Questions arise over video of San Diego deputy’s contact with fentanyl
- Share via
Handout-San Diego County Sheriff’s Department.
- Share via
A public service video from the San Diego County Sheriff’s Department about the dangers of fentanyl — with footage of a deputy allegedly overdosing after brief exposure — has sparked a backlash and allegations that the anti-drug effort could harm the very people it’s meant to help: law enforcement officers and drug users.
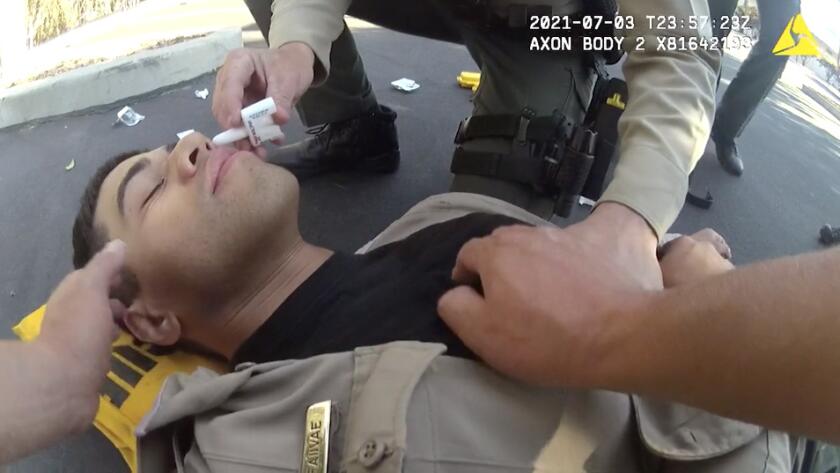
The body-worn camera video is stark and dramatic. A young sheriff’s deputy opens the back of a suspect‘s car, sees a white powder he thinks is fentanyl and then collapses to the pavement. His field training officer rips open a package of naloxone, the antidote to the deadly drug, and vows: “I’m not going to let you die.”
For the record:
2:16 p.m. Aug. 10, 2021This story misstates what was known about the medical condition of the deputy shown in the Sheriff Department’s video. The conclusion that his collapse was caused by contact with fentanyl was supplied by the Sheriff’s Department rather than by qualified medical experts, who have since cautioned that the risks from incidental contact are often overstated. A follow-up story can be found here.
The video ends with Sheriff Bill Gore warning that “being exposed to just a few small grains of fentanyl could have deadly consequences.”
There’s just one problem. The risks of so-called passive exposure to synthetic opioids such as fentanyl are overblown, according to interviews with medical experts and scientific studies. Such inaccurate messaging is instilling unnecessary fear in first responders, they said, and could cause them to be reluctant to treat people who have overdosed.
“This is a big deal,” Dr. Lewis Nelson, chairman of the Department of Emergency Medicine at Rutgers New Jersey Medical School, said Sunday. “I’m concerned that the officers themselves are being psychologically harmed. There is more of a PTSD-like fear of this drug when, in reality, it’s not warranted. There is no risk of poisoning from such an exposure. And I fear people won’t rescue those who have overdosed because of the fear of being exposed.”
The San Diego Sheriff’s Department did not respond to requests for comment Sunday.
A study published in the International Journal of Drug Policy in June found that law enforcement agents across the country “wrongly believed that dermal exposure to fentanyl was deadly and expressed fear about such exposure on scene. Officers had a lack of education about fentanyl exposure and faulty or dubious sources of information about it.”
Most had heard stories either in the news, on social media or by word of mouth about first responders who had overdosed from touching the drug, the study said, but the symptoms allegedly endured in those episodes were more akin to panic attacks than to fentanyl poisoning.
Two prominent medical associations released a joint position statement in the journal Clinical Toxicology in 2017 about preventing fentanyl exposure in emergency responders. It began with a caveat.
Although fentanyl and other drugs designed to mimic its effects have fueled an overdose epidemic in North America, “the risk of clinically significant exposure to emergency responders is extremely low,” according to the statement by the American Academy of Clinical Toxicology and the American College of Medical Toxicology.
“To date, we have not seen reports of emergency responders developing signs or symptoms consistent with opioid toxicity from incidental contact with opioids,” the groups wrote.
That is not the sense any viewer would get from watching the San Diego sheriff’s video, which was released Thursday. The somber four-minute public service announcement intersperses body-camera footage from a July 3 incident with interviews with Gore, Deputy David Faiivae and his training officer, Cpl. Scott Crane, to drive home the message about how deadly fentanyl is.
In one scene, Faiivae is looking into the back of a red SUV. Crane’s voice rings out, as he addresses the trainee: “It tested positive for fentanyl. That stuff’s no joke. It’s super dangerous.” Then Faiivae falls like a dead weight, stiff arms flapping as he hits the pavement.
Then Crane picks up the narrative. “I ran over to him. He was OD‘ing. I went to my trunk, got out the Narcan,” Crane said, using the brand name for naloxone. “I did one nasal spray in one nostril. ... Another nasal spray in the other one.”
What follows is a welter of dramatic scenes with grave pronouncements threaded throughout:
Crane: “It’s an invisible killer. He would have died in that parking lot if he was alone.”
Faiivae: “I almost died of a fentanyl overdose.”
Gore: “The dangers of fentanyl are real, and this drug is killing our communities.”
According to the body-camera footage, which was edited by the department, Faiivae was rushed to the hospital. Sheriff’s officials have not released medical records detailing his condition, nor have they said whether he was exposed to fentanyl by touching or inhaling it or even if fentanyl was found in his system.
The dangers Gore notes are real, just not in the way the video portrays them.
“The biological plausibility that it’s an overdose by touching is nil,” said Dr. Jeremy Samuel Faust, who has written about what he calls “opioid hysteria” in the New York Times and Slate magazine. Faust is an emergency physician at Brigham and Women’s Hospital in Boston and an instructor at Harvard Medical School.
As for briefly inhaling fentanyl in the air, “You have to really go for it.”
“People with opioid-use disorders don’t inject opioids because they want to,” he said in an interview Sunday. “It’s the only way they can get the effects they’re looking for. Otherwise they’d just touch it. ... I have never once seen a toxicology report from any of these [first responder] cases that showed that the ‘victim’ had actual fentanyl in their system.”
The San Diego video, Faust said, is “not diagnostic of anything. It shows that someone had an altered level of consciousness and got better but not why.”
Caleb Banta-Green, principal research scientist at the University of Washington Addictions, Drug & Alcohol Institute, said the fears over fentanyl poisoning from brief exposure remind him of how patients with HIV were treated in the early days of that pandemic.
“Medical providers were unwilling to care for or go into the room of people with HIV,” Banta-Green said. “Law enforcement has very difficult jobs to do ... but this spontaneous overdose response has never been documented. It’s been glorified.”
More to Read
Updates
4:36 p.m. Sept. 9, 2021: The headline on this story has been updated.
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.