Q&A: How California’s aid-in-dying law will work

Gov. Jerry Brown signed the End of Life Option Act into law in 2015.
- Share via
Starting June 9, terminally ill Californians can request prescriptions from physicians for medications that would end their lives. Here are questions and answers about the End of Life Option Act.
Who can get these prescriptions?
You must be a California resident, at least 18 years old and terminally ill with no more than six months to live.
Who can prescribe lethal medications?
All licensed medical doctors in California. A patient must be deemed terminally ill and mentally competent by two physicians to receive a prescription.
When was California’s law passed?
Gov. Jerry Brown signed the End of Life Option Act in October.
“In the end, I was left to reflect on what I would want in the face of my own death,” wrote Brown, a former Jesuit seminary student. “I do not know what I would do if I were dying in prolonged and excruciating pain. I am certain, however, that it would be a comfort to be able to consider the options afforded by this bill. And I wouldn’t deny that right to others.”
Do other states allow this practice?
Oregon became the first state to allow doctors to prescribe lethal medications starting in 1998. The practice has since become legal in Washington state, Vermont and Montana.
Is aid-in-dying the same as euthanasia?
No. Euthanasia means that the physician administers the medication or treatment that kills the patient. In aid-in-dying, the patient ingests the medicine on his or her own.
California’s law prohibits the practice from being referred to as euthanasia, mercy killing, assisted suicide or homicide.
Are doctors required to comply?
No, doctors are required to neither prescribe the medications nor refer patients to doctors who will write such a prescription.
How can I find a doctor that will write a prescription?
Other states don’t have databases of doctors who will prescribe these medications, and that will likely also be the case here. However, the organization that leads efforts nationwide to pass such laws, Compassion & Choices, runs a free hotline that might be able to help answer questions: (800) 893-4548.
What is the process for getting a prescription?
A patient must tell her doctor on two separate occasions, at least 15 days apart, that she wants the lethal medicines. She must also submit a written request to the doctor.
The doctor has to determine whether the patient is terminally ill with a life expectacy of no more than six months and that the patient has the mental capacity to make such a decision. The physician then must discuss details of aid-in-dying with the patient, as well as other treatment options, such as hospice care and pain control.
The physician then has to refer the patient to another doctor, who must separately confirm that the patient is terminally ill and of sound mental capacity to make such a decision.
Does a patient need to undergo psychiatric evaluation?
Not necessarily. According to the law, if a physician is concerned about a patient’s mental state, the doctor must refer the patient to a psychiatrist or psychologist. Both physicians who evaluate the patient must agree the patient is mentally competent.
In Oregon, 5% of those who have used the aid-in-dying law had been referred for a psychiatric evaluation, according to state data.
How many people in California are expected to take advantage of the law?
State officials expect that California “will mirror Oregon’s trend of very low utilization,” according to a state budget report.
In 2014, 155 Oregonians obtained prescriptions, or .00489% of the adult population, wrote a state analyst. He estimated that if the same percentage of Californians take advantage of the law in its first year, 1,476 would obtain prescriptions.
However, based on what happened in Oregon, that number could be much lower. In the first year that Oregon’s law was in effect, only 24 people requested prescriptions, though that number had climbed to 218 in 2015.
Plus, only some of the people who get the prescriptions actually take them. In Oregon, 64% of those who’ve ever received a prescription for the medicines died from ingesting them, according to state data.
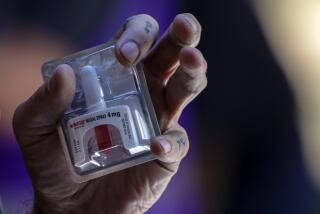
What is the medicine that is used?
The most common drug is secobarbital. It is usually prescribed with drugs that help suppress nausea or vomiting. Together, the medicines typically cost about $5,000.
Does insurance cover the cost of the medicine?
The law does not require insurance companies to cover this treatment. Administrators for private health plans are still figuring out how they’re going to implement the law, and people should contact their insurance company with questions, said Nicole Evans, spokeswoman for the California Assn. of Health Plans.
Medi-Cal, the state’s health plan for low-income Californians, will cover the treatment. The state has allocated $2.3 million for an estimated 443 people on Medi-Cal expected to request the medications in the upcoming fiscal year starting July 1.
However, both Medi-Cal and insurance companies are barred from informing patients that the treatments are covered. A controversy in Oregon in which the state’s Medicaid plan sent letters to terminally ill patients that both denied them an expensive cancer drug but notified them that aid-in-dying treatment would be covered was part of the reason why this line is included in California’s law.
Is the law permanent?
The law will expire in 2026 if the state Legislature doesn’t act to renew it.
Follow @skarlamangla on Twitter for more health news.
ALSO
Woody Allen says he’s done hiding behind comedy
Hyperloop One succeeds at first of many much-hyped tests
From coast to coast, middle-class communities are shrinking
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.