Most nursing home inspectors still haven’t been tested for the coronavirus, despite Newsom pledge

- Share via
A month after Gov. Gavin Newsom promised an aggressive program to test nursing home inspectors for the deadly coronavirus, at least 60% still have not been tested, state health officials acknowledged.
Newsom ordered the testing in late July after a Los Angeles Times investigation found that, since the beginning of the pandemic, state health officials had been sending inspectors from nursing home to nursing home — many of which had raging outbreaks — without testing those inspectors to make sure they were not spreading the virus themselves.
For the record:
6:13 p.m. Sept. 14, 2020Nursing homes inspectors: An article in the Aug. 27 Section A about testing of nursing home inspectors said California health officials had barred friends and relatives from visiting residents in nursing homes since March. In late June, state officials began allowing visits outdoors or in large communal spaces as long as everyone wears a mask, keeps at least six feet apart and there are no hugs or handshakes.
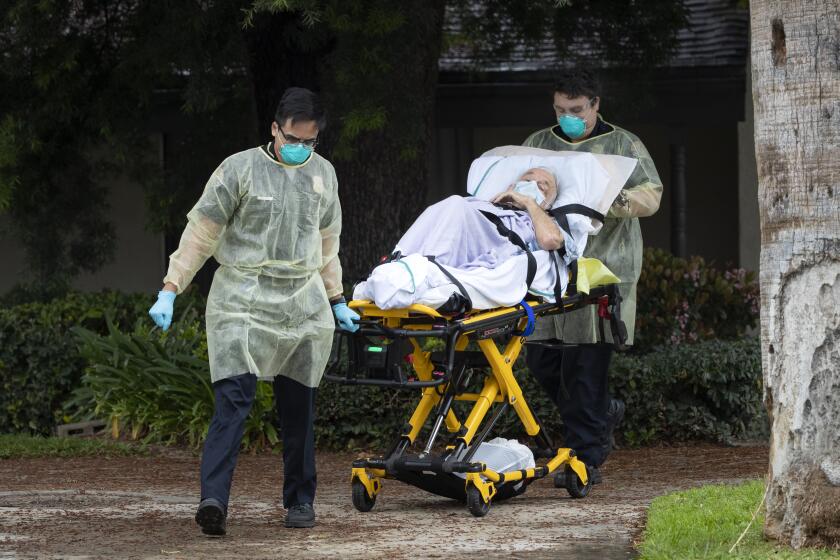
State inspectors worry they could be unwittingly spreading coronavirus from nursing home to nursing home while doing their jobs.
The testing program itself has been sharply criticized by some inspectors, who say it’s an informal and disorganized process with little supervision or clear protocols: They’re sent for do-it-yourself drive-through testing at Rite Aid. They are not required to quarantine during the long waits for the results. And some inspectors say they haven’t shared the results with the department because they don’t know how to.
Nursing homes, with their concentrated populations of vulnerable people, have suffered a disproportionate share of death and illness as the virus has spread across the country. In California, more than 40,000 nursing home residents and employees have tested positive for COVID-19, and more than 4,000 have died of the disease.
Since the start of the pandemic, state health officials have barred friends and family from visiting nursing homes, meaning thousands of residents have died without a final embrace from their loved ones. Since May, nursing home employees have been required to undergo an aggressive testing regime — all had to get a baseline test to begin with, and they have to get follow-up tests at least once a month for surveillance.
Those drastic measures are designed to prevent someone from picking up the virus outside a home and then inadvertently bringing it in, potentially sparking a lethal outbreak.
But while all of that was occurring, state officials failed to test the very inspectors responsible for ensuring infection-control procedures were being followed, even though many of those inspectors are exposed to the virus on a near-daily basis.
“For them to send us in without testing or screening is unconscionable,” an inspector in Southern California told The Times last month. “I think nursing homes shouldn’t let us in.”
As of Monday, a month after Newsom’s order, state officials had only received test results from 136 of the approximately 500 inspectors who visit nursing homes across the state. None had tested positive, according to Mark Smith, a spokesman for the California Department of Public Health.
The governor’s promise came after a Times report that the state hadn’t tested its health inspectors who regularly visit nursing homes and could unwittingly spread the virus.
On Tuesday, Smith said the number had climbed to 200 completed tests with one positive. That one positive test result was received by the department on Aug. 21, and the employee had last visited a state office or health facility on Aug. 12, Smith said.
“Additionally, the employee did not come into close contact with any other CDPH staff,” Smith said.
The deadline to complete the first round of baseline testing for all state inspectors is Aug. 31, Smith said.
Officials at the L.A. County Department of Public Health, which has about 180 of its own nursing home inspectors, refused to say how many have been tested.
“There’s no sense of urgency,” said Assemblyman Adrin Nazarian (D-North Hollywood), who has become an outspoken critic of state health officials for what he considers a dangerously lethargic response to the COVID-19 crisis in nursing homes.
During a hearing at the state Capitol on Aug. 17, Nazarian accused the state health department‘s deputy director, Heidi Steinecker, of being “elusive” when legislators pressed for specifics about her agency’s handling of the pandemic.
“Honestly, I sometimes feel, with your calm and measured responses, not much keeps you up at night,” he told her.
Elder advocates accuse the state of abdicating its responsibility to police nursing homes at a critical moment.
Nazarian also complained that Steinecker’s department had not set up a separate, designated system for testing nursing home inspectors, instead sending them off to seek testing from pharmacies or their own doctors like members of the general public.
Inspectors interviewed by The Times in the last week said that is precisely what is happening.
After Newsom’s vow to provide testing, inspectors said they were instructed to set up their own appointments at Rite Aid.
One inspector in the Central Valley, who asked that her name not be used for fear of retaliation, said she got her test in mid-August and waited six days for the result. Instead of being quarantined while she waited, she said she was sent the next day to inspect a home with dozens of known COVID-19 cases.
“It was so important to [CDPH administrators] that I get that COVID test so I could be sent out and they could say I’d had my test, even though I didn’t have the result,” the inspector said. Some nursing home officials have objected to being forced to allow untested state inspectors into their facilities.
Inspectors are not required to quarantine while awaiting their results as long as they don’t have symptoms and wear proper protective equipment while inside nursing homes, Smith said.
The inspector and two colleagues spent four days inside the stricken facility, she said, during which time dozens more residents tested positive. Nearly 80% of the residents had COVID-19, she said.
“It was a mess,” the inspector said. The facility’s air conditioning had gone out so, “they had fans blowing dirty air all over the place.” On top of everything else, the inspector said, her medical-grade N95 face mask didn’t fit properly the whole time she was in the facility.
The day she and her colleagues finished the inspection at the stricken facility, the inspector said she got the result from the test she had taken a week earlier. It was negative, but that doesn’t mean much anymore, she said.
“I did not have [COVID-19] when I got tested. Do I have it now? I don’t know,” she said.
When she asked state health administrators what to do, she said they did not offer to test her again at Rite Aid at the department’s expense. Instead, they suggested she go to her primary care physician. Her primary care physician refused to test her because she didn’t have symptoms, adding that if she thought she was exposed at work, it was up to her employer to test her.
“It’s just a big runaround,” the inspector said. For the last week, instead of quarantining, the inspector said she and her colleagues have been working from their district office. But all three are scheduled to resume visiting nursing homes in the coming days, without having been retested.
Another inspector in Southern California, who also asked that her name not be used for fear of retaliation, said she followed the department’s instructions and went to a drive-through testing site at a Rite Aid, which she described as, “pretty much do-it-yourself.”
The pharmacist handed her a test kit while she sat in her car and then watched her put the swab up her own nose. “He kept saying, ‘higher, higher, higher.’ I’m like, no, it’s already in my brain!”
A co-worker told her the pharmacist who handed over her test didn’t even bother to watch.
The inspector said she has not reported her results to the state health department and has received no instructions on how to do so.
Other inspectors said they were instructed to email the results to a department email address set up to receive them.
Sending health inspectors out to get tested like the general public, with no clear procedures for reporting the results, is no substitute for setting up a dedicated testing system with more immediate access to results, according to Nazarian.
“That doesn’t cut it,” he said, “Telling state employees to go get tested with the general public, that’s not a standard. That’s mediocrity at best.”
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.