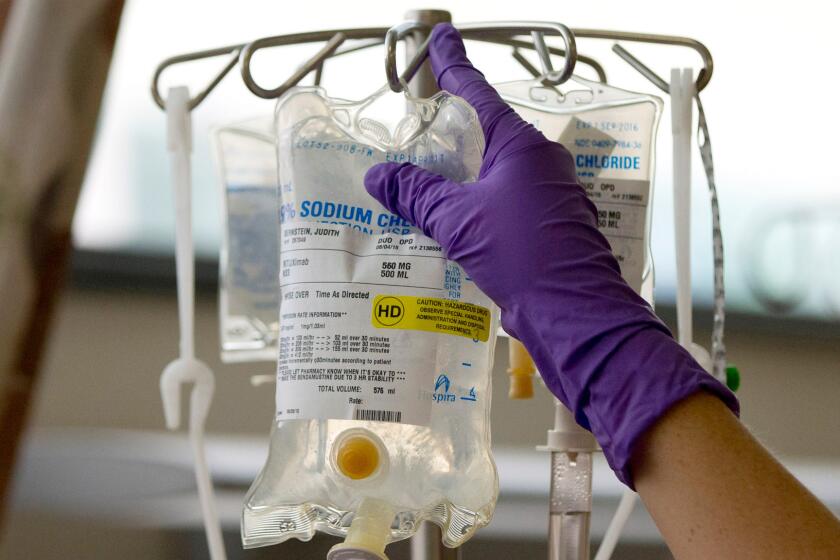
Another potential coronavirus casualty: the fight against other diseases

- Share via
NEW DELHI — Lavina D’Souza hasn’t been able to collect her government-supplied anti-HIV medication since the abrupt lockdown of India’s 1.3 billion people last month during the coronavirus outbreak.
Marooned in a small city away from her home in Mumbai, she’s run out of the medicine she needs to manage her disease and is afraid that her immune system will crash. “Any disease, the coronavirus or something else, I’ll fall sick faster,” said D’Souza, 43, adding that many people are “suffering because of the coronavirus without getting infected by it.”
As the world focuses on the COVID-19 pandemic, experts fear losing ground in the long fight against other infectious diseases — such as AIDS, tuberculosis and cholera — that kill millions every year. Also at risk are decades-long efforts that allowed the World Health Organization to set target dates for eradicating malaria, polio and other illnesses.
With the coronavirus overwhelming hospitals, redirecting medical staff, causing supply shortages and suspending health services, “our greatest fear” is resources for other diseases being diverted and depleted, said Dr. John Nkengasong, head of the Africa Centers for Disease Control and Prevention.
History shows that, during a pandemic, other diseases can make a major comeback. Amid an Ebola outbreak in Guinea, Liberia and Sierra Leone in 2014-16, almost as many people died of HIV, tuberculosis and malaria because of reduced access to healthcare.
Rashid Ansumana, a community health expert in Sierra Leone who studied the Ebola outbreak, said the coronavirus’ “impact will definitely be higher.”
The coronavirus, and Trump’s ire, draw increased attention to the World Health Organization.
That’s especially a danger in countries with already overburdened healthcare systems, such as Sudan. Doctors at Al-Ribat National Hospital in the Sudanese capital, Khartoum, shared a document detailing nationwide measures: fewer patients admitted to emergency rooms, elective surgeries indefinitely postponed, primary care eliminated for noncritical cases, and skilled doctors transferred to treat COVID-19 patients.
Similar scenes are unfolding worldwide. Even in countries with highly developed healthcare systems, such as South Korea, patients seeking treatment for diseases like TB had to be turned away, said Hojoon Sohn of the Johns Hopkins Bloomberg School of Public Health.
About 30% of global TB cases — out of 10 million each year — are never diagnosed, and the gaps in care are concentrated in 10 countries with the most infections, said Sohn, who is based in South Korea.
“These are people likely not seeking care even in normal circumstances,” he said. “So with the COVID-19 pandemic resulting in health systems overload, and governments issuing stay-at-home orders, it is highly likely that the number of TB patients who remain undetected will increase.”
Families say hospitals are rationing medical care for other life-threatening illnesses as India mobilizes its resources to fight the coronavirus.
In Congo, already overwhelmed by the latest outbreak of Ebola and years of violent conflict, the coronavirus comes as a measles outbreak has already killed over 6,000 people, said Anne-Marie Connor, national director for World Vision, a humanitarian aid organization.
“It’s likely we’ll see a lot of ‘indirect’ deaths from other diseases,” she said.
The cascading impact of the pandemic isn’t limited to treatment. Other factors, including access to transportation during a lockdown, are threatening India’s progress on TB. Patients and doctors can’t get to clinics, and it’s difficult to send samples for testing.
India has nearly a third of the world’s TB cases, and diagnosing patients has been delayed in many areas.
The fear of some diseases resurging is further aggravated by delays in immunization efforts for more than 13.5 million people, according to the vaccine alliance GAVI. The international organization said 21 countries are reporting vaccine shortages following border closures and disruptions to air travel — mostly in Africa — and 14 vaccination campaigns for diseases such as polio and measles have been postponed.
The Measles & Rubella Initiative said measles immunization campaigns in 24 countries already are delayed, and it fears that more than 117 million children in 37 countries may miss out.
A diagnosis of breast cancer is always accompanied by angst and uncertainty. It’s even more fraught when it comes in the midst of the coronavirus crisis.
Dr. Jay Wenger, who heads polio eradication efforts for the Bill & Melinda Gates Foundation, said recommending the suspension of door-to-door polio vaccinations was difficult, and while it could lead to a spurt in cases, “it is a necessary move to reduce the risk of increasing transmission of COVID-19.”
Programs to prevent mosquito-borne diseases also have been hampered. In Sri Lanka, where cases of dengue nearly doubled in 2019 over the previous year, health inspectors are tasked with tracing suspected COVID-19 patients, disrupting their regular work of destroying mosquito-breeding sites at homes, said Dr. Anura Jayasekara, director of Sri Lanka’s National Dengue Control Unit.
Some health providers are trying to ease the crisis for sufferers of non-coronavirus-related ailments by giving months of supplies to people with hepatitis C, HIV and TB, said Dr. Marc Biot, director of operations for the international aid group Doctors Without Borders.
As countries face difficult healthcare choices amid the pandemic, Nkengasong of the Africa CDC warns that efforts to tackle other diseases can’t fall by the wayside.
“The time to advocate for those programs is not when COVID is over,” he said. “The time is now.”
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.