Wastewater testing, vital in COVID-19 tracking, could help identify monkeypox spread

- Share via
As wastewater testing continues to prove useful in estimating the spread of the coronavirus, scientists again are using sewage to track the latest public health emergency: monkeypox.
In late June — about a month after the first California case was confirmed — monkeypox DNA was detected in wastewater in San Francisco, according to the WastewaterSCAN coalition, a group of scientists who have been testing sewage for the coronavirus since 2020.
The group recently confirmed the presence of the monkeypox virus in Los Angeles County waste.
“It helps understand how widespread this is,” said Stanford civil and environmental engineering professor Alexandria Boehm, one of the lead researchers on the WastewaterSCAN team.
She said coronavirus sewage testing has been particularly useful during “the onset phase,” or soon after a new variant has been identified, but it’s unclear its extent. Public health officials can use the information to theorize how great the spread could become, and where.
“We’re sort of in that [phase] for monkeypox now,” Boehm said.
How monkeypox spreads, how to get a vaccine and more: Your frequently asked questions about monkeypox, and answers from experts.
Monkeypox DNA was first detected in Los Angeles County wastewater July 31, about 20 days after the WastewaterSCAN group expanded its monkeypox testing beyond the Bay Area to almost 40 other facilities nationwide — including in L.A. — according to data from the group.
Samples from L.A.’s Joint Water Pollution Plant in Carson, which serves about 4 million residents and businesses, showed a small presence of the monkeypox virus July 31 and for three days during the first week in August, according to WastewaterSCAN data. The virus has not since been detected there, despite rising monkeypox cases in Los Angeles County.
By comparison, monkeypox DNA has been detected almost every day since June 27 at two wastewater facilities in San Francisco — and at much higher levels than in L.A. County.
Still, Boehm said that doesn’t mean there’s not more monkeypox in Los Angeles County; it’s just been difficult to detect among the massive sample size.
Testing sewage for the coronavirus may tell scientists how much disease is in a community — and when the virus has finally gone away.
Because the L.A. wastewater facility serves such a large number of people “you have to think about the sensitivity of detecting monkeypox relative to the incident rate in the population,” Boehm said. “Just because you don’t detect monkeypox, doesn’t mean there’s nobody [in that waste watershed] with monkeypox.”
The two facilities in San Francisco serve a much smaller population, about 100,000 residents each, she said.
While both Los Angeles and San Francisco have seen a rapid rise in monkeypox cases in recent weeks, the totals are still only a fraction of each county’s population: about 600 in San Francisco among fewer than 1 million residents and roughly 1,000 in L.A. County among 10 million residents, according to each county’s public health departments.
L.A. County’s cases have more than doubled in the last two weeks, and the county reported its first monkeypox case in a jail and in a homeless shelter, health officer Dr. Muntu Davis said Thursday.
“We have more cases, but the case rate is actually higher in San Francisco,” said Barbara Ferrer, the director of L.A. County’s public health department, adding that she looks forward to continuing to analyze the sewage data.
“We do believe this is a useful strategy,” Ferrer said. “It will take some time to look and assess the correlations between the concentrations and the case counts. ... [But] we’re excited to be part of a larger group that’s figuring out how to best use the wastewater data.”
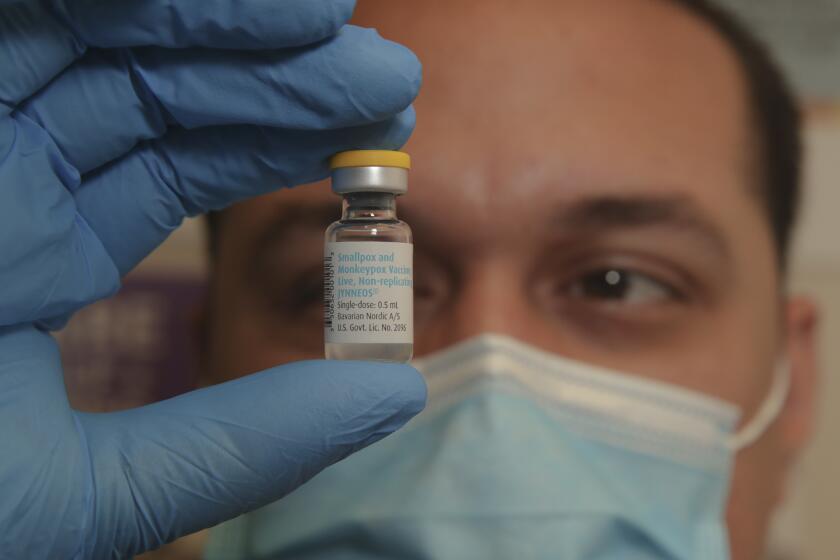
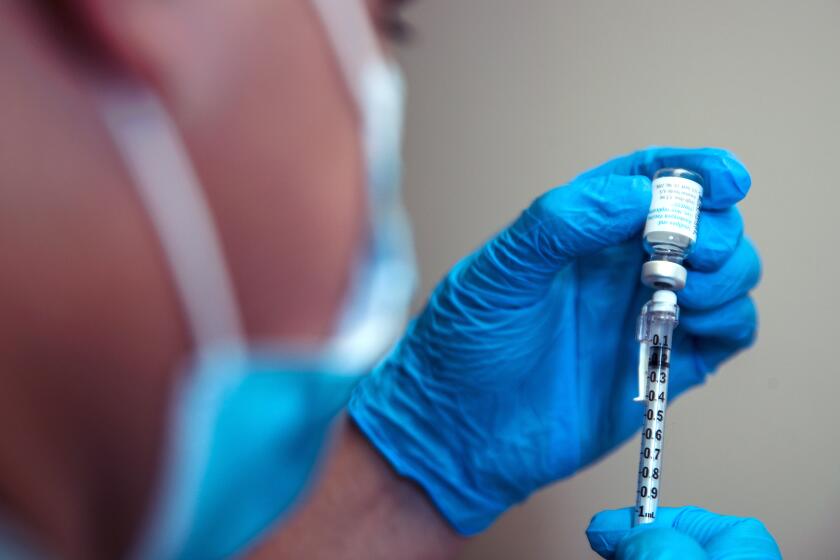
Hundreds of people received the monkeypox vaccine at St. John’s Community Health in Leimert Park. The federal government has allowed medical providers to give smaller does to stretch supplies.
It is not immediately clear whether the L.A. County health department plans to expand monkeypox testing in wastewater. The county has been monitoring wastewater for the coronavirus for months, including at the Joint Water Pollution Plant, as well as at the Hyperion Water Reclamation Plant in Playa Del Rey and facilities near Lancaster and Malibu.
When at-home COVID-19 testing began to limit the ability to monitor coronavirus case counts, L.A. County public health officials often used wastewater data to track transmission trends — one factor that played a role in Ferrer’s decision not to implement another indoor mask mandate last month.
“It’s helpful to have this additional lens into the epidemiology and dynamics of disease because it doesn’t rely on behaviors of people or testing,” Boehm said. “There’s kind of a health-equity component.”
She said wastewater data can also help inform public health decisions about where to target educational materials, clinics, treatment or other resources.
The scientists behind WastewaterSCAN call the data on viruses “invaluable,” having already found monkeypox in 22 California wastewater facilities, from San Diego to Sacramento, as well as at nine facilities in seven other states.
There’s not yet a national database to track monkeypox in waste, as the CDC established for COVID-19, but Boehm said she’d like to see the testing continue to expand. Her team also is working to test sewage for influenza A and respiratory syncytial virus (RSV), which she hopes can further help answer questions about viral transmission.
Gay and bisexual men, transgender people and others worried about monkeypox are strategizing to protect themselves as they wait for vaccinations.
She said she’d like to see the wastewater testing, which her team has found extremely accurate, to be used to inform care, treatment and even vaccine development of current viral outbreaks — as well as future ones.
“I’m a scientist, so I’m just curious how far we can take this,” Boehm said. “It’s turning out to be a really interesting and sort of amazing resource for understanding public health.”
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.