Weaning the county jail population off opioids
- Share via
SAN DIEGO — It wasn’t long ago that a complaint of pain at a San Diego County jail easily scored an inmate a prescription for an opioid.
These days, the highly addictive, highly abused painkillers have been largely swapped out for Tylenol and ibuprofen as part of a program to stem the cycle of opioid addiction behind bars.
So much so, that an inmate with an opioid prescription is a rarity.
Last month, only 23 inmates, including those with cancer, were prescribed an opioid. That’s less than 1 percent of the total jail population.
The number represents a 98 percent drop from the beginning of 2013, when nearly 1,000 inmates were prescribed more than 77,000 narcotic painkiller pills.
“This really cleaned up the jails,” said Dr. Alfred Joshua, the Sheriff’s Department’s chief medical officer who implemented the program in 2014. Sheriff’s officials report fewer opioids being diverted to other inmates, fewer inmates being bullied for their prescription pills, fewer overdoses and an overall calmer environment in the daily “med” lines.
“Any process that will help someone overcome addiction can only be viewed as successful,” said sheriff’s Cmdr. Mike Hernandez, who heads the Medical Services Division.
However, authorities have noticed an uptick in attempts to smuggle heroin into the jails, a trend officials attribute only partly to the reduction in prescription opioids. Under the 2011 Public Safety Realignment law, some inmates are serving longer terms in jails rather than prisons — an average of 215 days — and are directing smuggling operations, Hernandez said.
“They’re mirroring what they do in state prison,” he said.
The price for heroin in jail has increased significantly, Hernandez said, and demand remains high as short-term inmates addicted to the drug don’t fully withdraw and their strong cravings persist.
The effort to reduce prescription opioid use mirrors the cultural shift happening on the outside. Doctors who used to easily dash off prescriptions for opioids — many under the false belief that certain opioids were non-addictive and the best way to treat pain — suddenly were at the center of a national epidemic of addiction and overdose.
With public awareness mounting since around 2011, and drug overdose deaths reaching 64,000 nationwide in 2016, physicians are holding back their prescription pads and re-evaluating how to treat pain.
The general public has had to be re-educated in the process, and so have those admitted into San Diego County jails over the past few years. It is a problem especially critical behind bars, where up to three-quarters of the population have a history of substance abuse or are jailed on drug-related charges.
“Traditionally, they’d come in with back pain and get a prescription,” Hernandez said. “Now that the physicians have found alternatives to opiates, they’ve learned that when they come into our facilities they may not be receiving opiates.”
The ongoing education about the dangers of opioids has helped change inmates’ expectations, said Joshua.
“A lot realize that it does more harm than good,” the doctor said.
However, some inmates have accused the Sheriff’s Department of going too far with its policy. The reduction in opioid prescriptions has prompted a handful of federal lawsuits against Joshua and the department from inmates who claim their conditions warranted stronger pain treatment.
None of the inmates have prevailed in court thus far.
Joshua says the program doesn’t rule out opioid prescriptions altogether but gives a good deal of discretion to the physicians who treat the inmates. Prior medical records provide important clues to whether an inmate legitimately requires opioids, he said. The doctors are mainly looking for a current prescription by a consistent provider or a current chronic pain diagnosis.
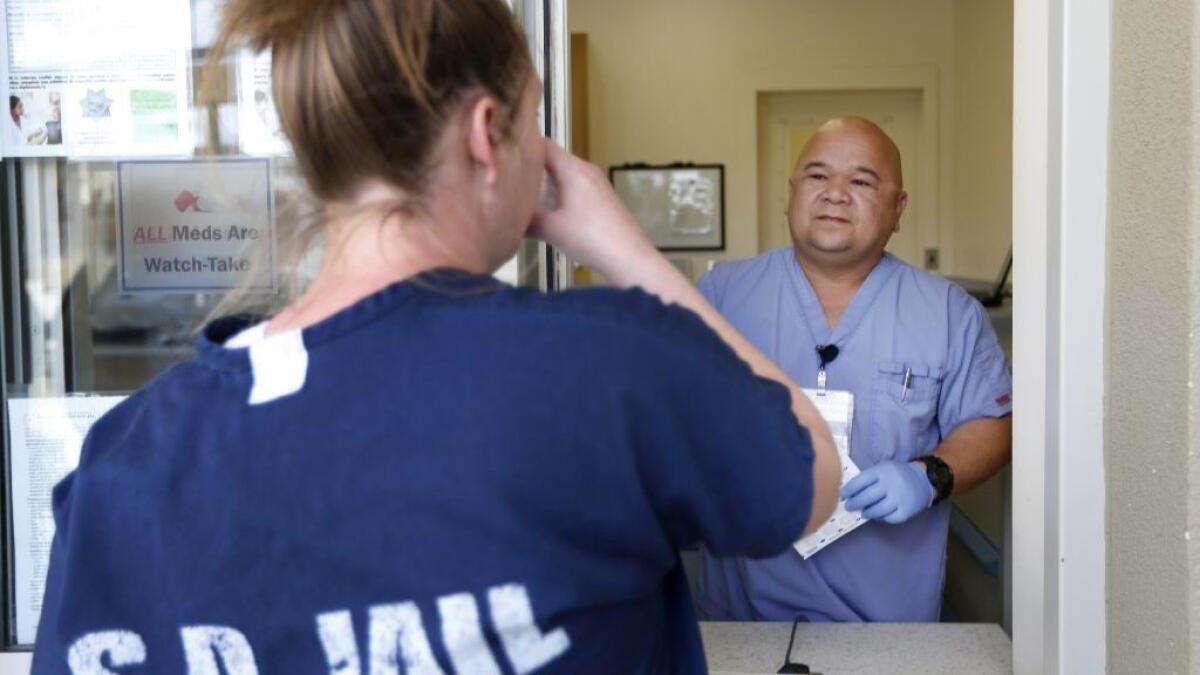
The select few who are granted opioid treatment are strongly counseled about the risks involved and warned of a zero-tolerance policy against diversion. Nurses and jail deputies make sure that inmates aren’t “cheeking” or “tonguing” the narcotics to give them to other inmates. If an opioid patient is caught trying save a dose, he or she might be taken off the opioid and given a non-narcotic alternative.
The doctors are also following recommendations based on recent research that shows over-the-counter stalwarts acetaminophen and ibuprofen can be more effective at treating pain than opioids. Inmates can request a higher level of painkiller, but that doesn’t always mean the doctor will agree.
Inmates who feel they aren’t being treated properly can file grievances to the command staff, and as a last resort, a lawsuit.
But it’s a high bar the inmate has to meet for a constitutional claim of cruel and unusual punishment.
An inmate must show that he or she has a serious medical condition and that prison officials were deliberately indifferent to the inmate’s health and safety.
The Constitution does not mandate “comfortable prisons” but prohibits extreme deprivations such as the “wanton and unnecessary infliction of pain” or conditions that deprive “inmates of the minimal civilized measures of life’s necessities,” pointed out U.S. Magistrate Judge Mitchell Dembin, citing a Supreme Court decision in one such San Diego lawsuit.
Difference of medical opinion is not enough, U.S. Magistrate Judge Ruben Brooks found in another case involving an inmate whose pain medication was replaced with non-narcotics.
“An inmate does not have a constitutional right to choose his own medication,” Brooks wrote in his opinion. “If medical personnel disagree on the course of patient treatment, subsequent health care providers are not deliberately indifferent when they choose one treatment over the inmate’s wishes.”
The National Commission on Correctional Health Care advocates for alternatives to opioids when appropriate, noting that the custodial environment provides a good opportunity to regularly assess how patients are functioning and monitor the efficacy of their treatments.
“Therefore, when patient function remains poor and pain is not well controlled, and other options have been exhausted, a therapeutic trial of medication, including opioids, should be available,” the commission wrote in its pain management guidelines.
It’s an issue that the Prison Law Office, a California-based nonprofit that advocates on behalf of inmates and prisoners, has closely monitored.
“When they have restricted those medications, we’ve made sure there’s a medical basis for doing so and other alternatives available,” said the group’s executive director, attorney Donald Specter.
“I think generally now there’s recognition in the community about the dangers of opioids,” he said, “the same guidelines in effect in the community should also be present in the prisons.”
kristina.davis@sduniontribune.com
Twitter: @kristinadavis
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.














