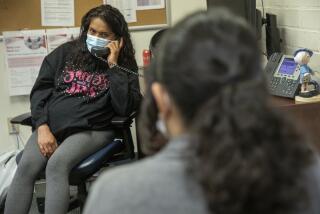Half of callers to Covered California give up as deadline looms

- Share via
Nearly half of callers to California’s health insurance exchange in February and March couldn’t get through and abandoned their call, state figures show.
Those service woes could worsen as more people try to beat the March 31 deadline to get Obamacare coverage under the Affordable Care Act.
Also Thursday, the Covered California exchange reported progress on another front: low enrollment among the state’s large Latino population.
At its monthly board meeting, the exchange said 32% of health plan enrollees in the first two weeks of March described themselves as Latino. That was up from 18% during the first three months of enrollment that ended in December.
“That is a very substantial increase,” said Peter Lee, executive director of Covered California.
Full coverage: Obamacare rolls out
Robert Ross, an exchange board member, applauded those gains with Latinos, but he expressed disappointment at the low sign-up rate among African Americans. It stood at less than 3% of health plan enrollment through mid-March.
California has led the nation with more than 1 million people enrolled in health plans through March 17, and it’s a bellwether state for the national rollout of the healthcare law.
An additional 1.5 million Californians have enrolled or been deemed eligible for an expansion of Medi-Cal, the state’s Medicaid program for the poor.
On the service front, Lee said the exchange has been able to reduce wait times on the phone from about 50 minutes to 30 minutes. The state has hired more call-center workers and added phone capacity in preparation for a last-minute rush.
Still, less than 5% of calls are answered within 30 seconds and about a third of callers get a busy signal, state data show. Overall, 40% of exchange customers surveyed said they found the enrollment process difficult.
Covered California has also been criticized by its certified enrollment counselors for payment delays. The exchange pays $58 for every successful enrollment by a counselor.
The state doesn’t pay them directly. Rather, it pays certified enrollment entities, which are primarily nonprofit groups, community organizations and clinics that oversee many of the 5,100 enrollment counselors statewide.
The exchange said the first payments were sent March 14, and it attributed the delay to the logistics of “getting a new system up and running along with a high volume of enrollments.”
Covered California is considering an increase to the $58 fee after hearing complaints from field workers. Many of them have said that amount doesn’t adequately compensate them for the level of work involved.
The complexity of the healthcare law and the amount of information consumers must sort through often requires considerable time and multiple discussions before a person can complete the process.
ALSO:
Covered California begins ad blitz in final weeks
State exchange pulls error-ridden physician directory--again
California says 14,500 must redo Obamacare applications after glitch
More to Read
Inside the business of entertainment
The Wide Shot brings you news, analysis and insights on everything from streaming wars to production — and what it all means for the future.
You may occasionally receive promotional content from the Los Angeles Times.