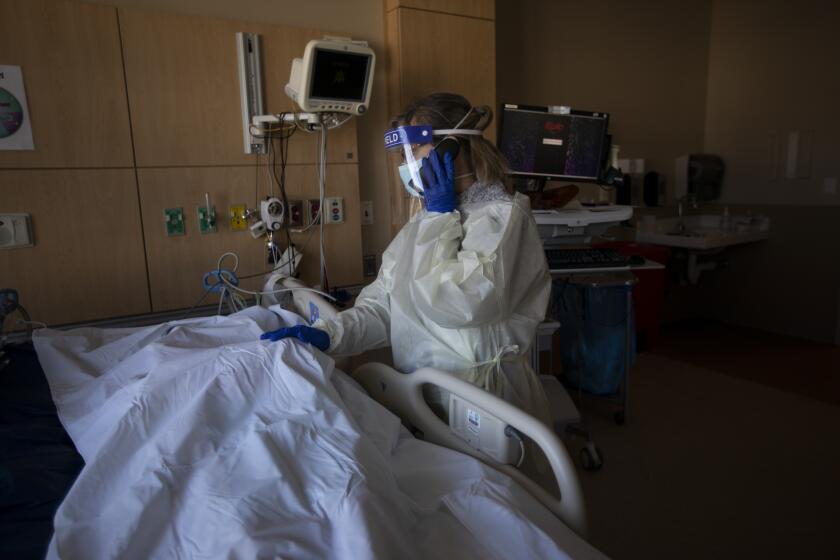
Marks cautioned that waning vaccine protection, new variants and colder weather in the fall could raise the risk of more surges.
“Our goal here is to stay ahead of future variants and outbreaks and ensure we do our best to reduce the toll of disease and death due to COVID-19,” said Marks, adding that he expects more meetings of the vaccine panel in coming months.
Some of the key questions the panel discussed:
How should the U.S. decide when to launch future rounds of booster shots?
One area in which experts appeared to agree is that vaccines should be judged on their ability to prevent severe disease that leads to hospitalization and death.
“We need to focus on the worst case, which is severe disease, and we need to change strains when we’re losing that battle,” said Dr. Mark Sawyer of UC San Diego.
By that measure, the current vaccines have held up remarkably well.
During the last Omicron-driven surge, two vaccine doses were nearly 80% effective against needing a breathing machine or death — and a booster pushed that protection to 94%, federal scientists recently reported.
But only about half of Americans eligible for a third shot have gotten one. And many experts said it was unsustainable to continue asking Americans to get boosted every few months.
The closer we get to the end of the pandemic, the harder it is to justify the risk of a COVID-19 vaccine mandate for young children.
A panelist from the Centers for Disease Control and Prevention suggested that the 80% protection from severe disease could become the standard for evaluating the vaccines.
“I think we may have to accept that level of protection and then use other alternative ways to protect individuals with therapeutics and other measures,” said Dr. Amanda Cohn, the CDC’s chief medical officer.
Presentations at the meeting by government health officials and independent researchers underscored the challenges of predicting when the next major coronavirus variant might appear.
Trevor Bedford, a disease modeler with the Fred Hutchinson Cancer Center, said a major new strain like Omicron could emerge anywhere from every 1.5 years to once a decade, based on currently available data. Given that unpredictability, researchers will need methods to quickly determine whether current vaccines work against emerging variants.
What’s the process for updating vaccines to address new variants?
All three COVID-19 vaccines now used in the U.S. are based on the original coronavirus that emerged in late 2019. Updating the vaccines will be a complex task, probably requiring coordination among the FDA, manufacturers and global health authorities.
To speed the vaccines to market, the FDA relied on research shortcuts to judge effectiveness, mainly looking at their early impact on the immune system’s antibody levels. A number of panelists said Wednesday they wanted more rigorous data from studies that track patients over time to see who gets sick or dies.
But that approach would probably be too time-consuming.
“We’re looking at a conundrum here in that it’s going to be hard to generate all the data we want in short order when a new variant emergences,” said Dr. Ofer Levy of Harvard Medical School.
Deciding how many Americans we are willing to let die of COVID-19 each year is necessary to put the pandemic behind us.
A representative for the U.S. Biomedical Advanced Research and Development Authority laid out the narrow window that manufacturers could face to reformulate, study and mass-produce an updated vaccine by September.
“If you’re not on your way to a clinical trial by the beginning of May, I think it’s going to be very difficult to have enough product across manufacturers to meet demand,” said Robert Johnson, deputy assistant secretary of BARDA.
The process for updating annual flu vaccines offers one possible model, as laid out by a representative from the World Health Organization.
Twice a year, WHO experts recommend updates to flu vaccines to target emerging strains. The FDA then brings those recommendations to its own vaccine panel, which votes on whether they make sense for the U.S., setting the stage for manufacturers to tweak their shots and begin mass production.
But COVID-19 hasn’t yet fallen into a predictable pattern like the flu. And as the coronavirus evolves, different strains may become dominant in different regions of the world.
Several experts said they would need more meetings with more data and proposals from the FDA to decide on a strategy.
“We’ve never been here before. We’re all working together to do the best we can and it’s very complex,” said Oveta Fuller of the University of Michigan’s Medical School.