Test-Tube Mother: It’s Not Just a Job : An ‘In Vitro’ Surrogate Parts With a Baby Who Was Never Her Own
- Share via
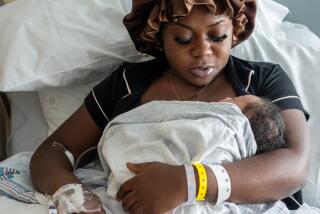
Melia Josephson gave birth to a girl last week. She is partial to baby girls, she admits. But after carrying her for nine months and holding the child for less than a day, she gave the baby away. The reason: Josephson is neither genetically nor legally the child’s mother.
Melia Josephson is the ultimate human vessel. Her baby was conceived by another woman’s egg, fertilized in a laboratory, then transplanted to Josephson’s womb.
The 7-pound, 3-ounce child, whose birth is to be publicly announced at a press conference today, was born at San Antonio Hospital in Upland on July 23. Josephson thus became only the third known surrogate mother in the world to deliver a “test-tube” baby.
The process by which the child was conceived--in vitro fertilization--blends cutting-edge reproductive technology with the already controversial practice of surrogate parenting.
Not surprisingly, it raises profound legal questions. Because California law states that the woman who actually gives birth to the child is its legal mother, motherhood had to be redefined in Josephson’s case, explained attorney William Handel, whose Center for Surrogate Parenting Inc. in Beverly Hills brought the surrogate and donor couple together.
Birth Certificate
Last month, Handel asked a Los Angeles County Superior Court judge to allow the genetic mother, the woman who donated the egg, to be designated as the mother on the birth certificate. Otherwise, he said, she would have been required to adopt her genetic child.
The judge agreed, only the second time any judge in the country has done so, Handel said. “No real legal precedent has been set here,” he said, “since the case is not at the appeals level. But California courts do influence decisions in the rest of the country.”
Melia Josephson is a slightly built redhead whose palpable spunk, ready giggle and all-American good looks trigger images of Gidget--even in her pregnant state.
A few days before the child was born last week, she and her husband, Mark, sat in the den of their new Moreno Valley home near Riverside. As they talked, their own three children dashed through the house to the backyard, where the installation of a swimming pool was nearly complete.
Josephson is being paid $10,000 in installments, for being a surrogate, and the money is being used as a down payment on the pool. “The pool costs a lot more,” she said, calling it a “gift to my family” for supporting her through the surrogate process during the last four years. Some of those years were tense, the couple admitted.
Her desire to become a surrogate mother began after the birth of her last child, Josephson explained. She and her husband had agreed that their third child would be their last. He had a vasectomy.
But her pregnancies and deliveries had been so easy, and the joy of holding a helpless newborn “totally dependent on me” so profound, that she longed to have another child.
“I didn’t actually do anything about those feelings for the first year” after her last child, Ashley, was born, Josephson said. “About 1983, I said, ‘I’ve got to do something about this.”’
Called Every Doctor
She got out the Yellow Pages and called every doctor she thought might know something about surrogate parenting. But none had any information. She told all her neighbors, “I’m thinking about becoming a surrogate, but I can’t find anybody who knows about it.”
Then one afternoon, a neighbor called and told her to turn on the “Donahue” television show. It was a program about the merits of surrogate parenting versus adoption. William Handel, the attorney with the Beverly Hills surrogate center, was one of the guests. Josephson called him after the show.
At the time, the center’s surrogate program did not use in vitro fertilization. All their surrogate mothers were artificially inseminated, as in the widely publicized Baby M case in New Jersey. In other words, the surrogates’ own eggs were fertilized in their bodies with sperm from prospective fathers.
Josephson’s husband balked. “My initial response was negative,” said Mark Josephson, a 30-year-old contractor who owns a wall-covering business. If she had gone ahead, “We would have been divorced.”
“Even to this day, I do not agree with that method (artificial insemination),” he said. “When a woman is inseminated with another man’s sperm and she’s giving half that baby away, it’s half her baby. I couldn’t give my baby away to anybody.”
The 10-year-old marriage already was under strain. In 1981, Josephson had reluctantly dropped out of Brea Police Academy at her husband’s insistence. He didn’t feel she could be a cop and a mother, she said. “When it came down to him or my job,” her husband won hands down, she said. “But I did have to compromise.”
They sought counseling. “We loved each other and wanted to make a go of it,” Melia Josephson said. And when the marriage was on solid ground again, she told the surrogate center that she still wanted to participate--but only if they could find a couple who couldn’t have a child because the wife could not carry the baby.
With that approach, Mark Josephson said, “I had no real concerns.”
“I guess he felt that he had stopped me from doing the one thing in the world I really wanted (being a policewoman),” his wife added. “I think he took the attitude that ‘I can’t stop her from this, too.’ ”
One reason the Beverly Hills center did not have an in vitro surrogate program when Josephson first inquired was cost. According to Handel, couples pay about $33,000 (including the surrogate fee) to have a child by the technique. And that’s if the first attempt is successful. Every attempt to implant an embryo in a surrogate runs an additional $4,000 to $5,000.
Some women are able to produce eggs but cannot carry a child because they have lost their uterus in a hysterectomy. Under the in vitro technique, the woman’s egg is fertilized by the genetic father’s sperm in the laboratory. Then, the tiny embryo is transplanted to the womb of the surrogate mother.
The IVF surrogate, as she is called, is only “nurturing the baby for nine months,” explained Dr. Jaroslav Marik, the infertility specialist who performed the procedure on Josephson. Genetically, the child is completely the donor couple’s.
The center decided to start such a program when it was able to match in vitro technology with a couple able to afford it. It eventually enrolled five surrogate mothers, of which Josephson was the first to be successfully impregnated, in October, 1986.
At first, Josephson said, she “felt like a baby-maker, a rent-a-womb.” In support-group sessions with other women participating in the program, she and the others took the approach: “I’m just here doing a job.”
But none of the other women have become pregnant yet, and Josephson felt distinctly different once she was. “It all changes when you feel it move, when you see it move,” she said.
When tests revealed she was carrying a girl, “it really hit home,” she said. “I hate to admit it, but I’m partial to girls. I started feeling attached. The more she stayed in me, the more attached I became.”
Looking back, she said, if she had been a conventional surrogate, “I couldn’t have gone through it. I think my husband knew that about me and that’s why he didn’t want me to do it that way. Half of me would be out there somewhere with red hair.”
But in the week before she delivered the baby, she had no doubt she’d be able to give up the tiny girl she had nurtured for nine months.
“I’ll be able to say goodby,” she predicted. “But I want lots of pictures. I do want to hold her. I want to do as much as the mother will let me those two or three days in the hospital. Because once they are gone, they are gone forever, and all I’ll have is the memory.”
Her time with the child was not measured in days but in hours.
As with all her pregnancies, she had an easy delivery. Labor had to be induced since she was a week overdue. But “three good pushes, and the baby was born” she said laughing the next day.
The baby’s genetic parents, a woman 40, and a man 38 who live on the Westside and asked not to be identified, had expected Josephson’s hospital stay to be longer. “But Melia was ready to go home the next day,” said the mother, and there wasn’t any need to keep the baby at the hospital longer.
As she spoke over the telephone, excited voices could be heard in the background. “Yes,” she explained, “we have a very active house.”
She has a daughter, 15, and a son, 17, from a previous marriage. She and her second husband decided to have a child through the in vitro surrogate process because although she had had a hysterectomy, they wanted another child. “We have two kids that are wonderful,” but it would have been “nice” for her husband “to have had a child of his own.”
“We personally have tried to protect our privacy through this whole matter,” said her husband, joining the conversation. “But we are interested in getting the message of the in vitro surrogate process out.”
Dr. Robert Aramada, the obstetrician who delivered the baby, cautioned that “there are still a lot of things we don’t know in the in vitro surrogate process. Everything went fine in Josephson’s case, but the “body is a complex thing,” he said. There is always the possibility, for instance, that the surrogate mother’s body will reject the embryo because it is not from her egg.
Emotionally, Armada said, the in vitro surrogate has to cope with all the hormonal and psychological changes wrought by a pregnancy with even less to show for it than the conventional surrogate--no child and absolutely no genetic connection to it.
“But Melia and her husband are good, they understand each other,” Armada said. “They have talked this through over and over again. He will support her, and they have had psychological help throughout this. For any other mother it would be difficult. But she has what it takes.”
Josephson will return to work as a part-time bank teller in September. Her husband, who describes himself as a “bad Jew” and his wife as a “bad Catholic,” said he saw nothing morally wrong with surrogate parenting, though it has been condemned by many religious leaders.
When Melia Josephson became pregnant, she received a five-page letter from an elderly aunt “condemning me to hell,” she said. She repeated her aunt’s words with pity in her voice: “If God wanted people to have children, he would let them have children. Other people shouldn’t be having children for them. This is the road he sent them on, to be childless. He’s trying to see if they can conquer it.”
Josephson says she and the rest of her family don’t agree.
“God gave man the ability to do this,” she said, “and as far as I am concerned, He is behind everything. If he gave man the knowledge to come up with this technique, he must want it to happen.”
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.