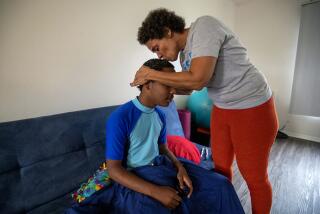
Mental health and children
- Share via
‘Ineed these pills refilled,” the weary mother says, displaying an array of empty bottles on the desk in my office. “My son is bipolar.”
The boy, a quiet slip of a 10-year-old, had been prescribed two antipsychotics, two mood stabilizers, one antidepressant, two attention deficit disorder medications and another medication to manage the side effects of the antipsychotics.
The mother explained that she had just regained custody of her son and his brother. During the last year, while they were in foster care, a doctor had diagnosed the 10-year-old with bipolar disorder and attention deficit disorder and prescribed eight medications.
In the hour I spent with the boy and his mother, he exhibited no signs or symptoms of bipolar disorder, though he did display some irritability. In school, he continued to perform poorly in his second attempt at third grade. Both irritability and poor school performance can be significant problems. But I strongly questioned his diagnosis.
Bipolar disorder is a serious and devastating disease characterized by extreme changes in mood, thought, energy or behavior. How did Ronnie get labeled with such a potentially debilitating illness and prescribed eight powerful medications within such a short time span? Unfortunately, his case isn’t unusual.
For a variety of reasons, bipolar diagnoses have become extremely popular. A Columbia University analysis of a National Center for Health Statistics survey found that the number of office visits for children diagnosed with bipolar disorder rose 40-fold between 1994 and 2003.
The reasons for the surge in bipolar diagnoses are complex. Despite advances in neuroscience, the brain, especially the developing brain, is still much of a mystery. More is unknown than known when it comes to effective treatment for children and adolescents with serious mental health problems. But that doesn’t stop doctors and parents from desperately wanting to believe there are simple solutions, and what could be simpler than a pill?
Since the 1980s, when pharmaceutical companies were granted permission to market their products directly to consumers, Americans have started believing that there is a drug to solve every discomfort and every mood. In my own practice, I’ve seen how determined parents can be to procure medication for their children that they have read about or seen advertised.
Meanwhile, pharmaceutical companies are paying inordinate sums of money to physicians to study their drugs. Doctors insist that they are not affected by the payments and that the research they do is pure, but it’s hard to believe that the funding streams have no influence.
Another impetus to prescribe is the changing nature of medical practices. Physicians spend more time now than ever waiting on the phone, filling out paperwork and jumping through a labyrinth of regulations from insurance companies in order to be allowed the opportunity to treat their patients. Additionally, insurance companies, via their reimbursement plans, discourage healthcare providers from spending the time necessary to assess and treat childhood mental health problems. The average doctor’s visit now wraps up in less than 15 minutes. It can be quicker and easier to medicate symptoms than to do a full assessment.
Even if doctors weren’t short on time, the country is short on board-certified child and adolescent psychiatrists, the physicians best-trained to diagnose and treat child mental health problems. This shortage puts pressure on child psychiatrists to increase their patient loads, which then reduces the amount of time they can spend with individual patients.
Adequately diagnosing psychiatric problems in a child requires multiple appointments and teamwork with the family, the school and the child. It requires a physician to stand up and say “no” to free gifts from drug companies and to critically review well-designed studies for appropriate assessment and treatment approaches. It requires our society to demand a healthcare system that affords access to appropriate levels of care, a system led by physicians who have demonstrated their commitment to the Hippocratic oath over financial gain. It requires the American people to take responsibility for their health and not expect pills to solve everything.
So what happened with the boy whose mother wanted me to refill his prescriptions? After an initial two-hour assessment at our clinic, he didn’t return for his next appointment. When the clinic called to ask why, the boy’s mother said that she had returned to his previous doctor. “Your doctor discriminated against me because I’m poor,” she said, “and my son needs those pills for his bipolar.”
Psychiatric assessment and treatment of a child can be hard. It often entails setting up educational testing to discover why he or she is failing in school, weekly individual and family therapy, and -- sometimes -- medication. I thought that my lengthy conversation with the boy’s mother had convinced her that the above plan would actually provide her son with better care than refilling all eight medications at once.
Unfortunately, families often put more faith in what they see and hear in advertising than they do in physicians. As physicians, we need to win them back.
Laurel L. Williams is program director of the Menninger Clinic’s adolescent treatment program and assistant director of residency training, child and adolescent psychiatry and assistant professor in the Menninger department of psychiatry and behavioral sciences at Baylor College of Medicine.
More to Read
A cure for the common opinion
Get thought-provoking perspectives with our weekly newsletter.
You may occasionally receive promotional content from the Los Angeles Times.