The Supreme Court just let a dangerous and intrusive abortion law stand
- Share via
This week, the Supreme Court announced, without explanation, that it would not hear a challenge to Kentucky’s so-called Ultrasound Informed Consent Act, which requires women to submit to a narrated ultrasound before receiving an abortion.
The court’s inaction leaves a dangerous law on the books, one that endangers not only women’s rights but also medical ethics.
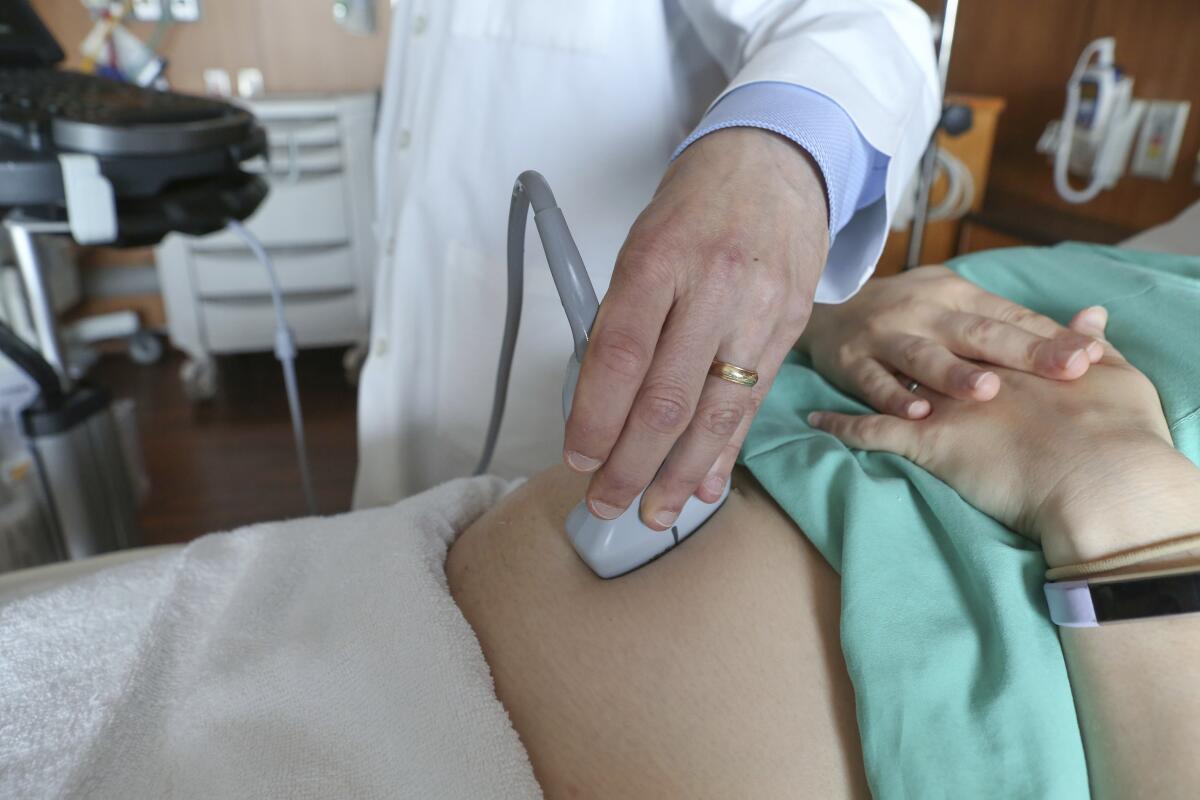
The Kentucky statute compels any doctor performing an abortion to first do an ultrasound on the patient and describe aloud the physical features of the fetus on the screen. The doctor must also play the sound of the fetal heartbeat.
Patients cannot opt out of hearing the doctor’s narration or the heartbeat. They cannot ask that the screen be turned away from them. The only way a patient has to avoid the ultrasound images or narration is to cover her ears and close her eyes while the physician speaks.
Physicians have no recourse either. There are no exceptions to the law’s ultrasound and narration requirement other than a narrow one for emergencies. They have to perform this grotesque ritual in every case — regardless of the patient’s wishes and the doctor’s assessment of whether it is appropriate. It must be read even when a patient has become pregnant through rape and in cases where there is a diagnosis of fetal anomaly that is incompatible with life.
Proponents of the law have said that it is based on “the commonsense notion that patients should be well equipped with relevant information before making important medical decisions.” Those are important values, central to moral requirements of informed consent, but this law does nothing to advance them.
To offer information that may assist patients in making medical decisions in alignment with their values, beliefs, and interests is the essence of the ethical practice of medicine. To force information on unwilling patients is precisely the opposite.
Informed consent serves two primary functions. First, it demonstrates respect for patients as autonomous, individuals who have control over their bodies, their lives, and their values; and second, it ensures patients have sufficient information about the risks, benefits, and alternatives to a procedure to make an informed decision about their health care.
The Kentucky law not only fails to honor the primary functions of informed consent but also violates them. We know the information contained in the ultrasound is not essential to informed consent — if it were, why would the law permit patients to close their eyes and block their ears? There is no justification for prohibiting physicians from respecting a patient’s request to stop speaking and to turn the images around.
Informed consent does not require that every patient be shown medical images in advance of a treatment decision. Certainly, images can be helpful to some patients, but for others they can undermine the patient’s ability to process the information relevant to their decision. Medical ethics require that physicians treat the patient as an individual, and the value or disvalue of viewing images will necessarily vary from patient to patient, and from decision to decision.
It is impossible to overstate how disrespectful forcing this information on patients is. The mandated speech occurs while the woman is in an extremely vulnerable position: half-naked, lying prone on an examination table with her legs in stirrups and a probe on her abdomen or inside her vagina. It is not only disrespectful but also in many cases is likely to be distressing, if not harmful. A woman who is terminating a wanted pregnancy due to a lethal fetal anomaly may suffer deeply from being forced to view and study the features of her fetus.
The Kentucky law reflects a complete misunderstanding of informed consent, turning it into something that has never existed in the long history of the concept. The law forces physicians to defy their professional ethical duties and contravene the trust that is essential in a doctor-patient relationship. It represents a state-mandated violation of “do no harm.”
I was one of more than 130 biomedical ethicists who joined together to urge the Supreme Court to hear the challenge to Kentucky’s law, and I was disappointed by the court’s decision not to weigh in on the issue. But it is critical to understand that the court’s decision not to hear this case is not a ruling on the underlying merits of the law or others like it. Similar laws have been struck down in Oklahoma and North Carolina, and those good decisions still stand. But there are also people working very hard to take Kentucky’s law to other states — and to pass a federal law as well.
In the wake of the court’s abdication, my colleagues and I will continue to speak out until politicians in Kentucky and around the country finally get the message to keep politics out of the exam room and the doctor-patient relationship.
Ruth Faden is founder of the Johns Hopkins Berman Institute of Bioethics and co-author of “A History and Theory of Informed Consent.”
More to Read
A cure for the common opinion
Get thought-provoking perspectives with our weekly newsletter.
You may occasionally receive promotional content from the Los Angeles Times.









