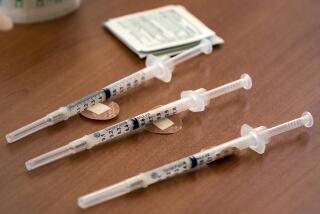
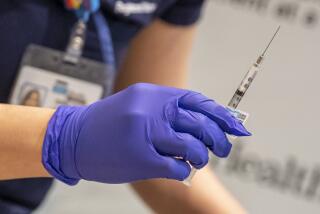
Pfizer says early data suggest its COVID-19 vaccine is 90% effective
Pfizer says early data on its coronavirus vaccine suggest that the shots may be 90% effective at preventing COVID-19.
- Share via
Pfizer says early data on its COVID-19 vaccine candidate suggest the shots may be 90% effective at preventing the disease, indicating the company is on track later this month to file an emergency-use application with U.S. regulators.
Monday’s announcement, which came less than a week after a presidential election that was seen as a referendum on President Trump’s handling of the coronavirus crisis, is a rare and major piece of encouraging news in the battle against a scourge that has killed more than 1.2 million people worldwide, including almost a quarter of a million in the U.S. alone.
Pharmaceutical companies and various countries are in a global race to develop a vaccine.
“We’re in a position potentially to be able to offer some hope,” Dr. Bill Gruber, Pfizer’s senior vice president of clinical development, told the Associated Press. “We’re very encouraged.”
Dr. Anthony Fauci, the government’s top infectious-disease expert, said the results suggesting 90% effectiveness were “just extraordinary,” adding: “Not very many people expected it would be as high as that.”
“It’s going to have a major impact on everything we do with respect to COVID,” Fauci said.
Pfizer’s announcement doesn’t mean a vaccine is imminent. This interim analysis, from an independent data monitoring board, looked at 94 infections recorded so far in a study that had enrolled nearly 44,000 people in the U.S. and five other countries.
Pfizer did not provide any more details about those cases, and cautioned that the initial protection rate might change by the time the study ended. Even revealing such early data is highly unusual.
Authorities have stressed that it’s unlikely any vaccine will arrive much before the end of the year, and limited initial supplies will be rationed.
“We need to see the data, but this is extremely promising,” said Dr. Jesse Goodman of Georgetown University.
The CEO of Pfizer said he won’t bend to pressure from the Trump administration to release a COVID-19 vaccine before it is warranted by science.
He ticked off many questions still to be answered, including how long the vaccine’s effects last and if it also protects older people as well as younger people.
If Pfizer’s vaccine does pan out, “it’s going to be a while before this has a major impact at the population level,” said Goodman, a former chief of Food and Drug Administration’s vaccine division.
Initial supplies of any COVID-19 vaccine will be scarce and rationed, with priority likely given to healthcare workers and others on the front lines. Pfizer has estimated that 50 million doses of its vaccine could be available globally by the end of 2020, which would cover 25 million people, since it is given in two doses.
Global markets, already buoyed by the victory of President-elect Joe Biden, exploded on the news from Pfizer. Trump, who had suggested during the presidential campaign that a vaccine could be ready by election day, tweeted: “STOCK MARKET UP BIG, VACCINE COMING SOON. REPORT 90% EFFECTIVE. SUCH GREAT NEWS!”
Pfizer Chairman and CEO Albert Bourla said on CNBC that the election was an artificial deadline and that the data would be ready when they were ready. Independent data monitors met Sunday, analyzing the test results so far and notifying Pfizer.
“I am very happy,” Bourla said, “but at the same time, sometimes I have tears in my eyes when I realize that this is the end of nine months’ day-and-night work of so many people and how many people — billions — invested hopes on this.” He added: “I never thought it would be 90%.”
Earlier this year, Fauci said he would be happy with a vaccine that was 60% effective. Scientists have warned for months that any shot may be only as good as flu vaccines, which are about 50% effective and require yearly shots.
The U.S. has signed a contract with Pfizer for delivery in December of the first 100 million doses of a COVID-19 vaccine the company is developing.
Biden, whose first public act in readying a new administration was the announcement of a new COVID-19 task force Monday, said in a statement that Pfizer’s data were a “cause for hope.” But he warned that it would “still be many more months before there is widespread vaccination in this country.”
Pfizer opted not to join the Trump administration’s Operation Warp Speed, which helped half a dozen drugmakers accelerate their vaccine testing and helped fund the work. Instead, Pfizer funded all its testing and manufacturing costs itself. The company said it had invested billions of dollars.
The shots made by Pfizer and its German partner, BioNTech, are among 10 possible vaccine candidates in late-stage testing around the world — four of them so far in huge studies in the U.S. Another U.S. company, Moderna, also has said it hopes to be able to file an application with the Food and Drug Administration later this month.
Volunteers in the final-stage studies and the researchers don’t know who received the real vaccine or a dummy shot. But a week after the volunteers’ second required dose, Pfizer’s study began counting how many of them developed COVID-19 symptoms and were confirmed to have the coronavirus.
Because the study hasn’t ended, Gruber could not say how many in each group had infections. Doing the math, that would mean almost all the infections counted so far had to have occurred in people who received the dummy shots.
Pfizer does not plan to stop its study until it records 164 infections among all the volunteers, a number that the FDA has agreed is enough to tell how well the vaccine is working. The agency has made clear that any vaccine must be at least 50% effective.
No participant so far has become severely ill, Gruber said. He couldn’t provide a breakdown of how many of the infections had occurred in older people, who are at highest risk from COVID-19.
Participants were tested only if they developed symptoms, leaving unanswered whether vaccinated people could get infected but show no symptoms and unknowingly spread the virus.
The FDA has required that U.S. vaccine candidates be studied in at least 30,000 people. In addition to adequate numbers of older adults, those studies must also include other groups at high risk, including minorities and people with chronic health problems.
And the agency has told companies that they must track half their participants for side effects for at least two months, the time period when problems typically crop up. Pfizer expects to reach that milestone later this month, but said Monday that no serious safety concerns had been reported so far.
Because the pandemic is still raging, manufacturers hope to seek permission from governments around the world for emergency use of their vaccines while additional testing continues — allowing them to get to market faster than normal but raising concerns about how much scientists will know about the shots.
The FDA’s scientific advisors last month said they were worried that allowing emergency use of a COVID-19 vaccine could damage confidence in the shots and make it harder to find out how well they really work. Those advisors said it was critical that these massive studies run to completion.