The amputation rate for diabetics in poor areas is high. This Boyle Heights clinic is trying to change that
- Share via
Maria Valdez didn’t have a lot of options. A wound on her foot that had become infected wasn’t healing because of her diabetes. She started using a wheelchair to get around. A year and a half ago, it seemed likely she was going to lose part of her leg.
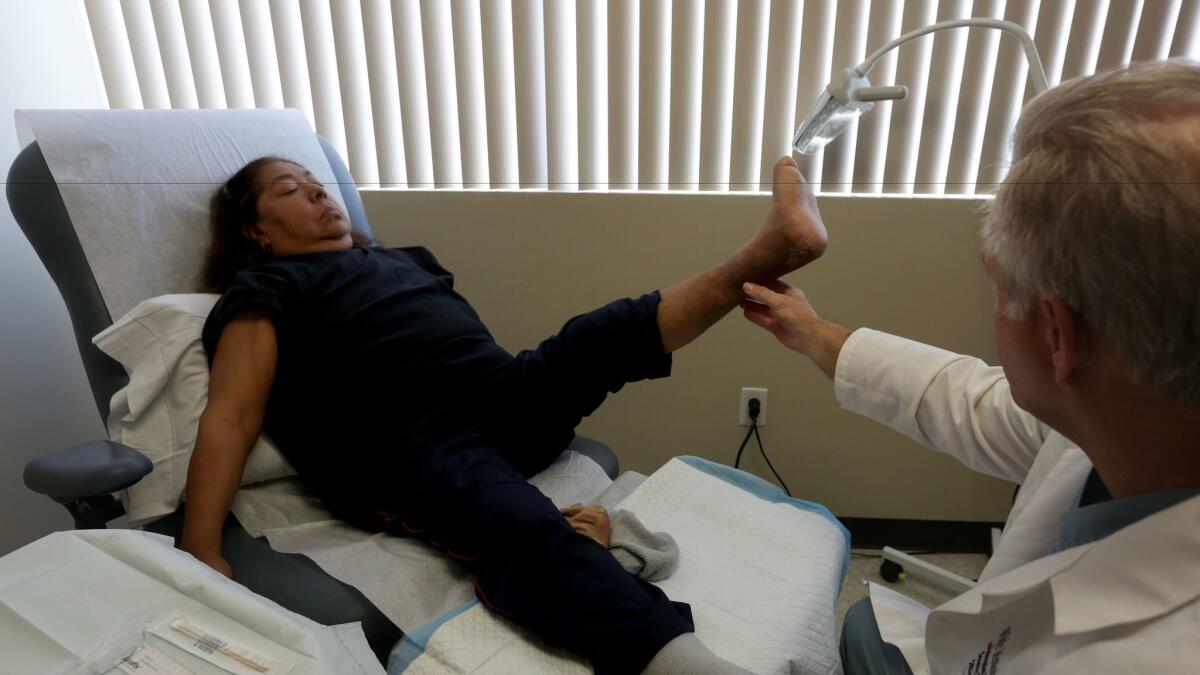
On a recent weekday, Valdez lay on a bed in a clinic in Boyle Heights. Her doctor, Stanley Mathis, pulled off her sock and lifted her foot toward the ceiling. The heel, which once was so decayed he could see the white of the bone, was now covered in smooth skin.
Valdez put her socks and shoes back on. She stood up and, though a little wobbly, walked down the hallway.
“I don’t like to lose, and I’m not used to losing,” especially when it comes to limbs, Mathis said.
Mathis, a podiatrist, runs a clinic at White Memorial Medical Center in Boyle Heights devoted to reducing amputations among diabetics — a tall order that requires treating wounds as well as helping people better manage the disease.
Diabetic amputations are preventable if problems are caught early enough. But poorer people tend to face more amputations; one study found that East L.A.’s amputation rate was eight times higher than in some of California’s richest neighborhoods.
“We continue to see people who’ve had diabetes for years and not received any treatment,” said Brian Johnston, an emergency medicine doctor who runs the clinic with Mathis. “We’re trying to change that.”
The clinic is one of many hospital initiatives that have cropped up across the country aiming to tackle health problems before they demand serious treatment — a philosophy promoted by the Affordable Care Act that is supposed to reduce the need for expensive medical care.
People with diabetes can lose sensation in their feet over time. They might not notice a small injury, for example, and the wound could stay open, eventually becoming infected.
“Sometimes you’ll find a nail they stepped on, a bottle cap that’s been there for two weeks — they can’t feel it,” Johnston said.
And because diabetics’ immune systems don’t always function properly, they also can struggle to clear infections, which then begin to spread dangerously. There are more than 7,000 leg or foot amputations each year among diabetics in California, according to the state health department.
A 2014 study published in the journal Health Affairs found that California neighborhoods with high amputation rates often also had a high concentration of low-income households, a trend the study’s authors called “deeply disturbing.” Amputation rates varied tenfold between the state’s richest and poorest neighborhoods, the study found.
White Memorial has invested $3 million in its Center for Limb Preservation & Advanced Wound Care to try to provide the kind of care and comfort typically reserved for richer patients. It starts in the waiting room: Mathis points out that they designed the check-in counter to be low so people in wheelchairs can easily pull up and sign in.
The clinic, which opened last year, is staffed by a team of medical providers that includes podiatrists, vascular surgeons, infectious disease doctors, cardiologists and neurologists. Together, they decide the best way to treat each patient.
Valdez, 59, had a pimple on her heel that became infected. Patients typically are referred to the clinic when doctors notice wounds aren’t healing at a normal pace. Valdez’s lesion had spread across the back of her foot, creating a bloody mixture of red and black — living and dead flesh. Many physicians said amputation was inevitable.
Mathis suggested medical maggots, which eat necrotic flesh. He inserted them into the wound for a few days and (though Valdez said they “creeped me out”), they cleaned up some of the sore. But her bone was still infected.
“This whole part of her heel bone was just mush,” Mathis said, pointing to her now-healed heel.
Instead of amputating, Mathis performed multiple surgeries on her foot, removing the infected bone and performing a skin graft. The clinic bought machines that allow doctors to see exactly where a foot is damaged so they can remove as little tissue as possible. Now Valdez’s foot is fully healed.
“Obviously she’s not going to be running a 5K,” but she’s mobile, Mathis said.
Heading off amputation is more than just saving a limb. Some studies have found that roughly three-fourths of people who lose a leg to diabetes will die within five years — a higher mortality rate than for many kinds of cancer.
That’s not necessarily because of amputation, but because the disease has progressed far enough to require such drastic measures, Johnston said.
In that way, wounds are merely an entry point to the clinic, he said. The overarching goal is to get patients’ diabetes under control and help them adopt healthy habits to manage it, he said. That’s why the clinic’s provider team also includes diabetes educators, nutritionists and endocrinologists.
“We recognize that we’re at the wrong end of this disease,” Johnston said. “We try to treat the wound and improve the underlying state of health for the patient.”
Hospitals haven’t historically had an incentive to keep people from getting sick or to improve their disease management. Quite the opposite: Physicians typically make money when patients need care because they bill to treat them.
But under changes put into motion by the Affordable Care Act, an increasing number of hospitals are paid a lump sum to provide all of a patient’s medical treatments for a year, instead of the typical fee-for-service model. So hospitals can save money when patients don’t need serious medical care, which is why they’re focusing on these sorts of preventative care initiatives, experts say.
Since the law took effect in 2014, hospitals have started offering free nutrition classes, starting community gardens and working with local grocery stores to promote healthy food. Martin Luther King Jr. Community Hospital in South Los Angeles opened a special center for patients with sickle cell anemia, a disease that primarily affects people of color. The goal is to make a hospital’s patients healthier by making the surrounding community healthier.
Republican plans to repeal Obamacare may not target the part of the law that changed how doctors are paid, experts say.
But even if that piece of the law were repealed, it’s not certain that hospitals would stop such projects, said John Romley, economist at the USC Schaeffer Center for Health Policy and Economics. Though it’s a little too early to know, some actually could be good investments that are saving hospitals money. Others might provide a competitive advantage over other hospitals and improve the facilities’ reputations, he said.
“Sometimes even if the boost was needed, it’s not needed forever,” Romley said. “Sometimes you’ve got to start pedaling the bike, and it becomes a lot easier.”
soumya.karlamangla@latimes.com
Twitter: @skarlamangla
ALSO
You know CPR. Now firefighters want you to treat shooting and bombing victims
Vaccination rate jumps in California after tougher inoculation law
The trees that make Southern California shady and green are dying. Fast.
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.














