California is finally making progress in the coronavirus battle, even as deaths keep rising
- Share via
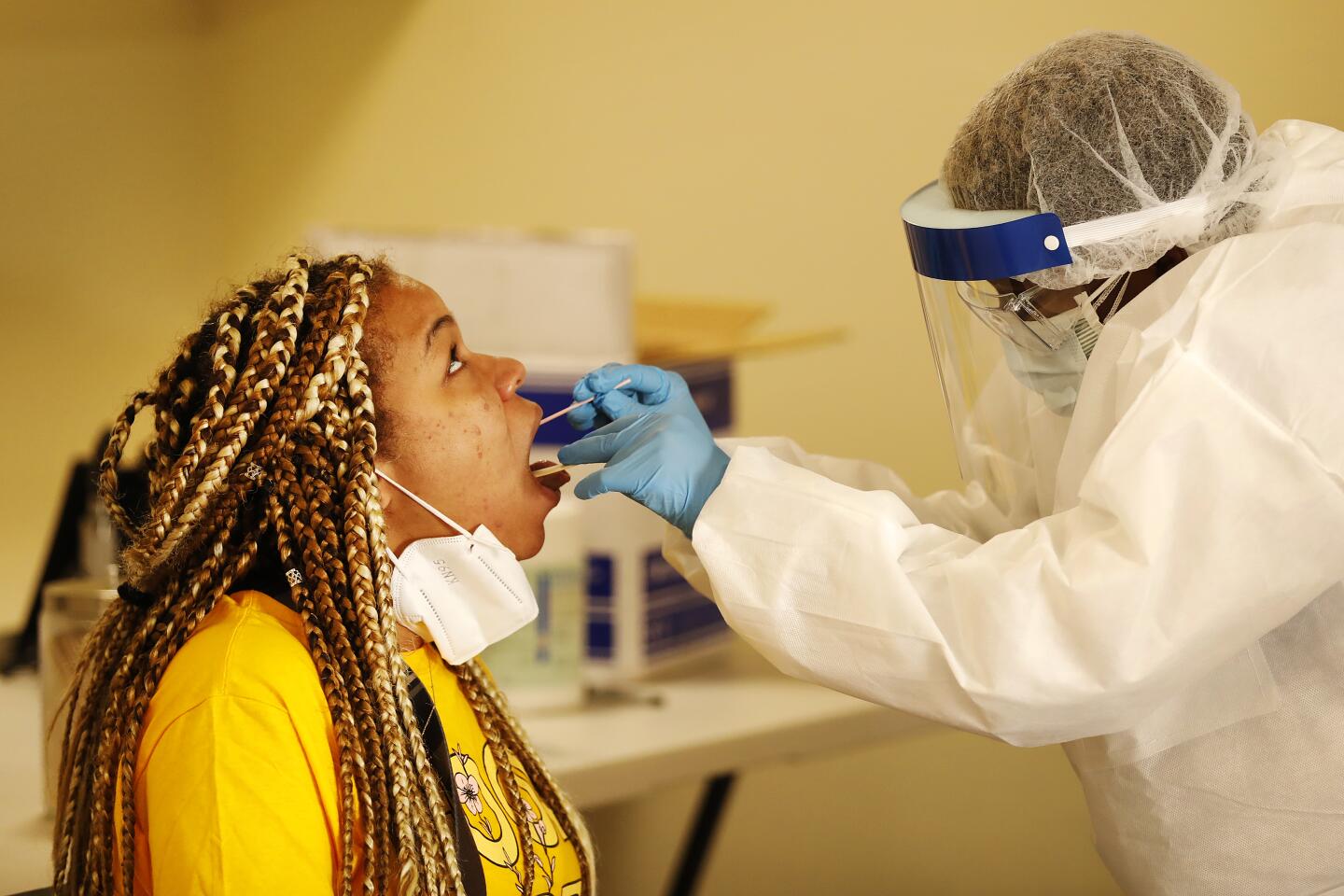
SAN FRANCISCO — Three months into California’s battle with the coronavirus, there are growing signs that the outbreak is ebbing even as the state death toll continues to climb past 3,400.
While deaths remain a stubborn challenge, other metrics analyzed by the Los Angeles Times show significant progress — enough that even some of the most cautious local health officials have agreed to begin reopening the economy.
The number of newly identified coronavirus cases across California has declined last week from the previous week, dropping to 12,229 cases from 13,041 the previous week. That’s a notable achievement, given the amount of increased testing.
And across California, hospitalizations have dropped more than 15% from its peak six weeks ago, The Times analysis found.
Gov. Gavin Newsom had initially tied reopening counties at a faster pace than the statewide standard to zero coronavirus deaths over a two-week period, a benchmark that some hard-hit counties like Los Angeles have little hope of achieving any time soon.
But with many other hopeful signs, Newsom dropped the requirement this week in a move that will allow many urban counties to reopen much more quickly. A Times data analysis found that some counties, including Contra Costa, Monterey, Napa, San Joaquin, San Luis Obispo, Santa Clara and Yolo counties meet two key requirements needed to move into the next phase of reopening, which includes dine-in restaurants and shopping malls.
On Tuesday, Napa County said it had received state approval to reopen restaurant dining rooms and retail stores for in-person shopping; wineries, hair and nail salons still remain shut, and tourism is not allowed. Sacramento County said it also got a green light to reopen dine-in restaurants.
“What’s really fantastic about this is that, for right now, our curve is not only flat, but it’s actually decreasing in terms of number of hospitalizations,” said Dr. Grant Colfax, San Francisco’s director of health. “So this is very hopeful.”
Deaths remain a persistent problem, with an average of 500 Californians dying from coronavirus infections every week, as is the growing disproportionate toll the disease is taking on blacks and Latinos. There remains deep worry about a resurgence of disease in the fall, and officials warn the disease may be with us for the next two years without a widely available vaccine.
But even officials who have taken the earliest, boldest steps to impose stay-at-home orders are now saying the situation has stabilized enough to permit a slow reopening of society.
There are two key indicators some officials are increasingly focusing on: hospitalizations and the percentage of people testing positive.
In Santa Clara County — the home of Silicon Valley and once a national epicenter of the coronavirus pandemic — in early April, 9% of people tested had positive results for the coronavirus, a time at which there were fewer than 600 tests a day in Silicon Valley, health officer Dr. Sara Cody said this week. In recent days, just 1% to 1.5% of people are testing positive, and the county is now able to receive results from around 1,600 tests a day.
“Hospitals have capacity... and finally, our testing capacity has also increased,” she said.
Just last week, Cody warned against easing the stay-at-home order, saying relaxing it “would see a brisk return of cases, of hospitalizations, and a brisk return of deaths.”
Since then, the number of deaths in Santa Clara County has continued to fall, dropping to six last week, the lowest weekly tally in 10 weeks.
The nine-county Bay Area recorded 43 deaths last week, a slight increase from the previous week tally of 38, but still below the all-time weekly high of 61 deaths last month.
On a statewide basis, Newsom this week said the decrease in the state’s hospitalizations was a factor in loosening requirements counties need to meet to reopen more broadly.
“Remember: the whole purpose of the stay-at home order was to prepare and to respond in the worst-case scenario,” Newsom said. In recent weeks, testing and the supply of personal protective equipment is up, and “our capacity to meet surge has been, I think, advanced.”
Two dozen mostly rural counties in Northern California have already entered a phase of broader opening some call the Expanded Phase 2, allowing restaurants and retail stores to legally reopen their doors for inside service in counties like San Benito, just east of Monterey County.
They met strict criteria issued by the governor on May 7, whose requirements included no deaths from coronavirus-infected individuals in the past 14 days, and no more than 10 cases per 100,000 residents in that same time period.
Those were just two of many standards Newsom asked counties to meet, and they were strict: A Times data analysis at the time showed that 95% of California residents lived in counties that failed those benchmarks.
Newsom’s new standards released Monday abandons the requirement that there be no COVID-19 deaths in a county within the last 14 days.
Instead, hospitalization data is a key indicator. A county must have stable or falling hospitalizations.
Hospitalization is considered stable if the average daily increase in patients is under 5% over the past week. (Smaller counties can meet the standard if they show no more than 20 hospitalizations on any single day in the past two weeks.)
Another key rule measures the rate of disease in a county. A county must either have less than 8% of people testing positive in the last week, or fewer than 25 new cases per 100,000 residents in the last 14 days.
Newsom estimated 53 of California’s 58 counties could meet these standards.
There are other standards counties must meet to open more broadly. They include a minimum level of testing capacity, robust disease investigation teams, ample hospital bed capacity, and plans to prevent or deal with nursing home outbreaks.
San Luis Obispo and Ventura counties are among the counties that are applying to meet the new standard.
While Ventura County has reported six deaths in the last two weeks, failing the previous rule, the county said Tuesday just 3.5% have tested positive for the virus in the last week, and hospitalizations have been declining.
Newsom said counties that likely would not be eligible to enter this accelerated phase of reopening include two in the San Joaquin Valley: Kings County, home to an outbreak at a meatpacking plant in Hanford, and Tulare County, where outbreaks in nursing homes have persisted. Redwood Springs Healthcare Center in Tulare County has seen 28 residents die and 116 patients and 61 staff members infected.
In recent days in Los Angeles County, 9% of people tested for the virus have had positive results, which fails the state maximum of 8%, said Barbara Ferrer, the director of public health for Los Angeles County.
The weekly average number of people in L.A. County hospitalized with confirmed or suspected coronavirus infections has declined in recent weeks.
On Tuesday, L.A. County Supervisor Kathryn Barger expressed a goal for a reopening of L.A. County by July 4, something Ferrer said the county would aim for, but also remains contingent on what the data says in terms of the progress of the outbreak.
Dr. Robert Kim-Farley, medical epidemiologist and infectious-disease expert at the UCLA Fielding School of Public Health, said he thought California was taking appropriate steps to reopen society safely.
It makes sense to allow places with few cases and sparse population to reopen sooner than dense, urban places hit hard by the pandemic, said Kim-Farley, a former senior official for the L.A. County Department of Public Health, the U.S. Centers for Disease Control and Prevention and the World Health Organization.
“Obviously, we have some tensions that will always exist, some wanting to move faster than others,” Kim-Farley said. “The idea here of ... trying to all agree on what are the guideposts along the way and then, let’s open up accordingly ... these phased processes are a good approach.”
Kim-Farley said officials should increasingly focus public health resources on where the coronavirus problem is greatest, like nursing homes.
Workers in skilled nursing facilities account for 44% of healthcare workers and first responders in L.A. County with confirmed coronavirus infections. Kim-Farley said it would be important, for instance, find ways to pay nursing home workers enough so they don’t have to work at multiple locations, or paying them enough so they can live at the facility for a period of time.
For all the focus on the improved numbers, experts still caution that things can get worse. Outbreaks at institutions like prisons, nursing homes and homeless shelters could spread to the broader community.
The 1918 flu pandemic saw a second wave of deaths many times worse than the first.
“It’s very easy to have a scenario where there’s more infections, and having more infections results in overwhelming the health care system,” Ferrer said.
Lin reported from San Francisco; Lee and Greene from Southern California. Times staff writers Maura Dolan, Taryn Luna, John Myers, Colleen Shalby and Phil Willon contributed to this report.
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.