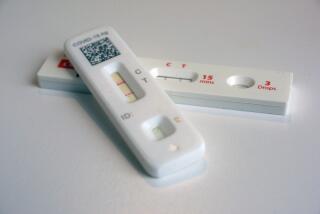
Coronavirus antibody tests are almost impossible to get. Meet three L.A. residents who got them

- Share via
Jake Warner came down with something in late February, but he wasn’t sure with what.
“It’s been a bad flu season, a bad allergy season,” Warner said. “There’s been a lot of what-ifs.”
The 27-year-old tech entrepreneur is hardly the only person to have wondered if he has unknowingly come down with the coronavirus before the extent of the pandemic was known and diagnostic testing was widely available. But he is among a rarefied group that has gotten some answers, thanks to a test that measures antibodies to the virus in the blood.
The antibody tests, also known as serology tests, have become increasingly publicized. Last week, Los Angeles County launched a study to test residents, including those without symptoms, to get a sense of how many people had the virus.
While the tests have captured growing attention, they’re not yet widely available to the public. Only a handful have been allowed by the federal government; others are approved for research use only. No test offers ironclad accuracy.
Three months into the coronavirus pandemic, the U.S. still lacks an effective testing system. Each step in the process involves bottlenecks.
“An imperfect test works fine in a research study because in the analysis you can sort of account for that inaccuracy, but when you’re dealing with an individual patient, you have to be right,” said Dr. Paul Simon, chief science officer for the county Department of Public Health. “And so I’m very concerned that the quality of the tests out there right now are highly variable, very little oversight.”
With antibody testing still relatively hard to obtain, The Times spoke to three Angelenos about what it’s like to get access to this coveted product.
‘The quarantine prom’
When Sara Benincasa, a writer and comic, tells people she’s had the antibody test, their reaction is akin to her getting an envy-inducing script deal.
“Some people assumed I must have some secret hookup,” Benincasa said. “That’s absolutely not the case.”
Instead, she owes her test to an eagle-eyed friend, who showed her an online survey from the county health department and USC. The survey was seeking people to participate in a randomized trial to collect blood samples to test for antibodies.
Since she had exposure to two people who had later been diagnosed with COVID-19, but had no sign of symptoms herself, her friend said she may be a good fit for the study.
Benincasa figured she probably hadn’t had the virus. But if she did, she wanted to donate her plasma, since plasma collected from those who have recovered from coronavirus is being evaluated as a potential treatment for those currently battling it.
She was selected and arrived last weekend to the East Los Angeles Library parking lot, wearing a cloth mask decorated with a unicorn, much to the delight of the USC medical students volunteering at the site.
“I spent careful time choosing what mask I wore because I figured it would give them a laugh, and I was correct,” she said. “This was my equivalent of going to the prom — the quarantine prom.”
The test consisted of quick finger prick to collect a tiny drop of blood. She was told her results would be available in 48 hours, but they returned in half that time. The next day she learned she tested negative.
“I had a simultaneous feeling of relief and disappointment,” she said. “The disappointment came from realizing, oh, I can still get this. And the disappointment was also, oh, I can’t be of service in this special way.”
At the very least, obtaining the test was an unlikely high point in this surreal time.
Before the pandemic started, she said, “if somebody told me the thrill of a lifetime would be driving my 10-year-old vehicle to a nearly deserted public municipal parking lot and say hi to strangers, one of whom would lightly stab me with a needle, I would say, ‘Wow, 2020 is really unfolding in a very special way.’”
‘I know how fortunate I am’
Stacy Rukeyser was scrolling on Instagram when she saw a friend posting about getting an antibody test. She immediately texted to find out where.
The answer was NextHealth, a boutique wellness center in West Hollywood where the offerings include cryotherapy and vitamin shots. The prospect appealed to Rukeyser for a number of reasons. She had been keeping her distance from her elderly mother for fear of inadvertently infecting her.
“If I knew I had the antibodies, I would go see her,” Rukeyser said. “That would make her life a lot better.”
She also saw the blood test as potentially a step forward in getting back to work. Rukeyser, the showrunner for the Netflix show “Sex/Life,” was two weeks into production in Toronto when coronavirus abruptly shut things down on March 13.
“What are the conditions that would have to exist in order for TV shows to go back into production? Nobody seems to know,” Rukeyser said. “Antibody tests are one of the things on the list of possibilities.”
The tests at NextHealth cost $249 apiece, and Rukeyser noted that being able to afford it put her in “an incredibly privileged position.”
“I know how fortunate I am,” she said. “I acknowledge the sort of pay-to-play aspect of it and the inequality of that. I’m trying to do it for a good purpose — to amplify the test.”
She and her husband went in for the test on Saturday, getting a blood draw from a vein in her arm. On Wednesday, they got their results: Both tested negative.
“I felt disappointed, of course, that I didn’t have any antibodies, and thus no potential immunity,” she said. “But I also felt glad to know — to have certainty one way or another.”
‘I don’t know if I’m in the clear’
For more than a month, Warner and his live-in girlfriend have been apart, for fear of unintentionally exposing each other to the virus. His girlfriend has an immune deficiency and asthma, which would make the coronavirus especially risky for her.
Warner said he would jump at “any way to triple-check when it comes to her safety.” The antibody test offered the chance to know if they should continue to stay apart.
His mother contacted her longtime doctor, who had recently received several hundred test kits. Warner, his mother and stepfather, as well as his girlfriend and her mother, all took the test during a home visit. The test required about half a vial of blood drawn from the forearm. Warner did not pay out of pocket for the test and believes his health insurance may have covered it.
Within 90 minutes, he got a phone call with the results. Warner’s entire immediate family tested positive for the antibodies. He followed up with a nasal swab test at an urgent care clinic to see if the virus was currently in his system and tested negative for that.
His girlfriend tested negative, meaning their distancing would have to continue.
But Warner, who has consulted with several doctors, says the antibody test hardly offers all the answers. Much is still unknown about what the presence of antibodies mean and whether that actually indicates of if someone is immune from the virus. The result is a confusing muddle of conflicting information.
“I’ve been told I’m in the clear, but also told I can still contract it again,” he said. “I’ve been told I’m not contagious, and I’ve been told I am contagious.”
The end result is not much practical change for how Warner is approaching the virus. He still wears a mask and gloves, washes his hands regularly and doesn’t go out unless absolutely necessary.
“The best move on my part and my family is continuously quarantine the way we were before,” he said. “There’s a little bit of ease of mind knowing I’m probably not going to get sick from this point forward.”
But he worries that many people are going to get a false sense of confidence from antibody tests.
“Rather than it being a means to more information or data about yourself and the population, people are going take it as a pass/fail,” he said. “It needs to be highly expressed on all fronts that’s not the case.”
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.