Coronavirus Today: The threat of viral variants
- Share via
Good evening. I’m Amina Khan, and it’s Tuesday, Feb. 2. Here’s what’s happening with the coronavirus in California and beyond.
While the latest COVID-19 surge appears to be abating, officials say the recent progress could be undone by new versions of the coronavirus that have been springing up across the globe. Some of these variants are armed with novel mutations that make them more transmissible and possibly more virulent than their predecessors.
It’s a reminder that evolution never stops. But it’s happening faster than many experts expected, and it’s worsening fears that the coronavirus is already finding ways to evade our new vaccines, my colleague Emily Baumgaertner reports.
Case in point: An experimental vaccine made by Novavax was nearly 90% effective at preventing COVID-19 in clinical trials in Britain. But that figure fell to just 49% in South Africa, where nearly all of the infections the company analyzed involved the B.1.351 variant that emerged there late last year (and has subsequently found its way to the U.S. and at least 30 other countries).
Then there’s Johnson & Johnson, which said its new shot was 72% effective at preventing moderate or severe illness in the United States, but just 66% effective in Latin America and 57% effective in South Africa.
The makers of the two vaccines authorized for use in the U.S. — Pfizer and BioNTech for one, Moderna for the other — also wondered whether their shots would show any signs of reduced effectiveness. (In clinical trials conducted in the fall, both vaccines were at least 94% effective.) So they ran laboratory tests, introducing the virus to blood samples from vaccinated people.
The neutralizing antibodies formed in response to Moderna’s vaccine were equally effective against the original coronavirus and the more contagious U.K strain, but they were far less effective against the South Africa strain. Antibodies generated by the Pfizer-BioNTech vaccine were only slightly less effective against the South Africa variant compared with others. (Take this all with a few grains of salt, because lab tests like this give an imperfect understanding of true immune response.)
There were other clues that worrisome changes were afoot. Among them: the significant number of people who were contracting the coronavirus for a second time. That’s a sign that the immune protection gained as a result of a coronavirus infection wasn’t able to stave off a second one.
“From an evolutionary biology perspective, this is totally expected and anticipated,” said Dr. Michael Mina, a Harvard epidemiologist. “But it never feels good to be validated on something so scary.”
At this point in the pandemic, well over 100 million people have been infected worldwide. And every infection is an opportunity for the virus to generate a random mutation, Baumgaertner explains. A mutation that happens to give the virus an advantage (for example, an ability to resist the body’s natural defenses) can become the basis for a hardier variant.
The most concerning mutations affect the spike protein, which the virus uses to invade cells. The current crop of vaccines trains the immune system to recognize that protein, so mutations there raise the odds that the virus will slip by undetected.
Mina compared the process to searching for a criminal by memorizing the appearance of only his nose and mouth. This may work at first, but if the criminal gets a nose job, investigators will wish they learned about his eyes, ears and hair as well. That’s why it’s crucial to develop an arsenal of vaccines that use a variety of different approaches to recognize a viral invader, he said.
In the meantime, Moderna is responding to the new threat by trying to develop a special booster shot that would target the South Africa variant. In addition, the company plans to test whether a third shot of its original formula would help against other strains. BioNTech is also considering developing an adjusted vaccine.
Dr. Anthony Fauci, the U.S.’s top infectious disease expert, said the arrival of more transmissible strains in the U.S. is a “wake-up call” that underscores the need to rapidly vaccinate Americans. “Vaccinating as many people as we can, as quickly as we can,” is the key to slowing the virus’ ability to mutate, he said. “Viruses cannot mutate if they cannot replicate.”
The U.S. is now vaccinating about 1.2 million people a day, but experts say that’s too slow a pace. There’s no way to know what kinds of variants will exist by the time the inoculation campaign reaches critical mass.
“If you think you’re going to simply vaccinate your way out of this, it’s going to be like whack-a-mole,” said Susan Butler-Wu, director of clinical microbiology at L.A. County-USC Medical Center. People also have to continue — or get better at — social distancing and mask-wearing if we want our collective investment in the vaccine effort to pay off.
Ultimately, an effective vaccination campaign can’t just happen in the U.S. and a few other countries; it has to encompass the whole world. If it doesn’t, there will still be places for new and more dangerous strains to develop. “You can vaccinate the hell out of America,” Mina said, but “until everyone is protected, we’re all still at risk.”
By the numbers
California cases, deaths and vaccinations as of 5:02 p.m. PST Tuesday:
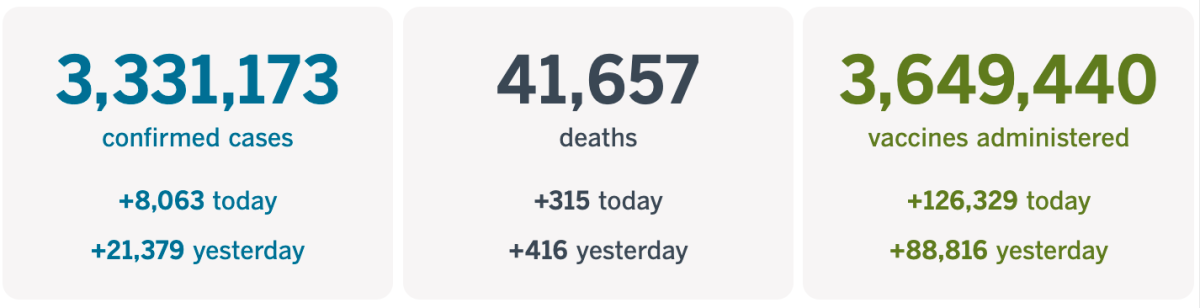
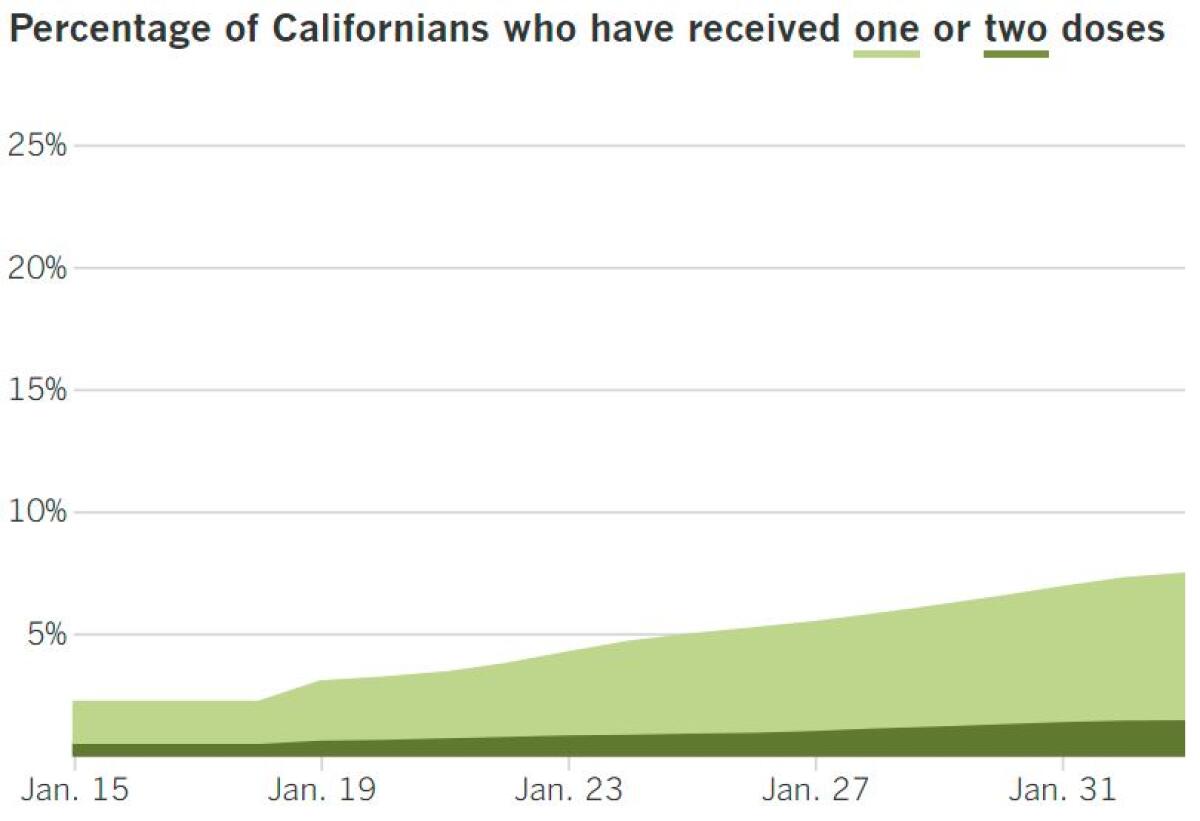
Track California’s coronavirus spread and vaccination efforts — including the latest numbers and how they break down — with our graphics.
Across California
A coronavirus variant from Brazil has been detected in the Bay Area, my colleague Alex Wigglesworth reports. Researchers at Stanford’s Clinical Virology Laboratory screened nearly 1,000 viral specimens during the last two weeks and found one case of the Brazilian variant known as P.2, said Dr. Benjamin Pinsky, the lab’s medical director. The find was reported to public health authorities in late January.
The researchers also identified four cases of the more transmissible, possibly more virulent coronavirus strain from the U.K., known as B.1.1.7, that was already known to be circulating in California. And they found that about 29% of the specimens had the L452R mutation, a feature of a homegrown variant that has been cropping up in tests across the state.
This proliferation of viral variants in the Golden State may have been a factor in “the humongous surge we’ve seen over the last six weeks or so,” said Dr. Edward Jones-Lopez, an infectious diseases expert at USC. “And it could get even worse if these strains are indeed fitter than previous strains and people lower their guard and we are not very logistically efficient in delivering vaccines.”
Meanwhile, vaccine troubles continue. Californians with disabilities are expressing outrage over losing their place in the vaccination line. Take 47-year-old Ntombi Peters, a Long Beach resident with severe asthma and multiple sclerosis who’d been eagerly awaiting the shots. Her health conditions put her at risk of a severe case of COVID-19, which is why she had expected her turn to be next — until Gov. Gavin Newsom announced last week that residents would be prioritized by age instead.
“They act as if we do not exist. Or if we do, we’re expendable,” said Peters, who uses multiple inhalers and is on immunosuppressant drugs. “It’s very disheartening.”
California has so far had one of the slowest vaccine rollouts in the country. The state has used a smaller percentage of its available doses and has vaccinated a smaller percentage of its population than other large states. Everyone agrees that’s an equity problem, because the burden of unchecked transmission falls disproportionately on those least able to shelter from the virus and those most vulnerable to its worst outcomes. The disagreement is over whether speed or fairness matters more.
“We talk about this as a trade-off of efficiency and equity, but I think there’s just issues of general effectiveness,” said Dr. Kirsten Bibbins-Domingo, an epidemiologist and co-founder of the UC San Francisco Center for Vulnerable Populations. “Age is not only efficient, it’s easy for the vaccination sites to confirm.”
In other news, state corrections officials ignored the warnings of front-line health workers and pressured them to transfer 189 potentially coronavirus-infected people incarcerated in a Chino men’s prison to San Quentin State Prison last May — triggering a deadly outbreak of COVID-19, according to the California Office of Inspector General. By the end of August, 2,237 prisoners and 277 staff members at the prison had been infected; 28 prisoners and one staffer ultimately died there.
At the time of the moves, the Chino prison reported more than 600 cases of COVID-19 and nine deaths. The 189 San Quentin-bound people were among 700 selected for transfer who had medical conditions that made them especially vulnerable to the virus.
Two of the prisoners had COVID-19 symptoms upon arrival at the storied Bay Area facility, including one with a fever of 101.1 degrees. But even though the San Quentin health staff suspected that those transferred from Chino had been exposed to the virus, the prison housed 119 of them in a unit that lacked solid doors, allowing air to flow freely through the cells. By the time coronavirus test results came back, 14 infected people had been housed in the unit for at least six days, the report noted.
The deaths sparked outrage from prisoner advocates and legal action by some inmates’ families. In September, lawyers for the family of 61-year-old Daniel Ruiz filed a government claim, a precursor to a lawsuit against the corrections agency. Ruiz died July 11 after contracting the virus while serving time in San Quentin for a minor drug crime.
“It is tragic and unacceptable that some prison bureaucrats treated them as less than human,” attorney Michael Haddad said. After reviewing the inspector general’s report, he added: “If these prison officials’ goal was to give prisoners COVID-19, it is hard to think what they could have done more effectively.”
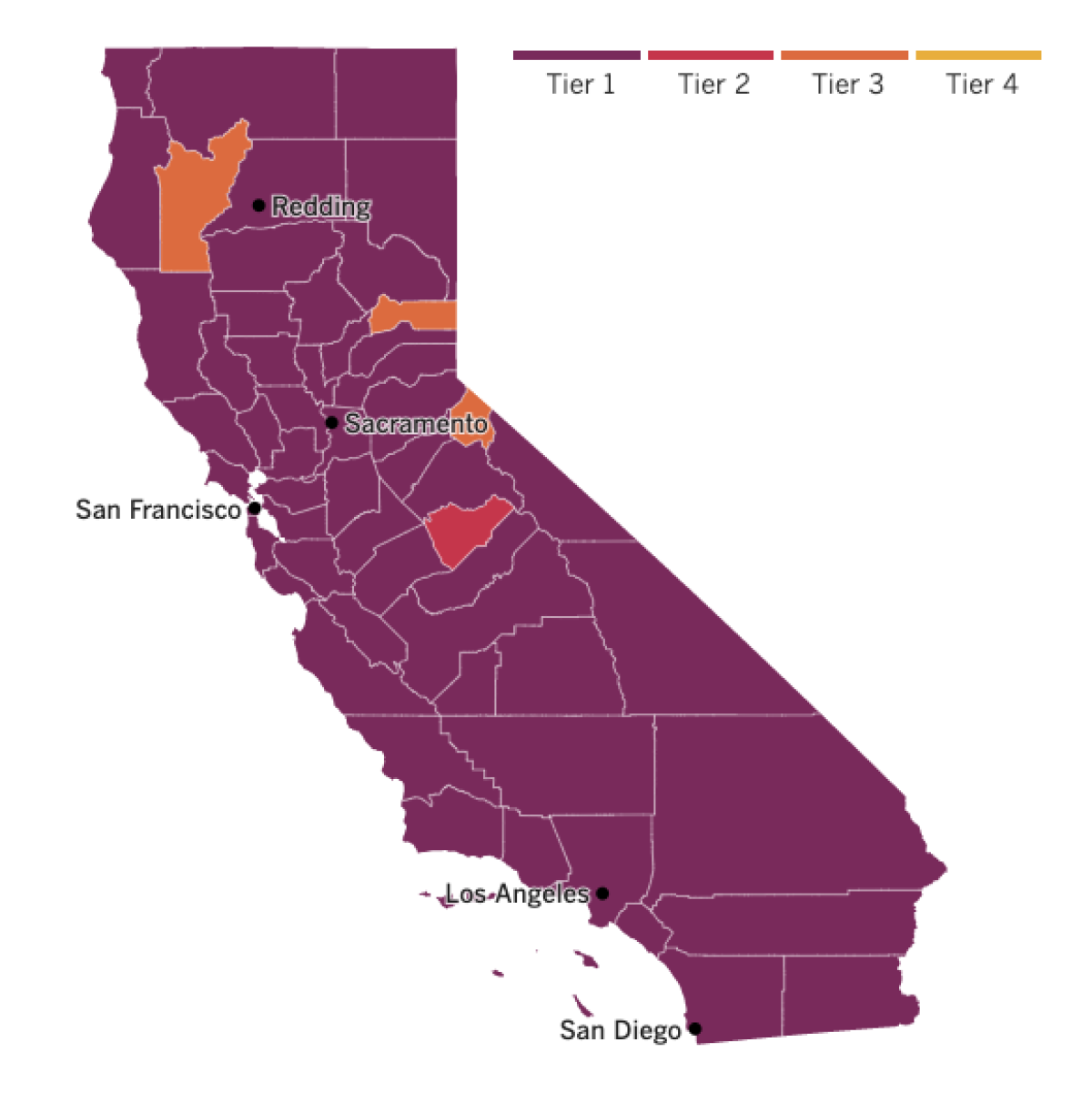
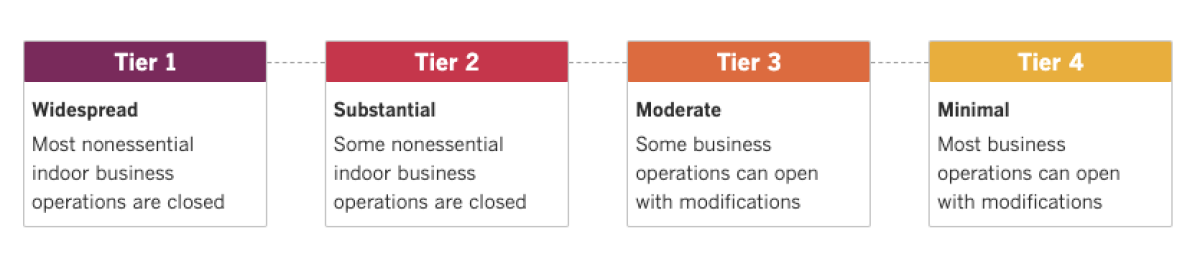
See the latest on California’s coronavirus closures and reopenings, and the metrics that inform them, with our tracker.
Consider subscribing to the Los Angeles Times
Your support helps us deliver the news that matters most. Become a subscriber.
Around the nation and the world
In Washington, senators moved Tuesday toward fast-tracking approval of President Biden’s $1.9-trillion coronavirus recovery package — with or without Republican support. Senate Majority Leader Charles E. Schumer (D-N.Y.) said Congress must take bold action toward “America’s long-awaited comeback.” The procedural vote launches a lengthy budget procedure that would allow Democrats, who have a slim majority, to pass Biden’s proposal on their own if Republicans object.
The move comes after Biden told Republican senators during a two-hour meeting that he’s unwilling to settle on a slimmed-down coronavirus aid package. No compromise was reached Monday night, and Biden has made it clear that he won’t delay aid in hopes of winning GOP support.
White House Press Secretary Jen Psaki said that although there were areas of agreement, “the president also reiterated his view that Congress must respond boldly and urgently, and noted many areas which the Republican senators’ proposal does not address.” The Republican group of 10 senators focuses primarily on the healthcare crisis and direct aid to Americans, while Biden’s proposal offers larger direct payments and a more sweeping rescue package to shore up households, local governments and a partly shuttered economy.
In China, authorities have apprehended more than 80 suspected members of a criminal group accused of manufacturing and selling fake COVID-19 vaccines, including to other countries (though it was unclear which ones). Police in Beijing and in Jiangsu and Shandong provinces broke up the ring, which was making fake vaccines out of a simple saline solution, the official Xinhua News Agency said. The group had reportedly been active since last September.
China has a long history of vaccine scandals. In 2016, for instance, police arrested two people in charge of a ring that sold millions of improperly stored vaccines. In response to such scandals, China reformed its vaccine-safety regulations and increased criminal penalties for those caught making counterfeits. And although surveys found public trust in vaccines reportedly fell after the scandals, some 74% of respondents in a recent survey said they would take a COVID-19 vaccine if it was available.
China has at least seven COVID-19 vaccines in the last stage of clinical trials, as well as one that has been approved for domestic use made by state-owned Sinopharm. Chinese vaccine makers have gone global during the pandemic, with Sinopharm and other domestic companies making deals with or donating their vaccines to at least 27 countries around the world.
A very sad follow-up to yesterday’s newsletter: Capt. Tom Moore, the British World War II veteran beloved for walking up and down his garden to raise money for healthcare workers during the pandemic, has died after testing positive for the coronavirus. He was 100.
Capt. Tom, as he became known in newspaper headlines and TV interviews, had set out to raise 1,000 pounds, equivalent to $1,364, for Britain’s National Health Service by walking 100 laps of his backyard during the first wave of the pandemic. But with donations pouring in from across Britain and as far away as the United States and Japan, he wound up raising some $40 million.
Moore’s family announced his death on Twitter, posting a picture of him behind his walker in a happy moment, ready for an adventure. “The last year of our father’s life was nothing short of remarkable. He was rejuvenated and experienced things he’d only ever dreamed of,” the family’s statement said. “Whilst he’d been in so many hearts for just a short time, he was an incredible father and grandfather, and he will stay alive in our hearts forever.”
Your questions answered
Today’s question comes from readers who want to know: Which company’s vaccine should I get?
There’s no sense being picky — experts say you should take the first authorized vaccine that’s offered to you.
It’s true that the newest COVID-19 vaccine on the horizon, from Johnson & Johnson, may be a little less effective at preventing illness than the Pfizer-BioNTech and Moderna offerings that are already being administered around the U.S. But experts say it’s still worth a (literal and proverbial) shot.
J&J recently said that in a 45,000-person trial, its vaccine was about 66% effective at preventing moderate to severe cases of COVID-19. No one who received the vaccine was hospitalized with or died of the disease, according to the company, which said it expected to seek emergency use authorization from the Food and Drug Administration as early as this week.
The J&J vaccine is similar to the shots from Pfizer-BioNTech and Moderna but uses a different strategy for transporting genetic code into human cells to stimulate an immune response to the virus. All three do a good job at preventing serious illness.
“It’s a bit like, do you want a Lamborghini or a Chevy to get to work?” said Dr. Gregory Poland, director of the Mayo Clinic’s Vaccine Research Group. “Ultimately, I just need to get to work. If a Chevy is available, sign me up.”
In their clinical trials, the Pfizer-BioNTech and Moderna vaccines were 95% and 94% effective at preventing COVID-19. But they were tested in different locations and at different phases of the pandemic, before the new, worrisome variants were circulating here. Contrast that with the J&J trial, which began in September in South America and South Africa as well as the U.S. The Pfizer-BioNTech and Moderna vaccines might not have gotten the same sparkling results had they been tested more recently — or in South Africa.
Also, J&J gave subjects in its trial only one dose of the vaccine, whereas Pfizer and Moderna have two-dose schedules, separated by 21 and 28 days, respectively.
“We don’t know which vaccines are the Lamborghinis,” Poland said, “because these aren’t true head-to-head comparisons.”
The J&J vaccine seems to cause fewer serious side effects, so it “may be a better vaccine for the infirm,” said Dr. Kathryn Edwards, scientific director of the Vanderbilt Vaccine Research Program. And it’s much easier to ship, store and administer. That makes it a simpler choice for rural areas.
“A vaccine doesn’t have to be 95% effective to be an incredible leap forward,” said E. John Wherry, director of the Institute for Immunology at the University of Pennsylvania’s Perelman School of Medicine. “When we get to the point where we have choices about which vaccine to give, it will be a luxury to have to struggle with that question.”
We want to hear from you. Email us your coronavirus questions, and we’ll do our best to answer them.
Resources
Need a vaccine? Keep in mind that supplies are limited, and getting one can be a challenge. Sign up for email updates, check your eligibility and, if you’re eligible, make an appointment where you live: City of Los Angeles | Los Angeles County | Kern County | Orange County | Riverside County | San Bernardino County | San Diego County | San Luis Obispo County | Santa Barbara County | Ventura County
Practice social distancing using these tips, and wear a mask. Here’s how to do it right.
Watch for symptoms such as fever, cough, shortness of breath, chills, shaking with chills, muscle pain, headache, sore throat and loss of taste or smell. Here’s what to look for and when.
Need to get tested? Here’s where you can in L.A. County and around California.
Americans are hurting in many ways. We have advice for helping kids cope, resources for people experiencing domestic abuse and a newsletter to help you make ends meet.
For our most up-to-date coverage, visit our homepage and our Health section, get our breaking news alerts, and follow us on Twitter and Instagram.




