Thinking about a C-section? Here’s why your hospital may say no.
- Share via
At hospitals across California, administrators are pushing doctors to perform fewer caesarean deliveries, hiring birth coaches and asking pregnant women to stay in labor longer.
For years, medical experts have said that C-sections — a surgical procedure in which a doctor makes an incision in the mother’s abdomen and uterus to remove the baby — were being done too often, yet the rates kept climbing.
In 2014, however, delivery hospitals in California reduced the number of C-sections performed by more than 1,000 compared with 2013, according to a Times analysis of new data.
DATABASE: Look up your hospital's C-section rate >>
What’s changed recently, some experts say, is the nature of the healthcare system, which focuses increasingly on eliminating unnecessary expenses. In the era of the Affordable Care Act and its emphasis on low-cost medical care, C-sections — which cost more than vaginal deliveries — have become a sticking point for hospitals and a target for the people paying the bills.
Childbirth is the most common reason for hospitalization in the U.S., said Katy Kozhimannil, a health policy professor at the University of Minnesota, so when insurers and self-insured employers “look at where their costs are going, you start to see caesarean delivery rises to the top.”
Hospitals not only face direct pressure from insurers to curb C-sections, but they’re also concerned that a high rate could affect business. As more data on medical facilities is available to patients, hospitals don’t want to fall to the bottom of the pack and lose patients who see higher C-section rates as unfavorable.
Dr. Allyson Brooks, an obstetrician and chief quality officer at Hoag Memorial Hospital Presbyterian in Newport Beach, remembers that a few years ago the hospital was under fire from its insurer because of a higher-than-average C-section rate.
In California, maternal care plus a vaginal delivery cost commercial insurers $15,259 on average, while maternal care plus a C-section cost $21,307, according to a report commissioned by the Center for Healthcare Quality and Payment Reform, a nonpartisan research center.
Over the last two decades, many U.S. doctors began opting for C-sections in part out of convenience, because the procedure is often much quicker than waiting for a woman to deliver vaginally, experts say. Some patients chose to have C-sections— a trend made famous by celebrities in the 2000s and labeled “too posh to push.”
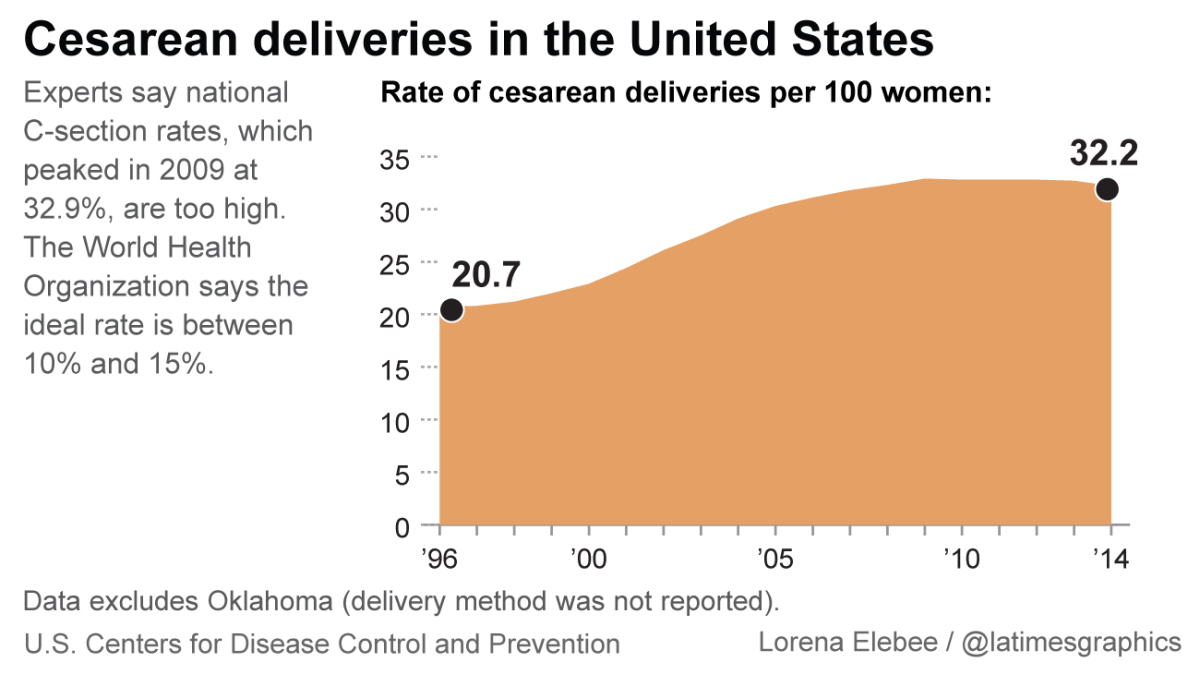
Though generally safe, C-sections are still invasive surgeries, with a longer recovery time than vaginal deliveries. And once a woman has one C-section, she has a 90% chance of delivering her next babies by C-section. The World Health Organization says the ideal C-section rate is around 15% but in the U.S. it reached 32.9% in 2009.
The rates were influenced by factors such as the culture of the hospitals and type of community it serves. Three years ago, Brooks recalled seeing posts on social media by Orange County residents such as, “If you want to have a vaginal delivery go to a different hospital, if you want to have a C-section go to Hoag.”
Brooks said that though most obstetricians agree C-section rates are too high, it can be difficult to get them to consider doing fewer. They worry that trying to bring down rates will harm women. C-sections can be necessary if the umbilical cord is dangerously tied around a baby’s neck, or a woman’s uterus is at risk of rupturing.
So she began calculating a low-risk, or NTSV, C-section rate for her hospital. It includes only women considered the least likely to need C-sections — first-time mothers, having a single baby around their due date, and carrying a baby positioned head down.
The U.S. surgeon general has called for reducing the low-risk C-section rate to 23.9% by 2020.
Hoag began requiring that doctors show clear medical reasons to induce labor in women, and also started calculating and sharing each doctor’s low-risk C-section rate.
At Hoag, the low-risk C-section rate dropped from 31% in 2013 to 26% in 2014, one of the biggest declines in the state.
And it wasn’t just Hoag. From 2013 to 2014, the rate of C-sections among low-risk moms in California dropped from 27.3% to 26.1%, a reduction of 1,219 procedures statewide, according to data released last month by the California Hospital Assessment and Reporting Task Force and analyzed by The Times.
The analysis also found that the percentage of California’s 244 delivery hospitals that met the surgeon general’s goal jumped from 32% to 42% between the two years.
Hoag negotiated with its insurer to be paid an equal rate for C-sections and vaginal deliveries so it wouldn’t lose money when rates dropped.
But other hospitals that have brought down their C-sections rates have faced financial consequences.
The six Providence Health & Service hospitals in Southern California took a revenue hit from doing fewer C-sections, said Regional Chief Medical Officer Michael Bernstein. They also spent money hiring obstetricians to staff the labor and delivery wards in shifts, so doctors wouldn’t feel rushed and opt for C-sections because they’re quicker procedures.
Bernstein said he thinks the change is better for patients and could be good for the hospital group in the long run.
Increasingly, under changes set into place by the Affordable Care Act, hospitals aren’t paid per treatment, but based on the quality of the care. Hospital leaders say C-section rates could become one of the metrics used in such calculations.
But Dr. Aaron Caughey, chair of the Department of Obstetrics and Gynecology at Oregon Health & Science University School of Medicine, said there’s no single low-risk C-section rate that all hospitals should aim for, and that rates will vary from hospital to hospital because of differences in the patient population.
“I would hate it if Medicaid said, ‘Every hospital whose rate is above the median, we’re not going to pay you a chunk of money.’ That is a bad approach because then people squeeze it down without attention to what’s best for patients,” Caughey said.
Even if hospitals aren’t being officially penalized for high C-section rates, administrators are worried about the financial effect of losing patients who want a vaginal birth. Deliveries aren’t big moneymakers for hospitals, but once a hospital treats a mother, it's likely to care for the rest of her family in the years to come.
Some mothers say that they felt as if their physicians rushed into C-sections, and they don’t want to repeat the experience.
When Anastasia Stone, 32, was pregnant with her first child, her doctor told her she needed to be medically induced to begin labor, which resulted in a C-section. “I was a typical first-time mom,” she said.
Stone, who lived in Santa Cruz at the time, said she later came to believe she could’ve had a vaginal delivery instead of a C-section if her physician had waited.
When she was pregnant with her second child, Stone went looking for a doctor who would try for a vaginal birth.
Dr. William Gilbert, regional medical director for women’s services at Sutter Health in the Sacramento region, said Sutter Davis Hospital has drawn such women from around the Sacramento area because it had the lowest C-section rate in the state in 2014 — 12%.
| Hospital | City | C-sections | Deliveries | Rate |
|---|---|---|---|---|
| Sutter Davis Hospital | Davis | 71 | 598 | 12.0% |
| Emanuel Medical Center | Turlock | 51 | 391 | 13.0% |
| Mammoth Hospital | Mammoth Lakes | 5 | 43 | 14.0% |
| Sonoma Valley Hospital | Sonoma | 7 | 49 | 14.3% |
| Bakersfield Memorial Hospital | Bakersfield | 174 | 1170 | 15.0% |
The hospital uses nurse midwives, who deliver most of the babies, and reserves obstetricians for backup. Birth is treated as a natural process instead of a “health condition” that always requires medical intervention, said Carolyn Campos, nursing manager of the hospital’s birthing center.
Gilbert thinks that as more data on specific rates of procedures or treatments is available, patients will increasingly turn to that information when choosing where to seek care.
In 2014, low-risk C-section rates ranged from 12% to 70% at California hospitals.
Six years ago at Sutter Medical Center, Sacramento, Gilbert began encouraging physicians to allow longer labor in women, and began posting each physician’s low-risk C-section rate in the doctors’ lounge. From 2010 to 2014, the hospital’s low-risk C-section rate dropped from 31% to 27%.
Gilbert thinks that most of the success came from publishing the doctor’s rates internally.
“Doctors don’t want to be the highest rate,” he said.
soumya.karlamangla@latimes.com
Twitter: @skarlamangla
Twitter: @ryanvmenezes
ALSO
Want to look like super-fit Kate Hudson? You won't get there with quick fixes or fad diets
7 reasons why you're about to fall in love with floating
Now you can dine in or grab healthful goods to go at these L.A. restaurants and juice bars





