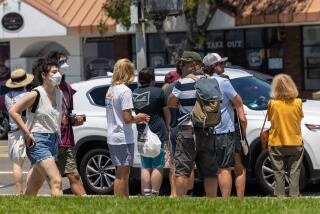Proportion of Omicron BA.2 cases rising rapidly. Is a surge coming or just a ripple?
- Share via
The proportion of coronavirus cases of the ascendant Omicron subvariant BA.2 is rising across the U.S. and along the West Coast, new federal forecasts show.
For now, weekly coronavirus cases remain flat nationally and in California, and are still declining in Los Angeles County.
But the data could be a prelude to an increase in coronavirus cases nationally for the first time since early January, when an earlier Omicron variant swept the nation, resulting in record high numbers of simultaneously infected people and putting many hospitals under strain.
It’s hard to know for certain what BA.2’s growth will mean for the nation. It’s possible BA.2 could develop into a full-blown surge and strain hospitals, especially in areas with poor vaccination and booster rates. But BA.2 could also plausibly just result in simply a slower decline in cases, with communities better protected since the winter Omicron wave infected so many people and left them with an extra boost to their immunity, at least for the short term.
Nationally, BA.2 comprised an estimated 35% of analyzed coronavirus samples between March 13 to March 19; the previous week, it made up 22%, according to data published Tuesday by the U.S. Centers for Disease Control and Prevention.
In the Southwestern U.S. — which includes California, Arizona, Nevada and Hawaii — BA.2 made up an estimated 41% of coronavirus samples; the previous week, it was 28%.
And for the first time, BA.2 is now believed to become the dominant subvariant in the Northeast, comprising more than half of analyzed coronavirus cases in New York, New Jersey and New England.
There are hints that weekly coronavirus cases have stopped falling in New York. For the week that ended Monday, New York State was recording 82 cases a week for every 100,000 residents, up from a rate of 58 the prior week, according to Johns Hopkins University.
Still, coronavirus cases in much of the nation are still either flat or declining. Nationwide, the U.S. has been averaging about 28,000 new coronavirus cases a day, a figure that has remained flat for the last few days. California has been logging between 3,000 to 4,000 cases a day, or roughly between 60 to 70 cases a week for every 100,000 residents.
L.A. County has seen its overall weekly coronavirus case numbers continue declining, at least when subtracting out a backlog of cases from earlier in the Omicron surge.
By Tuesday afternoon, L.A. County hit its health officials’ long-awaited goal — fewer than 730 cases a day over the last week, or roughly 50 cases a week for every 100,000 residents, according to a Times analysis of county data, indicating a moderate level of transmission. (Hitting that goal comes exactly in the time range forecast by L.A. County Public Health Director Barbara Ferrer, who said in February that she suspected the county would hit this goalpost of fewer than 730 cases a day by mid-to-late March.)
It can be hard to predict exactly what path the pandemic will take. There have been plenty of times when many have been eager to declare the end of the pandemic, only to be stunned at the emergence of the Delta variant last summer, and the original version of the Omicron variant over Thanksgiving and into New Year’s.
But there are also times in which signs pointing to a rise in cases end up fizzling out. That happened almost exactly one year ago, when Dr. Rochelle Walensky, the director of the U.S. Centers for Disease Control and Prevention, on March 29, 2021, said she had a feeling of “impending doom” amid an increase in coronavirus cases so soon after the winter surge faded.
In the end, though, what she was worried about was essentially a relatively brief interruption in a long-term reduction in new weekly coronavirus cases, and the pandemic continued to decrease for the rest of that spring until the Delta variant emerged in the summer.
Experts say it’s prudent to be prepared for a possible increase in coronavirus transmission by getting up-to-date of vaccinations and boosters; adhering to California health officials’ strong recommendation to continue wearing masks in indoor public settings; and being prepared to get tested before and after gatherings.
There are some potentially worrisome signs out of Europe. Austria is reporting a record number of new case — more than 3,500 weekly cases for every 100,000 residents — and the government has decided to implement stricter pandemic orders governing indoor public spaces.
Britain is recording a rapid rise in new daily cases, with a rate of 1,200 cases a week for every 100,000 residents, more than triple the rate from late February. And the number of coronavirus-positive hospital patients is on the rise, increasing by more than 20% over the last week.
“A number of U.S. public health authorities are forecasting a smaller BA.2 wave than the original Omicron wave. What if they’re wrong and it turns out to be a bigger wave?” tweeted Myoung Cha, chief strategy officer for San Francisco-based Carbon Health. Cha still expressed hope the U.S. could avoid a BA.2 surge in cases, like South Africa, “but hope isn’t a strategy. My advice: mask up, get boosted and prepare.”
But there are also a number of countries in Europe and elsewhere that offer hope for the U.S. and California to avoid a severe surge.
For instance, Britain — despite rising cases and hospitalizations — has still not seen a jump in coronavirus-related intensive care unit demand, Dr. Anthony Fauci, the president’s chief medical advisor, told reporters in broadcast interviews recently.
In Britain, “despite the fact that there are cases going up, there does not appear to be any increase in the degree of severity of the outbreak,” Fauci said on a Washington Post Live broadcast Tuesday. “So hopefully, when we do … see an uptick, hopefully it won’t be accompanied by an increase in hospitalizations. But it just remains to be seen.”
But it’s also possible that more severe illness could end up being reported in Britain as more data comes in. Dr. Eric Topol, director of the Scripps Research Translational Institute in La Jolla, on Twitter Wednesday cited data showing a 10% week-over-week increase in patients needing mechanical ventilation to help them breathe, and a 14% increase in COVID-19 deaths.
Another bright spot in Europe so far is Spain. That nation’s winter peak, on a per capita basis, mirrored California’s, and the case rate in both places is still declining or has flattened.
“It’s not all as bad as you think,” said Dr. George Rutherford, a UC San Francisco epidemiologist, who is optimistic that BA.2 will spare California from a difficult surge.
Dr. Robert Kim-Farley, epidemiologist and infectious diseases expert at the UCLA Fielding School of Public Health, said he expects to see either coronavirus cases flatten or a modest increase in cases, but nothing close to resembling the most recent Omicron winter surge.
Kim-Farley said he suspected that California won’t get hit hard by BA.2 simply because so many people now have a reasonable degree of immunity, either through vaccination or having survived an infection of the subvariants that were dominant earlier, BA.1 or its descendant, BA.1.1. All that, “I feel, will blunt the effect of the increasing percentage of BA.2.”
Kim-Farley said he also expected weekly COVID-19 hospitalizations and deaths to continue falling, as more anti-COVID drugs become more plentiful, such as Paxlovid.
What he would be more concerned about is a new variant that was even more transmissible and able to overcome the immunity provided by either vaccination or prior infection.
“That is always the wild card that could potentially lead to a significant problem,” Kim-Farley said.
It’s still important that people who have had prior infection get vaccinated and boosted because the strength and duration of natural immunity appears to be less than through vaccinations, including the booster doses, as appropriate, Kim-Farley said.
Topol on Tuesday expressed surprise that the U.S. hasn’t seen an overall increase in coronavirus cases so far, even though the BA.2 wave in Europe is now starting to turn around three weeks into it.
“It’s surprising, not easily explained, but gratifying to see — and hope it holds up,” Topol tweeted.
Orange County’s coronavirus case rates are particularly low at the moment. According to data released Tuesday by Orange County health officer Dr. Regina Chinsio-Kwong, Orange County is reporting about 26 cases a week for every 100,000 residents, and is reporting a high vaccination rate for its seniors, with more than 95% of seniors having received at least one dose.
The high rate of vaccination among seniors is essential to preventing a surge in deaths. Dr. Clayton Chau, director of the Orange County Health Care Agency, said he recently spoke to his uncle who lives in Hong Kong, which is experiencing a staggering rate of COVID-19 deaths exacerbated by low vaccination rates among seniors.
The numbers of deaths are so high in Hong Kong that funeral homes and hospitals aren’t able to store bodies, Chau said. That’s an echo of the kind of scenario Southern California faced during its first winter surge, before vaccines were widely available.
Chinsio-Kwong, however, urged residents not to get too complacent about official reports of low case numbers, noting that many people are now testing with at-home kits, whose results are not shared with the government.
“Even though we may not have a mask mandate in our county, it is still very important for everyone to continue to use precaution,” said Chinsio-Kwong; health officials across California are still strongly recommending universal wearing of masks in indoor public settings.
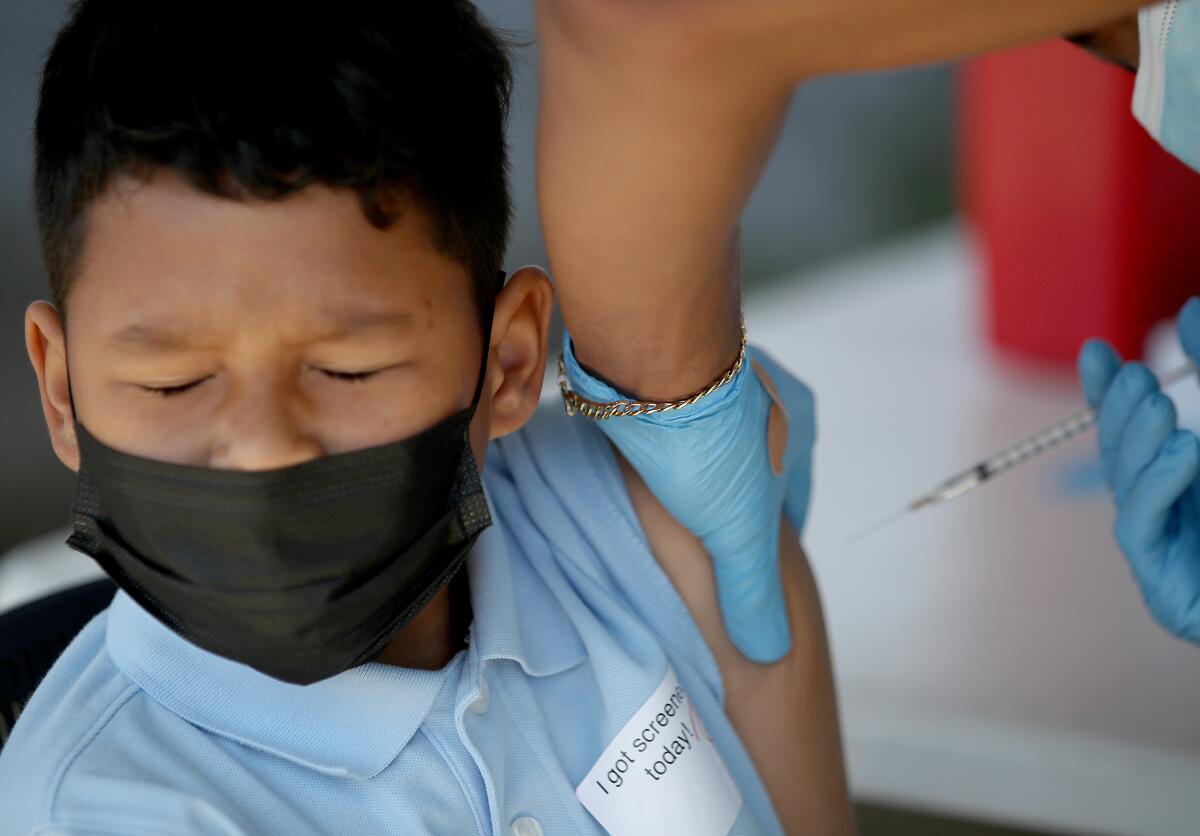
And that includes getting a booster shot if you’re overdue for one, Chinsio-Kwong added. Recipients of the Pfizer-BioNTech shot age 12 and up, and all recipients of the Moderna shot, are eligible for a booster shot five months after completing the primary two-dose COVID-19 vaccination series.
Those who got the Johnson & Johnson single-dose vaccination can get a booster two months later.
“The most protected are those who are fully vaccinated and boosted. So get your booster shot,” Chinsio-Kwong said.
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.