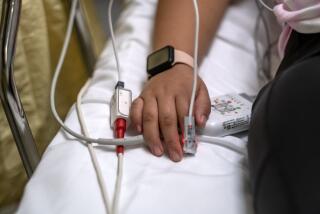
Coronavirus threatens a South L.A. clinic that’s long been a lifeline for the working poor

- Share via
On a typical day, the line starts forming outside South Central Family Health Center before sunrise.
For thousands of patients, this clinic run by a devoted team of doctors in Central-Alameda has become a one-stop shop for all their aches and pains and chronic woes.
Now, because of the COVID-19 pandemic, much of the crucial work this health center and other community clinics do to help Los Angeles’ most vulnerable populations is at risk as many people have stopped leaving their home to see their doctor.
“We were already dealing with a delicate situation,” said David Roman, spokesman for the South Central Family Health Center, which has been operating for nearly 40 years. “Now we have an underserved population with diabetes, asthma, hypertension that is avoiding their routine. They’re having to make a choice. Do they come in and stay healthy or do they stay home and get sicker?”

Since stay-at-home orders went into effect in mid-March, patient visits have fallen by 25% at South Central, costing the nonprofit clinic an unprecedented loss of about $310,000.
Other clinics run by community health center organizations across Los Angeles County are also struggling.
The coronavirus outbreak forced many of the county’s 350 clinics to take drastic measures such as closures, furloughs, layoffs and job reassignments, said Louise McCarthy, president and chief executive of the Community Clinic Assn. of Los Angeles County. Collectively, she estimates, centers are losing an average of about $6 million per week. Some clinics have lost 30% to 70% of their patient visits.
“This pandemic has eclipsed all other crises we’ve experienced to date and we’re still in the relief phase,” McCarthy said. “We don’t know yet what our new reality is going to be, but nothing will be the same again.”
At risk is the health of a vast Latino and black population the clinics serve, a community that’s already been disproportionately hit by COVID-19. Countywide, 60% of those who rely on local clinics live below the poverty level, about $26,000 per year for a household of four. An additional 20% of households that rely on clinics make less than $52,000 per year.
For these families, community clinics provide a vital safety net. Without these services, many people are likely to end up in hospital emergency rooms, putting further strain on the healthcare network.
At South Central Family Health Center, patients come from immigrant communities. About 92% are Latino. They labor in construction, hotels, factories and restaurants. Those in dire need often turn to the clinic for food donations, help with evictions and immigration resources.
Over the years, they’ve come to trust the medical team. Some physicians, such as Dr. José Luis Perez, as well as several staff members, grew up in South L.A. Perez attended high school just a mile from the clinic.
“Working here for me is really personal,” said Perez, a native of Nicaragua who is also the center’s chief medical officer. “Most of my patients look like my grandma or my cousins. I understand their lives because I’ve lived a lot of it myself.”
In recent days, Perez has found himself worrying about patients who have not been coming in — those with diabetes, high blood pressure, terminal cancer.
Despite concern from medical staff, the clinic has cut services, closing four of its nine sites and stopping construction of a new vision care center. It also has furloughed dozens of workers and reduced their hours.
Federal stimulus funds this month provided temporary relief for a number of clinics. South Central received $1.1 million. That’s enough to support services until the first week of May, Roman said.
“We’ve taken some extraordinary measures in order to save cash,” he said. “Legislators really need to understand the impact this pandemic has had in the community, on the fragile balance of this safety net.”
Community clinics have also had to battle to get personal protective gear and testing. Officials say that while much of the national focus has been on hospital shortages, the needs of community clinics have been largely overlooked.
South Central had only 20 coronavirus tests available for patients in early April. When it was unable to get more, a testing lab advised the clinic to use gonorrhea collection kits it had in storage. The kits are processed like other coronavirus tests and deliver solid results, Roman said.
Another clinic network, St. John’s Well Child & Family Center, has been facing its own challenges. Jim Mangia had to put a half-dozen employees to work full-time hunting down masks for his 18 centers, which serve a total of about 100,000 patients. They managed to patch together a stockpile with help from donations, local leaders and one center worker who had connections to a factory in China.
“It was so touch and go, we were literally about to run out when an order came in,” said Mangia, chief executive of St. John’s, which operates centers across South L.A., Mid-City and northeast Los Angeles.
Now, Mangia said, his clinics are pushing to meet a tremendous demand for tests. Last week, medical staff opened 13 testing sites. They administered more than 1,300 tests in one week, using up their supply.
“We keep fighting, but it’s like trying to fight with both your hands tied behind your back,” Mangia said. “We’re on the front lines, too, and we’re seeing all the health disparities and inequities people here experience every day magnified tenfold because of this pandemic.”
One positive note is that community clinics in California are now allowed to charge insurance providers for treating patients via Telehealth — by phone and video. Until now, that service was off-limits because of federal regulations. It was permitted only in rural areas or among more well-to-do patients with private insurance.
In South L.A., some clinics are now treating up to half of their patients by phone. They’ve seen far fewer appointment cancellations this way.
“For so many years, people have had to take three or four buses to visit the doctor because we’re not removing these socioeconomic barriers,” said Adel Syed, chief executive of the University Muslim Medical Assn., a center that serves about 8,000 patients in South L.A., most of them working-poor Latinos.
There’s no indication so far that clinics will be allowed to continue billing for Telehealth appointments after the pandemic, but the Community Clinic Assn. of Los Angeles County plans to fight for it, McCarthy said.
Back at South Central Family Health Center on a recent afternoon, patients wearing masks trickled in, forming a line outside the front door. A medical assistant checked their temperatures, screening for coughs and fevers before allowing them inside. A few patients had just been released from the hospital after battling COVID-19.
Emilia Flores, 67, a first-time patient, sat in the lobby feeling jittery about having left her house, just a few blocks away. But she had run out of depression medication and her usual clinic in San Pedro had shut down.
“I was so afraid to come and was really trying to push through on my own, but I can’t live without my medicine,” said Flores, who has struggled ever since her son-in-law and two grandchildren died in a fiery car crash two years ago.
Her husband, fortunately, has a secure job that provides health insurance. He works at a factory that makes medical supplies. Their family has always counted on community clinics for all their health needs.
“I wouldn’t know where else to go,” Flores said.
A few days after her visit to the clinic, she was stressed about the pandemic and still struggling with her ongoing grief, but she felt at ease knowing there was a health center standing by to help, so close to her home.
“This place took really good care of me,” she said.
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.