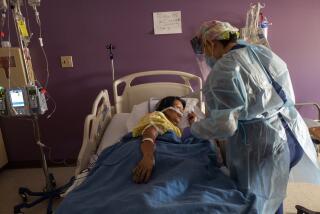L.A. County shatters COVID-19 record with 12,741 new cases in one day
- Share via
Los Angeles County shattered its daily record for new coronavirus cases, with 12,741 reported Thursday as hospitals continued to fill with patients, according to an independent Times tally.
The new total is more than 2,800 more coronavirus cases than L.A. County has seen in a single day — breaking the previous record set Sunday — and shows the coronavirus is still spreading rapidly through communities. The county also reported 74 new deaths, the fourth-highest single-day total of the COVID-19 pandemic.
The surge in cases likely represents the consequence of an explosion of virus transmission over the Thanksgiving holiday, officials said.
“I do think that we’re starting to see some of the increases from Thanksgiving week, and the thousands of people that were either traveling or mingling with people outside their household for the holiday,” L.A County Public Health Director Barbara Ferrer said earlier this week.
With the new numbers, L.A. County is now averaging nearly 9,500 new coronavirus cases a day over the last week, and 52 COVID-19 deaths a day. Those are both records in this pandemic. Until Thursday, the highest average daily number of COVID-19 deaths in L.A. County over a weekly period was 50, a record set for the seven-day period that ended April 24.
L.A. County is now recording double the number of daily coronavirus cases than it saw on Nov. 30, and quadruple its daily coronavirus cases since mid-November. Cumulatively, L.A. County has tallied 488,519 coronavirus cases and 8,151 COVID-19 deaths.
California has averaged nearly 29,000 new coronavirus cases a day over the last week, a new record. More Californians are also dying of COVID-19 than at any other point in the pandemic. The state has averaged about 150 deaths a day over the last week — breaking a record set in August.
California on Thursday recorded 33,995 new coronavirus cases, marking the third highest tally for a single day, and 172 deaths.
Cumulatively, the state has logged more than 1.48 million coronavirus cases and more than 20,600 COVID-19 deaths.
At the same time, the availability of intensive care beds in Southern California and the Central Valley hit alarming new lows.
“Like a speeding car approaching a cliff, if we do not rapidly change course, we are in jeopardy of catastrophic consequences,” Dr. Paul Simon, chief science officer for the Los Angeles County Department of Public Health, said during a briefing Thursday.
In Southern California, ICU availability fell to 7.7% on Thursday, down from 9% the day before, the latest data show. The state defines the region as Imperial, Inyo, Los Angeles, Mono, Orange, Riverside, San Bernardino, San Diego, San Luis Obispo, Santa Barbara and Ventura counties.
The situation was even more dire in the San Joaquin Valley region, which is reporting 1.9% ICU availability, down from 4.2%. Numbers have also worsened in the Greater Sacramento area, which reported in at 13.3%, down from 14.3%; and the San Francisco Bay Area, which was at 17.8%, down from 20.9%.
Rural Northern California remains in comparatively solid shape, at 30.3% ICU availability.
Statewide, an all-time high of 11,497 coronavirus-positive patients were hospitalized as of Wednesday, the most recent day for which complete data are available.
That number increased by 485 in just one day and has swelled by 30% over the last week, state figures show.
The story is much the same when it comes to ICUs. The number of Californians requiring that level of care jumped 115 in just one day to a record 2,621 as of Wednesday.
As of Wednesday, L.A. County had 3,624 people in its hospitals with coronavirus infections, the 11th consecutive day that number has been a new high. The county’s net number of COVID-19 hospitalizations increased overnight between Tuesday and Wednesday by 191 — the highest single-day jump in the pandemic.
San Bernardino and Orange counties are the only others that have more than 1,000 coronavirus-positive patients, according to state data.
Southern California and the Central Valley are by far the state’s biggest contributors of total COVID-19 deaths in the last week.
Hospitals can take steps to gird themselves against an influx of new patients — by canceling scheduled surgeries and outpatient visits; discharging patients as quickly as possible; and temporarily diverting ambulances with certain types of patients, for instance.
But ICU beds require high-tech equipment and specially trained healthcare professionals, which are in high demand throughout the state and nation.
Healthcare systems can move trained staff around to help plug gaps where needed, but “at a certain point, you run out of options, and that’s what we’re worried about,” Simon said.
“The worst-case scenario is what we saw back in the spring in New York City and in northern Italy where there were literally people in gurneys in hallways that were dying or near death, and that’s beyond a tragedy,” he said. “It’s just something that we can’t let happen. We have to do everything possible to prevent that.”
As officials met to discuss approval of a coronavirus vaccine on Thursday, the number of cases and deaths grew ever more stunning.
The way the state calculates regional ICU capacity is more complicated “than just looking at how many beds are full at any given point in time,” said Ferrer.
She said Wednesday that the state had set a threshold that only 30% of ICU beds should be occupied by COVID-19 patients and that, should an area exceed that, “they make a downward adjustment — sort of, you get a penalty.”
The California Department of Public Health elaborated in response to an inquiry from The Times Thursday: “If a region is utilizing more than 30% of its ICU beds for COVID-19 positive patients, then its available ICU capacity is reduced by 0.5% for each 1% over the 30% threshold. This is done to preserve the capacity of the ICU to also treat non-COVID-19 conditions.”
“The ICU is an important tool to save lives for those with COVID-19 and other critical medical conditions such as cancer, heart attacks and strokes,” the department statement continued. “If a disproportionate number of ICU beds are being utilized to treat COVID-19 patients, then patients with non-COVID medical issues may not be receiving or be able to receive the level of care they need.”
According to data provided by Los Angeles County, 47% of the region’s intensive care beds were filled with COVID-19 patients as of Tuesday. That’s a significant cause for alarm, officials said.
“We’re always going to need ICU beds for those many other conditions and so there is greater concern if, in addition to seeing a reduced overall capacity, we’re seeing a greater proportion of these ICU beds taken up by COVID-19 patients,” Simon said.
How California determines ICU availability is of keen interest, as that’s the metric the state uses to determine whether to hand down additional restrictions on businesses and activities.
The state is implementing new stay-at-home orders in any region that sees its ICU capacity drop below 15%.
Those orders — which reduce capacity at retail stores; close businesses including hair salons, nail salons, card rooms, museums, zoos and aquariums; and prohibit outdoor restaurant dining — are already in place in Southern California and the San Joaquin Valley.
Those restrictions will also go into effect in Greater Sacramento beginning Thursday night.
Officials have said they hope the additional restrictions will help stymie the latest coronavirus surge.
Given how widespread the virus is in communities up and down the state, experts say the best thing residents can do to keep themselves and their loved ones from being infected is to stay home as much as possible over the next few weeks.
“To be blunt, we have one chance to turn this serious surge around, and that chance is right now,” San Francisco health director Dr. Grant Colfax said this week. “But our window is narrowing and closing fast.”
With grim case counts, officials have pointed to the relief a vaccine will soon bring as a way to encourage people to continue to maintain precautions.
Ferrer announced earlier this week that the county would likely get its first doses of the coronavirus vaccine as early as next week. During a Thursday news conference, L.A. Mayor Eric Garcetti said that as many as 500,000 doses may be distributed by the end of December.
“Vaccines will be our most important tool in getting this crisis under control,” he said. “FDA authorization will mean that it’s safe and that it’s effective, and I urge all Angelenos to get vaccinated as soon as they qualify and those vaccines are available.”
He urged residents, however, to continue to stay at home as much as possible, stating that “the worst is not yet behind us.”
Times staff writers Maura Dolan, Ryan Menezes and Leila Miller contributed to this report.
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.