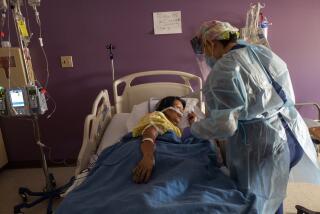Paramedics having some patients stay home as hospitals struggle with COVID-19 wave
- Share via
Paramedics and emergency medical technicians are declining to transport some less severely ill patients whom they might take to the hospital under ordinary circumstances, one of the many extreme steps being taken in Los Angeles County to deal with the COVID-19 surge crippling hospitals.
It’s one of a limited number of tools left to deal with the wave amid a crisis due to a flood of COVID-19 patients.
In Los Angeles County, EMTs “are assessing patients and releasing them to stay at home, because they aren’t quite sick enough to need hospital-level care. ... If they did come to the hospital, they may not get the type of attention that they might expect,” said Dr. Mark Ghaly, the California health and human services secretary.
Many hospitals are now going to contingency care, in which staffers work longer hours and wards are reconfigured to take more patients. The next step could be “crisis care,” in which more medical rationing would occur.
State officials have yet to hear reports of the direst circumstances, such as a hospital having to choose who gets the last ventilator. But there are fears that day could come.
For the first time, the number of people hospitalized for COVID-19 statewide has exceeded 20,000, a figure eight times higher than that on Nov. 1.
In Southern California, hospitals are at the breaking point, doing all they can to treat patients with the staff they have.
Providence St. Joseph of Orange has been working at a constant level of overcapacity, and ambulances that would usually drop off patients at smaller hospitals have increasingly become more frequent.
The situation is “overwhelming and growing daily,” said Dr. Glenn Raup, executive director for critical care, emergency and behavioral health services, in describing the increase in COVID-19 patients at the hospital. “This wave started with a lot more of a vengeance.”
On Tuesday, it had about 250 COVID-19 patients. Staffed beds were 67% over capacity, he said, a number that is constantly fluctuating but has remained the norm for the last month.
“That is a very hard thing for a hospital to maintain that day in and day out,” Raup said. “That’s 67% more staff, 67% more resources, such as oxygen.” The signs of how much worse the situation could get are there.
Hospitals in lower-income, densely populated and nonwhite communities face the greatest challenge in providing care, a Times data analysis finds.
Raup said the hospital was put on notice by distributors that distribution and creation of oxygen and oxygen tanks are becoming a concern. “We’re trying to be very frugal in how we use and when we use and where we use and how much we use of the oxygen reserves that we do have,” Raup said.
Here is what is going on now in hospitals and what would come:
What are strategies medical officials are now using?
Hospital systems are already coming up with triage plans, which entail prioritizing the time of highly trained staff — such as respiratory therapists, ICU nurses and critical care doctors — in a way to keep as many people alive as possible. That means that those less likely to survive might not receive the same level of care they would have otherwise.
Most hospitals in California are no longer able to offer regular hospital services, switching instead to “contingency care,” Ghaly said, in which staff are asked to work longer shifts, hospital rooms are reconfigured to hold more beds than originally intended, scarce supplies are conserved or even reused and the movement of patients within the hospital is delayed because of a lack of space or staff.
What would ‘crisis care’ look like?
Even worse is “crisis care,” when patients are placed on cots instead of standard hospital beds; patients normally grouped in one unit are scattered across the facility; and certain supplies, therapies and staff need to be rationed, Ghaly said.
If some hospitals in a region declare that they’re in “crisis care” mode, other hospitals in the region will be asked to share their resources to relieve the worst-hit facilities, Ghaly said.
Kim McCoy Wade, director of the California Department of Aging, said Tuesday that tough decisions on how to allocate medical care must be “grounded in the likelihood of [a patient] surviving in the near term.”
Such decisions cannot be based on age, race, disability, chronic medical conditions, gender, sexual orientation, gender identity, ethnicity, national origin, language spoken, ability to pay, weight, socioeconomic status, insurance status, perceived self-worth, perceived quality of life, immigration status, incarceration status, homelessness or past or future use of resources, she said.
The state Department of Public Health on Monday issued a memo about its “California Crisis Care Continuum Guidelines,” which, they said, must follow ethical principles, health equity goals and civil rights laws. Facilities that need to begin to ration critical care resources must notify local and state public health departments immediately.
According to a state memo issued in June, in a situation when there is a severe shortage of medical resources and a patient has a poor immediate survival prognosis, healthcare providers may need to decide to give palliative care aimed at providing patients relief from pain as they die, rather than improving their prognosis.
When it comes to deciding who is eligible for ICU admission or should have access to a ventilator, patients who are more likely to survive with such care will receive priority.
A hospital-appointed triage officer is expected to make decisions to benefit populations of patients, “even though these decisions may not necessarily be best for some individual patients,” according to the memo.
What has the trendline looked like?
At Providence St. Joseph of Orange, November began as a quiet month for the hospital, reaching its lowest number of COVID-19 patients since March, said Jeremy Zoch, chief executive of the hospital.
But that is no longer the case. COVID-19 patients, who once shared rooms with one other person, are now four to a room, and the hospital placed 12 beds in what was once the neonatal intensive care unit. There are plans in place to move into other parts of the hospital if needed, but staff across all parts of the hospital has been stretched thin — last week, Zoch said he worked the tray line to help serve food because it was short-staffed.
“It’s really pushed us to the absolute max,” he said.
A majority of patients are now coming in with COVID-19, Raup said, but the staff has managed to triage patients needing ICU beds.
On any given day, the number of people waiting for an ICU bed can range from a couple to 10 on particularly bad days. Raup, who helped during Hurricane Katrina, has been through trying moments like going without a ventilator and having people come off ventilators.
He knows what it’s like to go through a disaster, and the hospital has so far been prepared for a worsening situation. The surges of patients is comparable to what happens after a hurricane, he said, with surges of people getting sick. But he worries that some individuals have not done enough to take precautionary measures seriously, and the coming month, after Christmas and New Year’s, could push the hospital further.
Orange County has been ground zero for protests against measures to stop the spread of COVID-19.
“This is ongoing, and individuals and communities need to recognize that, like any viral condition, you really have to be diligent for a longer period of time if you really want to return to what you consider a state of normalcy,” Raup said. “And I think that’s where everybody’s tired. And unfortunately, that fatigue in the community is going to lead to more stress on the hospitals.”
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.