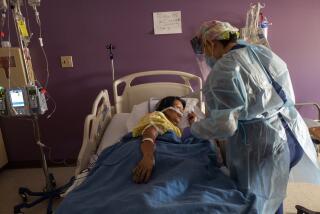L.A. County hospitals are losing the battle against COVID-19 surge as problems multiply

- Share via
Hospitals across Los Angeles County were fighting a losing fight Tuesday to stay ahead of the coronavirus surge as the number of hospitalized COVID-19 patients topped 8,000 and the countywide coronavirus death toll rose by nearly 1,300 in the last week.
L.A. County hit another distressing milestone, surpassing 11,000 deaths Tuesday since the beginning of the pandemic. Officials warned that conditions will only worsen in coming weeks as people infected during the holidays become sick and need medical care.
More than 2,200 people who work at hospitals in L.A. County tested positive for the coronavirus in December alone.
“It is getting harder and harder for healthcare workers to care for those coming to the hospital with gunshot wounds, heart attacks, strokes and injuries from car accidents,” said Los Angeles County Supervisor Hilda Solis. “Hospitals are declaring internal disasters and having to open church gyms to serve as hospital units.”
Over the past week, L.A. County averaged 183 COVID-19 deaths a day — the equivalent of one every eight minutes — and 13,500 new coronavirus infections, a count expected to grow with the reopening of testing sites after the holidays. The county’s cumulative coronavirus case count now tops 841,000.
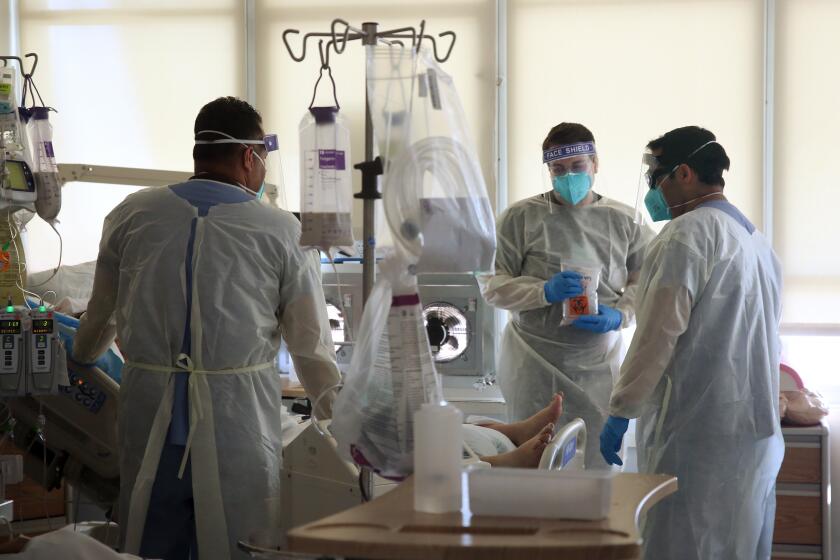
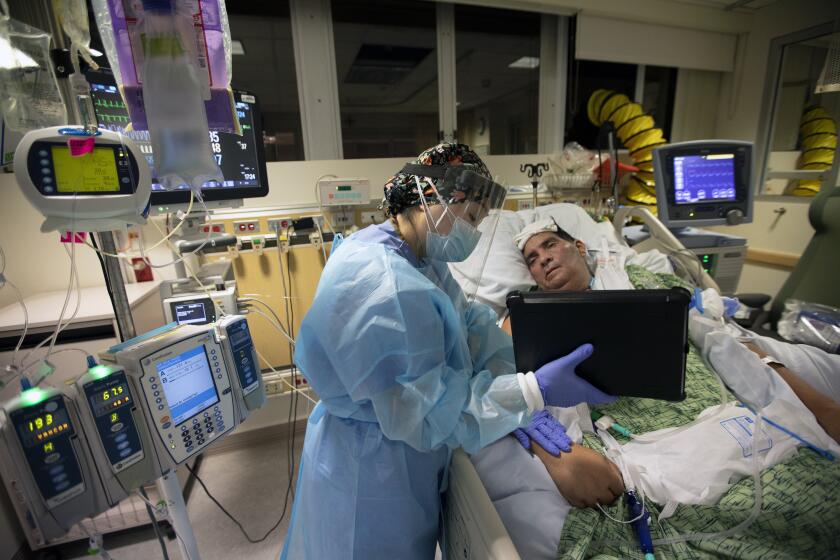
Hospital staffing remains stressed across the county, and officials have warned that the quality of care is being compromised. Over three-quarters of the patients in ICUs have COVID-19.
All hospitals are experiencing a large number of staff members unable to work because they are under isolation or quarantine, Dr. Christina Ghaly, the L.A. County director of health services, told the county Board of Supervisors on Tuesday.
Another major problem is being able to quickly discharge patients. Across the four county-run hospitals, about 10% of hospital patients no longer need hospital care, yet “we’re having a number of problems and delays in moving them out” to lower levels of care settings, such as nursing homes, Ghaly said.
Some nursing homes are refusing patients from hospitals; sometimes, patients don’t want to be moved to a lower level of care and state law prohibits the movement of a patient unless the person agrees to the placement. Skilled nursing facilities and other areas that can provide lower levels of care are facing their own staffing shortages, limiting the number of patients they can take in.
Dialysis centers are starting to struggle with staffing shortages, too, and there are now not enough outpatient dialysis resources available. That’s causing problems because hospitals are unable to discharge patients from hospitals when there’s not enough of outpatient dialysis chairs available to accommodate them. Dialysis facilities are also sending patients to the emergency room to receive coronavirus testing rather than performing the testing at the site of the dialysis center, Ghaly said.
It has also been hard to find portable oxygen canisters needed to send patients home from hospitals who still need oxygen treatment. There’s a shortage of canisters needed to transport oxygen around the hospitals and to store them in tents that are being used to provide care for patients.
Like facilities across California, the county-run hospital system is struggling to find temporary medical staff to backfill the staffing shortage. The county hospital system has increased its offer of pay to find contract medical staff and submitted requests for help to the state.
So far, the county-run system has received 36 contract nurses from the state and is anticipating two 20-person medical teams from the U.S. Department of Defense, which will be deployed at Harbor-UCLA Medical Center near Torrance and L.A. County-USC Medical Center on the Eastside this week.
Problems on Sunday caused at least five hospitals in L.A. County to declare an internal disaster, which closed the facilities to all ambulance traffic.
Five privately run hospitals in L.A. County are also due to receive federal health teams to support medical staffing, Ghaly said.
The biggest source of additional hospital staffing is coming from the county’s own outpatient clinics.
The county has closed five of its public outpatient clinics and reduced hours and services at the rest of them to divert more than 800 nurses and other staff to work in emergency departments and quarantine-and-isolation sites for people who have COVID-19 or have been exposed to the virus.
The county-run hospital system has already ordered more ventilators, BiPAP machines and more high-flow oxygen devices — all devices intended to help patients breathe — and officials do not believe there will be a supply problem for those devices in the coming weeks, Ghaly said.
Two of the county-run hospitals have had problems with the delivery of oxygen in the hospital to their patients, Ghaly said. Olive View-UCLA Medical Center in Sylmar has resolved its issue of oxygen freezing in its pipes; Harbor-UCLA Medical Center is still having a problem with the flow of oxygen through its pipes. It’s not creating urgent patient care issues at Harbor-UCLA, “but it does provide some limitations into which physical spaces within Harbor we can use to keep patients,” Ghaly said.
Amid the already overwhelming surge, California faces another potential threat: the presence of a new coronavirus variant, which has grown rapidly in England, that some scientists believe is more likely than the conventional version to infect people who are exposed to it.
Officials in San Diego County report 32 cases of the potentially more contagious variant of the coronavirus that has also spread rapidly in England.
Though it’s unclear how prevalent the variant is statewide, San Diego County health officials Tuesday reported 24 additional confirmed cases and four likely cases. That raises the county’s total of known or suspected infections by the variant virus to 32.
The two dozen newly infected patients “are believed to have no travel history and to have come from 19 different households, but the investigation and contact tracing are ongoing,” according to a statement by San Diego County officials. Those infected are widely dispersed geographically and range in age from 10 to their 70s.
The variant has also been identified in two people of the same household in Big Bear in San Bernardino County.
Experts say there’s no evidence that, once it infects a person, the variant — known as B.1.1.7 — is more likely to cause death, more severe illness or renders vaccines less effective. But any heightened risk of infection is unwelcome news, particularly in areas already reeling from sky-high levels of coronavirus transmission.
Though L.A. County officials have yet to document the variant’s presence, “having a virus that is able to infect more people more quickly than what we’re seeing today” is a “frightening thought,” county Public Health Director Barbara Ferrer said Tuesday.
Although many of those infected may experience only mild symptoms or none at all, California health officials have warned that a sizable slice, about 12%, will fall ill enough to require hospitalization within a few weeks after they are exposed. Twelve percent of people who are hospitalized end up in the intensive care unit.
The number of COVID-19 patients in the county’s beleaguered hospitals has hit a new all-time high
A significant and sustained wave of new infections, then, will invariably slam hospitals with additional patients.
State officials have asked hospitals to come up with a plan in which they must offer “crisis standards of care,” in which the most severe form of catastrophe has arrived at the hospital and, in the worst-case scenario, forces certain supplies, therapies and staff to be rationed.
In such a situation, it would be necessary to prioritize the time of highly trained staff — such as respiratory therapists, ICU nurses and critical care doctors — in a way to keep as many people alive as possible. That means that those less likely to survive might not receive the same level of care they would have otherwise.
According to a state memo issued in June, in a situation when there is a severe shortage of medical resources and a patient has a poor immediate survival prognosis, healthcare providers may need to decide to give palliative care aimed at providing patients relief from pain as they die, rather than improving their prognosis.
When it comes to deciding who is eligible for ICU admission or should have access to a ventilator, patients who are more likely to survive with such care will receive priority.
A hospital-appointed triage officer is expected to make decisions to benefit populations of patients, “even though these decisions may not necessarily be best for some individual patients,” according to the memo.
The L.A. County Department of Public Health said Tuesday night that no hospital has formally declared to the county that they are operating under “crisis standards of care.”
Times staff writer Andrea Roberson contributed to this report.
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.