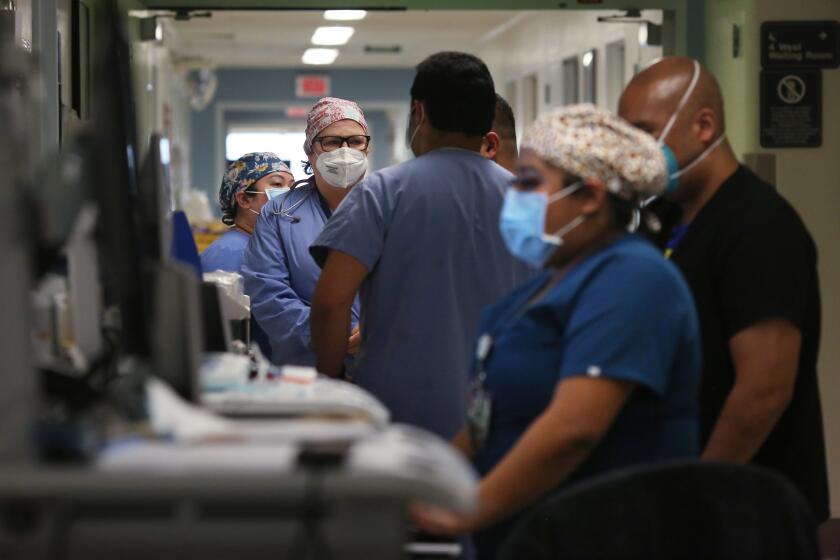
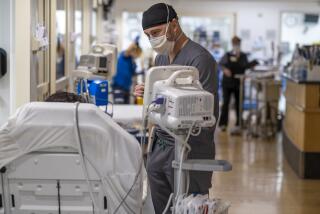
As bodies pile up at hospital morgues, National Guard and refrigerated trucks arrive to help
- Share via
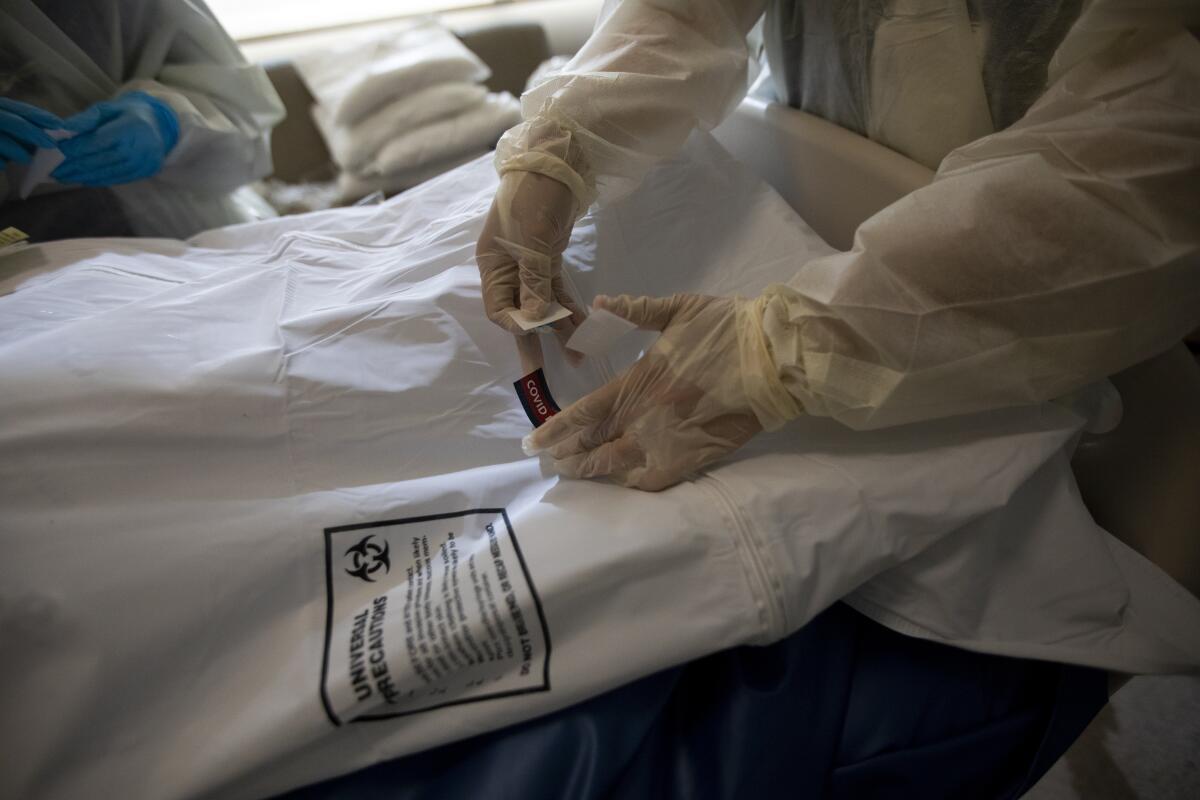
The intensity of the pandemic continues to worsen, with the rising COVID-19 death toll overwhelming funeral homes and causing state officials to send refrigerated trucks across California to hold corpses.
The National Guard has been called to Los Angeles County to help with the temporary storage of bodies at the county medical examiner-coroner’s office, relieving pressure on hospital morgues and private mortuaries that have run out of storage space for bodies.
Deaths from COVID-19 have been spiking both in L.A. County and the rest of California. Earlier this week, L.A. County exceeded 11,000 COVID-19 deaths. Officials warned of dark weeks ahead amid a post-Christmas surge that is expected to put pressure on already overwhelmed hospitals.
There have been, on average, 183 deaths reported each day over the last week, and nearly 1,600 deaths have been recorded since Dec. 30.
Worried public health officials said the region was losing its battle against COVID-19, adding that only immediate and decisive changes can prevent a steep rise in deaths.
Many hospital morgues are now filled with bodies, and officials are trying to move them for temporary storage at the county medical examiner-coroner’s office.
Mortuary and funeral home operators say they are having to turn away bereaved families because they don’t have the capacity to handle more bodies.
Officials said last week that the California National Guard was being called in to help county workers as corpses from hospital morgues are moved into storage at the L.A. County Department of the Medical Examiner-Coroner.
Among the hospitals with refrigerated trucks is Harbor-UCLA Medical Center, one of many hospitals where the morgues have been full.
As of last week, guard troops were stationed at 13 medical facilities in the state, including Adventist Health White Memorial in Los Angeles, Methodist Hospital of Southern California in Arcadia and Pacifica Hospital of the Valley in Sun Valley.
Each team consists of six to 10 medical corps members, led by a physician or a nurse. Some facilities, such as El Centro Regional Medical Center in Imperial County, have two teams.
Lt. Col. Jonathan Shiroma, a spokesman with California National Guard, told The Times last week there has been “more of an effort to help the civilian healthcare providers, by providing them additional support through our military.”
L.A. County Supervisor Janice Hahn had requested the return to Southern California of the Navy hospital ship USNS Mercy.
But the state said this week the Mercy “is now under mandatory maintenance, in dry dock, and not available for deployment.” Instead, California is asking for an additional 500 federal medical personnel, officials said Wednesday.
Hospitals across L.A. County are reporting significant shortages of staff, with so many employees out sick or on quarantine, and officials have warned they’re running out of ambulances, with emergency rooms so full that ambulances must sometimes wait hours to drop off patients, which forces those calling 911 to wait even longer for paramedics and emergency medical technicians to arrive.
L.A. County health agency tells EMTs not to transport by ambulance those who have virtually no chance at recovery.
The ambulance shortage is so dangerous that officials have instituted an emergency setting that will allow paramedics and emergency medical technicians to drop off patients at tents outside emergency rooms, with a paramedic or EMT monitoring up to four patients there. This will allow ambulances to return to circulation faster, rather than waiting to offload patients.
Hospital intensive care units are so crowded that critically ill patients must stay in the emergency rooms for long periods of time, and often, ICU beds become available only after a COVID-19 patient dies.
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.