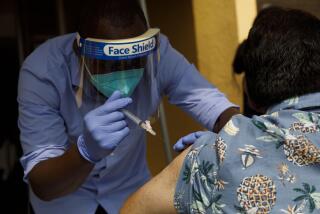
Vaccination rates rise in nursing homes, but when will families be able to visit?

- Share via
Melissa Traub hasn’t hugged her 92-year-old mom since March. Like countless others locked out of a family member’s nursing home because of COVID-19, she has spent nearly a year listening helplessly on the phone as her aging mom struggles to comprehend her isolation.
“I have to hear her crying when she’s having an anxiety attack, asking, ‘Why can’t I just come live with you?’” Traub said. “She’s incontinent. She’s in a diaper. I would have to move to a bigger place and hire live-in help.”
But Traub’s mom is now fully vaccinated, as are most of the residents in her Reseda nursing home. Traub has had her first injection, and her second is scheduled in the coming days. So why can’t she go give her mom a hug?
Because regulators haven’t yet loosened strict rules that impede most visitation.
As vaccination rates climb rapidly in U.S. nursing homes and the number of new coronavirus infections plummets, doctors, residents and family members have begun pushing to ease the crushing isolation that descended on the facilities last spring. But it’s not as simple as just opening the doors and hoping for the best.
What about the residents and staffers who refuse to get the shots? Can you segregate nursing homes based on vaccination status, creating two very distinct classes within the same building — one allowed to hug their grandkids, eat together and play bingo, the other left alone and isolated indefinitely?
Complicating the equation is the fact that many of the residents and staffers hesitating to take the vaccine are people of color, many of whom are less likely to trust the assurances of a healthcare system that has not historically worked for their benefit.
As regulators begin to grapple with the science and ethics of reopening, despondent residents and their families are left waiting.
“It just sucks,” Traub said. “Hopefully, it’ll all be over soon and she’ll be alive when it is. But there’s always the horrible possibility that she won’t make it that long, we won’t ever see her again.”
When COVID-19 began its deadly march through nursing homes last spring — it has killed more than 160,000 residents and staff members nationwide so far — the only way for the beleaguered facilities to fight the disease was to lock down, cutting off their fragile inhabitants from families and friends. But those early days stretched into weeks, and the weeks into months. In March, it will have been a full year.
And though the coronavirus is a swift and obvious killer, the crushing isolation created by the lockdowns has taken a more subtle, but still devastating, toll. Depression, always a concern in nursing homes, is on the rise, according to caregivers. Many residents have lost weight because they’ve simply stopped eating. “Failure to thrive” — a term more commonly associated with undernourished infants — is increasingly applied to elderly residents in long-term care facilities, say doctors who work in them.
That’s why, as more and more homes complete their two-dose vaccination regimens, geriatricians and advocates for the elderly are pushing to reopen to visitors as soon as possible. “More nursing home residents have been vaccinated than the rest of the community,” said Molly Davies, who serves as an ombudsman for long-term care residents and their families in Los Angeles County. “At some point, a nursing home is going to be the place to be.”
But it’s not easy or automatic to take that step. Though the vaccine appears to do an excellent job preventing serious illness and death, it’s still unclear whether a vaccinated person can become infected and transmit the virus to others. And despite the carnage wrought by COVID-19 in nursing homes, there are still plenty of people in them who are reluctant to get the injections.

“I think the government’s nervous about making decisions at the federal level and that filters down to the state level, but the residents, the families and the caregivers have had enough,” said Dr. Michael Wasserman, past president of the California Assn. of Long Term Care Medicine, which represents doctors, nurses and others working in long-term care facilities.
In the early days of the pandemic, when family members begged to be allowed to visit, nursing homes had to turn them away because their individual rights were far outweighed by the risk to everyone else in the facility. “Now, we’re quickly approaching a point where, if you’re not vaccinated in a nursing home, the primary risk is to yourself,” Wasserman said.
The California Department of Public Health is “in the process of evaluating potential adjustments to visitation policies in nursing homes while also remaining focused on ensuring all nursing home staff and residents have the opportunity to be fully vaccinated against COVID-19,” spokeswoman Kate Folmar wrote in an email to The Times.
This month, the U.S. Centers for Disease Control and Prevention reported that 78% of residents who have been offered a vaccine took it, but only 38% of staff members did.
Current state guidelines allow visitors in residents’ rooms where community spread is low, but so far only a handful of rural California counties qualify. State officials say several more could reach the threshold next week. In dire circumstances, such as imminent death, family members have also been allowed “compassionate care” visits in full mask and gowns.
Outdoor visits — with no touching, mandatory masks and six feet of separation required at all times — have been permitted statewide since the summer. But many homes have limited space and staff to supervise such visits, making them hard to schedule at the best of times and subject to cancellation when a facility experiences an outbreak, according to family members.
And they’re no substitute for normal visits.

The last time Melody Taylor Stark held her 84-year old husband, Bill, was March 13, just before the lockdowns. They kept in touch the best they could electronically, but the technology was unfamiliar and glitchy. Bill missed two telemedicine appointments with doctors outside his nursing home because the iPad used for such visits was locked and the employee who knew the password wasn’t at work, Stark said.
When state health officials began allowing limited outdoor visitation, she thought for sure she’d get to see him soon. Instead, she got a “constant flow of pushback” from the administrators of the Arcadia home, who seemed nervous about opening up without explicit permission from the corporate owners of the facility and the county health department.
Eventually they got a few outdoor visits, but she knew things were bad when her previously upbeat, optimistic husband “started crying and saying this is no way to live.”
He died in November. She never got to hold him again.
Nancy Klein’s 53-year-old son has been in long-term care facilities for five years, since a massive brain hemorrhage left him unable to move, talk or feed himself. Phone calls and FaceTime, the lifelines for so many during the pandemic, are not options for him.
Though there have been some kind employees at the string of Los Angeles and Riverside County facilities he has lived in — she didn’t want to name the current one for fear of upsetting administrators and making visitation even harder — not everybody is as caring as she would be. Her son is big and hard to move, so she worries nursing assistants will “bounce his head off the headboard” while trying to change him.
The nurses also test the water temperature with gloved hands before they bathe him, instead of with the soft spot in the crook of an elbow, as she does. “They don’t know if it’s too hot…. It’s just like washing a car to them,” Klein said.
Klein, 79, has had her first injection and expects the second shot in early March. Her son still has antibodies from a recent bout with COVID-19, but she will allow him to be vaccinated as soon as possible.
Before the pandemic, Klein said, she was with her son almost seven hours a day. She said it’s awful to imagine what goes through his mind now without her there. “He must really think I deserted him,” Klein said.
Still, not everybody is sure it’s safe to open to visitors yet.
Dr. Swati Gaur is a geriatrician for two nursing homes in rural Georgia, north of Atlanta. Although some data suggest that vaccination also reduces a person’s ability to catch and transmit the virus, “I can’t take that to the bank,” Gaur said.
“I have seen what it looks like when the facility goes down,” Gaur said, describing the grief and chaos of an outbreak. “I don’t know if I’m prepared to relive that. I don’t know that’s a loss anyone has an appetite for.”
Instead, she said, she plans to introduce communal dining slowly, with about 12 residents at a time in a room designed to seat 50. That way, if there’s an outbreak, it can be limited.
“If the first thing that I do is allow visitation, then we are talking about an unvaccinated person walking the halls, touching patients,” Gaur said. “We create a potential network for disease transmission.”
Complicating matters is how few people in her conservative, Republican region are willing to wear masks, let alone get vaccinated, Gaur said.
“I think people take it as a sign of disloyalty to our previous president if they wear a mask,” Gaur said. “That might be why I am so reluctant about bringing families into the nursing home.”
Another strategy proposed for dealing with residents and staffers who decline vaccinations is to isolate them in a separate part of the building — de facto segregation.
But many of the residents and staff members hesitating to take the vaccine are people of color, creating the disturbing prospect of homes segregated along racial lines.
“One of my residents who refused is an African American man in his 70s, who simply ‘doesn’t believe in it,’” an Indiana geriatrician wrote in response to a California Assn. of Long Term Care Medicine survey of healthcare professionals on reopening.
The resident, who recently endured a second below-the-knee amputation due to diabetes, is mentally competent and capable of understanding the issues and making his own choices, the doctor wrote. Staffers talked to him and his family, but they have not been able to change his mind.
“Is he seriously not going be allowed to play bingo?” the doctor asked her colleagues.
In an interview, the doctor, who asked not to be identified to protect her patients’ privacy, agreed that the primary risk for residents who refused to get vaccinated is to themselves. She’s not planning to segregate them because of their decision.
“Any notion that you are going to have a handful of people kept away from the rest of population, not allowed to dine, not allowed to socialize, not allowed to visit, is not OK,” the doctor said.
Pam Dransfeldt said nursing homes should require people who don’t want the vaccine to sign a waiver and let everyone else get back to their normal lives.
Dransfeldt hadn’t seen her 90-year-old father, Jack Spencer, since his Camarillo nursing home had an outbreak in November and stopped allowing outdoor visits. They could still communicate by phone, but it wasn’t easy. “I have definitely seen a decrease in his memory with all the isolation. Also, he’s a loner. And when a loner is desperate for company, you know it’s bad,” Dransfeldt said.
Spencer had his first vaccine injection and is expected to receive his second next week.
Like many California nursing homes, Spencer’s allowed infrequent outdoor visits before the dizzying surge in cases in November, but they were a poor substitute, Dransfeldt said. They couldn’t touch and the masks muffled their voices, which made it particularly hard for him to hear. “You’re kind of yelling across this table,” Dransfeldt said.
On top of that, her dad has hay fever, which gives him a runny nose, so he’d take his mask off and use it as a tissue. “I was always saying, ‘Dad, you can’t do that, we’ll get in trouble!’”
The staff did tolerate her bringing a small dog that would sneak across the table to get cuddled by her father.
She saw him for the first time in months on Sunday. It was another outdoor visit. In a Facebook post she wrote: “Dad came out and went right for the sun. I asked where he was going and he said, ‘I haven’t seen this for a while.’ He took in the sun and the birds singing.”
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.