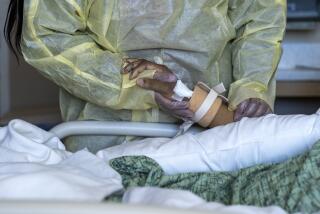
Little noticed, Filipino Americans are dying of COVID-19 at an alarming rate

- Share via
On March 10, Loretta Mendoza Dionisio became the first person in Los Angeles County known to have died of COVID-19.
Dionisio was 68, had diabetes and had just returned from a trip to her native Philippines. That made her a precursor of the coming pandemic in more ways than one.
For a variety of reasons, Filipino Americans have been hit hard by the novel coronavirus. People with roots in the Philippines account for about one-quarter of the Asian Americans in California, yet data compiled by The Times show that Filipino Americans account for at least 35% of COVID-19 deaths in the state’s Asian population.
Of 48 Filipino Americans known to have been infected with COVID-19 in Southern California, 19 have died, according to the Philippine Consulate General of Los Angeles. Although the data may be skewed by a small sample size, this puts Filipino Americans at a 40% mortality rate, significantly higher than the overall 3.7% mortality rate in the U.S., according to research by Johns Hopkins.
Data compiled by The Times have shown that preexisting health conditions and occupational hazards are among factors that contribute to the high number of Filipino American deaths during the pandemic. Most of those who died were older than 60, and many had diabetes and hypertension. Many were retired, living in multigenerational housing with their children or in nursing homes. Younger victims worked essential jobs, providing healthcare, working in law enforcement and at grocery stores.
The pandemic’s toll: Lives lost in California
Hundreds of people have died in California due to the COVID-19 pandemic. These are some of their stories.
Although the death rate among Asian Americans is about proportional to their share of the population, studies show health and socioeconomic disparities in the Filipino American community may be causing more severe cases of infection. A March 30 report from the UC Davis Bulosan Center for Filipinx Studies listed undocumented status, exposure for health workers, poverty and economic insecurity, preexisting respiratory conditions and lack of health insurance as factors that made Filipino Americans more at risk.
“It’s the perfect storm,” said Adrian De Leon, an assistant professor in USC’s department of American studies and ethnicity. “In terms of exposure to the pandemic, exposure to the virus, but also exposure to a lot of other factors, too — like dense housing tends to be in places that have environmental hazards.”
Black and Latino Americans also have alarmingly high mortality rates, and as more data are released, it has become clear to researchers that coronavirus affects racial groups differently. But the California Department of Public Health does not report ethnicity by Asian subgroups, which makes it difficult to identify more data from Filipino Americans. “Using ‘Asian American’ as an overarching label obscures a lot of the inequalities within and among communities,” De Leon said.
According to Dr. Melinda Bender, who specializes in health intervention work for Filipino Americans at San Francisco State University, Filipinos have relatively high rates of obesity, high blood pressure and heart disease, all of which are associated with more serious cases of COVID-19.
“People think that Asians as a whole are pretty healthy,” said Bender, who is Filipina. “But in fact, we are all very different in how we are represented in chronic disease.”
“Filipinos,” she added, “have the highest sedentary behavior of Asian Americans, and the Filipino diet is high in fat. All of these factors put Filipinos at risk.”
Bender also said that asthma was prevalent in the Filipino population in the United States, which would affect susceptibility to a respiratory infection like the coronavirus.
Another factor: In California, almost a fifth of registered nurses are Filipino, putting them at greater risk while on the frontlines in hospitals and nursing homes. They also tend to work in the ICU, acute care and surgical units, where COVID-19 patients are treated. This combination of working essential jobs while having underlying health conditions increases the risk of contracting more serious infections of COVID-19.
“People in certain ethnic groups are predisposed to working really hard — and they’re ‘heroes’ or things like that, which is an Asian American stereotype — but it’s more so because people need to continue to work in order to survive,” De Leon, who is Filipino Canadian, said. “In a country that has such weak social security, such as the United States, you have people ultimately sacrificing much-needed healthcare for themselves for the opportunity to work and continue to make money for the family.”
The high number of Filipino Americans in healthcare goes back to the United States’ colonial history in the Philippines. Medical education in the Philippines was modeled after the American medical education system. When there was a shortage of nurses in the United States in the 1960s, it was easy for American hospitals to recruit Filipino nurses who had learned nursing the American way.
“It’s a colonial relationship that reinforces the U.S. dependence on foreign labor,” Dr. Maria Rosario Araneta, a Filipina American who is a professor in the department of family medicine and public health at UC San Diego School of Medicine.
In the Midwest, the Filipino Consulate in Chicago tracked 17 Filipino American deaths. Half of the victims had been working in healthcare. “Nursing intrinsically requires being in close quarters with patients, and there is no way you can do six-feet social distancing,” said Dr. VJ Periyakoil, the director at the Stanford Aging and Ethnogeriatrics Research Center, which examines ethnicity and health.
According to Periyakoil, socioeconomic conditions are a big risk factor for Filipinos. “If you’re poor, your housing circumstances are going to be quite limited; there will be more people sharing the same space; you’ll be working on daily-wage or low-paying jobs, which require you to go into work,” she said. “When you’re forced to go into work, forced to be in contact, forced to take public transport, the nature of your finances imposes certain realities and restrictions on your daily life that put you at risk for higher stress and infections including COVID.”
Several generations of a Filipino family might live under the same roof, which can lead to difficulties isolating sick family members.
Dulce Amor Aguilo, a 55-year-old caregiver from San Jose, died of complications from COVID-19 on April 19. Although she was not working at the time, she was receiving dialysis for end-stage renal disease and also had type 2 diabetes, high blood pressure and hyperlipidemia.
The family is unsure how Aguilo contracted the virus, but she began exhibiting symptoms three days after her last dialysis treatment. In the small, two-bedroom home in a retirement community she shared with her parents and sister, her mom would wear a mask and try to take care of her as best as she could.
But when Aguilo began having shortness of breath and fever, she was sent to the hospital. Ten days later, she died. “For Filipinos who already have these co-morbidities, this puts them at higher risk when they contract COVID-19,” Bender said.
According to Aguilo’s mother, Dalisay, diabetes is common in her side of the family, and all her children had it, as well as her mom. Her oldest daughter, Pamela, is also on dialysis.
Bender’s work focuses on creating preventive measures to lower Filipino Americans’ risk of developing chronic diseases. “There are a lot of cultural factors that go into why they have a lifestyle like this, and we’re trying to make lifestyle changes such as helping them be able to cook Filipino dishes in a healthier way,” she said. “These are lifestyle-related chronic diseases that are preventable.”
More research needs to be done to address the disparities within the Asian American community. A research brief published on Health Affairs reported that Asian Americans appeared to have a fatality rate from COVID-19 four times higher than that of the overall population. The article noted, however, that this result could be due to inadequate data on Asian Americans, and lack of standardization on the ethnicities counted as Asian American. Recently, Pacific Islanders have been found to suffer the highest infection rate of any racial or ethnic group in Los Angeles County, but the data remain limited.
Pacific Islanders are seeing higher rates of infection from the coronavirus than any other racial or ethnic group in Los Angeles County.
Dr. Tung Nguyen, endowed chair in general internal medicine and professor of medicine at UC San Francisco, co-authored the article. He said disaggregating data on Asian Americans was one of the first steps to addressing health disparities among communities of color. “At best, it should be disaggregated by Asian American national origin group, and primary language,” Nguyen said. “And then they should also invest efforts in collecting data so that there is a minimum amount of unknowns, because it is really hard to clarify disparities when there’s a big group of people who we don’t know anything about at all.”
“The lack of investment,” said UC San Diego professor Araneta, “the invisibility of health issues in the Asian community, is something that I’m hopeful [we can expose]. … We can’t continue being invisible. We contribute meaningfully, financially, professionally to the growth of this country but remain invisible.”
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.