Addressing an epidemic of Rx deaths
- Share via
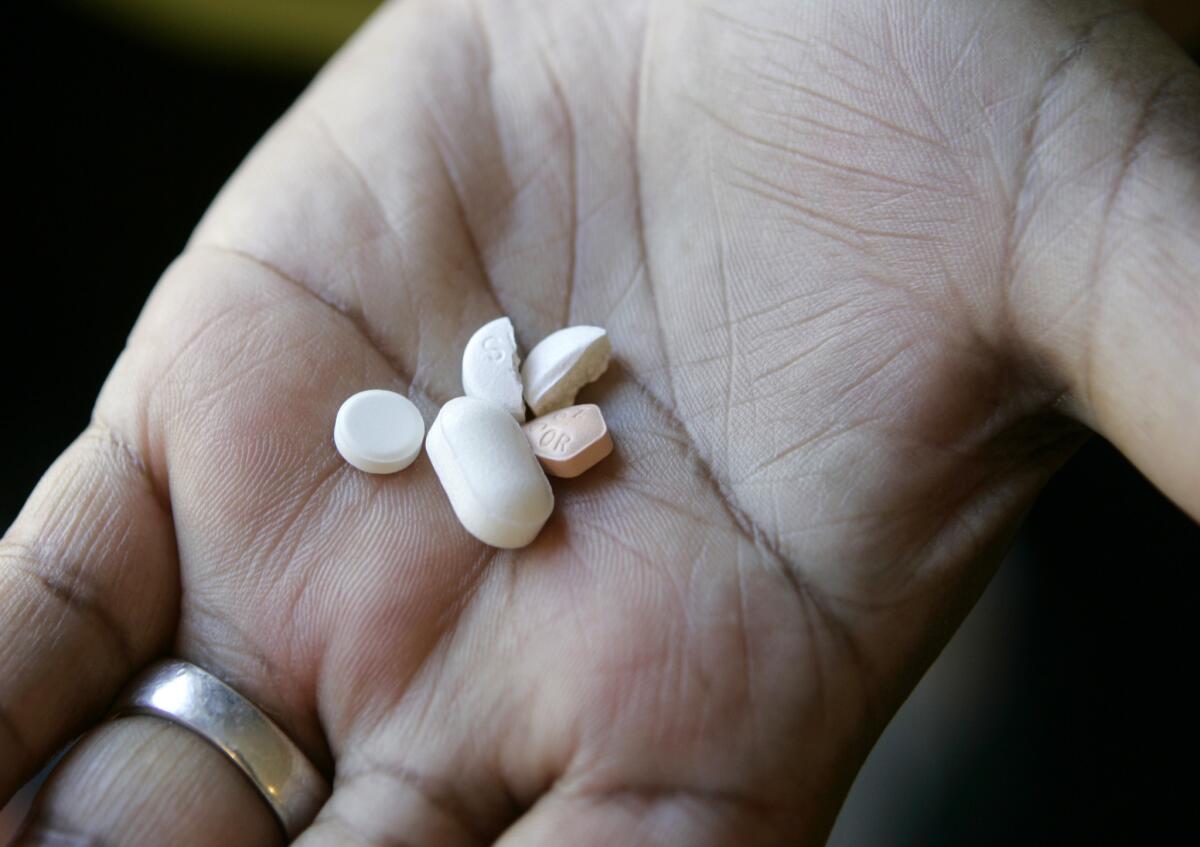
Prescription drug overdoses killed more than 37,000 Americans in 2009, according to the U.S. Centers for Disease Control; that death rate has tripled since 1990. The increase is not surprising, considering these additional CDC statistics: The number of prescriptions for painkillers has more than quadrupled since 1999, and more than 12 million Americans reported using prescription painkillers for non-medical reasons during 2010. In emergency rooms, more than 1 million patients were treated in 2009 for problems involving prescription painkillers or psychotherapeutic drugs such as anti-anxiety and sleep medications.
It’s a terrible and hideously expensive toll, made even sadder in California by the fact that the state has the data in its hands to help stave off some of the injury and death but isn’t using the information effectively.
In a series of investigative reports, “Dying for Relief,” Times staff writers Lisa Girion and Scott Glover delved into the cases of more than 1,700 people who, according to coroner’s records, died after taking drugs that had been prescribed to them. They found that a tiny proportion of doctors — one tenth of 1% — had written prescriptions for 17% of those who died.
TIMES INVESTIGATION: Legal drugs, deadly outcomes
Obviously, not all doctors who prescribe Oxycontin, Xanax and other such medications are being irresponsible, even those who write prescriptions in larger-than-normal numbers. Humane treatment of people in pain is as important as keeping drugs away from addicted or habitual users. But the series made it clear that a very small number of doctors have been linked in coroner’s records to an inordinate amount of suffering and death. And they and others could perhaps have been stopped if the state made better use of its CURES database, a system within the attorney general’s office that tracks prescriptions so that the state can monitor which doctors write them, which pharmacies fill them and which patients buy them.
One part of CURES, which stands for Controlled Substance Utilization Review and Evaluation System, was established in 2009 specifically for online monitoring of frequently abused drugs, so that physicians and other providers could tap in a patient’s identifying information and discover whether he or she had been obtaining similar prescriptions elsewhere. That same information, as Glover and Girion reported, could be reversed — the Medical Board of California, which oversees doctors, could use it to find, for example, the 50 or 100 doctors who had been writing the most prescriptions for frequently abused medications during the previous six months.
The system, however, doesn’t work quickly and was never fully updated, and it has never been used to identify doctors who might be overprescribing. In 2011, because of the state’s fiscal crisis, all funding for CURES was cut. Atty. Gen. Kamala Harris moved around enough money to keep CURES on life support — with one full-time staff member where there used to be several — but that has put the system even further behind and made it slower to use. Only about 10% of the medical providers who should be using the database actually do so. Harris’ office said last week that as a result of The Times’ series, doctors are lining up to join the monitoring program, but there’s not enough staff to add them in a timely fashion.
VIDEO: Pain doctors talk about their patients
It would take about $2.8 million to retool the system so that doctors could get practically instantaneous responses and so that the Medical Board could begin the necessary task of checking on doctors whose prescribing patterns look suspicious. Maintaining and staffing it properly would cost about $1.6 million a year.
Harris, the Medical Board and the Legislature should look for ways to make this happen while minimizing the impact on the general fund. For example, the state might assess an annual fee of less than $10 on each of the more than 200,000 healthcare professionals who should be using the system.
The state must then use the database to check on doctors whose prescribing habits look wildly out of whack. Even if the Medical Board looked only for that small segment of doctors prescribing the most potentially habit-forming drugs — not a difficult enforcement goal — it could probably prevent a hugely disproportionate number of medical emergencies and deaths.
More to Read
A cure for the common opinion
Get thought-provoking perspectives with our weekly newsletter.
You may occasionally receive promotional content from the Los Angeles Times.









