Coronavirus Today : What does it mean to be ‘fully vaccinated’?
- Share via
Good evening. I’m Karen Kaplan, and it’s Tuesday, Dec. 14. Here’s the latest on what’s happening with the coronavirus in California and beyond.
If there’s something public health officials love as much as COVID-19 vaccines, it’s COVID-19 booster shots.
Dr. Anthony Fauci, President Biden’s senior advisor on the pandemic: “Optimal protection is going to be with a third shot.”
Dr. Rochelle Walensky, director of the Centers for Disease Control and Prevention: “CDC is strengthening its booster recommendations and encouraging everyone 16 and older to receive a booster shot.”
Dr. Janet Woodcock, acting Food and Drug Administration commissioner: “Vaccination and getting a booster when eligible ... remain our most effective methods for fighting COVID-19.”
Barbara Ferrer, director of the Los Angeles County Department of Public Health: “Please don’t wait any longer. The boosters are essential.”
What accounts for these ardent endorsements? The passage of time has made clear that the vaccines’ impressive early effectiveness lasted only a few months before beginning to wane.
The first signs came over the summer. Breakthrough infections were occurring with increasing frequency in two groups: older adults and people with compromised immune systems. These are folks who typically don’t mount a strong immune response to vaccines, and many experts hoped these groups were not indicative of a larger problem, my colleague Melissa Healy reports.
Alas, in the weeks and months that followed, the evidence piled up showing that all three vaccines used in the United States were not offering as much protection as they did initially. It was true for people of all ages — even young adults who were fully vaccinated were coming down with breakthrough infections that, in rare cases, caused severe illness and even death.
That’s the bad news. The good news is that it appears immunity can be restored with a booster shot. There’s even some evidence that antibody levels after a booster dose are higher than antibody levels soon after becoming fully vaccinated.
Here’s one piece of evidence in favor of getting a booster if it’s been at least six months since your second dose of the Pfizer-BioNTech or Moderna vaccine or at least two months since you got the Johnson & Johnson shot: During the week that ended Nov. 29, L.A. County reported 43 new coronavirus infections per 100,000 residents who were fully vaccinated but had not received a booster shot — but just seven new infections per 100,000 residents who were vaccinated and boosted.
In other words, the infection risk was six times lower for those who had gotten a booster shot.
Such data have prompted some experts not only to recommend booster shots but to argue that until you’ve had one, you shouldn’t be considered “fully vaccinated.”
There’s precedent for requiring three — or more — doses of a vaccine, said Dr. William Schaffner, an infectious-disease specialist at Vanderbilt University Medical School. Becoming fully immunized against polio, hepatitis B, diphtheria, tetanus or pertussis requires at least three shots, sometimes more.
Dr. Peter Hotez, dean of Baylor College of Medicine’s National School of Tropical Medicine, agreed that our past experience with other shots offered strong hints that one or two doses of COVID-19 vaccine wouldn’t cut it over the long term.
“From the beginning, I’ve said this is a three-dose vaccine,” Hotez said.
Not everyone agrees. The evidence in favor of offering boosters to healthy people under 50 is not as strong as it is for other groups, said Dr. Emily P. Hyle, an infectious-disease specialist at Massachusetts General Hospital. Giving booster shots to comparatively low-risk Americans when so much of the world is still waiting for its initial doses may be unethical, she said.
It may even be counterproductive, considering that large, unvaccinated populations provide fertile ground for new coronavirus variants to emerge before spreading around the world. (Omicron, I’m talking about you.)
So far, the CDC hasn’t amended its definition of “fully vaccinated,” so booster shots are still optional. Americans who are subject to job-related vaccination mandates or are required to show proof of “full vaccination” to enter gyms, restaurants or public events can satisfy the requirement without a booster.
Fauci, too, has stopped short of advocating for a new definition. But it’s clear he expects it to happen sooner or later.
“It’s going to be a matter of when, not if,” Fauci said.
By the numbers
California cases and deaths as of 5:05 p.m. Tuesday:
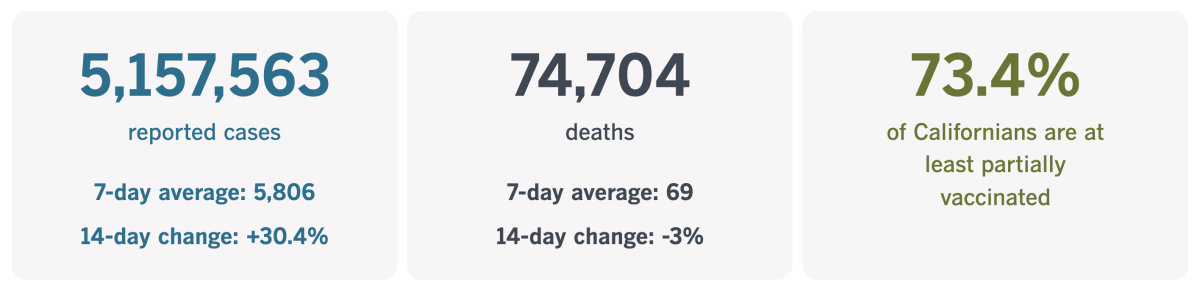
Track California’s coronavirus spread and vaccination efforts — including the latest numbers and how they break down — with our graphics.
Meet the woman who facilitated thousands of vaccinations in South L.A.
There are people — lots of them — who feel strongly that the best way to protect a community from COVID-19 is to help folks get vaccinated. And in California, the demographic group with the highest percentage of unvaccinated members is Black residents.
According to The Times’ tracker, 46% of Black Californians have not received a single dose of COVID-19 vaccine. That compares with 35% of white residents, 44% of Latinos, 11% of Asians and 42% of Native American and Alaska Natives. The disparity is one reason Black residents make up a disproportionate share of the state’s COVID-19 deaths.
This far into the pandemic, it should be news to no one that the coronavirus has treated some groups worse than others. Public health leaders lament this fact regularly and pledge to do something about it.
Tsega Habte is beating them to it.
Habte is Eritrean by birth, a pharmacist by trade and a concerned community member at heart. She has lived in the Los Angeles area since 1983 and threw herself into civic life by joining the faculty of the Charles R. Drew University of Medicine and Science and becoming an active congregant of the First African Methodist Episcopal Church.
Habte is “a meddler too interested in the lives of others,” as my colleague Donovan X. Ramsey put it. “But she meddles for good.”
You could see her commitment on the fliers she posted to advertise her first COVID-19 vaccination clinic: She was so determined to recruit people that she included her personal cellphone number.
Habte joined the fight against the coronavirus in April 2020, working with Eritrea’s Ministry of Health to provide personal protective equipment and other resources to Eritreans in Los Angeles. Last December, when the first COVID-19 vaccines were authorized, she shifted her focus to immunizations.
Ramsey describes a March meeting at the Kedren Community Health Center, a vaccination hub for Black Los Angeles. Dr. Jerry P. Abraham, Kedren’s director of vaccines, brought together community leaders to brainstorm ideas for increasing the number of shots the center could administer each day.
Most people in the room where reserved. But not Habte.
“I said, ‘Dr. Abraham, I am here dedicated to make sure Eritreans, Ethiopians and all other Black and brown people get vaccinated,’” she recalled.
Abraham said he was astonished by her eagerness: “She just stepped up.”
And she followed through.

She recruited volunteers to staff events and provide translation services. She partnered with L.A.’s Civil + Human Rights and Equity Department to get face masks and hand sanitizer to people who needed them. In April, she worked with Kedren to set up a vaccination clinic at First AME geared toward members of the East African community. Another clinic followed in May, targeting West African immigrants.
Habte was able to bring in people who were largely beyond the reach of public health officials. As fellow immigrants, many were not English speakers, and some had limited access to technology.
Altogether, her work with Kedren has helped at least 3,000 people get vaccinated. “It’s probably more, to be honest,” said Abraham. The efforts have earned Habte the title “Mama Tsega.”
Other fans include L.A. Mayor Eric Garcetti, who was the first guest on Habte’s new YouTube talk show.
“First of all, Tsega, thank you for everything that you do and everything that you are,” Garcetti said. “Your work saves lives.”
Carmen Hayward-Stetson is one of Habte’s closest friends. She says her pal’s formula for success is straightforward.
“When it comes to approaching people about whatever it is that she’s trying to accomplish, she thinks ‘no’ means ‘not yet,’” Hayward-Stetson said.
California’s vaccination progress
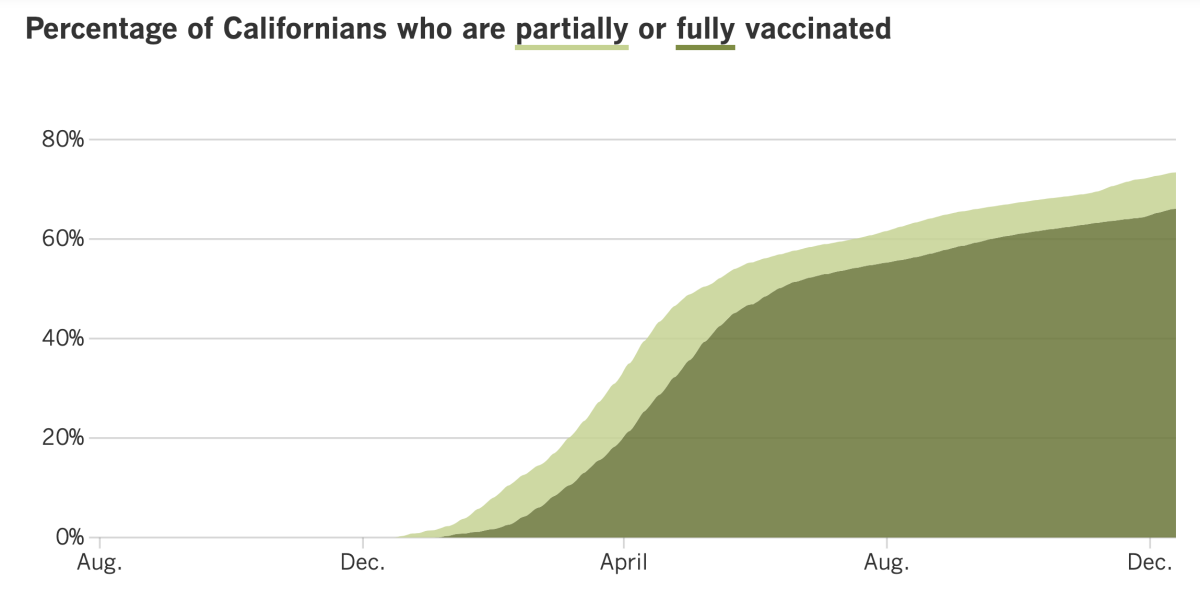
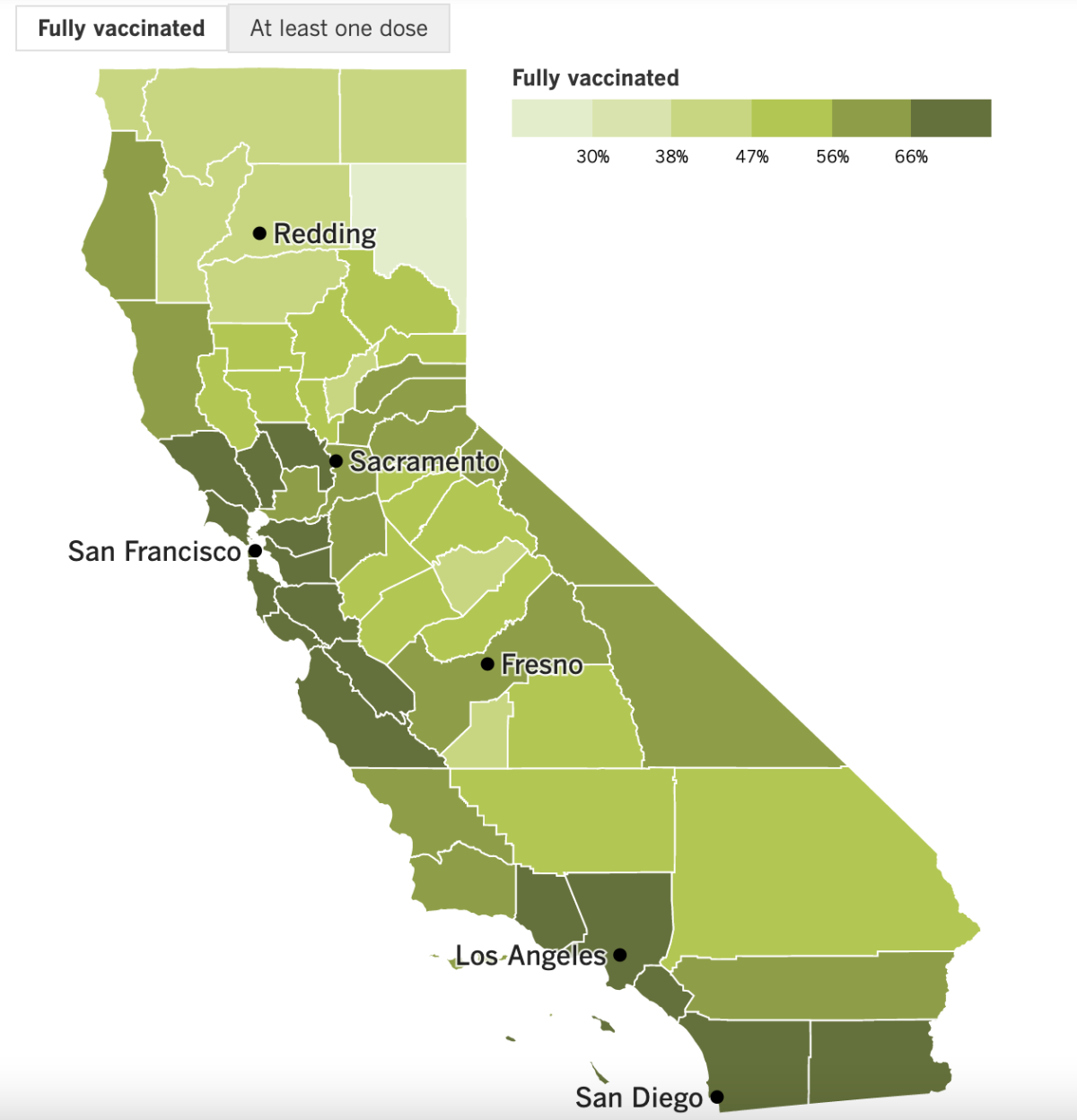
See the latest on California’s vaccination progress with our tracker.
Your support helps us deliver the news that matters most.
In other news ...
We’re still in the getting-to-know-you phase of our relationship with Omicron, but thanks to researchers in South Africa, we have a lot more insight into the coronavirus variant today than we did yesterday.
For starters, it looks like Omicron is less impressed with immunity than other variants. Echoing earlier findings, the researchers said people who’d already had COVID-19 were more likely to be reinfected with Omicron than with other versions of the coronavirus.
Vaccine-induced immunity also took a hit. Two doses of the Pfizer-BioNTech vaccine were only 33% effective at preventing coronavirus infections during the country’s Omicron-driven wave and 70% effective at reducing the risk of hospitalization. Earlier in the pandemic, the same vaccine reduced infection risk by 80% and hospitalizations by 93%. (The researchers didn’t report findings about booster shots, which aren’t widely available in South Africa.)
Regardless of vaccination status, adults sickened by Omicron are about 29% less likely to need hospital treatment than adults infected with earlier variants.
The findings are based on records of more than 211,000 coronavirus tests conducted between Sept. 1 and Dec. 7. The researchers divided them into two groups — before and after Omicron — and compared how patients fared. They didn’t confirm whether people in the second period were infected with Omicron, but they said it was a good proxy for assessing the variant.
Before we leave South Africa, I’ll note that President Cyril Ramaphosa tested positive for a coronavirus infection on Sunday and was being treated for mild COVID-19 symptoms. He is 69 and fully vaccinated. Officials didn’t say whether his case was caused by Omicron.
In the United Kingdom, Prime Minister Boris Johnson has warned that a “tidal wave” of Omicron infections may be coming soon and urged all adults in England to get a booster shot by the end of December, a month sooner than previously planned. The public listened, lining up Monday at vaccination centers across Britain.
Johnson said cases involving the highly transmissible variant were doubling there every two to three days. The U.K. Health Security Agency warned that Omicron was quickly gaining ground on Delta there and could surpass it “in mid-December” — in other words, any day now.
Americans appear to be paying attention to the threat, but they’re certainly not panicking. A poll conducted Dec. 2-7 — a week or more after Omicron burst into the headlines — found that 36% of those surveyed were “very” or “extremely” worried that they or a family member would become infected with the coronavirus. That’s up from 25% in late October but less than in August, when the Delta surge was getting underway.
Most respondents who were vaccinated said they were at least “somewhat” concerned about becoming infected, whereas 55% of unvaccinated respondents said they weren’t. The increased worry among the vaccinated majority is also reflected in the fact that 57% of Americans are wearing masks “always” or “often” when they’re around other people in public, up from 51% in August. (In February and March, before vaccines were widely available, 82% of Americans said they usually wore masks under those conditions.)
Speaking of which, all Californians — vaccinated or not — will have to start wearing masks in indoor public spaces under a statewide order that goes into effect Wednesday and lasts until Jan. 15.
Coronavirus cases in the Golden State have risen almost 50% in the last 2½ weeks, and COVID-19 hospitalizations are up nearly 15%. These could be signs that an Omicron surge, another winter surge or a combination of the two is in the offing, and health officials hope the mask mandate will help nip it in the bud.
“This is a critical time where we have a tool that we know has worked and can work,” said Dr. Mark Ghaly, the California health and human services secretary. “We are proactively putting this tool of universal indoor masking in public settings in place to ensure we get through a time of joy and hope without a darker cloud of concern and despair.”
Roughly half the state’s population is already subject to a county-level indoor mask mandate, including residents of Los Angeles and Ventura counties and most of the San Francisco Bay Area. Now San Diego and Orange counties, the Inland Empire, the Central Valley and rural Northern California will have to mask up as well.
New York state has also enacted a statewide mask mandate for indoor public spaces, although there’s an exception for cases where everyone indoors is vaccinated.
Moving from mask mandates to vaccine mandates: A judge in Los Angeles has denied a request from the L.A. police union to temporarily block implementation of the city’s vaccination requirement until a lawsuit challenging it could proceed. It was the second time this month that a judge sided with the city, having rejected a similar request from the union that represents L.A. firefighters on Dec. 3.
L.A. County Superior Court Judge Mitchell L. Beckloff concluded that to protect both city workers and the public, the vaccination mandate could not be put on hold. The mandate requires workers to be vaccinated against COVID-19 unless they get a medical or religious exemption.
And finally, the U.S. Air Force has discharged 27 people who refused to comply with a federal vaccine mandate and didn’t seek a medical, religious or administrative exemption. They are believed to be the first service members removed from the military for disobeying the order to get the shots.
Your questions answered
Today’s question comes from readers who want to know: Can I use money in my flexible spending account to buy COVID-19 supplies?
You sure can.
With just 17 days left in the year, you might be looking for purchases that can be reimbursed with the funds in your flexible spending account. (If you have one, you already know that an FSA allows you to set aside pretax income to spend on medical purchases. The main catch is that the funds you set aside usually have to be used within the calendar year.)
Traditionally, the money in an FSA is used to pay for prescription drugs, co-pays for doctor’s visits, a new pair of eyeglasses or the like. If there’s still money left in December, you may find yourself stocking up on qualifying items like over-the-counter medications, a heating pad or sunscreen.
Now COVID-19 supplies are eligible for FSA reimbursement too. Qualifying items include face masks, hand sanitizer and sanitizing wipes. More durable items like thermometers and pulse oximeters count too.
So do rapid COVID-19 tests, which you can take at home. They can be purchased in drug stores or online (prices range from $14 to $35 for a two-pack). This month, President Biden announced a plan to require health insurance companies to reimburse members who buy the tests. If you’re willing to file whatever paperwork that might entail, you can save your FSA funds for something else. (Under Biden’s plan, people who don’t have health insurance can get free COVID-19 tests at community health centers and rural clinics.)
Keep in mind that you don’t have to spend down all the money in your account by Dec. 31. As my colleague Jessica Roy explains, the maximum amount you could put into an FSA this year was $2,750, and up to $550 of that can be rolled over into your account for 2022. (The exact amount you can save depends on your particular plan, so be sure to check.)
There’s one more caveat you should know about: Since the pandemic prompted some people to put off non-urgent healthcare visits, Congress changed the rules for this year and made it possible to roll over all the money in your account — but you have this option only if your workplace opted in. You can find out by asking your benefits provider or human resources department.
We want to hear from you. Email us your coronavirus questions, and we’ll do our best to answer them. Wondering if your question’s already been answered? Check out our archive here.
Resources
Need a vaccine? Here’s where to go: City of Los Angeles | Los Angeles County | Kern County | Orange County | Riverside County | San Bernardino County | San Diego County | San Luis Obispo County | Santa Barbara County | Ventura County
Practice social distancing using these tips, and wear a mask or two.
Watch for symptoms such as fever, cough, shortness of breath, chills, shaking with chills, muscle pain, headache, sore throat and loss of taste or smell. Here’s what to look for and when.
Need to get a test? Testing in California is free, and you can find a site online or call (833) 422-4255.
Americans are hurting in many ways. We have advice for helping kids cope, resources for people experiencing domestic abuse and a newsletter to help you make ends meet.
We’ve answered hundreds of readers’ questions. Explore them in our archive here.
For our most up-to-date coverage, visit our homepage and our Health section, get our breaking news alerts, and follow us on Twitter and Instagram.




