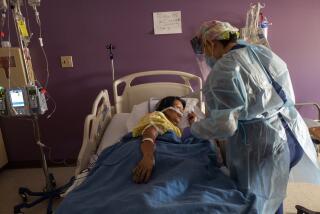ICU beds already near capacity with non-coronavirus patients at L.A. County hospitals

- Share via
Intensive care beds at Los Angeles County’s emergency-room hospitals are already at or near capacity, even as those facilities have doubled the number available for COVID-19 patients in recent days, according to newly released data obtained by The Times.
Fewer than 200 ICU beds were available Wednesday, with most ICU beds occupied by non-coronavirus patients, according to the data which covers the roughly 70 public and private hospitals in Los Angeles County that receive emergency patients.
The figures, which haven’t been disclosed previously, offer the first real-time glimpse of capacity levels at hospitals from Long Beach to the Antelope Valley and raise fresh worries that the hospital system, which is already strained by shortages, could soon run short of beds.
“I am very concerned. We have a limited number of ICU beds available in L.A. County,” said Supervisor Janice Hahn, who urged residents to heed social-distancing orders to reduce infection rates and strain on medical resources. “I would like to begin exploring every possible solution to increase the capacity of our hospital system, including building pop-up hospital sites.”
The anticipated surge of coronavirus patients is setting off a scramble to increase capacity of all types of beds, some of which could be converted to ICU units, according to county health officials.
To accomplish that, hospitals are halting elective services to open up more space, and are considering other plans to expand capacity, including converting existing space or erecting tents.
That effort shows in the figures, with the number of beds overall nearly doubling in the last several days — from 624 on March 13 to 1,182 as of Wednesday. That change includes an increase of ICU beds, which have more equipment and a higher staff-to-patient ratio, from 85 to 191, according to the figures.
Christina Ghaly, a physician who directs the county’s vast system of providers, clinics, and hospitals known as the Department of Health Services, said hospitals can add ICU beds by converting existing space. That entails equipping beds with special equipment and adding personnel and, in some cases, getting approval from state regulators. Rooms could also be opened in non-emergency room hospitals, which aren’t included in the current figures.
“The hospitals across the entire county are working very hard to free up capacity, and also to create capacity,” said Ghaly.
County officials stressed that the figures represent the current staffing needs by hospitals, which have a greater “surge” capacity as more patients get sick. She said they are also asking state officials to fast-track additional capacity.
But despite the progress, as many as 90% percent of licensed ICU beds are already occupied with patients who have suffered other medical emergencies, such as heart attacks, car accidents and other cases, according Ghaly said.
She estimated the total number of coronavirus patients at county hospitals was fewer than 100. More specific numbers were not made available by the county’s Department of Public Health.
The data in the report also showed a surge in capacity of ventilators, from 400 to 800 in the last several days.
The numbers varied widely based on region. Beds in the Antelope Valley were sparse, with only a handful available, but higher in central L.A. County hospitals and those in the San Fernando Valley.
ICU beds statewide total about 7,200, and Newsom has said officials are seeking ways to boost that capacity.
Ventilators, which are crucial for the care of coronavirus patients who suffer from respiratory difficulties, have increased to more than 800. Receiving a major boost is central Los Angeles County, which includes LAC+USC Medical Center and Cedars Sinai, among others, the records show.
Cathy Chidester, who directs the county’s Emergency Medical Services agency, which compiled the report, said adequate staffing levels is emerging as a a more critical need than bed space in recent days. Medical labor groups have complained about a lack of protective gear, and about constraints on their members’ ability to work because of school closures.
“They are more concerned about staffing and keeping their staff healthy — that they have child care so they can come in and do their job,” she said.
The report comes as healthcare experts across the country warn about capacity shortages. A new report by the Urban Institute and the Robert Wood Johnson Foundation, for example, shows that hospital beds are already mostly occupied nationwide, increasing the need for officials to take emergency steps to make more spots available.
“As federal, state and local policymakers prepare for large increases in demand for inpatient hospital care, they need to understand the variation in bed capacity across states and communities — which will likely not match the spread of the virus,” said Kathy Hempstead, senior policy adviser at the foundation. “Now is the time to identify contingency plans.”
The county hospital capacity report is expected to be released each week, and will provide important insight into how hospitals are responding to the disease, which has killed at least 21 people in California and infected more than 1,000.
Health officials hope social distancing will stem the spread of the virus and ease capacity levels at hospitals.
“The public needs to be careful to really very carefully follow the public health orders that have been issued by the state and the county,” Ghaly said. “It spreads out cases over a longer period of time so we don’t get a spike all at once, which could hypothetically overwhelm the hospital system.”
Staff writer Anita Chabria contributed to this story.
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.