‘Long haul’ COVID-19 sufferers take a page from AIDS/HIV activism to be heard

- Share via
Early in the pandemic, Fiona Lowenstein knew that the full story of COVID-19 was not being told.
She was 26 and healthy, and after testing positive for the virus last spring, she expected an easy recovery. But after a two-night stay in the hospital, she came home to experience severe fatigue and an upset stomach. She had a difficult time focusing her thoughts, and she was scared.
For the record:
3:18 p.m. April 26, 2021An earlier version of this article identified Jennifer Brier as a professor at the University of Illinois. Brier is a professor at the University of Illinois Chicago.
No one had said anything about these symptoms, and after posting on Instagram, she learned she wasn’t alone. As co-founder of a queer and feminist collective in New York exploring issues of health and social justice, she suddenly saw purpose in forming a new community.
Today, the Body Politic COVID-19 Support Group has registered 10,500 COVID-19 patients and their caregivers and families, who have started an independent research group and advised the National Institutes of Health. It is among dozens of grass-roots organizations around the world that have formed to make sure that a year into the pandemic — as fatigue mounts, vaccines become more available and infection rates drop — COVID-19 and its lingering symptoms remain in the public eye. Mindful of the battles that HIV/AIDS activists have fought over the years, its members know that their greatest enemies are fear, ignorance and apathy.
Mobilizing around the syndrome known as ”long COVID,” members have organized administrative teams and executive boards and enlisted the support of physicians. They write grant applications and mount GoFundMe campaigns, and they worry that long COVID will spark an invisible and untreated epidemic.
“The pandemic has shaken our infrastructure and belief systems,” Lowenstein said. “Cracks in the healthcare system and the disability system have emerged. It is clear that the system is not able to meet the demands of COVID patients in general and long COVID.”
If projections are accurate, their concerns are well-founded. More than 32 million cases of COVID-19 have been reported in the United States, and according to one study, long COVID can affect up to a third of those who have had the disease.
Because the full course of COVID-19 is poorly understood, the National Institutes of Health announced in February a $1.15-billion initiative to study its long-term effects.
Activists and advocates believe there is little time to waste.
One-third of COVID-19 survivors were diagnosed with a psychiatric or neurological condition within six months of being infected with the coronavirus.
Post-viral diseases like long COVID must be treated immediately, said Emily Taylor of the Long COVID Alliance. Otherwise, they can lead to chronic symptoms.
“We see a two-year window,” Taylor said, “and if we don’t get things done, many, many people will be disabled for many years to come, possibly for the rest of their lives.”
::
Angela Meriquez Vázquez, 33, has lived with long COVID for 13 months. She sees six doctors, takes up to 25 pills a day and tries not to be overwhelmed managing her health and her jobs as a policy director for a children’s advocacy group and on the state redistricting commission.
Working out of her home in Mount Washington with her husband, two cats and a Dalmatian, she remembers her early symptoms — the migraines, turning stomach, sleeplessness — and feels the sting of the doctors who dismissed her concerns.

She had gone to the emergency room in May with chest pains and heart palpitations, and the hospital staff quizzed her: Did she have a cough? Not really. Had she been tested for the coronavirus? Yes. And the results? Negative.
She tried to explain the unreliability of the tests, but doctors, after their assessment, believed she was having a panic attack. She fought back her tears and went home, feeling stereotyped as “hysterical Latinx woman.” She grew depressed, even suicidal, as her long COVID symptoms progressed.
The Body Politic support group was the only place where she felt heard. She began posting reports she’d found on the internet, and Lowenstein invited her to moderate discussions. Today, Vázquez is the organization’s vice president.
Helping others with long COVID and gaining a better understanding of this disease, she believes, started her recovery.
“To talk about what is it like to be in this body with long COVID — to be able to name and label these symptoms with a diagnosis — is part of the transformation from being a person at the mercy of a virus to someone with information that they can use to understand, cope and even heal,” she said.
She is grateful to have doctors today who understand her condition and is critical of earlier medical teams for a “lack of compassionate curiosity” that left her feeling powerless in the face of an illness that was slowly changing her life. She wants to make sure no one else experiences the same “gaslighting.”
::
Like Lowenstein and Vázquez, Diana Berrent became sick early in the pandemic. Hers was an average case, best treated by “Tylenol, Gatorade, thoughts and prayers.” Once the initial infection had passed, she continued to experience relapsing symptoms.
After sharing her experience in the New York Post (“Coronavirus Diary Day 1: Long Island mom describes symptoms, testing struggles”), she became an advocate for treating COVID-19 patients with plasma drawn from survivors whose blood is rich with virus-fighting antibodies.
Berrent, 46, founded Survivor Corps to give individuals an opportunity to donate convalescent plasma and enroll in COVID-19 studies. The group claims nearly 160,000 members and is partially funded by a $440,000 grant from the Gates Foundation.
Working to eliminate the “dissonance” between science and policy, Berrent describes Survivor Corps as “an army,” partnering with the medical and scientific communities to close the gap between “what is happening in people’s lives and what is happening in the laboratories.”
Their work has included a poll of its members to find out if their long COVID symptoms improved following vaccination. About 40% of the 577 patients said yes, which helped prompt an immunologist at Yale School of Medicine to begin studying the phenomenon.
Similarly, Patient-Led Research, the independent research group started by members of Body Politic, published a report characterizing the symptoms of long COVID among nearly 3,800 members. Their findings, released late last year, helped establish an early understanding of the disease.
While little is known about long COVID, researchers believe it is related to similar and equally puzzling syndromes — such as mast cell activation syndrome and dysautonomia — that occur following a severe viral infection. Symptoms arise from the body’s inability to regulate metabolism.
Because public awareness and federal research of these syndromes is small, advocacy groups have played a role in raising their profile. They are now finding common cause with long COVID.
The Long COVID Alliance, for instance, was co-founded by the organization Solve M.E., which for 30 years has lobbied for research and funding into chronic fatigue syndrome, which can follow a COVID-19 infection.
As more organizations focus on long COVID, a common agenda has emerged: clinical education, so healthcare providers are informed of symptoms; an expansion of disability benefits, so those with the disease can be supported in their recovery; and a revision of the disease classification code, so insurers can reimburse physicians and patients for treatment.

Activists argue that healthcare equity must be addressed.
“Vaccines ... will not make us healthy. They will keep us from getting sick. But we can’t understand the effects of long COVID and then think we can develop a vaccine for that. Health and well-being are more than the absence of disease,” said Jennifer Brier, a professor at the University of Illinois Chicago who has written extensively about the early years of the AIDS crisis.
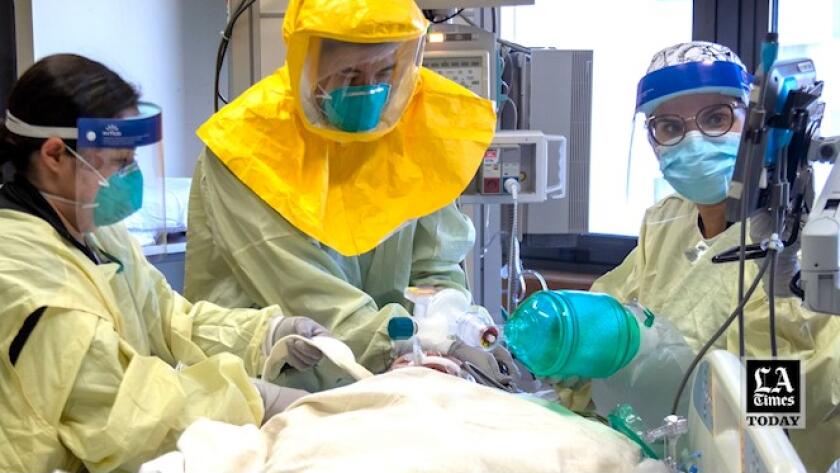
Researchers are getting serious about understanding a disease patients call “long COVID.” Its symptoms include aches, fatigue, sleep problems and brain fog.
The AIDS epidemic provides a useful perspective, said Pato Hebert, an HIV/AIDS activist since the 1990s. An understanding of the disease as a public health crisis came after years of fighting against stigma, racism and misinformation.
That awareness, argues Hebert, who has long COVID and is a member of Body Politic, owes itself to the work of those who were sick and vulnerable.
“In order for public health to work, it has to be community work,” he said. “We have to understand what people’s lived experience is and what that requires in terms of access, fear, precarity with work, shelter, food.”
Dr. Michael Joyner with the Mayo Clinic, a member of Survivor Corps’ medical advisory board, is encouraged by the urgency that activists have brought to long COVID.
“In the midst of pandemic, you are concerned that you will get to a point of socially learned helplessness, that there’s nothing that can be done. ... But that isn’t the case,” Joyner said. “We can try to understand what is going on. We can support people and families. We can and we will. It is like a barn raising.”
- Share via
Watch L.A. Times Today at 7 p.m. on Spectrum News 1 on Channel 1 or live stream on the Spectrum News App. Palos Verdes Peninsula and Orange County viewers can watch on Cox Systems on channel 99.
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.