FDA allows first emergency use of a COVID-19 antibody drug

- Share via
WASHINGTON — U.S. health officials have allowed emergency use of the first antibody drug to help the immune system fight COVID-19, a disease that has killed more than 238,000 Americans.
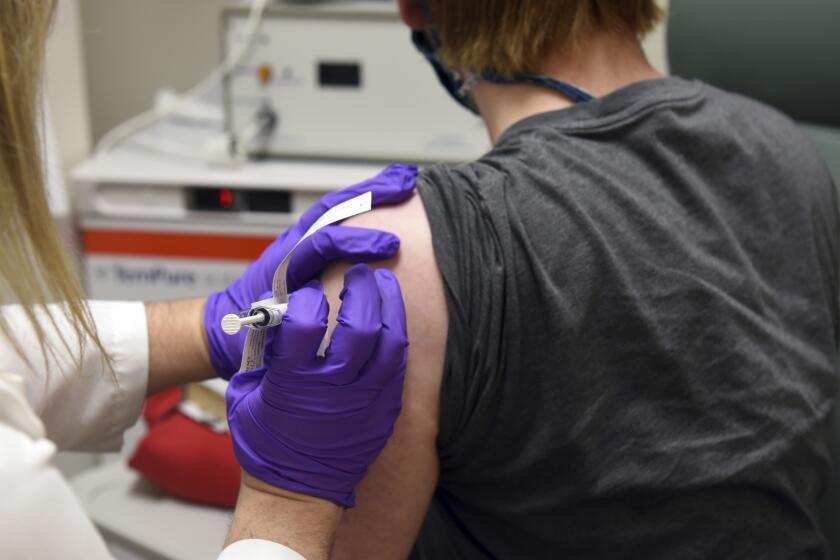
The Food and Drug Administration on Monday cleared the experimental drug from Eli Lilly for people 12 and older with mild or moderate COVID-19 who do not require hospitalization. The one-time treatment is given through an IV.
The therapy is still undergoing additional testing to establish its safety and effectiveness. It is similar to a treatment President Trump received after contracting the virus last month.
Lilly’s studies of the antibody drug are continuing. Early results suggest it may help patients clear the coronavirus sooner and possibly cut hospitalizations in people with mild to moderate COVID-19.
A study of it in hospitalized patients was stopped when independent monitors saw that the drug did not seem to be helping in that situation.
The government previously reached an agreement to buy and supply much of the early production of the Lilly drug, known as bamlanivimab.
One other treatment has an emergency use designation now — convalescent plasma, which comes from the blood of COVID-19 survivors. No large studies have shown it to be more effective than usual care alone, however.
Scientists searching for a medicine to treat patients with COVID-19 are looking for it in the blood of people who have already survived the disease.
The new drug is part of an emerging family of biologic therapies that offer a promising new approach to preventing serious disease and death from COVID-19. Experts say the infused drugs could serve as a therapeutic bridge to help manage the virus until vaccines are widely available.
The drugs are laboratory-made versions of antibodies, blood proteins that the body creates to help target and eliminate infections. The new therapies are concentrated versions of the antibodies that proved most effective against the virus in patient studies.
Regeneron Pharmaceuticals Inc. also has asked for emergency authorization for the antibody drug it is testing, which Trump received and later touted.
FDA regulators authorized the Lilly drug using their emergency powers to quickly speed the availability of experimental drugs and other medical products during public health crises.
Pfizer says early data on its coronavirus vaccine candidate suggest that the shots may be 90% effective at preventing COVID-19.
In normal times the FDA requires “substantial evidence” to show that a drug is safe and effective, usually through one or more large, rigorously controlled patient studies. But during public health emergencies, the agency can lower those standards and require only that an experimental treatment’s potential benefits outweigh its risks.
The emergency authorization functions like a temporary approval for the duration of the COVID-19 pandemic. To win full approval, Lilly will have to submit additional research to fully define the drug’s safety and benefit for patients.
The government has signed an agreement with Lilly to spend $375 million to buy 300,000 vials of the drug. How many doses that would provide is unclear. Each vial contains 70 milligrams, and that dose proved ineffective in the early results. It took four times that amount — 2,800 milligrams — to show any effect.