- Share via
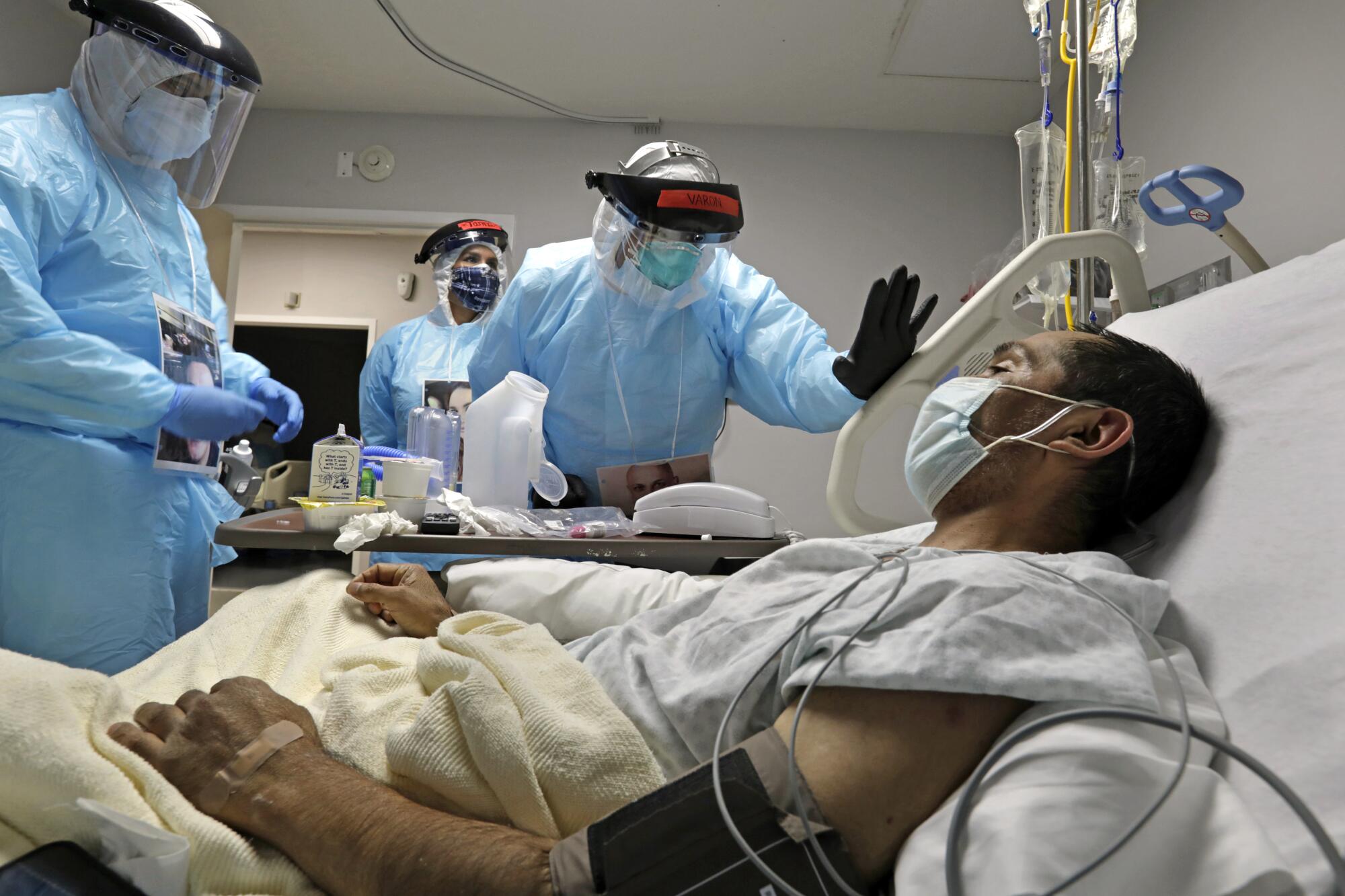
HOUSTON — Before the doctor unzipped his COVID unit’s plastic curtain, he grabbed a laminated photo from a hook labeled “Faces Behind the Mask.” He draped the ribbon holding the photo over his protective suit so patients could see who he was: Dr. Joseph Varon, 58, bald and trim with intense blue eyes.
Varon entered the 20-bed unit hyper as usual, rustling through the airlock of an entrance like an astronaut, raising the final curtain with hands coated in several sets of black rubber gloves.
A lung doctor specializing in intensive care, he’d managed emergency rooms at larger hospitals, spoken a half-dozen languages in clinics around the world. When SARS erupted in Asia, Varon flew to Singapore to learn how to treat it. Now he was pulling 20-hour shifts, phoning medical students late at night to scan the latest research.
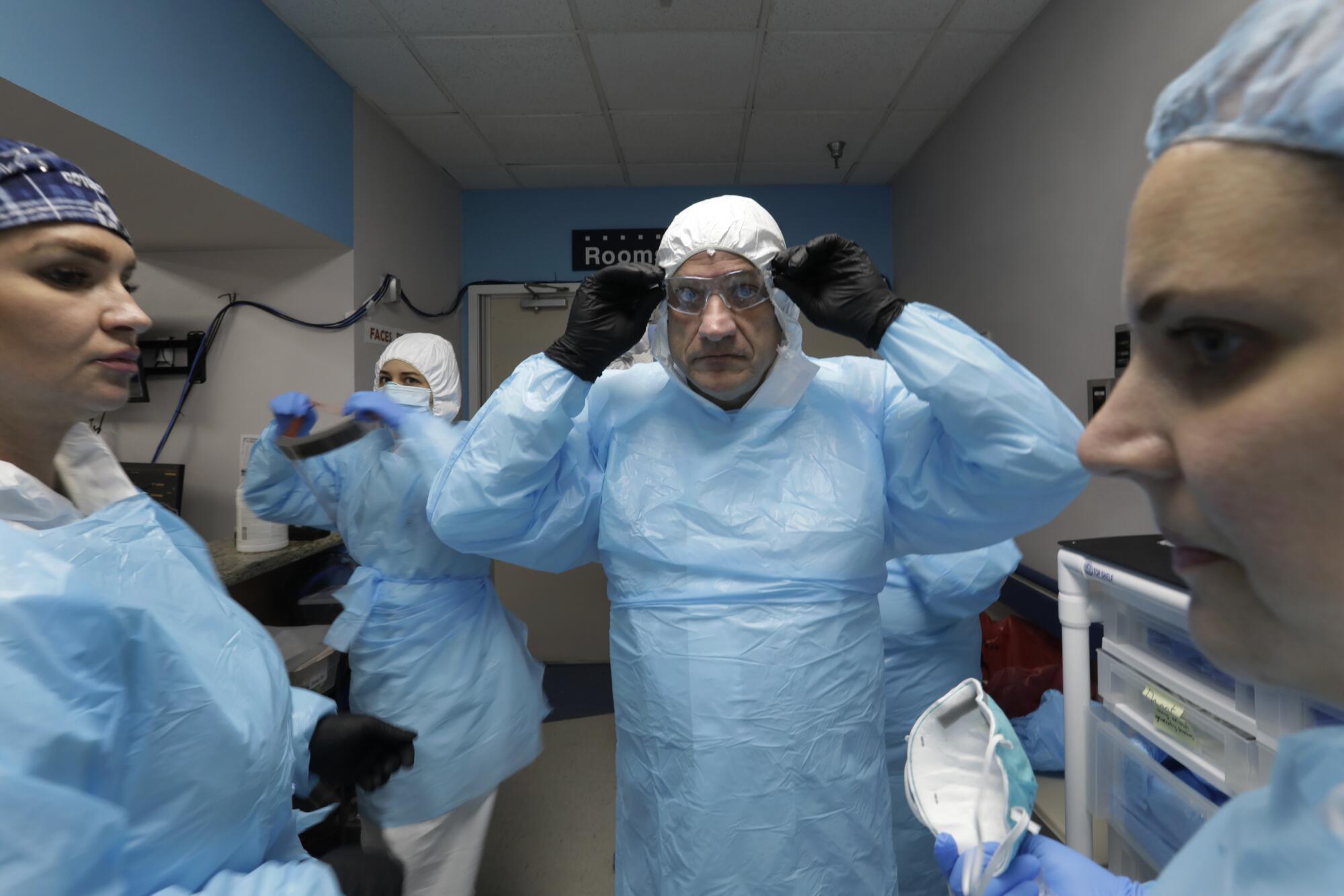
As he noted in a recent medical journal, being a “COVIDoligist” means, “No days off, no time for family. No time for anything else other than COVID-19.”
“This,” he said, “is what I’m meant to do.”
As chief of staff and chief of critical care services at United Memorial Medical Center in Houston, Varon and his small team of nurses and medical student volunteers have treated COVID-19 patients with surprising success.

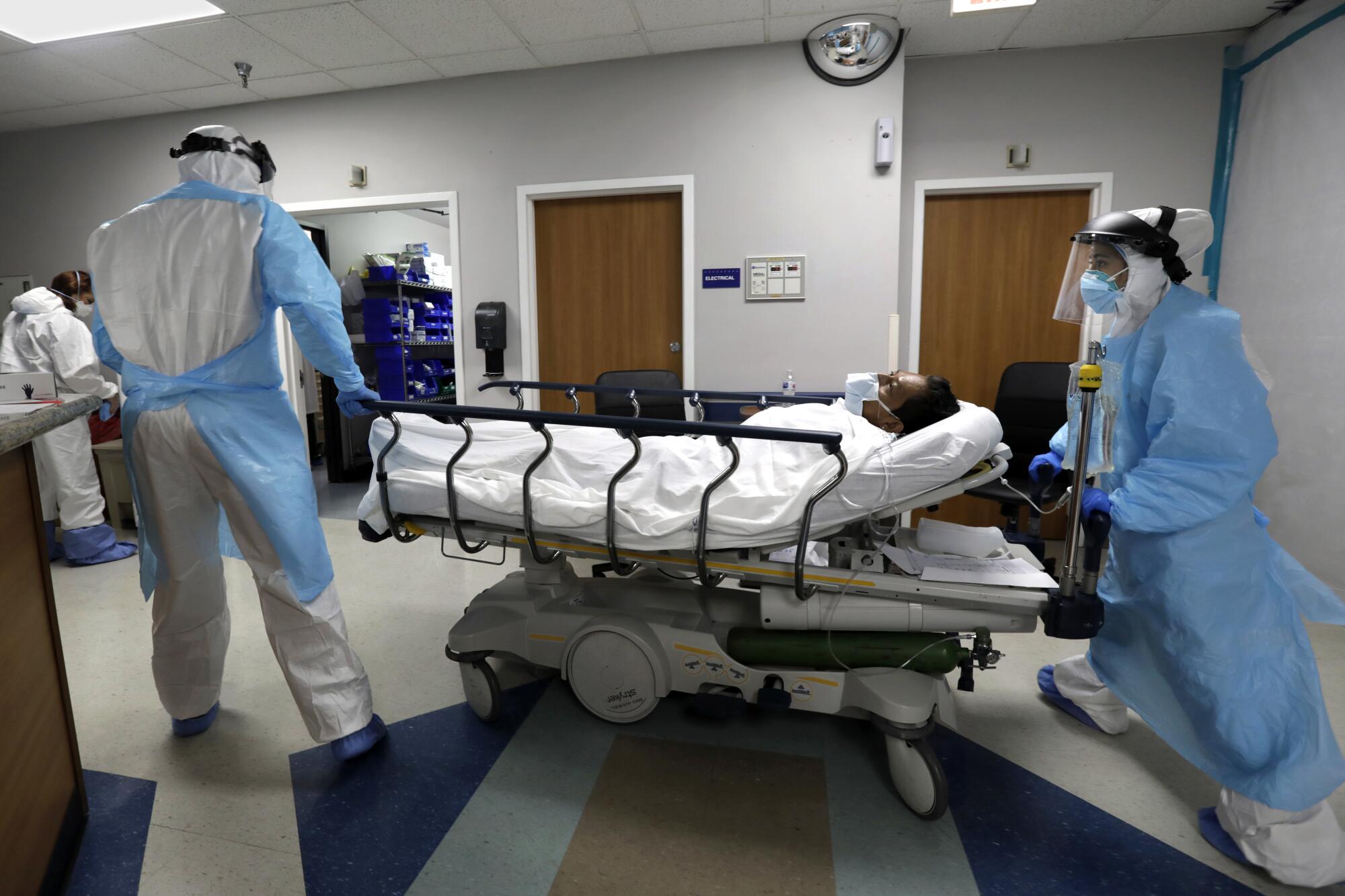
Last week, the unit’s central hallway was chilly, the air conditioning cranked. But Varon was sweating inside his hooded white protective suit, breath fogging his face shield even through two layers of masks. He strode swiftly past a boxy negative-pressure machine that hummed as it blocked contaminated air from escaping the unit.
A double layer of shoe covers muffled Varon’s steps, sparing him from having to disinfect his shoes. A half-dozen nurses and medical students hurried behind him.
“This is a real war,” Varon said. “And it’s a war that has more intricate elements, because what we’re dealing with is patients coming to terms with having it,” he said of the virus. “People don’t like to believe they have this illness.”
The first patient he checked was Rochelle Hodges, 43, a call center operator. She had returned to the unit the day before after leaving against his advice, potentially exposing others.
The doctor leaned within inches of Hodges’ face to be heard as his staff helped her sit up. They eased her long brown ponytail aside and gingerly lowered her hospital gown to slide an ultrasound wand across her chest. Her lungs appeared on a black-and-white monitor, inflamed.

Dr. Joseph Varon is fighting COVID-19 as Texas reopens and admissions increase.
Nurses reviewed her chart and jotted down her vital signs on one of few available surfaces — the white legs of their Tyvek suits, which they would wear until the end of their 12-hour shifts.
“How are you feeling, baby?” Varon asked, touching Hodges’ shoulder. “You look much better.”
Hodges frowned. “When I get up and try to walk, I’m short of breath.”
The doctor reassured her that she was healing. By the time he moved on, Hodges was smiling.
Varon checked on a woman who had arrived at the hospital days before seeking narcotics, needle pricks in her arms, only to be diagnosed with COVID-19.
Then he visited a jail guard a few doors down who may have been exposed at work. At least 229 county jail employees had contracted COVID, one inmate had died, and of 800 others tested, 40% were positive, making the jail a national hot spot for infections.
Next, the doctor greeted Melequiades Cervantes, a cook at an Italian restaurant.
“How are you feeling?” Varon asked in Spanish as nurses lowered Cervantes’ gown for his chest ultrasound.
Cervantes, 43, had been hospitalized 11 days. He said he felt well enough to return to work to support his wife and four kids.
But he could barely sit up in bed. On the ultrasound monitor, Varon saw blood clots that could cause a stroke.
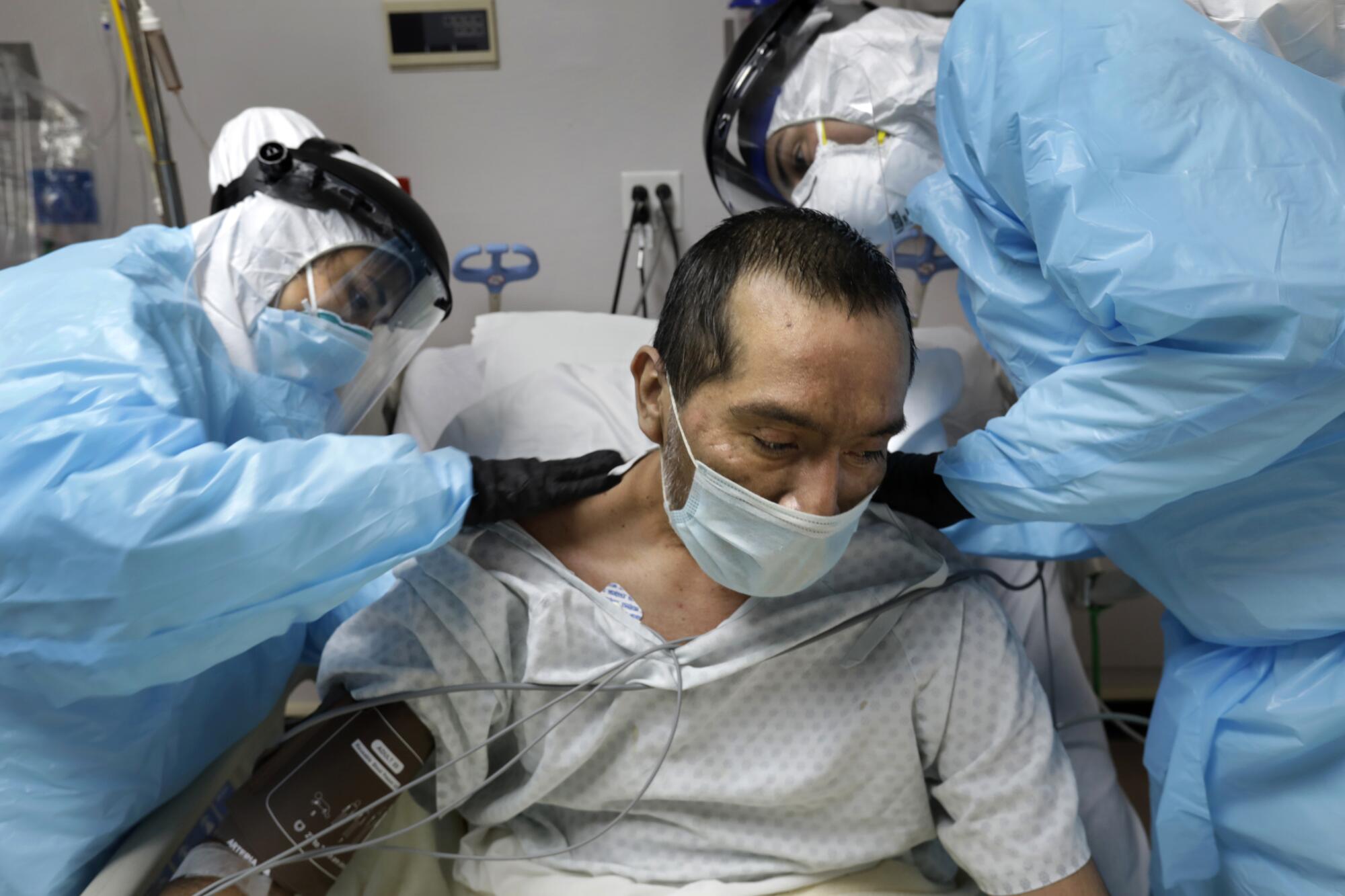
The doctor decided Cervantes would have to stay a bit longer.
“Little by little, you’re getting better,” said Anita Pandey, 26, the hospital’s chief nursing officer.
Cervantes was not put on a ventilator. Though the breathing machines have become commonplace, Varon fears that if a ventilator is required, a patient’s chances of survival are only about 20%.
As he passed the rooms of his patients, they could be heard chatting on cellphones and watching television programs in English and Spanish. Nurses had their own children draw pictures to decorate the rooms, with crayoned messages like, “Be paciant. You will survive.”
So far, all 50 patients treated on the unit have lived.
“I don’t know what place in the U.S. knows more about COVID than this little hospital — the treatment and the social issues,” Varon said.
The next patient, Ira Brown, a 67-year-old wrecker truck driver, insisted he didn’t have the virus even though his chest scans showed telltale lung damage.
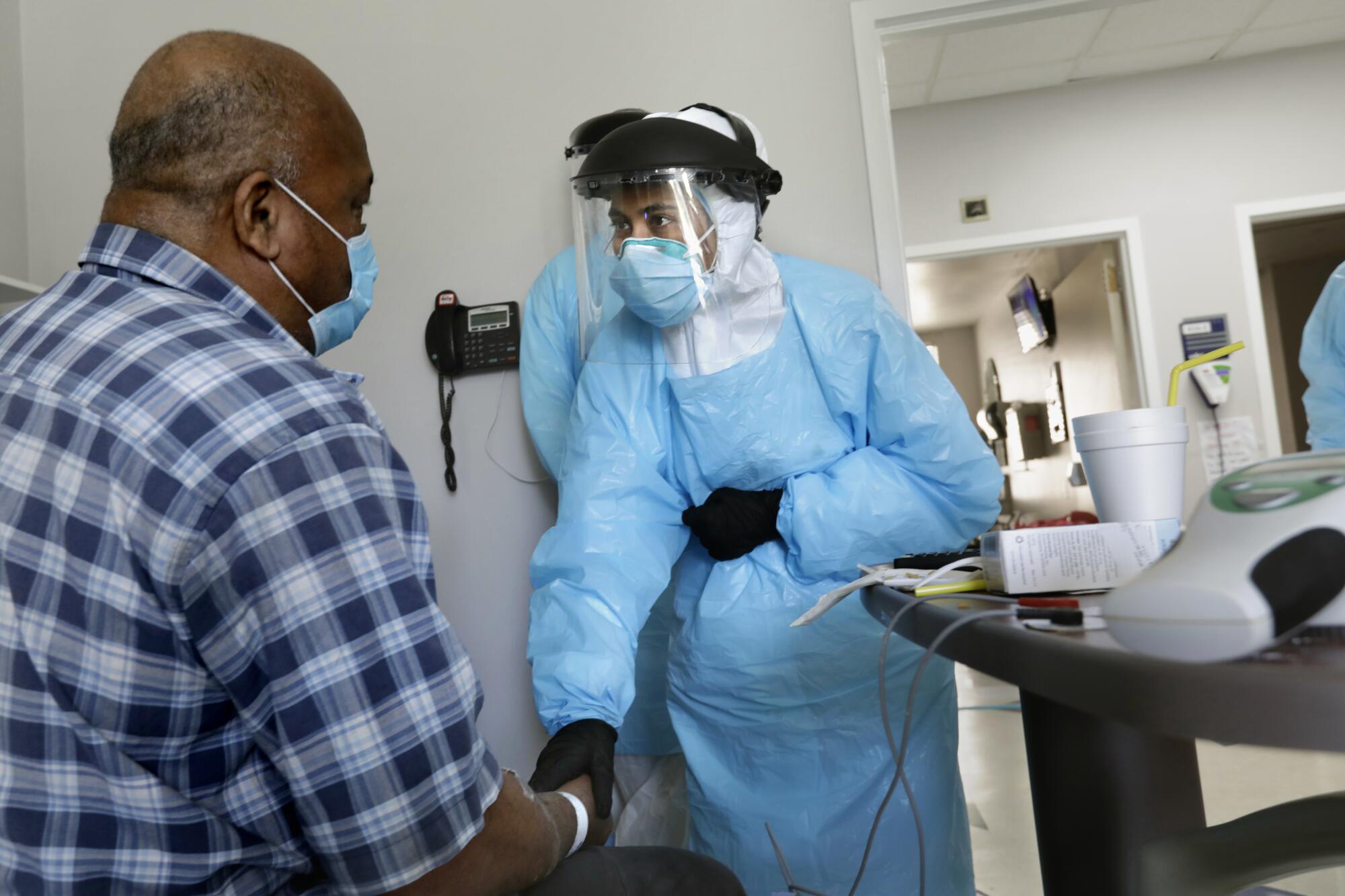
“Now everyone thinks they’re a COVID expert,” Varon muttered, shaking his head.
Before finishing morning rounds, the doctor stopped to check a senile woman. She was still on oxygen, but ready for discharge. The problem: The nursing home where she lived refused to accept her because she’d had COVID.
“We cannot find a place for her. No nursing home wants her,” Varon said.
After morning rounds, Pandey settled into the nurses’ station to contact nursing homes that might accept the woman.
COVID stigma also made it difficult to staff the unit. When it opened, three nurses quit. Almost all of the hospital’s respiratory therapy department stayed home. Varon has relied on loyal nurses, temps and a slew of medical student volunteers like Alan Araiza.

Araiza, 24, had traveled from Tijuana, where he attended school. He has been sleeping in a vacant hospital room since March 29. Sometimes Pandey naps nearby, when she manages to sleep at all.
After making a few more calls without success to nursing homes, Pandey reentered the COVID unit for a task everyone enjoys: Preparing a patient for discharge.
Ruth Medrano had spent nearly a week in the unit. Medrano, 46, was eager to return to her disabled 20-year-old daughter. In Spanish, Pandey explained that Medrano would need to quarantine for at least a week, take her medications and visit the hospital’s outpatient COVID clinic.
“Can I go to the store? I don’t have anything to eat at home,” Medrano said.
The nurse said she could, but to wear a mask.
Medrano also requested a letter clearing her to return to work as a waitress. Pandey agreed as Varon scrawled “Qué te mejores!” (Get well) on a trophy certificate he awards every discharged patient: “Nice try COVID — I survived.”


Varon posed for a photo with Medrano before gathering with staff to watch her walk out. They all applauded.
Varon received a similar certificate from his family after he survived a stroke six years ago.
He worries those who leave without finishing treatment could die. He worries as well for those who never seek treatment at all. Texas has the most uninsured people in the country and has refused to expand Medicaid.
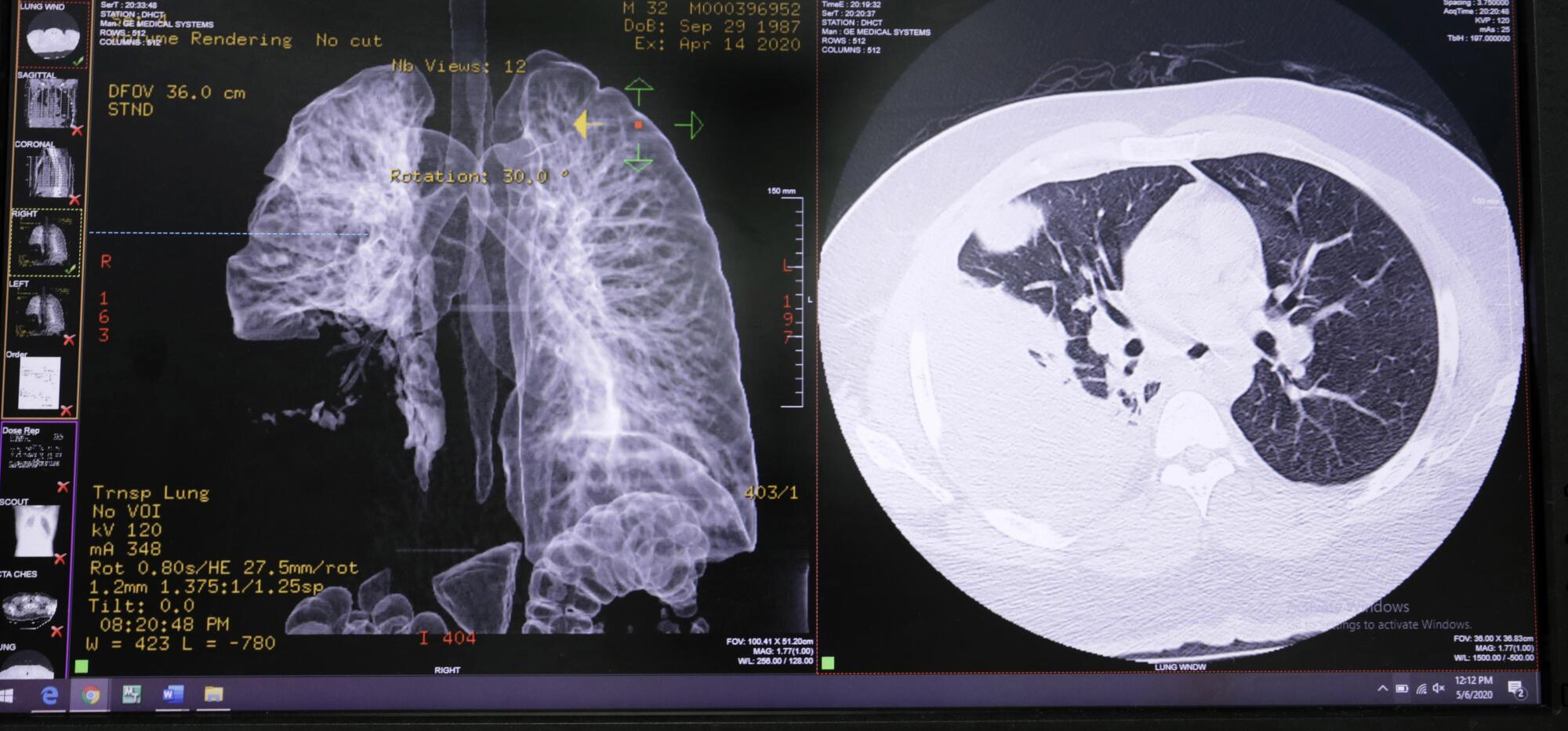
Varon wheeled out a monitor to review patient lung and heart scans. Brown’s lungs were crisscrossed with damage, Varon said, pointing to a web of white lines. Another scan showed Brown’s heart was enlarged, with a large clot.
“He’s going to drop dead if he goes home,” Varon said.
As for Cervantes, the medical team noted that he had a low platelet count, which made giving him blood thinners a risk. But his blood clots also were life threatening. The team gathered around his scans, debating what to do.
“Let’s wait 24 hours,” Varon said.
Pandey reentered the COVID unit to inform patients that they would not be leaving yet.
Cervantes agreed to stay, grudgingly shaking Pandey’s hand.
The nurse moved a few doors down to Brown, who was irate.
“I’m not sick like some other people,” he said, exasperated.
The nurse asked if he had been exposed to anyone with COVID. Brown said he had not left home since the pandemic started except to try to refill his blood pressure medication, unsuccessfully. That’s why he came to the hospital, to fill that prescription.
Pandey urged him to stay. He dismissed her suited figure, saying, “All of y’all look alike.”
“Tell the doctor I’m going to leave whether you want me to or not. I’m walking out of here,” he said.
Pandey called in temp nurse Sherron Lovelady to try to reason with him. Lovelady, 53, is African American like Brown. She had just lost her 79-year-old father, a nursing home patient, to suspected COVID.
Just stay until morning, she pleaded. Brown was still hooked to an IV.
“Are you going to take it out, or am I?” he said.
Face shields, double masks, gloves and shoe covers: How we covered patients infected with the coronavirus.
At the same time, across the hospital, Varon admitted another COVID patient to the emergency room, a 40-year-old man with extremely low blood oxygen.
“This is probably one of the worst we have seen,” Varon said. “If this guy did not come here, he would be dead.”
Eliazar Angel Rodriguez, a mover and father of two, had driven himself to the hospital’s COVID outpatient clinic. He said an ambulance dispatcher had refused transport, telling him, “We will not take you to the hospital unless you are gasping on the floor and turning purple.”
Varon fumed. He vowed to contact the ambulance company to investigate, but wasn’t optimistic. Not everyone was willing to treat the uninsured and hope for reimbursement from the government, as his hospital was.
“We have to tell people to come straight here, not to call an ambulance,” he told his staff.
In the COVID unit, Pandey and Araiza attached a blood oxygen monitor to Rodriguez’s finger and slowly flipped him onto his belly to keep his airways clear. He could barely hold his head up as they attached an oxygen tube to help him breathe and an IV that pumped him with a unique cocktail of medication.
By the next day, he would be sitting up, talking, eating and watching telenovelas. So would Cervantes.
Varon has been fine-tuning his COVID treatment with Dr. Joseph Gathe Jr., 63, a local infectious disease specialist who pioneered HIV treatments in the 1980s.
They‘ve started a nonprofit foundation to test and treat the uninsured for COVID. While the Centers for Disease Control and Prevention explores vaccines and alternative treatments, Varon said, “we have to make our own way.”
Varon, who has also been consulting with colleagues in China, Italy and Spain, employs a treatment of steroids, blood thinners, Vitamin C and hydroxychloroquine, one of the drugs touted by President Trump.
But an effective treatment is useless if a patient refuses care. Texas COVID patients who try to leave against doctors’ advice have not been ordered hospitalized by the courts, although those with tuberculosis have, Varon noted.
Some COVID patients left his hospital’s outpatient clinic last week when the line grew too long, dumping admission paperwork in the hedge outside.
Nurses could only watch as Brown pulled out his IV and left the isolation unit, blood trickling down his forearm. He made it as far as the parking lot before staff persuaded him to return inside to clean up and complete discharge paperwork.
As he signed out, nurse Tanna Ingraham sat in the nurses station holding her tongue behind a rhinestone-studded Dallas Cowboys mask.
Her great uncle had just died of COVID. Ingraham, 42, had been staying in a hotel to protect her immunocompromised mother and two young daughters.
“Please wear a mask,” Ingraham told Brown. “And if you feel sick, call.”
She waited until Brown sauntered out before retreating to the break room, muttering, “I want to cry.”
“With this second wave coming, people are in denial,” she said, reheating a plate of roast beef from the hospital cafeteria.
Lovelady joined her. “I just have a feeling that man’s last breath will be gasping for air,” she said.
The next morning, Brown would indeed awake unable to breathe.
He rushed to the hospital and was readmitted, still refusing to believe he had the virus, even after Gathe visited and confirmed his diagnosis.

A week earlier, Lovelady’s temp agency had called to ask, “Do you do COVID?” She wasn’t sure. She had handled complicated cases: HIV patients, drug addicts and adults with disabilities. But if she worked on the unit, she would have to isolate from her family, including her first grandchild, a newborn. Still, she said yes.
The first time the nurse suited up for the COVID unit, she felt lightheaded and had to will herself not to pass out. But she discovered that aiding the isolated patients helped her grieve for her father. By the end of this, her first six-day week of 12-hour shifts with few breaks, Lovelady had reached a decision: She wanted to work the COVID unit full time.
Before leaving the nurses’ station last Friday, even as she longed to hit the shower and grab a beer, Lovelady stopped to ask if the team would need her to work Sunday, Mother’s Day. Maybe, a manager said.
Lovelady’s late father used to organize a family brunch to celebrate the holiday. But now she felt like she belonged on the COVID unit. She would wait on call.
The following night, she got a message: The COVID unit needed her. And so, she worked Mother’s Day.

More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.










