ICU capacity explained: What to know about a key coronavirus metric in California
- Share via
Coronavirus cases are surging, hospitalizations are rising and public health officials are increasingly watching an important metric: intensive care unit capacity.
The new stay-at-home order that hit 36 million Californians recently was triggered when several regions’ ICU availability slipped under 15%.
Public health officials fear that as the surge continues, hospitals could be overwhelmed — including the most vulnerable patients in the hospitals’ highest level care units. Staying home and preventing coronavirus infections will help hospitals manage the influx of patients. As officials wait and hope for the stay-at-home order to tame the surge, they are anxiously tracking ICU capacity.
Here’s what you need to know about ICU capacity and why it’s important at this stage of the pandemic.
What is an ICU?
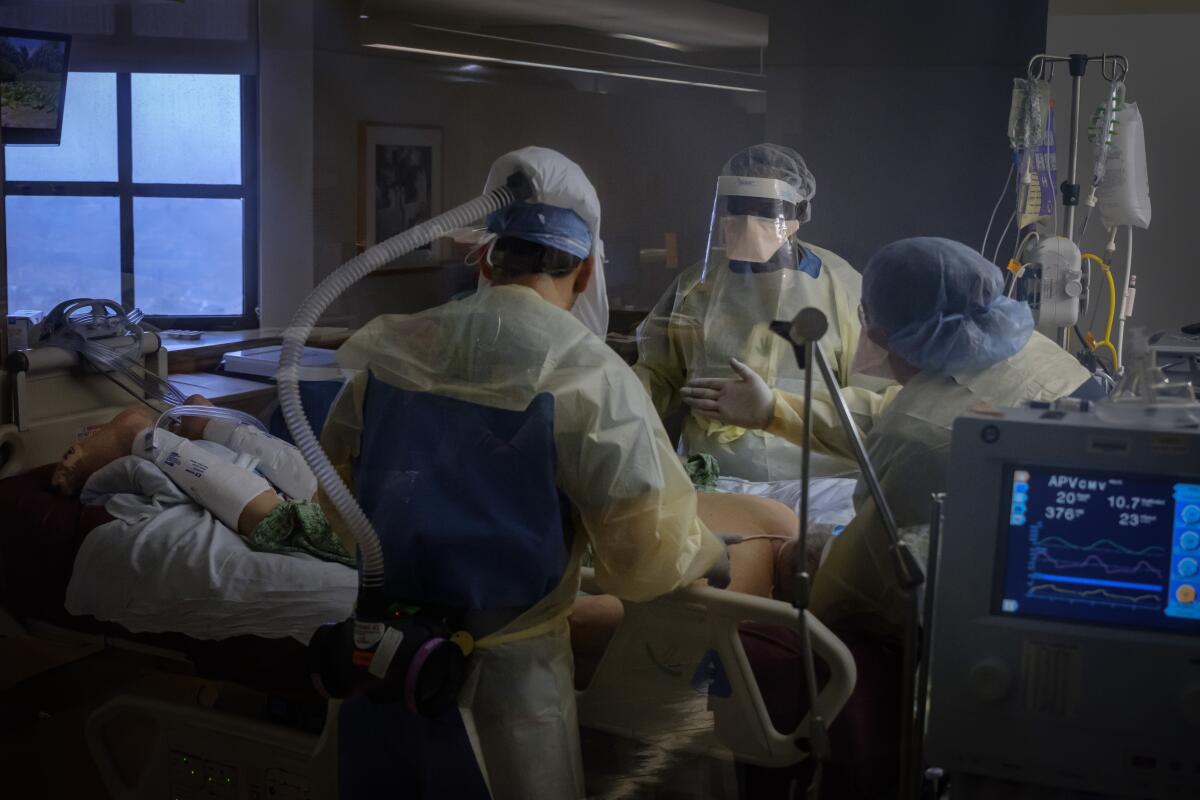
An ICU, or intensive care unit, is a specialized hospital department that cares for people in the most critical health situations, such as those with life-threatening injuries or severe illnesses. ICUs are equipped with specialized equipment, such as ventilators.
Most important, ICUs are staffed with highly trained nurses and physicians who provide round-the-clock care to their patients — checking their breathing, blood pressure, fluids and other vital signs. Dr. Shruti Gohil, an infectious disease specialist at UCI Health, said there is a 1-to-1 ratio of nurses to patients in ICUs.
“That kind of minute-to-minute, hour-to-hour care requires a level of training on the nurses to ... recognize problems quickly and address them quickly and then know what needs to be done while waiting,” Gohil said.
A COVID-19 patient with severe difficulty breathing may require ventilator support in an ICU.
“We are responding at the moment to a tsunami of COVID-19 patients in the hospital,” said Carmela Coyle, president and chief executive of the California Hospital Assn. “But that does not stop the heart attacks, the strokes, the cancer patients with serious, immediate needs.”
What is ICU capacity?
Capacity is the number of staffed beds available at a point in time.
Determining whether capacity has been reached is more nebulous.
The state determines a region’s ICU capacity with a weighted formula to ensure that some ICU beds remain open for non-COVID patients. When the state says a region has reached 0%, it may actually still have some beds available. Individual counties, such as Fresno, have reported having no open ICU beds.
Capacity also fluctuates as patients exit the ICU and others enter.
“There’s always sort of this movement that’s not always quite captured by the snapshots that we get,” said Dr. Rais Vohra, interim health officer for Fresno County. “Overall, the capacity is severely impacted.”
What happens when an ICU reaches 0% capacity?
Hospitals will likely place patients in open beds elsewhere in the hospital, such as emergency department rooms.
Having open beds in other parts of the hospital does not mean a hospital is equipped to handle more intensive care patients. Dr. Bill Stringer, chief pulmonologist at Harbor-UCLA Medical Center in Torrance, said the “limiting step is not going to be space or equipment. It’s going to be staff.”
Because of their specialized training in high-intensity situations, ICU medical professionals are scarce resources.
ICU availability in Southern California at 0%, and the crisis is expected to get worse, officials warn.
“The problem is, we’ve got a nationwide shortage of critical care nurses,” Coyle said. “It is not the case where you can pull any nurse into the ICU to provide that level of care.”
And when ICUs are stretched beyond capacity, the quality of care can decline and mortality rates can rise.
As ICU capacity shrinks, a hospital is likely to scale back elective procedures, freeing up staff. Some healthcare workers — such as those who work in trauma, surgery and anesthesia — are already trained for high-stress scenarios, so they would be “natural pivots” to the ICU, Gohil said. A critical care professional would supervise.
“In a poor, catastrophic state, it would be an all-hands-on-deck approach,” Gohil said.
If a hospital’s beds fill, some patients may be transferred to neighboring hospitals. But moving ICU patients is risky, Stringer said.
“Just imagine somebody who is just completely inert, that is sedated, that is being supported at least with a ventilator,” Stringer said. “It’s the most fragile and vulnerable patient being transferred. That’s a very difficult decision.”
How do I find out the ICU capacity where I live?
The state keeps an updated list of ICU bed availability by county.
Hospitals report their capacities daily, and the state tallies them.
Here are the regional numbers as of Thursday afternoon:
- Southern California: 7.7%, down from 9% Wednesday
- San Joaquin Valley: 1.9%, down from 4.2%
- Greater Sacramento: 13.3%, down from 14.3%
- Bay Area: 17.8%, down from 20.9%
- Northern California: 30.3%, an improvement from 27.1%
I live in a region where ICU space is at capacity, but I have a medical emergency. What do I do?
You should still seek help. If you’re in a serious emergency, call 911.
Otherwise, Stringer said, call the hospital emergency departments near you to check their capacity. Then wear a mask and go.
“The hospital, even though we have plenty of COVID patients, is still a safe place to get care,” Stringer said. “It’s probably not as safe as being on a backpacking trip in the Rockies. But if you’ve got an emergency, you need to call.”
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.






![Vista, California-Apri 2, 2025-Hours after undergoing dental surgery a 9-year-old girl was found unresponsive in her home, officials are investigating what caused her death. On March 18, Silvanna Moreno was placed under anesthesia for a dental surgery at Dreamtime Dentistry, a dental facility that "strive[s] to be the premier office for sedation dentistry in Vitsa, CA. (Google Maps)](https://ca-times.brightspotcdn.com/dims4/default/07a58b2/2147483647/strip/true/crop/2016x1344+29+0/resize/840x560!/quality/75/?url=https%3A%2F%2Fcalifornia-times-brightspot.s3.amazonaws.com%2F78%2Ffd%2F9bbf9b62489fa209f9c67df2e472%2Fla-me-dreamtime-dentist-01.jpg)







