Dexamethasone can improve COVID-19 survival, study shows
- Share via
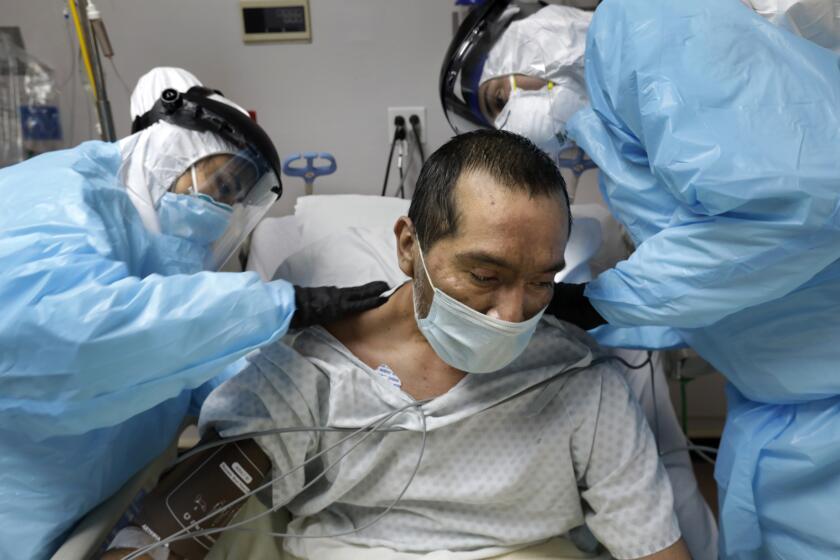
In a development that could dramatically shrink the death toll of the COVID-19 pandemic, British researchers have found that a cheap and readily available steroid prevented more than a third of the sickest patients from dying.
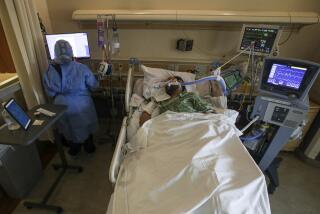
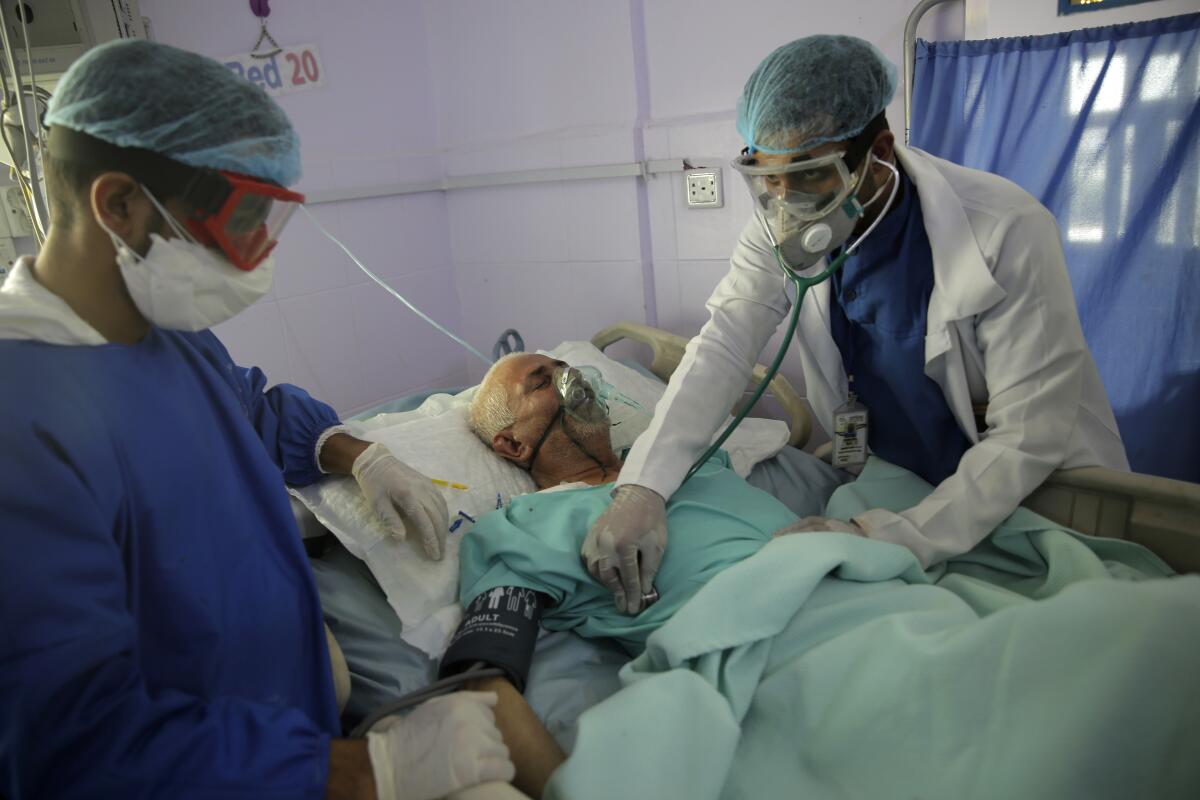
In a large group of coronavirus-infected patients who required mechanical ventilation to breathe, a 10-day course of dexamethasone drove down mortality by 35%, researchers from the University of Oxford announced Tuesday. In patients whose illnesses were less extreme, but who still required supplemental oxygen, the steroid treatment reduced death rates by 20%.
If the preliminary findings hold up to scrutiny by other researchers, dexamethasone would become the first lifesaving drug treatment for COVID-19 patients. Only one other medication — the antiviral drug remdesivir — has proved effective in a rigorous clinical trial, but its benefit was limited to shortened recovery time.
However, experts were adamant that the steroid would be dangerous for patients with early-stage infections and milder symptoms. If people are tempted to use it inappropriately, it “will cause much sicker patients,” said Dr. Steven J. O’Day, director of regional research at Providence St. John’s Health Center in Santa Monica.
Dexamethasone is a corticosteroid that mimics the effect of cortisol, a hormone produced by the adrenal glands. The drug powerfully tamps down inflammation and is prescribed to treat skin diseases, allergic reactions, autoimmune diseases and rheumatoid arthritis.
The steroid “is the first drug to be shown to improve survival in COVID-19,” said Oxford University’s Dr. Peter Horby, an infectious-diseases expert and one of the clinical trial’s chief investigators. “The survival benefit is clear and large in those patients who are sick enough to require oxygen treatment, so dexamethasone should now become standard of care in these patients.”
Dexamethasone, he added, “is inexpensive, on the shelf, and can be used immediately to save lives worldwide.”
Doctors who weren’t involved in the trial shared Horby’s enthusiasm.
“This is unbelievably exciting,” said Dr. Craig Coopersmith, director of Emory University’s critical care center. For patients with such a high risk of dying, a one-third reduction in mortality is “remarkable,” he said.
Cities and states are pressing ahead with plans to do so. But has anything changed about the coronavirus that makes it safer to go out now?
Experts stressed that the reported benefits of dexamethasone or any other steroid are limited to coronavirus patients whose symptoms have become very severe.
Corticosteroids inhibit the production of T cells, a type of white blood cell that the immune system relies upon to fight a coronavirus infection. With fewer T cells at work, the treatment could actually backfire by making a person more vulnerable to infection, O’Day cautioned.
“Steroid use in early viral disease is exactly what you don’t want,” he said.
Critical care physicians were heartened by a finding that could aid their sickest patients, whose prognoses are bleak. Roughly 40% of COVID-19 patients who need the aid of a mechanical ventilator will die of the disease, and a passel of clinical trials has so far turned up nothing in the way of effective treatments.
At the same time, physicians responded cautiously to the glowing study findings that were summarized in a news release rather than published in detail in a medical journal, as is customary.
“The results do need to go through peer review, and some physicians will wait for that to change their practices,” Coopersmith said. “But I imagine some will change their practice literally today.”
Dr. Mark Hepokoski, a critical care specialist at UC San Diego’s School of Medicine, said that if the study’s preliminary results stand up to review by independent scientists, “it would give me a lot of comfort that there’s a treatment I can offer to our sickest patients.”
As a physician whose patients have varying income levels, he added, “it’s reassuring not only that it works, but that it’s affordable and in large supply.”
From the opening days of the pandemic, doctors caring for hospitalized COVID-19 patients have been buffeted by conflicting views over the value of steroid medications.
COVID-19 most closely resembles two forms of critical illness that are widely treated in intensive care units. One of them is septic shock, a diagnosis for which steroid medications are viewed as helpful. The other is acute respiratory distress syndrome, a diagnosis for which steroids are often avoided.
“You put that together and you get, ‘We don’t have any idea what to do,’” Coopersmith said.
If the study’s findings prove accurate, the strength of dexamethasone’s effect and the clarity of the results will make it a “game changer,” he added, noting that he does not use the term lightly.
COVID-19 has killed more than 100,000 people in the U.S., but some are more vulnerable than others. These charts show how Americans have been affected.
The new results emerged from a clinical trial in the United Kingdom called Randomized Evaluation of COVID-19 Therapy, or RECOVERY. This arm of the RECOVERY trial included 2,104 patients who got dexamethasone, and 4,321 who received the care routinely administered in hospitals throughout the United Kingdom.
The results of the British study suggest a 10-day regimen of dexamethasone would prevent the death of 1 in 8 mechanically ventilated patients. Among patients who require supplemental oxygen alone, roughly 1 in 25 patients could be saved by the treatment.
The drug’s use is not without risks. By tamping down a key immune system response, it can make extremely ill patients more susceptible to opportunistic fungal and bacterial infections, which can be fatal. It can make patients’ blood sugar difficult to regulate, and when used in patients who are heavily sedated and on a respirator, it can increase the risk of profound muscle weakness.
In patients who are not critically ill, or in circumstances where the benefit of treatment is uncertain, those risks would discourage the steroid’s use.
While dexamethasone is sometimes used already in critically ill patients, the new findings might prompt critical care specialists who have saved it as a last resort to turn to it sooner, Hepokoski said. That might spare some patients the need for mechanical ventilation, he said.
Several experts stressed that dexamethasone could be all the more powerful for its wide availability and small price tag. At a time when the world’s richest nations are sparing no expense to develop new therapies for COVID-19, there is widespread concern that lower-income countries will be left behind.
Dexamethasone “is highly affordable, easy to make, can be scaled up quickly and only needs a small dosage,” said Dr. Nick Cammack, who directs COVID-19 research programs supported by the British philanthropy Wellcome Trust. “Finding effective treatments like this will transform the impact of the COVID-19 pandemic on lives and economies across the world.”