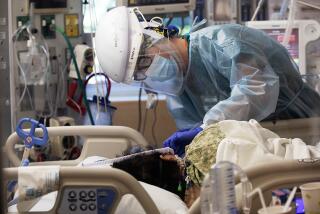
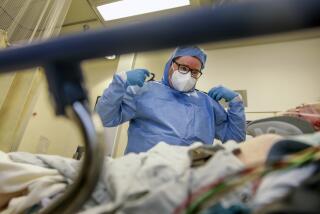
With ICUs 100% full, Marin County turns down calls for help from San Joaquin Valley
- Share via
Marin County this week reported that it has 0% intensive care unit beds available and workers in the county north of San Francisco were being stretched thin.
Marin County Supervisor Damon Connolly said at a public meeting this week that some healthcare workers “are pulling double shifts and working tirelessly to save lives.”
But the loss of available ICU beds due to the worsening COVID-19 pandemic is leaving few good options. Marin County has already had to turn down requests to accept patients from overloaded hospitals in the San Joaquin Valley region, which has seen its ICU availability drop to zero in recent days and has appealed to other regions to accept as many as 40 patients.
“We’re not allowing patients from the outside to come into our ICUs right now, because we’re not able to accept them,” Dr. Matt Willis, the Marin County health officer, told the Marin County Board of Supervisors this week.
Dr. Laura Eberhard, chief of the critical care department at Kaiser Permanente San Rafael Medical Center, told the Board of Supervisors in a video message that she has never seen anything like this surge in her 20 years of caring for the critically ill in Marin County.
“As an ICU doctor I’m not scared by much,” Eberhard said. “But I find the prospect of having a hospital and an ICU overflowing — and concerned about not being able to take good care of our residents of Marin — I find that scary.
“We’re not the first line, we are the last line,” Eberhard said. She urged the community to follow public health orders to stay home as much as possible.
“It really starts with our community by the time people get to us. It’s really late in the game. Only our community really can stop this epidemic,” Eberhard said.
In response to the crisis, some hospitals are canceling scheduled procedures and asking ICU nurses to take care of multiple patients.
Marin County, however, hasn’t yet had to raise nursing ratios just yet. “That will be one of the first things that would start to erode as we start to see more cases coming in,” Willis, told the Board of Supervisors this week.
Other options include asking other nurses to take a quick online training course so they can help care for critically ill patients.
“Those are probably the most important measures that can be taken right now. And none of them are good. I mean, none of them feel safe,” Willis said. “And that’s why the only ultimate solution is to reduce the number of people going in with infections that require critical care.”
Few of the options a hospital could normally take to reduce strain on its ICU are available with the entire nation facing the same crisis simultaneously. Bringing in outside, traveling nurses is not really possible.
“The historical systems are not working right now, because there’s never been a level of strain on the system as a whole,” Willis said.
“As soon as we start encroaching into those other elements, it also immediately begins to affect the standard of care,” Willis said. “So each of these steps we would take to increase our functional ICU capacity has an associated harm that we would need to take into account.”
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.