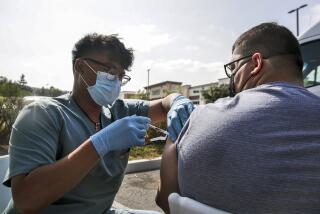
Chaotic COVID-19 vaccine rollout leads to more deaths, experts say
- Share via
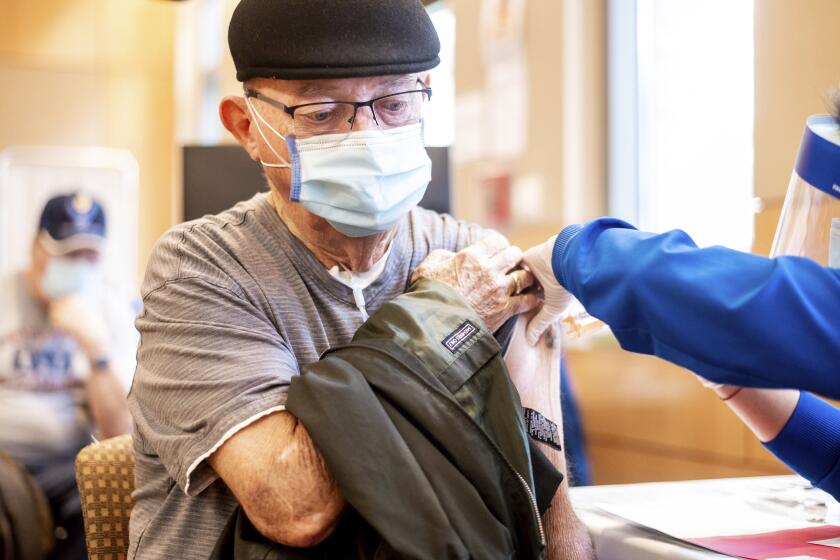
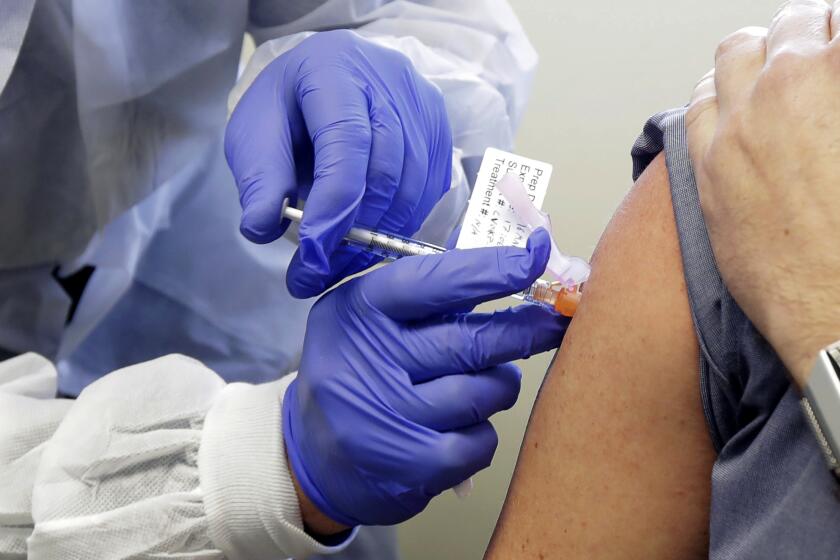
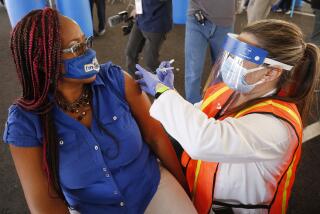
As roughly 4,000 Americans die each day from COVID-19, public health and medical experts are aghast that the vaccines that could save them remain beyond reach — due to multiple governmental failures involving planning, coordination and public communication.
“Many people are eager to get the vaccine, and they want to know when and where they are going to get it,” said Dr. Eric Toner, a senior scholar with the Johns Hopkins Center for Health Security. “For the most part, people at the local level don’t know, and people at the state level are still trying to figure it out.”
Calls to doctor offices and pharmacies about vaccines yield no answers, leaving people frustrated and anxious. Emails from doctors’ offices lack specifics. County public health websites may offer the best information, and people in some places can use them to sign up for vaccinations.
Some experts said the situation should vastly improve within a couple of weeks, but for now, most people who want to know more about being vaccinated may just have to wait.
“Almost every practical question I ask anybody, the answer I get is a shrug of the shoulders,” said Dr. Robert Wachter, professor and chair of the Department of Medicine at UC San Francisco. “It is not good. It just feels like the plans have been made without any attention to the practicalities of the last mile.”
The botched rollout of COVID-19 vaccines starts at the top, with President Trump. His Health and Human Resources Secretary, Alex Azar, promised on Dec. 10 that 20 million Americans would be vaccinated within several weeks. As of Monday, only 9 million had been vaccinated, according to the CDC, and administration officials have acknowledged a “planning error” for the unavailability of doses.
Until now, vaccines had been reserved mostly for first responders and health care workers. But now, people 65 and over can also get vaccines. Here’s what the changes mean.
On the state level, vaccine distribution is being at least partially slowed by technical problems with a software program used by California, as The Times reported Friday, citing state and local officials. Another problem is the vast number of healthcare providers across the state and nation, including pharmacy chains, slow to prepare communication plans to notify nearby eligible people that they can come in and quickly get vaccinated.
A Los Angeles writer, 67, said that she called her doctor’s office in Pasadena and her local pharmacy on Tuesday after hearing that Gov. Gavin Newsom had promised to speed up vaccinations.
Her doctor’s office “said they have gotten no instructions about dispensing the vaccine,” said the resident, who asked that her name not be used because she didn’t want others to know of her anxiety. Her local Walgreens also said “they hadn’t heard anything yet.” She said she also signed up at the county to be notified about vaccines, but has not yet received any emails.
“Really stunning,” she said, about the lack of information.
Dr. John Swartzberg, a UC Berkeley infectious disease expert, said he gets emails from people he doesn’t know asking him when they will be informed about how to get the vaccine.
“We have done a miracle thing in developing these vaccines,” Swartzberg said, “but it is ironic that things we know how to do and can do [vaccinations] we just are not doing.”
Lack of adequate funding for the vaccine rollout has left states about two months behind in planning, he said. Health economists projected the states would need $8.4 billion for the vaccination campaign, but until recently were given only $400 million, he said.
Wait times for vaccines still could last weeks as counties struggle to keep up with demand.
“The money should have come two months ago,” he said. “We don’t have time. Every month we lose between 2,500 and 3,000 people a day [to COVID-19].”
Walgreens, which did not immediately return a call for comment, says on its website that it has “remained on track” vaccinating nursing home residents and other vulnerable populations prioritized for first vaccines. Vaccines eventually will be given at all of Walgreen’s 9,000 stores, and people will be able to schedule inoculations on a Walgreen’s app or online, the chain said.
As of Wednesday, California had administered 816,301 vaccines, according to the CDC. Its vaccination rate of 2,066 per 100,000 people places it among the lower tier of states.
Faced with criticism, California recently loosened rules for who may be vaccinated, and the locations of future mass vaccination sites were announced this week.
The California Department of Public Health, in response to emailed questions from The Times, said healthcare workers should contact their employers, nursing home residents their caretakers and the public their doctors for information about vaccines. The Los Angeles County Department of Public Health did not make logistic experts available to answer questions.
Dr. David P. Eisenman, a UCLA professor of medicine and public health and director of the Center for Public Health and Disasters, said public health departments have long been overstretched.
At a time when they also are overwhelmed with a huge virus surge, “they have to design these massive vaccination programs, and they don’t know where to start,” he said.
“It is much harder in the United States,” he added, “where we have so much private healthcare that has little to no connection established with public health departments.”
Vaccine distributors also have been afraid to provide injections to people who are not in the priority group, even when not doing so may result in the loss of the vaccine, he said. He cited an isolated Los Angeles County community that had unfrozen vials of the vaccine left and decided to call its local utility to send people over.
When a freezer malfunctioned, a small Ukiah hospital had to use or lose its Moderna COVID dosages quickly, becoming a case study in mass inoculation.
“They were smart to do it,” he said, declining to identify the community. The prioritized lists for vaccinations “are guidelines, not mandates,” he said.
Vaccines have made COVID-19 a “highly preventable disease at this point, so the sooner you get it to people who are most likely to die, the sooner we can reduce deaths,” he said.
Lack of funding for planning was only part of the problem, said Dr. Ori Tzvieli, deputy health officer for Contra Costa County.
“You need to know how much vaccine you are going to have,” Tzvieli said. “The lack of forecasting, of clear expectation of how much vaccine you are going to have, has made it hard to plan that well. That has been a frustrating factor, but I think it is getting a little bit better.”
Counties like Contra Costa have dusted off older, mass vaccination plans for the COVID-19 effort, “but each vaccine is different,” he said.
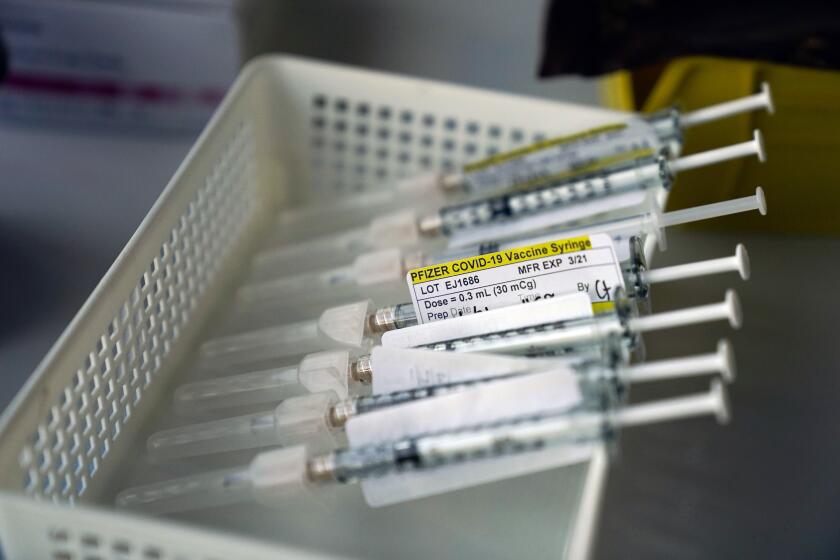
The COVID-19 vaccines now being disseminated must be given in two doses and kept in special freezers, and the state has established the rules about who should get the vaccine first.
“All of that is unique to each pandemic,” Tzvieli said. Participating pharmacies had to obtain freezers and staff to start the vaccination process, and healthcare professionals like dentists had to be trained for the job, many of them through online courses.
But Tzvieli said he remains “really optimistic” and believes all the residents in the county who want vaccines will have them by summer.
The county began vaccinating about 700 individuals a day and will soon be up to 4,000 a day. “I think it will be totally different two weeks from now,” he said. “There will be a lot more vaccine moving.”
Wachter of UC San Francisco said the vague rules about eligibility for vaccines make it “just ripe for shenanigans.”
“I have heard of venture capitalists going to work for Uber for a day just to get a vaccine,” he said.
Tzvieli said his health department was not policing applicants. Contra Costa offers online vaccination appointments for health workers and people 75 and older who self-certify their eligibility. “We are not spending a lot of our energy on trying to catch the line skippers,” Tzvieli said. “We really trust that most people will tell the truth.”
Confusion also sets in when the rules appear to change. The Trump administration decided this week that people 65 and older should be given priority for vaccines. New York Gov. Andrew Cuomo said Tuesday that vaccine eligibility would be opened to that age group.
In California, Health and Human Services Secretary Dr. Mark Ghaly said Tuesday that Newsom had directed a vaccine advisory committee to consider the new federal guidance. On Wednesday, the state said people 65 and older would be in the next eligibility group.
On top of the information vacuum, scammers may be at work. Santa Clara County reported Tuesday that some residents have received text messages about “extra” vaccine being available with registration links for appointments. The county called it “misinformation” and said it was investigating the source of the advisories.
For now, the vaccine is still designated for medical personnel and first responders. But officials expect to provide details soon about the next wave.
Eligibility requirements for vaccines also have led to questions about how people will prove they are entitled to injections. For certain occupations, people may need to bring pay stubs, John Hopkins’ Toner said. When the vaccinating category involves people with underlying health conditions, proof might be trickier.
Toner said health insurers have information about patients’ underlying conditions, but “whether the states have engaged with the insurers, I don’t know.”
He said Congress should have provided money for the vaccination effort back in June.
“There are a lot of good people working very very hard,” Toner said, “but things are in flux.”
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.