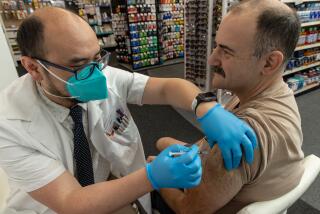
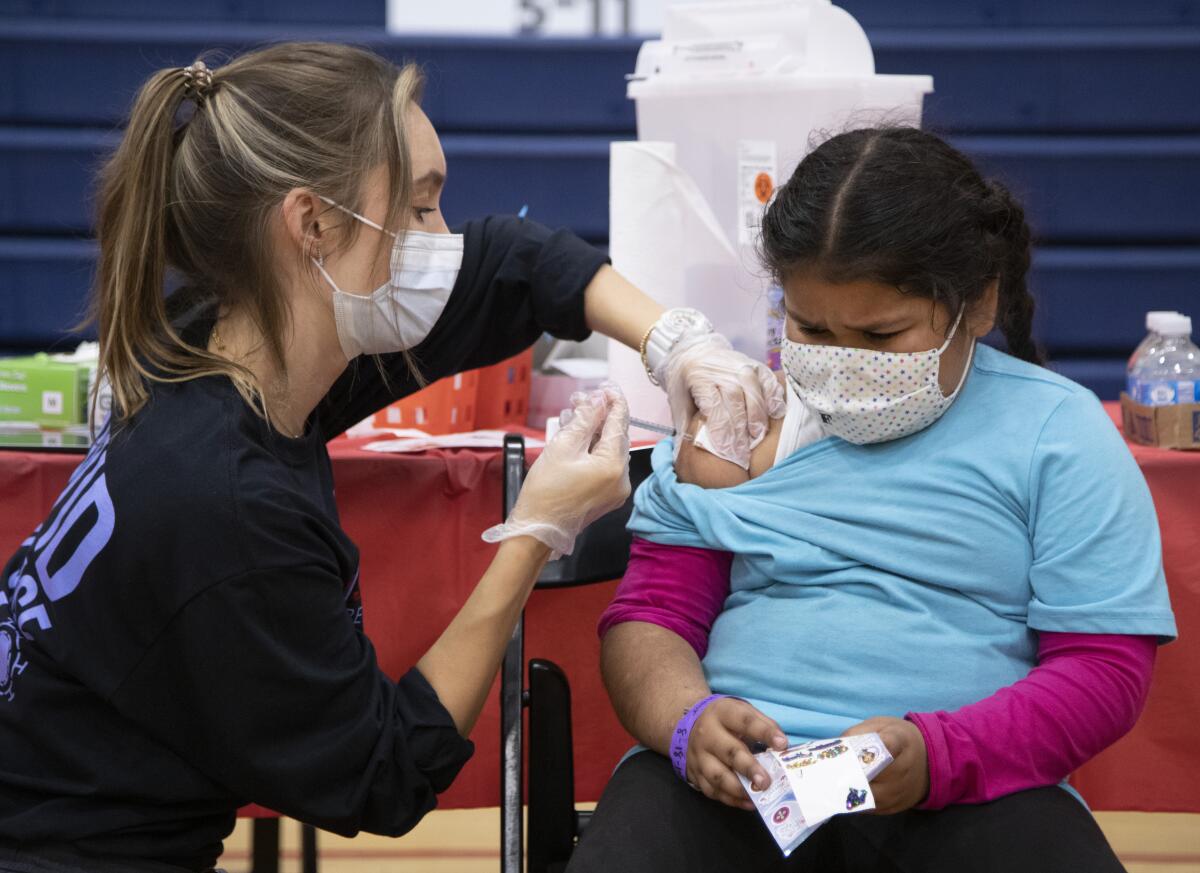
California gave up on mandating COVID vaccines for schoolchildren. Here’s why that’s wise
- Share via
A California Supreme Court decision last week reaffirmed that individual school districts lack the authority to require students to be vaccinated against COVID-19. A few weeks before that, officials in Gov. Gavin Newsom’s administration confirmed that they had abandoned plans to require COVID vaccination of schoolchildren, and legislation to similar effect was dropped last year. That means that, at least for the foreseeable future, COVID vaccines are unlikely to be added to the list of 10 inoculations California requires to attend school.
Some may fear this puts children and communities at unnecessary risk. But both our current scientific understanding of the COVID-19 vaccines and the drawbacks of mandating them suggest state officials and courts made the right call.
Unlike the other vaccines required for school enrollment in California, the COVID vaccines are unreliable at preventing infection or transmission, providing at best modest protection against infection for only a couple of months.
In contrast, the vaccines already required for school attendance, such as those for measles, mumps, rubella and polio, reliably prevent outbreaks when local vaccination rates reach a certain threshold. The hepatitis B and varicella (chickenpox) vaccines afford protection against infection for years, diminishing long-term transmission risks. The tetanus vaccine provides only individual protection, but it is administered in combination with vaccines for diphtheria and pertussis, which protect against outbreaks over the long term.
We never had any evidence that the COVID vaccines would work like vaccines that provide a high degree of lasting protection against infection and transmission, conferring so-called herd immunity. It has been clear that they would not since 2021 and even clearer since the emergence of the Omicron variant. One study found that after around five months, the COVID infection rate among vaccinated and unvaccinated adolescents ended up being essentially the same. And COVID vaccines do not appear to reduce infected people’s chances of infecting others either.
To be clear, there is good evidence that the COVID-19 vaccines have provided individual protection against severe disease and death. But the risks to most children at this point are slight. The Centers for Disease Control and Prevention estimate that over 96% of children have been infected with the virus, and studies continue to show that post-infectious or “natural” immunity is at least as protective as vaccine-induced immunity.
What’s more, a recent study of the Omicron variant in England found a COVID death rate in those under 20 of just 2 for every 1 million infections. It also found no children with prior infections had died of a subsequent SARS-CoV-2 infection. The COVID-associated condition known as multisystem inflammatory syndrome in children (MIS-C) has fortunately all but disappeared, and high-quality studies continue to demonstrate that long COVID is rare among children.
Some children are at higher risk from COVID than others. The absence of a state mandate, however, will not discourage families and physicians from deciding to vaccinate those children.
My own research team’s risk-benefit analyses for children and young adults support individualized approaches to COVID vaccination that weigh expected benefits against known potential side effects. One well-defined vaccine-associated risk is myocarditis, or inflammation of the heart muscle, which occurs disproportionately in adolescent and young adult males with potentially serious and lasting consequences. A high-quality prospective study estimated that the side effect would occur in about 1 in 3,000 13-to-18-year-old males who receive second doses of the Pfizer vaccine. A school mandate would therefore require many children to assume known risks for unclear benefits.
For international context, schools and universities in Europe are generally not requiring COVID vaccination. The European CDC is focusing on providing the bivalent booster to those who are 60 and older or have underlying conditions that put them at high risk. Britain is offering boosters only to those who are 50 and older, working in care homes or otherwise at high risk. France just announced that as of next fall, it will not recommend vaccination of people under 65 who are not deemed to be at high risk.
A statewide vaccine mandate also threatens to return thousands of students to remote schooling. That’s why the Los Angeles Unified School District indefinitely postponed its January 2022 deadline for students 12 and older to obtain a COVID vaccination. It became apparent that more than 30,000 unvaccinated students could be excluded from classrooms, disproportionately affecting young people of color who had already suffered substantial educational setbacks during the pandemic.
With California’s COVID vaccination rates hovering around 68% among 12-to-16-year-olds, 38% among 5-to-11-year-olds and just 8% among those under 5, mandating the vaccines in California schools could exacerbate declining public school enrollment, further jeopardizing the budgets of struggling districts whose students are, again, disproportionately the most vulnerable.
Restoring public trust requires practices that weigh the expected gains of any intervention against potential harms. A school vaccination mandate for COVID-19 would not substantially reduce the health risks to our children or communities, but it could unnecessarily exclude students from classrooms where they need to be.
Tracy Beth Høeg is a research epidemiologist at UC San Francisco and a physician. These views are her own.
More to Read
A cure for the common opinion
Get thought-provoking perspectives with our weekly newsletter.
You may occasionally receive promotional content from the Los Angeles Times.