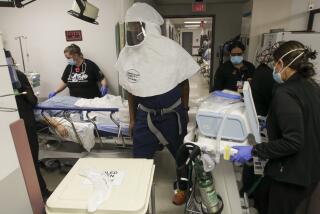
Pandemic exposes low pay and scant protections for nursing assistants and home-care aides
- Share via
When she heard friends working at Lowe’s were in line for $300 hazard-pay bonuses, Allanah Smit wondered why her employer, Memorial Hospital in Gulfport, Miss., had no such plans. “Healthcare workers deserve hazard pay too,” she declared on Twitter. “Yes, we chose this profession, but we didn’t sign up to fight a global pandemic with ONE N-95 respirator and improper PPE.”
As a certified nursing assistant, Smit makes just over $14 an hour to bathe, feed, and reposition patients recovering from car accidents, strokes, and major surgeries like hip replacements. When elective surgeries were suspended last week as the coronavirus spread from hot spots such as New Orleans, Smit began caring for patients with symptoms of COVID-19.
As the healthcare system braces for the full impact of the pandemic, the shortage of doctors and nurses in epicenters like New York has gotten massive attention.
Less scrutiny has been paid to home health aides, personal care aides and certified nursing assistants — who collectively represent the largest category of healthcare workers in the country, nearly 5 million people working across a fragmented landscape that includes teaching hospitals and nursing homes, as well as homes and apartments. These are jobs that do not require an associate’s degree.
Even in hospitals, where wages are higher and full-time employment is the norm, these workers are typically paid less than $15 an hour. The pandemic has highlighted the low pay, lack of equipment and scant job security for these workers.
Emersen Peco, a certified nursing assistant at Sarasota Memorial Hospital in central Florida, has begun caring for overflow COVID-19 patients and “rule-outs” — patients awaiting test results — from other parts of the hospital.
But unlike salaried employees, she is not eligible for paid time off unless she shows symptoms and tests positive for COVID-19, and she has access only to paper surgical masks instead of N95 masks. Last week, Peco said, she and her colleagues were alarmed when a patient who had tested positive for COVID-19 wandered into the hallway without personal protective equipment.
“It’s hard to be confident in your job and patient care when you don’t have the protection you need,” she said. She says the hospital isn’t offering tests because “if we test positive they’re scared they’ll lose the healthcare workers.”
A hospital spokesperson, Kim Savage, says Sarasota Memorial hasd followed CDC guidance for use of personal protective equipment during a shortage, and that the hospital has begun offering paid leave to employees who get sick from COVID-19.
The risk of infection is often greater outside hospitals — at home health agencies and long-term-care facilities, where fewer workers have health benefits or paid leave.
“They feel compelled to go to work,” said Barbara Meinke, a nursing professor emerita at McHenry County Community College in Illinois. “These are the folks who can least afford not to go work — they may be tempted to go to work when they’re not feeling well, and they may be unfortunately the ones who spread the virus.”
Now, with hospitalizations increasing rapidly around the country, direct-care workers are expected to be a vital part of building up the capacity of a strained health system. Health and Human Services Secretary Alex Azar recently urged governors to waive restrictions on licensing, scope of practice, and certification “so that healthcare workers can be deployed as needed.”
Daniel Bustillo, director of the Healthcare Career Advancement Program, a Service Employees International Union training program that serves a million healthcare workers, said those changes would lead to greater demand. “There’s no way we’re going to be able to support the level of care needed without expanding the workforce that can help,” he said.
Rebecca Hanson, who runs training programs for SEIU members in California and other Western states, said the union was rushing to introduce online modules so certified nursing assistants could be trained to perform tasks that might usually be reserved for nurses — such as screening patients for symptoms — and on the proper use of personal protective equipment, or PPE.
Many healthcare facilities have already scaled back employees’ hours or laid off workers in response to the cancellation of routine medical procedures. Hospitals have rearranged staffing patterns to minimize the number of staff at risk of infection. But as hospitals gear up for a surge in COVID-19 cases, adding additional bed space however they can, Hanson anticipates “a kind of domino effect,” whereby nurses move to more acute care settings and nursing assistants take on greater responsibility in screening and caring for patients.
At Stony Brook University Hospital, on New York’s Long Island, strict measures to minimize infection and conserve scarce PPE have been in place for weeks. Tamethiea Bradley, an anesthesia technician, now spends her shifts as a runner, ferrying IV drips, thermometer probes, and other supplies and equipment back and forth to nurses, doctors and respiratory therapists working with COVID-19 patients on the other side of a closed door.
Patient care technicians only enter the rooms of COVID-19 patients under urgent circumstances — for example, a sudden blood pressure drop or cardiac arrest. The limits on the workers who can enter those wards, and the need to wear full-body protective gear, have only made the work more intense.
“You do everything for them, from cleaning them, to bathing them, to turning them every two hours to make sure their lungs don’t collapse,” she said. “There’s no way you can’t be in the room.”
Several colleagues have gotten sores on their faces from the pressure of wearing a tight N95 respirator for an entire shift at a time, Bradley said.
Jasmine Travers, a postdoctoral fellow at Yale’s medical school, says the coronavirus crisis appears to be spurring closer communication between patient care techs and the hospital nurses they work with.
“That’s what the PCTs are saying — nurses are checking in with them often, making sure they have what they need,” Travers said. “This collaborative relationship has emerged between the nurses and the nursing assistants that wasn’t there previously.”
Gabriel Montoya, an emergency room technician at Kaiser Permanente Hospital in Downey, credits his workplace with including all staff in huddles at the start of each shift “so they can get the information about changes to PPE or the daily workflow.”
Federal guidance on PPE has fluctuated seemingly by the day, causing anxiety for the workers. “Workers believe the CDC’s making recommendations based on supply availability, and not the science behind protecting us from this disease,” Montoya said.
Stony Brook has struggled, at times, to provide staff with clear instructions on the use and reuse of PPE — at one point they advised workers, incorrectly, to store used N95 respirators in plastic bags between uses. That instruction was amended to breathable paper bags only 10 days later, after Bradley and her colleagues made calls to the manufacturer and the state health department to learn for themselves. The hospital didn’t respond to a request for comment.
As a public hospital with a unionized workforce, Stony Brook’s direct-care workers tend to have better pay and benefits than many of their counterparts, but Bradley said many CNAs still felt “underpaid and under-appreciated.”
She is responding by showing appreciation for all her colleagues, including those not involved in patient care.
“I said it to a housekeeper the other day: ‘Thank you so much for being here. You’re on the front lines because if you weren’t here, we’d be getting shut down because the hospital isn’t clean,’” Bradley said.
Moore Gerety is a special correspondent.
More to Read
Inside the business of entertainment
The Wide Shot brings you news, analysis and insights on everything from streaming wars to production — and what it all means for the future.
You may occasionally receive promotional content from the Los Angeles Times.